| Colitis | |
|---|---|
 | |
| A micrograph demonstrating cryptitis, a microscopic correlate of colitis. H&E stain. | |
| Specialty | Gastroenterology |
Colitis is swelling or inflammation of the large intestine (colon).[1] Colitis may be acute and self-limited or long-term. It broadly fits into the category of digestive diseases.
In a medical context, the label colitis (without qualification) is used if:
- The cause of the inflammation in the colon is undetermined; for example, colitis may be applied to Crohn's disease at a time when the diagnosis is unknown, or
- The context is clear; for example, an individual with ulcerative colitis is talking about their disease with a physician who knows the diagnosis.
Signs and symptoms
[edit]The signs and symptoms of colitis are quite variable and dependent on the cause of the given colitis and factors that modify its course and severity.[2]
Common symptoms of colitis may include: mild to severe abdominal pains and tenderness (depending on the stage of the disease), persistent hemorrhagic diarrhea with pus either present or absent in the stools, fecal incontinence, flatulence, fatigue, loss of appetite and unexplained weight loss.[3]
More severe symptoms may include: shortness of breath, a fast or irregular heartbeat and fever.[3]
Other less common or rare non-specific symptoms that may accompany colitis include: arthritis, mouth ulcers, painful, red and swollen skin and irritated, bloodshot eyes.[3]
Signs seen on colonoscopy include: colonic mucosal erythema (redness of the colon's inner surface), ulcerations and hemorrhage.[4]
Diagnosis
[edit]Symptoms suggestive of colitis are worked-up by obtaining the medical history, a physical examination and laboratory tests (CBC, electrolytes, stool culture and sensitivity, stool ova and parasites et cetera). Additional tests may include medical imaging (e.g. abdominal computed tomography, abdominal X-rays) and an examination with a camera inserted into the rectum (sigmoidoscopy, colonoscopy).[5]
An important investigation in the assessment of colitis is biopsy for histopathology. A very small piece of tissue (usually about 2mm) is removed from the bowel mucosa during endoscopy and examined under the microscope by a histopathologist. A biopsy report generally does not state the diagnosis, but should state any presence of chronic colitis, give an indication of disease activity, as well as state the presence of any epithelial damage (erosions and ulcerations).[6]
Histopathology findings generally associated with chronic colitis include:[6]
-
Crypt degeneration
-
Crypt branching and other architectural distortions
-
Paneth cell (pictured) or gastric metaplasia (only applies in the left colon and rectum)
Other findings include basal plasmacytosis and mucin depletion.[6] Histopathology findings generally associated with active colitis include:[6]
-
Neutrophilic cryptitis (neutrophils within crypt epithelium)
-
Crypt abscesses (luminal neutrophilic aggregates)
-
Gland destruction
-
Ulceration (seen here as absence of epithelium, and granulation tissue with many fibroblasts)
Types
[edit]There are many types of colitis. They are usually classified by the cause.
Types of colitis include:
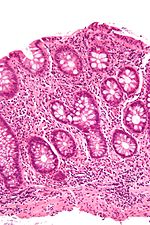
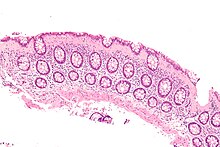
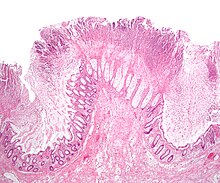
Autoimmune
[edit]- Inflammatory bowel disease (IBD) – a group of chronic colitides.
- Ulcerative colitis (UC) – a chronic colitis that affects the large intestine.[7]
- Crohn's disease (CD) – another type of IBD that often leads to colitis.
Unknown
[edit]- Microscopic colitis – a colitis diagnosed by microscopic examination of colonic tissue; macroscopically ("to the eye") it appears normal.
Treatment-caused
[edit]- Diversion colitis
- Chemical colitis
- Chemotherapy-induced colitis
- Radiation colitis
- Checkpoint inhibitor induced colitis
Vascular disease
[edit]Infectious
[edit]
- Infectious colitis
A subtype of infectious colitis is Clostridioides difficile colitis,[8] which is informally abbreviated as "C-diff colitis". It classically forms pseudomembranes and is often referred to as pseudomembranous colitis, which is its (nonspecific) histomorphologic description.
Enterohemorrhagic colitis may be caused by Shiga toxin in Shigella dysenteriae or Shigatoxigenic group of Escherichia coli (STEC), which includes serotype O157:H7 and other enterohemorrhagic E. coli.[9]
Parasitic infections, like those caused by Entamoeba histolytica, can also cause colitis.
Unclassifiable colitides
[edit]Indeterminate colitis is the classification for colitis that has features of both Crohn's disease and ulcerative colitis.[10] Indeterminate colitis' behaviour is usually closer to ulcerative colitis than Crohn's disease.[11]
Treatment
[edit]Treatment for this condition can include medications such as steroids and dietary changes. In some instances, hospitalization and surgery may be required.[12]
Moreover, several studies recently have found significant relationship between colitis and dairy allergy (including: cow milk, cow milk UHT and casein),[13][14][15] suggesting some patients may benefit from an elimination diet.
Microbiome modification
[edit]The use of oral probiotic supplements to modify the composition and behavior of the microbiome has been considered as a possible therapy for both induction and maintenance of remission in people with Crohn's disease and ulcerative colitis. A Cochrane review in 2020 did not find clear evidence of improved remission likelihood, nor lower adverse events, in people with Crohn's disease, following probiotic treatment.[16]
For ulcerative colitis, there is low-certainty evidence that probiotic supplements may increase the probability of clinical remission.[17] People receiving probiotics were 73% more likely to experience disease remission and over 2x as likely to report improvement in symptoms compared to those receiving a placebo, with no clear difference in minor or serious adverse effects.[17] Although there was no clear evidence of greater remission when probiotic supplements were compared with 5‐aminosalicylic acid treatment as a monotherapy, the likelihood of remission was 22% higher if probiotics were used in combination with 5-aminosalicylic acid therapy.[17] Whereas in people who are already in remission, it is unclear whether probiotics help to prevent future relapse, either as a monotherapy or combination therapy.[18]
Research
[edit]One study reported successfully treating experimental colitis in mice with mesenchymal stem cells.[19]
Additional research was conducted by Huang et al. that analyzed specific genes and biological markers that are associated with the risk of colon cancer development in patients with colitis. The results showed a correlation between certain biomarkers and the development of disease.[20]
Colitis is common in parts of the world where helminthic colonisation is rare, and uncommon in those areas where most people carry worms. Infections with helminths may alter the autoimmune response that causes the disease. Early trials of Trichuris suis ova (TSO) showed promising results when used in people with IBD[21][22][23][24] but later trials failed at Phase 2, and most were eventually discontinued.[25] However, the phase 2 trials had used a different formulation of TSO from the one that had been used in the earlier studies that had shown positive outcomes.[26]
References
[edit]- ^ "Colitis". www.pennmedicine.org. July 1, 2021. Retrieved 2022-11-18.
- ^ "Ulcerative colitis - Symptoms and causes". Mayo Clinic. Retrieved 2024-04-11.
- ^ a b c NHS Choices. "Ulcerative colitis - Symptoms - NHS Choices". www.nhs.uk. Retrieved 2015-11-03.
- ^ "Colonoscopy for ulcerative colitis: Why to get one, prep, and more". 30 July 2021.
- ^ "Diagnosis of Ulcerative Colitis | NIDDK". National Institute of Diabetes and Digestive and Kidney Diseases. Retrieved 2022-11-18.
- ^ a b c d Kellermann L, Riis LB. (2021). "A close view on histopathological changes in inflammatory bowel disease, a narrative review". Dig Med Res. 4 (3): 3. doi:10.21037/dmr-21-1.
- ^ Elghobashy M, Steed H (2024). "Ulcerative colitis". Medicine. 52 (4): 232–237. doi:10.1016/j.mpmed.2024.01.001. ISSN 1357-3039.
- ^ "Clostridium Difficile Colitis – Overview". WebMD, LLC. Retrieved 2006-09-15.
- ^ Beutin L (September 2006). "Emerging enterohaemorrhagic Escherichia coli, causes and effects of the rise of a human pathogen". Journal of Veterinary Medicine. B, Infectious Diseases and Veterinary Public Health. 53 (7): 299–305. doi:10.1111/j.1439-0450.2006.00968.x. PMID 16930272.
- ^ Romano C, Famiani A, Gallizzi R, Comito D, Ferrau' V, Rossi P (December 2008). "Indeterminate colitis: a distinctive clinical pattern of inflammatory bowel disease in children". Pediatrics. 122 (6): e1278–e1281. doi:10.1542/peds.2008-2306. PMID 19047226. S2CID 1409823.
- ^ Melton GB, Kiran RP, Fazio VW, He J, Shen B, Goldblum JR, et al. (October 2010). "Do preoperative factors predict subsequent diagnosis of Crohn's disease after ileal pouch-anal anastomosis for ulcerative or indeterminate colitis?". Colorectal Disease. 12 (10): 1026–1032. doi:10.1111/j.1463-1318.2009.02014.x. PMID 19624520. S2CID 44406331.
- ^ "Treatment for Ulcerative Colitis - NIDDK". National Institute of Diabetes and Digestive and Kidney Diseases. Retrieved 2024-04-20.
- ^ Yang M, Geng L, Chen P, Wang F, Xu Z, Liang C, et al. (March 2015). "Effectiveness of dietary allergen exclusion therapy on eosinophilic colitis in Chinese infants and young children ≤ 3 years of age". Nutrients. 7 (3): 1817–1827. doi:10.3390/nu7031817. PMC 4377883. PMID 25768952.
- ^ Lucendo AJ, Serrano-Montalbán B, Arias Á, Redondo O, Tenias JM (July 2015). "Efficacy of Dietary Treatment for Inducing Disease Remission in Eosinophilic Gastroenteritis". Journal of Pediatric Gastroenterology and Nutrition. 61 (1): 56–64. doi:10.1097/MPG.0000000000000766. PMID 25699593. S2CID 26195645.
- ^ Sun J, Lin J, Parashette K, Zhang J, Fan R (February 2015). "Association of lymphocytic colitis and lactase deficiency in pediatric population". Pathology, Research and Practice. 211 (2): 138–144. doi:10.1016/j.prp.2014.11.009. PMID 25523228.
- ^ Limketkai BN, Akobeng AK, Gordon M, Adepoju AA (2020-07-17). Cochrane Gut Group (ed.). "Probiotics for induction of remission in Crohn's disease". Cochrane Database of Systematic Reviews. 2020 (7): CD006634. doi:10.1002/14651858.CD006634.pub3. PMC 7389339. PMID 32678465.
- ^ a b c Kaur L, Gordon M, Baines PA, Iheozor-Ejiofor Z, Sinopoulou V, Akobeng AK (2020-03-04). Cochrane IBD Group (ed.). "Probiotics for induction of remission in ulcerative colitis". Cochrane Database of Systematic Reviews. 3 (3): CD005573. doi:10.1002/14651858.CD005573.pub3. PMC 7059959. PMID 32128795.
- ^ Iheozor-Ejiofor Z, Kaur L, Gordon M, Baines PA, Sinopoulou V, Akobeng AK (2020-03-04). Cochrane IBD Group (ed.). "Probiotics for maintenance of remission in ulcerative colitis". Cochrane Database of Systematic Reviews. 3 (3): CD007443. doi:10.1002/14651858.CD007443.pub3. PMC 7059960. PMID 32128794.
- ^ Yang F, Ni B, Liu Q, He F, Li L, Zhong X, et al. (September 2022). "Human umbilical cord-derived mesenchymal stem cells ameliorate experimental colitis by normalizing the gut microbiota". Stem Cell Research & Therapy. 13 (1): 475. doi:10.1186/s13287-022-03118-1. PMC 9476645. PMID 36104756.
- ^ Huang Y, Zhang X, Li Y, Yao J (June 2022). "Identification of hub genes and pathways in colitis-associated colon cancer by integrated bioinformatic analysis". BMC Genomic Data. 23 (1): 48. doi:10.1186/s12863-022-01065-7. PMC 9219145. PMID 35733095.
- ^ Summers RW, Elliott DE, Urban JF, Thompson RA, Weinstock JV (2005). "Trichuris suis therapy for active ulcerative colitis: a randomized controlled trial". Gastroenterology. 128 (4): 825–32. doi:10.1053/j.gastro.2005.01.005. PMID 15825065.
- ^ Pommerville J (2014). Fundamentals of microbiology. Burlington, MA: Jones & Bartlett Learning. ISBN 978-1-4496-8861-5.
- ^ Elliott DE, Weinstock JV (November 2012). "Where are we on worms?". Current Opinion in Gastroenterology. 28 (6): 551–6. doi:10.1097/MOG.0b013e3283572f73. PMC 3744105. PMID 23079675.
- ^ Weinstock JV, Elliott DE (March 2013). "Translatability of helminth therapy in inflammatory bowel diseases". International Journal for Parasitology. 43 (3–4): 245–51. doi:10.1016/j.ijpara.2012.10.016. PMC 3683647. PMID 23178819.
Early clinical trials suggested that exposure to helminths such as Trichuris suis or Necator americanus can improve IBD.
- ^ Coronado Biosciences (November 7, 2013). "Coronado Biosciences Announces Independent Data Monitoring Committee Recommendation to Discontinue Falk Phase 2 Trial of TSO in Crohn's Disease". Archived from the original on August 16, 2016. Retrieved August 16, 2016.
- ^ Parker W (December 2017). "Not infection with parasitic worms, but rather colonization with therapeutic helminths". Immunology Letters. 196: 104–105. doi:10.1016/j.imlet.2017.07.008. PMID 28720335.






