Serological tests
Serological tests are diagnostic methods that are used to identify antibodies and antigens in a patient's sample. Serological tests may be performed to diagnose infections and autoimmune illnesses, to check if a person has immunity to certain diseases, and in many other situations, such as determining an individual's blood type.[1] Serological tests may also be used in forensic serology to investigate crime scene evidence.[3] Several methods can be used to detect antibodies and antigens, including ELISA,[4] agglutination, precipitation, complement-fixation, and fluorescent antibodies and more recently chemiluminescence.[5]
Applications
Microbiology

In microbiology, serologic tests are used to determine if a person has antibodies against a specific pathogen, or to detect antigens associated with a pathogen in a person's sample.[6] Serologic tests are especially useful for organisms that are difficult to culture by routine laboratory methods, like Treponema pallidum (the causative agent of syphilis), or viruses.[7]
The presence of antibodies against a pathogen in a person's blood indicates that they have been exposed to that pathogen. Most serologic tests measure one of two types of antibodies: immunoglobulin M (IgM) and immunoglobulin G (IgG). IgM is produced in high quantities shortly after a person is exposed to the pathogen, and production declines quickly thereafter. IgG is also produced on the first exposure, but not as quickly as IgM. On subsequent exposures, the antibodies produced are primarily IgG, and they remain in circulation for a prolonged period of time.[6]
This affects the interpretation of serology results: a positive result for IgM suggests that a person is currently or recently infected, while a positive result for IgG and negative result for IgM suggests that the person may have been infected or immunized in the past. Antibody testing for infectious diseases is often done in two phases: during the initial illness (acute phase) and after recovery (convalescent phase). The amount of antibody in each specimen (antibody titer) is compared, and a significantly higher amount of IgG in the convalescent specimen suggests infection as opposed to previous exposure.[8] False negative results for antibody testing can occur in people who are immunosuppressed, as they produce lower amounts of antibodies, and in people who receive antimicrobial drugs early in the course of the infection.[7]
Transfusion medicine

Blood typing is typically performed using serologic methods. The antigens on a person's red blood cells, which determine their blood type, are identified using reagents that contain antibodies, called antisera. When the antibodies bind to red blood cells that express the corresponding antigen, they cause red blood cells to clump together (agglutinate), which can be identified visually. The person's blood group antibodies can also be identified by adding plasma to cells that express the corresponding antigen and observing the agglutination reactions.[9][6]
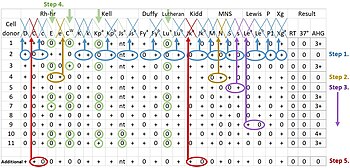
Other serologic methods used in transfusion medicine include crossmatching and the direct and indirect antiglobulin tests. Crossmatching is performed before a blood transfusion to ensure that the donor blood is compatible. It involves adding the recipient's plasma to the donor blood cells and observing for agglutination reactions.[9] The direct antiglobulin test is performed to detect if antibodies are bound to red blood cells inside the person's body, which is abnormal and can occur in conditions like autoimmune hemolytic anemia, hemolytic disease of the newborn and transfusion reactions.[10] The indirect antiglobulin test is used to screen for antibodies that could cause transfusion reactions and identify certain blood group antigens.[11]
Immunology
Serologic tests can help to diagnose autoimmune disorders by identifying abnormal antibodies directed against a person's own tissues (autoantibodies).[12] All people have different immunology graphs.[citation needed]