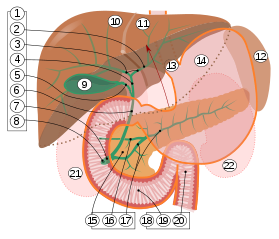
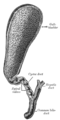
Anatomy
The cystic duct typically[2] measures (sources differ) 2–4 cm[3][4]/2–3 cm[2] in length (though its lengh has been known to range from 0.5 cm to 9 cm[3]), and 2–3 mm in diameter.[2][4] It is often tortuous.[3][4]
It is the distal continuation of the neck of the gallbladder, from where it is directed inferoposteriorly and to the left[2]/medially[4] (this occurs in half of individuals[3]). It typically[2] terminates by uniting with the common hepatic duct to form the bile duct (usually anterior to the right hepatic artery).[2] It usually joins the common bile duct from the right lateral side (forming an oblique angle between the two),[4] and at such a distance that the bile duct is twice as long as the common hepatic duct.[3][4] It often fuses with the common hepatic duct before actually opening into it after a variable distance[4][3] (this arrangement may have the purpose of directing bile flow distally instead of back towards the liver[3]).
Structure
The inner surface of the cystic duct features spiral, crescentic mucosal folds - the spiral folds of cystic duct.[4][3]
The inner surface of the proximal cystic duct exhibits a network of submicroscopic convoluted folds (rugae), whereas that of the distal cystic duct exhibits submicroscopic parallel longitudinal folds.[3]
Histology
The epithelial lining of the inner surface of the duct is similar to that of the gallbladder and consists mostly of columnar epithelial cells with short microvilli upon their apical surfaces.[3]
The subepithelial layer consists of elastic connective tissue and is highly vascular; vessels that are adjacent to the epithelial basement membrane are fenestrated, possibly to facilitate ion and fluid exchange with the bile as is the case in the gallbladder itself.[3]
The outer fibromuscular layer contains smooth muscle continuous with that of the gallbladder; some of the smooth muscle extends into the spiral valves.[3]
Relations
It usually lies next to the cystic artery.[citation needed]
Variation
The cystic duct may rarely be doubled.[2][3]
An accessory hepatic duct may join the cystic duct.[2][4]
A pathological diverticulum known as the Hartmann’s pouch may be present at the junction of the neck of bladder and the cystic duct.[2]
Length
The duct may sometimes be extremely short (making cholecystectomy risky)[2] or may rarely be altogether absent (so that the gallbladder is directly attached to the bile duct).[2][4][3]
Shape
While most often tortuous, it may occasionally be curved, straight, or S-shaped.[3]
Termination
The cystic duct may unite with the common hepatic duct so that the common hepatic duct is either very short or very long (and the bile duct in turn very long or very short, respectively),[4] or it may instead unite with the a hepatic duct.[3]
Occasionally, the cystic duct may first run alongside the common hepatic duct for some distance[2][4] within the hepatoduodenal ligament[4] before joining it.[2][4] It sometimes join the common hepatic duct at its anterior, posterior, or medial side[4][3] (in the latter case by passing posteriorly around the common bile duct to join it from the other side).[2] It may spiral around the common hepatic duct before joining it.[4]
Very rarely, the cystic duct opens into the duodenum.[3]
Function
Bile can flow in either direction between the gallbladder, and the common bile duct and hepatic duct.[3] In this way, bile is stored in the gallbladder in between meal times. The hormone cholecystokinin, when stimulated by a fatty meal, promotes bile secretion by increased production of hepatic bile, contraction of the gall bladder, and relaxation of the Sphincter of Oddi.
The bile duct was once thought to possess a sphincteric function, however, it is now known that bile flow through the cystic duct proceeds unimpeded and is instead regulated by other mechanisms at other points of the biliary system.[3]
Clinical significance
Gallstones can enter and obstruct the cystic duct, preventing the flow of bile. The increased pressure in the gallbladder leads to swelling and pain. This pain, known as biliary colic, is sometimes referred to as a gallbladder "attack" because of its sudden onset.
During a cholecystectomy, the cystic duct is clipped two or three times and a cut is made between the clips, freeing the gallbladder to be taken out.