| COVID-19 pandemic | |||||||
|---|---|---|---|---|---|---|---|
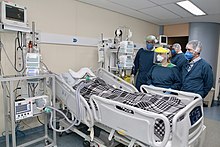
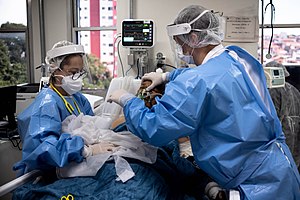 Medical professionals treating a COVID-19 patient in critical condition in an intensive care unit in São Paulo in May 2020 | |||||||
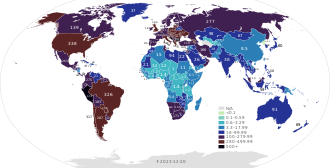 Confirmed deaths per 100,000 population
as of 20 December 2023 | |||||||
| |||||||
| Disease | Coronavirus disease 2019 (COVID-19) | ||||||
| Virus strain | Severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2) | ||||||
| Source | Bats,[1] indirectly[2] | ||||||
| Location | Worldwide | ||||||
| Index case | Wuhan, China 30°37′11″N 114°15′28″E / 30.61972°N 114.25778°E | ||||||
| Dates | Assessed by WHO as pandemic: 11 March 2020 (4 years and 4 months ago)[3]
Public health emergency of international concern: 30 January 2020 – 5 May 2023 (3 years, 3 months and 5 days)[4] | ||||||
| Confirmed cases | 775,673,955[5] (true case count is expected to be much higher[6]) | ||||||
Deaths | 7,053,524[5] (reported) 18.2–33.5 million[7] (estimated) | ||||||
| Fatality rate | As of 10 March 2023: 1.02%[8][needs update] | ||||||
| Part of a series on the |
| COVID-19 pandemic |
|---|
 |
|
|
|
The COVID-19 pandemic (also known as the coronavirus pandemic), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), began with an outbreak of COVID-19 in Wuhan, China, in December 2019. It spread to other areas of Asia, and then worldwide in early 2020. The World Health Organization (WHO) declared the outbreak a public health emergency of international concern (PHEIC) on 30 January 2020, and assessed the outbreak had become a pandemic on 11 March.[3]
COVID-19 symptoms range from asymptomatic to deadly, but most commonly include fever, sore throat, nocturnal cough, and fatigue. Transmission of the virus is often through airborne particles. Mutations have produced many strains (variants) with varying degrees of infectivity and virulence.[9] COVID-19 vaccines were developed rapidly and deployed to the general public beginning in December 2020, made available through government and international programs such as COVAX, aiming to provide vaccine equity. Treatments include novel antiviral drugs and symptom control. Common mitigation measures during the public health emergency included travel restrictions, lockdowns, business restrictions and closures, workplace hazard controls, mask mandates, quarantines, testing systems, and contact tracing of the infected.
The pandemic caused severe social and economic disruption around the world, including the largest global recession since the Great Depression.[10] Widespread supply shortages, including food shortages, were caused by supply chain disruptions and panic buying. Reduced human activity led to an unprecedented temporary decrease in pollution. Educational institutions and public areas were partially or fully closed in many jurisdictions, and many events were cancelled or postponed during 2020 and 2021. Telework became much more common for white-collar workers as the pandemic evolved. Misinformation circulated through social media and mass media, and political tensions intensified. The pandemic raised issues of racial and geographic discrimination, health equity, and the balance between public health imperatives and individual rights.
The WHO ended the PHEIC for COVID-19 on 5 May 2023.[4] The disease has continued to circulate, but as of 2024, experts were uncertain as to whether it was still a pandemic.[11][12] Pandemics and their ends are not well-defined, and whether or not one has ended differs according to the definition used.[11][13] As of 26 July 2024, COVID-19 has caused 7,053,524[5] confirmed deaths. The COVID-19 pandemic ranks as the fifth-deadliest pandemic or epidemic in history.
Terminology

Pandemic
In epidemiology, a pandemic is defined as "an epidemic occurring over a very wide area, crossing international boundaries, and usually affecting a large number of people". During the COVID-19 pandemic, as with other pandemics, the meaning of this term has been challenged.[14]
The end of a pandemic or other epidemic only rarely involves the total disappearance of a disease, and historically, much less attention has been given to defining the ends of epidemics than their beginnings. The ends of particular epidemics have been defined in a variety of ways, differing according to academic field, and differently based on location and social group. An epidemic's end can be considered a social phenomenon, not just a biological one.[13] This means that it is possible for the pandemic to have ended according to one definition (e.g., according to a definition based on how people behave) and still be ongoing according to another definition (e.g., according to a definition based on the number of infections).
Virus names
During the initial outbreak in Wuhan, the virus and disease were commonly referred to as "coronavirus", "Wuhan coronavirus",[15] "the coronavirus outbreak" and the "Wuhan coronavirus outbreak",[16] with the disease sometimes called "Wuhan pneumonia".[17][18] In January 2020, the WHO recommended 2019-nCoV[19] and 2019-nCoV acute respiratory disease[20] as interim names for the virus and disease per 2015 international guidelines against using geographical locations (e.g. Wuhan, China), animal species, or groups of people in disease and virus names in part to prevent social stigma.[21] WHO finalized the official names COVID-19 and SARS-CoV-2 on 11 February 2020.[22] Tedros Adhanom Ghebreyesus explained: CO for corona, VI for virus, D for disease and 19 for when the outbreak was first identified (31 December 2019).[23] WHO additionally uses "the COVID-19 virus" and "the virus responsible for COVID-19" in public communications.[22]
WHO named variants of concern and variants of interest using Greek letters. The initial practice of naming them according to where the variants were identified (e.g. Delta began as the "Indian variant") is no longer common.[24] A more systematic naming scheme reflects the variant's PANGO lineage (e.g., Omicron's lineage is B.1.1.529) and is used for other variants.[25][26][27]
Epidemiology
| For country-level data, see: | |
 | |
|
As of 26 July 2024
|
Background
SARS-CoV-2 is a virus closely related to bat coronaviruses,[28] pangolin coronaviruses,[29][30] and SARS-CoV.[31] The first known outbreak (the 2019–2020 COVID-19 outbreak in mainland China) started in Wuhan, Hubei, China, in December 2019.[32] Many early cases were linked to people who had visited the Huanan Seafood Wholesale Market there,[33][34][35] but it is possible that human-to-human transmission began earlier.[36][37] Molecular clock analysis suggests that the first cases were likely to have been between October and November 2019.[38]
The scientific consensus is that the virus is most likely of a zoonotic origin, from bats or another closely related mammal.[36][39][40] While other explanations such as speculations that SARS-CoV-2 was accidentally released from a laboratory have been proposed,[41][42][43] as of 2021 these were not supported by evidence.[44]
Cases
Official "case" counts refer to the number of people who have been tested for COVID-19 and whose test has been confirmed positive according to official protocols whether or not they experienced symptomatic disease.[45][46] Due to the effect of sampling bias, studies which obtain a more accurate number by extrapolating from a random sample have consistently found that total infections considerably exceed the reported case counts.[47][48] Many countries, early on, had official policies to not test those with only mild symptoms.[49][50] The strongest risk factors for severe illness are obesity, complications of diabetes, anxiety disorders, and the total number of conditions.[51]
During the start of the COVID-19 pandemic it was not clear whether young people were less likely to be infected, or less likely to develop symptoms and be tested.[52] A retrospective cohort study in China found that children and adults were just as likely to be infected.[53]
Among more thorough studies, preliminary results from 9 April 2020 found that in Gangelt, the centre of a major infection cluster in Germany, 15 percent of a population sample tested positive for antibodies.[54] Screening for COVID-19 in pregnant women in New York City, and blood donors in the Netherlands, found rates of positive antibody tests that indicated more infections than reported.[55][56] Seroprevalence-based estimates are conservative as some studies show that persons with mild symptoms do not have detectable antibodies.[57]
Initial estimates of the basic reproduction number (R0) for COVID-19 in January 2020 were between 1.4 and 2.5,[58] but a subsequent analysis claimed that it may be about 5.7 (with a 95 percent confidence interval of 3.8 to 8.9).[59]
In December 2021, the number of cases continued to climb due to several factors, including new COVID-19 variants. As of that 28 December, 282,790,822 individuals worldwide had been confirmed as infected.[60] As of 14 April 2022[update], over 500 million cases were confirmed globally.[61] Most cases are unconfirmed, with the Institute for Health Metrics and Evaluation estimating the true number of cases as of early 2022 to be in the billions.[62][63]

Deaths



As of 10 March 2023, more than 6.88 million[8] deaths had been attributed to COVID-19. The first confirmed death was in Wuhan on 9 January 2020.[65] These numbers vary by region and over time, influenced by testing volume, healthcare system quality, treatment options, government response,[66] time since the initial outbreak, and population characteristics, such as age, sex, and overall health.[67]
Multiple measures are used to quantify mortality.[68] Official death counts typically include people who died after testing positive. Such counts exclude deaths without a test.[69] Conversely, deaths of people who died from underlying conditions following a positive test may be included.[70] Countries such as Belgium include deaths from suspected cases, including those without a test, thereby increasing counts.[71]
Official death counts have been claimed to underreport the actual death toll, because excess mortality (the number of deaths in a period compared to a long-term average) data show an increase in deaths that is not explained by COVID-19 deaths alone.[72] Using such data, estimates of the true number of deaths from COVID-19 worldwide have included a range from 18.2 to 33.5 million (≈27.4 million) by 18 November 2023 by The Economist,[7][72] as well as over 18.5 million by 1 April 2023 by the Institute for Health Metrics and Evaluation[73] and ≈18.2 million (earlier) deaths between 1 January 2020, and 31 December 2021, by a comprehensive international study.[74] Such deaths include deaths due to healthcare capacity constraints and priorities, as well as reluctance to seek care (to avoid possible infection).[75] Further research may help distinguish the proportions directly caused by COVID-19 from those caused by indirect consequences of the pandemic.[74]
In May 2022, the WHO estimated the number of excess deaths by the end of 2021 to be 14.9 million compared to 5.4 million reported COVID-19 deaths, with the majority of the unreported 9.5 million deaths believed to be direct deaths due the virus, rather than indirect deaths. Some deaths were because people with other conditions could not access medical services.[76][77]
A December 2022 WHO study estimated excess deaths from the pandemic during 2020 and 2021, again concluding ≈14.8 million excess early deaths occurred, reaffirming and detailing their prior calculations from May as well as updating them, addressing criticisms. These numbers do not include measures like years of potential life lost and may make the pandemic 2021's leading cause of death.[78][79][64]
The time between symptom onset and death ranges from 6 to 41 days, typically about 14 days.[80] Mortality rates increase as a function of age. People at the greatest mortality risk are the elderly and those with underlying conditions.[81][82]
-
Semi-log plot of weekly deaths due to COVID-19 in the world and top six current countries (mean with cases)
-
Excess deaths relative to expected deaths (The patterns indicate the quality of the all-cause mortality data that were available for each respective country.)[64]
-
Excess deaths relative to expected deaths (global and WHO region)[64]
-
The 25 countries with the highest total estimated COVID-19 pandemic excess deaths between January 2020 and December 2021[64]
-
The 25 countries with the highest mean P-scores (excess deaths relative to expected deaths)[64]
Infection fatality ratio (IFR)
| Age group | IFR |
|---|---|
| 0–34 | 0.004% |
| 35–44 | 0.068% |
| 45–54 | 0.23% |
| 55–64 | 0.75% |
| 65–74 | 2.5% |
| 75–84 | 8.5% |
| 85 + | 28.3% |
The infection fatality ratio (IFR) is the cumulative number of deaths attributed to the disease divided by the cumulative number of infected individuals (including asymptomatic and undiagnosed infections and excluding vaccinated infected individuals).[84][85][86] It is expressed in percentage points.[87] Other studies refer to this metric as the infection fatality risk.[88][89]
In November 2020, a review article in Nature reported estimates of population-weighted IFRs for various countries, excluding deaths in elderly care facilities, and found a median range of 0.24% to 1.49%.[90] IFRs rise as a function of age (from 0.002% at age 10 and 0.01% at age 25, to 0.4% at age 55, 1.4% at age 65, 4.6% at age 75, and 15% at age 85). These rates vary by a factor of ≈10,000 across the age groups.[83] For comparison, the IFR for middle-aged adults is two orders of magnitude higher than the annualised risk of a fatal automobile accident and much higher than the risk of dying from seasonal influenza.[83]
In December 2020, a systematic review and meta-analysis estimated that population-weighted IFR was 0.5% to 1% in some countries (France, Netherlands, New Zealand, and Portugal), 1% to 2% in other countries (Australia, England, Lithuania, and Spain), and about 2.5% in Italy. This study reported that most of the differences reflected corresponding differences in the population's age structure and the age-specific pattern of infections.[83] There have also been reviews that have compared the fatality rate of this pandemic with prior pandemics, such as MERS-CoV.[91]
For comparison the infection mortality rate of seasonal flu in the United States is 0.1%, which is 13 times lower than COVID-19.[92]
Case fatality ratio (CFR)
Another metric in assessing death rate is the case fatality ratio (CFR),[a] which is the ratio of deaths to diagnoses. This metric can be misleading because of the delay between symptom onset and death and because testing focuses on symptomatic individuals.[93]
Based on Johns Hopkins University statistics, the global CFR is 1.02 percent (6,881,955 deaths for 676,609,955 cases) as of 10 March 2023.[8] The number varies by region and has generally declined over time.[94]
Disease
Variants
Several variants have been named by WHO and labelled as a variant of concern (VoC) or a variant of interest (VoI). Many of these variants have shared the more infectious D614G. As of May 2023, the WHO had downgraded all variants of concern to previously circulating as these were no longer detected in new infections.[95][96] Sub-lineages of the Omicron variant (BA.1 – BA.5) were considered separate VoCs by the WHO until they were downgraded in March 2023 as no longer widely circulating.[96]
| Name | Lineage | Detected | Countries | Priority |
|---|---|---|---|---|
| Alpha | B.1.1.7 | UK | 190 | VoC |
| Beta | B.1.351 | South Africa | 140 | VoC |
| Delta | B.1.617.2 | India | 170 | VoC |
| Gamma | P.1 | Brazil | 90 | VoC |
| Omicron | B.1.1.529 | Botswana | 149 | VoC |
Signs and symptoms

Symptoms of COVID-19 are variable, ranging from mild symptoms to severe illness.[99][100] Common symptoms include headache, loss of smell and taste, nasal congestion and runny nose, cough, muscle pain, sore throat, fever, diarrhoea, and breathing difficulties.[99] People with the same infection may have different symptoms, and their symptoms may change over time. Three common clusters of symptoms have been identified: one respiratory symptom cluster with cough, sputum, shortness of breath, and fever; a musculoskeletal symptom cluster with muscle and joint pain, headache, and fatigue; a cluster of digestive symptoms with abdominal pain, vomiting, and diarrhoea.[101] In people without prior ear, nose, and throat disorders, loss of taste combined with loss of smell is associated with COVID-19 and is reported in as many as 88% of cases.[102][103][104]
Transmission
The disease is mainly transmitted via the respiratory route when people inhale droplets and small airborne particles (that form an aerosol) that infected people exhale as they breathe, talk, cough, sneeze, or sing.[105][106][107][108] Infected people are more likely to transmit COVID-19 when they are physically close to other non-infected individuals. However, infection can occur over longer distances, particularly indoors.[105][109]
Cause

SARS‑CoV‑2 belongs to the broad family of viruses known as coronaviruses.[110] It is a positive-sense single-stranded RNA (+ssRNA) virus, with a single linear RNA segment. Coronaviruses infect humans, other mammals, including livestock and companion animals, and avian species.[111]
Human coronaviruses are capable of causing illnesses ranging from the common cold to more severe diseases such as Middle East respiratory syndrome (MERS, fatality rate ≈34%). SARS-CoV-2 is the seventh known coronavirus to infect people, after 229E, NL63, OC43, HKU1, MERS-CoV, and the original SARS-CoV.[112]
Diagnosis

The standard method of testing for presence of SARS-CoV-2 is a nucleic acid test,[113] which detects the presence of viral RNA fragments.[114] As these tests detect RNA but not infectious virus, its "ability to determine duration of infectivity of patients is limited."[115] The test is typically done on respiratory samples obtained by a nasopharyngeal swab; however, a nasal swab or sputum sample may also be used.[116][117] The WHO has published several testing protocols for the disease.[118]
Prevention

Preventive measures to reduce the chances of infection include getting vaccinated, staying at home or spending more time outdoors, avoiding crowded places, keeping distance from others, wearing a mask in public, ventilating indoor spaces, managing potential exposure durations, washing hands with soap and water often and for at least twenty seconds, practicing good respiratory hygiene, and avoiding touching the eyes, nose, or mouth with unwashed hands.[119][120]
Those diagnosed with COVID-19 or who believe they may be infected are advised by healthcare authorities to stay home except to get medical care, call ahead before visiting a healthcare provider, wear a face mask before entering the healthcare provider's office and when in any room or vehicle with another person, cover coughs and sneezes with a tissue, regularly wash hands with soap and water and avoid sharing personal household items.[121][122][123]
Vaccines

A COVID-19 vaccine is intended to provide acquired immunity against severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2), the virus that causes coronavirus disease 2019 (COVID-19). Prior to the COVID-19 pandemic, an established body of knowledge existed about the structure and function of coronaviruses causing diseases like severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS). This knowledge accelerated the development of various vaccine platforms during early 2020.[124] The initial focus of SARS-CoV-2 vaccines was on preventing symptomatic and severe illness.[125] The COVID-19 vaccines are widely credited for their role in reducing the severity and death caused by COVID-19.[126][127]
As of March 2023, more than 5.5 billion people had received one or more doses[128] (11.8 billion in total) in over 197 countries. The Oxford-AstraZeneca vaccine was the most widely used.[129] According to a June 2022 study, COVID-19 vaccines prevented an additional 14.4 million to 19.8 million deaths in 185 countries and territories from 8 December 2020 to 8 December 2021.[130][131]
On 8 November 2022, the first recombinant protein-based COVID-19 vaccine (Novavax's booster Nuvaxovid) was authorized for use in adults in the United Kingdom. It has subsequently received endorsement/authorization from the WHO, US, European Union, and Australia.[132][133]
On 12 November 2022, the WHO released its Global Vaccine Market Report. The report indicated that "inequitable distribution is not unique to COVID-19 vaccines"; countries that are not economically strong struggle to obtain vaccines.[134]
On 14 November 2022, the first inhalable vaccine was introduced, developed by Chinese biopharmaceutical company CanSino Biologics, in the city of Shanghai, China.[135]
Treatment
For the first two years of the pandemic, no specific and effective treatment or cure was available.[136][137] In 2021, the European Medicines Agency's (EMA) Committee for Medicinal Products for Human Use (CHMP) approved the oral antiviral protease inhibitor, Paxlovid (nirmatrelvir plus the HIV antiviral ritonavir), to treat adult patients.[138] FDA later gave it an EUA.[139]
Most cases of COVID-19 are mild. In these, supportive care includes medication such as paracetamol or NSAIDs to relieve symptoms (fever,[140] body aches, cough), adequate intake of oral fluids and rest.[137][141] Good personal hygiene and a healthy diet are also recommended.[142]
Supportive care in severe cases includes treatment to relieve symptoms, fluid therapy, oxygen support and prone positioning, and medications or devices to support other affected vital organs.[143] More severe cases may need treatment in hospital. In those with low oxygen levels, use of the glucocorticoid dexamethasone is recommended to reduce mortality.[144] Noninvasive ventilation and, ultimately, admission to an intensive care unit for mechanical ventilation may be required to support breathing.[145] Extracorporeal membrane oxygenation (ECMO) has been used to address the issue of respiratory failure.[146][147]
Existing drugs such as hydroxychloroquine, lopinavir/ritonavir, and ivermectin are not recommended by US or European health authorities, as there is no good evidence they have any useful effect.[136][148][149] The antiviral remdesivir is available in the US, Canada, Australia, and several other countries, with varying restrictions; however, it is not recommended for use with mechanical ventilation, and is discouraged altogether by the World Health Organization (WHO),[150] due to limited evidence of its efficacy.[136]
Prognosis
The severity of COVID-19 varies. It may take a mild course with few or no symptoms, resembling other common upper respiratory diseases such as the common cold. In 3–4% of cases (7.4% for those over age 65) symptoms are severe enough to cause hospitalization.[151] Mild cases typically recover within two weeks, while those with severe or critical diseases may take three to six weeks to recover. Among those who have died, the time from symptom onset to death has ranged from two to eight weeks. Prolonged prothrombin time and elevated C-reactive protein levels on admission to the hospital are associated with severe course of COVID-19 and with a transfer to intensive care units (ICU).[152][153]
Between 5% and 50% of COVID-19 patients experience long COVID,[154] a condition characterized by long-term consequences persisting after the typical convalescence period of the disease.[155][156] The most commonly reported clinical presentations are fatigue and memory problems, as well as malaise, headaches, shortness of breath, loss of smell, muscle weakness, low fever and cognitive dysfunction.[157][158][159][160]
Strategies

Many countries attempted to slow or stop the spread of COVID-19 by recommending, mandating or prohibiting behaviour changes, while others relied primarily on providing information. Measures ranged from public advisories to stringent lockdowns. Outbreak control strategies are divided into elimination and mitigation. Experts differentiate between elimination strategies (known as "zero-COVID") that aim to completely stop the spread of the virus within the community,[164] and mitigation strategies (commonly known as "flattening the curve") that attempt to lessen the effects of the virus on society, but which still tolerate some level of transmission within the community.[165] These initial strategies can be pursued sequentially or simultaneously during the acquired immunity phase through natural and vaccine-induced immunity.[166]
Nature reported in 2021 that 90 percent of researchers who responded to a survey "think that the coronavirus will become endemic".[167]
Containment
Containment is undertaken to stop an outbreak from spreading into the general population. Infected individuals are isolated while they are infectious. The people they have interacted with are contacted and isolated for long enough to ensure that they are either not infected or no longer contagious. Screening is the starting point for containment. Screening is done by checking for symptoms to identify infected individuals, who can then be isolated or offered treatment.[168] The zero-COVID strategy involves using public health measures such as contact tracing, mass testing, border quarantine, lockdowns, and mitigation software to stop community transmission of COVID-19 as soon as it is detected, with the goal of getting the area back to zero detected infections and resuming normal economic and social activities.[164][169] Successful containment or suppression reduces Rt to less than 1.[170]
Mitigation
Should containment fail, efforts focus on mitigation: measures taken to slow the spread and limit its effects on the healthcare system and society. Successful mitigation delays and decreases the epidemic peak, known as "flattening the epidemic curve".[161] This decreases the risk of overwhelming health services and provides more time for developing vaccines and treatments.[161] Individual behaviour changed in many jurisdictions. Many people worked from home instead of at their traditional workplaces.[171]
Non-pharmaceutical interventions

Non-pharmaceutical interventions that may reduce spread include personal actions such as wearing face masks, self-quarantine, and hand hygiene; community measures aimed at reducing interpersonal contacts such as closing workplaces and schools and cancelling large gatherings; community engagement to encourage acceptance and participation in such interventions; as well as environmental measures such as surface cleaning.[172]
Other measures
More drastic actions, such as quarantining entire populations and strict travel bans have been attempted in various jurisdictions.[173] The Chinese and Australian government approaches have included many lockdowns and are widely considered the most strict. The New Zealand government response included the most severe travel restrictions. As part of its K-Quarantine program, South Korea introduced mass screening and localised quarantines, and issued alerts on the movements of infected individuals. The Singaporean government's response included so-called "circuit breaker lockdowns" and financial support for those affected while also imposing large fines for those who broke quarantine.[174]
Contact tracing
Contact tracing attempts to identify recent contacts of newly infected individuals, and to screen them for infection; the traditional approach is to request a list of contacts from infectees, and then telephone or visit the contacts.[175] Contact tracing was widely used during the Western African Ebola virus epidemic in 2014.[176]
Another approach is to collect location data from mobile devices to identify those who have come in significant contact with infectees, which prompted privacy concerns.[177] On 10 April 2020, Google and Apple announced an initiative for privacy-preserving contact tracing.[178][179] In Europe and in the US, Palantir Technologies initially provided COVID-19 tracking services.[180]
Health care
WHO described increasing capacity and adapting healthcare as a fundamental mitigation.[181] The ECDC and WHO's European regional office issued guidelines for hospitals and primary healthcare services for shifting resources at multiple levels, including focusing laboratory services towards testing, cancelling elective procedures, separating and isolating patients, and increasing intensive care capabilities by training personnel and increasing ventilators and beds.[181][182] The pandemic drove widespread adoption of telehealth.[183]
Improvised manufacturing

Due to supply chain capacity limitations, some manufacturers began 3D printing material such as nasal swabs and ventilator parts.[184][185] In one example, an Italian startup received legal threats due to alleged patent infringement after reverse-engineering and printing one hundred requested ventilator valves overnight.[186] Individuals and groups of makers created and shared open source designs, and manufacturing devices using locally sourced materials, sewing, and 3D printing. Millions of face shields, protective gowns, and masks were made. Other ad hoc medical supplies included shoe covers, surgical caps, powered air-purifying respirators, and hand sanitizer. Novel devices were created such as ear savers, non-invasive ventilation helmets, and ventilator splitters.[187]
Herd immunity
In July 2021, several experts expressed concern that achieving herd immunity may not be possible because Delta can transmit among vaccinated individuals.[188] CDC published data showing that vaccinated people could transmit Delta, something officials believed was less likely with other variants. Consequently, WHO and CDC encouraged vaccinated people to continue with non-pharmaceutical interventions such as masking, social distancing, and quarantining if exposed.[189]
History
2019
The outbreak was discovered in Wuhan in November 2019. It is possible that human-to-human transmission was happening before the discovery.[36][37] Based on a retrospective analysis starting from December 2019, the number of cases in Hubei gradually increased, reaching 60 by 20 December and at least 266 by 31 December.[190]
A pneumonia cluster was observed on 26 December and treated by Chinese pulmonologist Zhang Jixian. She informed the Wuhan Jianghan CDC on 27 December.[191] After analyzing pneumonia patient samples, a genetic sequencing company named Vision Medicals reported the discovery of a novel coronavirus to the China CDC (CCDC) on 28 December.[192][193]
On 30 December, a test report from CapitalBio Medlab addressed to Wuhan Central Hospital reported an erroneous positive result for SARS, causing doctors there to alert authorities. Eight of those doctors, including Li Wenliang (who was also punished on 3 January), were later admonished by the police for spreading false rumours. Director of the Emergency Department at the Central Hospital of Wuhan, Ai Fen, was also reprimanded.[194][195] That evening, Wuhan Municipal Health Commission (WMHC) issued a notice about "the treatment of pneumonia of unknown cause".[196] The next day, WMHC made the announcement public, confirming 27 cases[197][198]—enough to trigger an investigation.[199]
On 31 December, the WHO office in China was notified about the cluster of unknown pneumonia cases[200][197] and immediately launched an investigation.[199]
Official Chinese sources claimed that the early cases were mostly linked to the Huanan Seafood Wholesale Market, which also sold live animals.[201] In May 2020, CCDC director George Gao initially ruled out the market as a possible origin, as animal samples collected there had tested negative.[202]
2020

On 11 January, WHO was notified by the Chinese National Health Commission that the outbreak was associated with exposures in the market, and that China had identified a new type of coronavirus, which it isolated on 7 January.[200]
Initially, the number of cases doubled approximately every seven and a half days.[203] In early and mid-January, the virus spread to other Chinese provinces, helped by the Chinese New Year migration. Wuhan was a transport hub and major rail interchange.[204] On 10 January, the virus' genome was shared publicly.[205] A retrospective study published in March found that 6,174 people had reported symptoms by 20 January.[206] A 24 January report indicated human transmission was likely occurring, and recommended personal protective equipment for health workers. It also advocated testing, given the outbreak's "pandemic potential".[207][208] On 31 January, the first published modelling study warned of inevitable "independent self-sustaining outbreaks in major cities globally" and called for "large-scale public health interventions."[209]
On 30 January, 7,818 infections had been confirmed, leading WHO to declare the outbreak a Public Health Emergency of International Concern (PHEIC).[210][211][212] On 11 March, WHO announced its assessment that the situation could be characterized as a pandemic.[3]
By 31 January, Italy indicated its first confirmed infections had occurred, in two tourists from China.[213] On 19 March, Italy overtook China as the country with the most reported deaths.[214] By 26 March, the United States had overtaken China and Italy as the country with the highest number of confirmed infections.[215] Genomic analysis indicated that the majority of New York's confirmed infections came from Europe, rather than directly from Asia.[216] Testing of prior samples revealed a person who was infected in France on 27 December 2019[217][218] and a person in the United States who died from the disease on 6 February.[219]

In October, WHO reported that one in ten people around the world may have been infected, or 780 million people, while only 35 million infections had been confirmed.[220]
On 9 November, Pfizer released trial results for a candidate vaccine, showing a 90 percent effectiveness in preventing infection. That day, Novavax submitted an FDA Fast Track application for their vaccine.[221][222]
On 14 December, Public Health England reported that a variant had been discovered in the UK's southeast, predominantly in Kent. The variant, later named Alpha, showed changes to the spike protein that could make the virus more infectious. As of 13 December, 1,108 infections had been confirmed in the UK.[223][224]
On 4 February 2020, US Secretary of Health and Human Services Alex Azar waived liability for vaccine manufacturers in all cases except those involving "willful misconduct".[225][226]
2021
On 2 January, the Alpha variant, first discovered in the UK, had been identified in 33 countries.[227] On 6 January, the Gamma variant was first identified in Japanese travellers returning from Brazil.[228] On 29 January, it was reported that the Novavax vaccine was 49 percent effective against the Beta variant in a clinical trial in South Africa.[229][230] The CoronaVac vaccine was reported to be 50.4 percent effective in a Brazil clinical trial.[231]

On 12 March, several countries stopped using the Oxford-AstraZeneca COVID-19 vaccine- due to blood clotting problems, specifically cerebral venous sinus thrombosis (CVST).[232] On 20 March, the WHO and European Medicines Agency found no link to thrombosis, leading several countries to resume administering the vaccine.[233] In March WHO reported that an animal host was the most likely origin, without ruling out other possibilities.[2][35] The Delta variant was first identified in India. In mid-April, the variant was first detected in the UK and two months later it had become a full-fledged third wave in the country, forcing the government to delay reopening that was originally scheduled for June.[234]
On 10 November, Germany advised against the Moderna vaccine for people under 30, due to a possible association with myocarditis.[235] On 24 November, the Omicron variant was detected in South Africa; a few days later the World Health Organization declared it a VoC (variant of concern).[236] The new variant is more infectious than the Delta variant.[237]
2022

On 1 January, Europe passed 100 million cases amidst a surge in the Omicron variant.[238] Later that month, the WHO recommended the rheumatoid arthritis drug Baricitinib for severe or critical patients. It also recommended the monoclonal antibody Sotrovimab in patients with non-severe disease, but only those who are at highest risk of hospitalization.[239]
On 24 January, the Institute for Health Metrics and Evaluation estimated that about 57% of the world's population had been infected by COVID-19.[62][63] By 6 March, it was reported that the total worldwide death count had surpassed 6 million people.[240] By 6 July, Omicron subvariants BA.4 and BA.5 had spread worldwide.[241] WHO Director-General Tedros Ghebreyesus stated on 14 September 2022, that "[The world has] never been in a better position to end the pandemic", citing the lowest number of weekly reported deaths since March 2020. He continued, "We are not there yet. But the end is in sight—we can see the finish line".[242][243][244][245]
On 21 October, the United States surpassed 99 million cases of COVID-19, the most cases of any country.[246] By 30 October, the worldwide daily death toll was 424, the lowest since 385 deaths were reported on 12 March 2020.[247] 17 November marked the three-year anniversary since health officials in China first detected COVID-19.[248]
On 11 November, the WHO reported that deaths since the month of February had dropped 90 percent. Director-General Tedros said this was "cause for optimism".[249] On 3 December, the WHO indicated that, "at least 90% of the world's population has some level of immunity to Sars-CoV-2".[250] In early December, China began lifting some of its most stringent lockdown measures. Subsequent data from China's health authorities revealed that 248 million people, nearly 18 percent of its population, had been infected in the first 20 days of that month.[251] On 29 December, the US joined Italy, Japan, Taiwan and India in requiring negative COVID-19 test results from all people traveling from China due to the new surge in cases. The EU refused similar measures, stating that the BF7 omicron variant had already spread throughout Europe without becoming dominant.[252][253]
2023
On 4 January 2023, the World Health Organization said the information shared by China during the recent surge in infections lacked data, such as hospitalization rates.[254] On 10 January, the WHO's Europe office said the recent viral surge in China posed "no immediate threat."[255] On 16 January, the WHO recommended that China monitor excess mortality to provide "a more comprehensive understanding of the impact of COVID-19."[256]
On 30 January, the three-year anniversary of the original declaration, the World Health Organization determined that COVID-19 still met the criteria for a public health emergency of international concern (PHEIC).[257]
On 19 March, WHO Director-General Tedros indicated he was "confident" the COVID-19 pandemic would cease to be a public health emergency by the end of the year.[258] On 5 May, the WHO downgraded COVID-19 from being a global health emergency, though it continued to refer to it as a pandemic.[259] The WHO does not make official declarations of when pandemics end.[4][260] The decision came after Tedros convened with the International Health Regulations Emergency Committee, wherein the Committee noted that due to the decrease in deaths and hospitalisations, and the prevalence of vaccinations and the level of general immunity, it was time to remove the emergency designation and "transition to long-term management".[261] Tedros agreed, and the WHO reduced the classification to an "established and ongoing health issue".[261] In a press conference, Tedros remarked that the diminishing threat from COVID-19 had "allowed most countries to return to life as we knew it before COVID-19".[262]
In September the WHO said it had observed "concerning" trends in COVID-19 case numbers and hospitalisations, although analysis was hampered because many countries were no longer recording COVID-19 case statistics.[263]
In November 2023, in response to viral mutations and changing characteristics of infection, the WHO adjusted its treatment guidelines. Among other changes, remdesivir and molnupiravir were now recommended only for the most severe cases, and deuremidevir and ivermectin were recommended against.[264]
Responses
National reactions ranged from strict lockdowns to public education campaigns.[265] WHO recommended that curfews and lockdowns should be short-term measures to reorganise, regroup, rebalance resources, and protect the health care system.[266] As of 26 March 2020, 1.7 billion people worldwide were under some form of lockdown.[267] This increased to 3.9 billion people by the first week of April—more than half the world's population.[268][269]
In several countries, protests rose against restrictions such as lockdowns. A February 2021 study found that protests against restrictions were likely to directly increase the spread of the virus.[270]
Asia
As of the end of 2021, Asia's peak had come at the same time and at the same level as the world as a whole, in May 2021.[271] However, cumulatively they had experienced only half of the global average in cases.[272]

China opted for containment, instituting strict lockdowns to eliminate viral spread.[273][274] The vaccines distributed in China included the BIBP, WIBP, and CoronaVac.[275] It was reported on 11 December 2021, that China had vaccinated 1.162 billion of its citizens, or 82.5% of the total population of the country against COVID-19.[276] China's large-scale adoption of zero-COVID had largely contained the first waves of infections of the disease.[273][277][278] When the waves of infections due to the Omicron variant followed, China was almost alone in pursuing the strategy of zero-Covid to combat the spread of the virus in 2022.[279] Lockdown continued to be employed in November to combat a new wave of cases;[280][281] however, protests erupted in cities across China over the country's stringent measures,[282][283] and in December that year, the country relaxed its zero-COVID policy.[284] On 20 December 2022, the Chinese State Council narrowed its definition of what would be counted as a COVID-19 death to include solely respiratory failure, which led to skepticism by health experts of the government's total death count[285][286] at a time when hospitals reported being overwhelmed with cases following the abrupt discontinuation of zero-COVID.[287]
The first case in India was reported on 30 January 2020. India ordered a nationwide lockdown starting 24 March 2020,[288] with a phased unlock beginning 1 June 2020. Six cities accounted for around half of reported cases—Mumbai, Delhi, Ahmedabad, Chennai, Pune and Kolkata.[289] Post-lockdown, the Government of India introduced a contact tracking app called Aarogya Setu to help authorities manage contact tracing and vaccine distribution.[290] India's vaccination program was considered to be the world's largest and most successful with over 90% of citizens getting the first dose and another 65% getting the second dose.[291][292] A second wave hit India in April 2021, straining healthcare services.[293] On 21 October 2021, it was reported that the country had surpassed 1 billion vaccinations.[294]

Iran reported its first confirmed cases on 19 February 2020, in Qom.[296][297] Early measures included the cancellation/closure of concerts and other cultural events,[298] Friday prayers,[299] and school and university campuses.[300] Iran became a centre of the pandemic in February 2020.[301][302] More than ten countries had traced their outbreaks to Iran by 28 February, indicating a more severe outbreak than the 388 reported cases.[302][303] The Iranian Parliament closed, after 23 of its 290 members tested positive on 3 March 2020.[304] At least twelve sitting or former Iranian politicians and government officials had died by 17 March 2020.[305] By August 2021, the pandemic's fifth wave peaked, with more than 400 deaths in 1 day.[306]
COVID-19 was confirmed in South Korea on 20 January 2020. Military bases were quarantined after tests showed three infected soldiers.[307] South Korea introduced what was then considered the world's largest and best-organised screening programme, isolating infected people, and tracing and quarantining contacts.[308] Screening methods included mandatory self-reporting by new international arrivals through mobile application,[309] combined with drive-through testing,[310] and increasing testing capability to 20,000 people/day.[311] Despite some early criticisms,[312] South Korea's programme was considered a success in controlling the outbreak without quarantining entire cities.[308][313][314]
Europe

The COVID-19 pandemic arrived in Europe with its first confirmed case in Bordeaux, France, on 24 January 2020, and subsequently spread widely across the continent. By 17 March 2020, every country in Europe had confirmed a case,[315] and all had reported at least one death, with the exception of Vatican City. Italy was the first European nation to experience a major outbreak in early 2020, becoming the first country worldwide to introduce a national lockdown.[316] By 13 March 2020, the World Health Organization (WHO) declared Europe the epicentre of the pandemic[317][318] and it remained so until the WHO announced it had been overtaken by South America on 22 May.[319] By 18 March 2020, more than 250 million people were in lockdown in Europe.[320] Despite deployment of COVID-19 vaccines, Europe became the pandemic's epicentre once again in late 2021.[321][322]
The Italian outbreak began on 31 January 2020, when two Chinese tourists tested positive for SARS-CoV-2 in Rome.[213] Cases began to rise sharply, which prompted the government to suspend flights to and from China and declare a state of emergency.[323] On 22 February 2020, the Council of Ministers announced a new decree-law to contain the outbreak, which quarantined more than 50,000 people in northern Italy.[324] On 4 March, the Italian government ordered schools and universities closed as Italy reached a hundred deaths. Sport was suspended completely for at least one month.[325] On 11 March, Italian Prime Minister Giuseppe Conte closed down nearly all commercial activity except supermarkets and pharmacies.[326][327] On 19 April, the first wave ebbed, as 7-day deaths declined to 433.[328] On 13 October, the Italian government again issued restrictive rules to contain the second wave.[329] On 10 November, Italy surpassed 1 million confirmed infections.[330] On 23 November, it was reported that the second wave of the virus had led some hospitals to stop accepting patients.[331]

The virus was first confirmed to have spread to Spain on 31 January 2020, when a German tourist tested positive for SARS-CoV-2 on La Gomera in the Canary Islands.[332] Post-hoc genetic analysis has shown that at least 15 strains of the virus had been imported, and community transmission began by mid-February.[333] On 29 March, it was announced that, beginning the following day, all non-essential workers were ordered to remain at home for the next 14 days.[334] The number of cases increased again in July in a number of cities including Barcelona, Zaragoza and Madrid, which led to reimposition of some restrictions but no national lockdown.[335][336][337][338] By September 2021, Spain was one of the countries with the highest percentage of its population vaccinated (76% fully vaccinated and 79% with the first dose).[339] Italy is ranked second at 75%.[339]
Sweden differed from most other European countries in that it mostly remained open.[340] Per the Swedish constitution, the Public Health Agency of Sweden has autonomy that prevents political interference and the agency favoured remaining open. The Swedish strategy focused on longer-term measures, based on the assumption that after lockdown the virus would resume spreading, with the same result.[341][342] By the end of June, Sweden no longer had excess mortality.[343]
Devolution in the United Kingdom meant that each of its four countries developed its own response. England's restrictions were shorter-lived than the others.[344] The UK government started enforcing social distancing and quarantine measures on 18 March 2020.[345][346] On 16 March, Prime Minister Boris Johnson advised against non-essential travel and social contact, praising work from home and avoiding venues such as pubs, restaurants, and theatres.[347][348] On 20 March, the government ordered all leisure establishments to close,[349] and promised to prevent unemployment.[350] On 23 March, Johnson banned gatherings and restricted non-essential travel and outdoor activity. Unlike previous measures, these restrictions were enforceable by police through fines and dispersal of gatherings. Most non-essential businesses were ordered to close.[351] On 24 April 2020, it was reported that a promising vaccine trial had begun in England; the government pledged more than £50 million towards research.[352] On 16 April 2020, it was reported that the UK would have first access to the Oxford vaccine, due to a prior contract; should the trial be successful, some 30 million doses would be available.[353] On 2 December 2020, the UK became the first developed country to approve the Pfizer vaccine; 800,000 doses were immediately available for use.[354] In August 2022 it was reported that viral infection cases had declined in the UK.[355]
North America
The virus arrived in the United States on 13 January 2020.[356] Cases were reported in all North American countries after Saint Kitts and Nevis confirmed a case on 25 March, and in all North American territories after Bonaire confirmed a case on 16 April.[357]

Per Our World in Data, 103,436,829[5] confirmed cases have been reported in the United States with 1,190,579[5] deaths, the most of any country, and the nineteenth-highest per capita worldwide.[358] COVID-19 is the deadliest pandemic in US history;[359] it was the third-leading cause of death in the US in 2020, behind heart disease and cancer.[360] From 2019 to 2020, US life expectancy dropped by 3 years for Hispanic Americans, 2.9 years for African Americans, and 1.2 years for white Americans.[361] These effects have persisted as US deaths due to COVID-19 in 2021 exceeded those in 2020.[362] In the United States, COVID-19 vaccines became available under emergency use in December 2020, beginning the national vaccination program. The first COVID-19 vaccine was officially approved by the Food and Drug Administration on 23 August 2021.[363] By 18 November 2022, while cases in the U.S. had declined, COVID variants BQ.1/BQ.1.1 had become dominant in the country.[364][365]
In March 2020, as cases of community transmission were confirmed across Canada, all of its provinces and territories declared states of emergency. Provinces and territories, to varying degrees, implemented school and daycare closures, prohibitions on gatherings, closures of non-essential businesses and restrictions on entry. Canada severely restricted its border access, barring travellers from all countries with some exceptions.[366] Cases surged across Canada, notably in the provinces of British Columbia, Alberta, Quebec and Ontario, with the formation of the Atlantic Bubble, a travel-restricted area of the country (formed of the four Atlantic provinces).[367] Vaccine passports were adopted in all provinces and two of the territories.[368][369] Per a report on 11 November 2022, Canadian health authorities saw a surge in influenza, while COVID-19 was expected to rise during winter.[370]
South America

The COVID-19 pandemic was confirmed to have reached South America on 26 February 2020, when Brazil confirmed a case in São Paulo.[371] By 3 April, all countries and territories in South America had recorded at least one case.[372] On 13 May 2020, it was reported that Latin America and the Caribbean had reported over 400,000 cases of COVID-19 infection with 23,091 deaths. On 22 May 2020, citing the rapid increase of infections in Brazil, the World Health Organization WHO declared South America the epicentre of the pandemic.[373][374] As of 16 July 2021, South America had recorded 34,359,631 confirmed cases and 1,047,229 deaths from COVID-19. Due to a shortage of testing and medical facilities, it is believed that the outbreak is far larger than the official numbers show.[375]
The virus was confirmed to have spread to Brazil on 25 February 2020,[376] when a man from São Paulo who had traveled to Italy tested positive for the virus.[377] The disease had spread to every federative unit of Brazil by 21 March. On 19 June 2020, the country reported its one millionth case and nearly 49,000 reported deaths.[378][379] One estimate of under-reporting was 22.62% of total reported COVID-19 mortality in 2020.[380][381][382] As of 26 July 2024, Brazil, with 37,511,921[5] confirmed cases and 702,116[5] deaths, has the third-highest number of confirmed cases and second-highest death toll from COVID-19 in the world, behind only those of the United States and India.[383]
Africa

The COVID-19 pandemic was confirmed to have spread to Africa on 14 February 2020, with the first confirmed case announced in Egypt.[384][385] The first confirmed case in sub-Saharan Africa was announced in Nigeria at the end of February 2020.[386] Within three months, the virus had spread throughout the continent; Lesotho, the last African sovereign state to have remained free of the virus, reported its first case on 13 May 2020.[387][388] By 26 May, it appeared that most African countries were experiencing community transmission, although testing capacity was limited.[389] Most of the identified imported cases arrived from Europe and the United States rather than from China where the virus originated.[390] Many preventive measures were implemented by different countries in Africa including travel restrictions, flight cancellations, and event cancellations.[391] Despite fears, Africa reported lower death rates than other, more economically developed regions.[392]
In early June 2021, Africa faced a third wave of COVID infections with cases rising in 14 countries.[393] By 4 July the continent recorded more than 251,000 new COVID cases, a 20% increase from the prior week and a 12% increase from the January peak. More than sixteen African countries, including Malawi and Senegal, recorded an uptick in new cases.[394] The World Health Organization labelled it Africa's 'Worst Pandemic Week Ever'.[395] In October 2022, WHO reported that most countries on the African continent will miss the goal of 70 percent vaccination by the end of 2022.[396]
Oceania

The COVID-19 pandemic was confirmed to have reached Oceania on 25 January 2020, with the first confirmed case reported in Melbourne, Australia.[397][398] It has since spread elsewhere in the region.[399][398] Australia and New Zealand were praised for their handling of the pandemic in comparison to other Western nations, with New Zealand and each state in Australia wiping out all community transmission of the virus several times even after re-introduction into the community.[400][401][402]
As a result of the high transmissibility of the Delta variant, however, by August 2021, the Australian states of New South Wales and Victoria had conceded defeat in their eradication efforts.[403] In early October 2021, New Zealand also abandoned its elimination strategy.[404] In November and December, following vaccination efforts, the remaining states of Australia, excluding Western Australia, voluntarily gave up COVID-Zero to open up state and international borders.[405][406][407] The open borders allowed the Omicron variant of COVID-19 to enter quickly, and cases subsequently exceeded 120,000 a day.[408] By early March 2022, with cases exceeding 1,000 a day, Western Australia conceded defeat in its eradication strategy and opened its borders.[409] Despite record cases, Australian jurisdictions slowly removed restrictions such as close contact isolation, mask wearing, and density limits by April 2022.[410]
On 9 September 2022, restrictions were significantly relaxed. The aircraft mask mandate was scrapped nationwide, and daily reporting transitioned to weekly reporting.[411][412][413] On 14 September, COVID-19 disaster payment for isolating persons was extended for mandatory isolation.[414] By 22 September, all states had ended mask mandates on public transport, including in Victoria, where the mandate had lasted for approximately 800 days.[415] On 30 September 2022, all Australian leaders declared the emergency response finished and announced the end of isolation requirements. These changes were due in part to high levels of 'hybrid immunity' and low case numbers.[416]
Antarctica
Due to its remoteness and sparse population, Antarctica was the last continent to have confirmed cases of COVID-19.[417][418][419] The first cases were reported in December 2020, almost a year after the first cases of COVID-19 were detected in China. At least 36 people were infected in the first outbreak in 2020,[420] with several other outbreaks taking place in 2021 and 2022.[421]
United Nations
The United Nations Conference on Trade and Development (UNSC) was criticised for its slow response, especially regarding the UN's global ceasefire, which aimed to open up humanitarian access to conflict zones.[422][423] The United Nations Security Council was criticized due to the inadequate manner in which it dealt with the COVID-19 pandemic, namely the poor ability to create international collaboration during this crisis.[424][425]
On 23 March 2020, United Nations Secretary-General António Manuel de Oliveira Guterres appealed for a global ceasefire;[426][427] 172 UN member states and observers signed a non-binding supporting statement in June,[428] and the UN Security Council passed a resolution supporting it in July.[429][430]
On 29 September 2020, Guterres urged the International Monetary Fund to help certain countries via debt relief and also call for countries to increase contributions to develop vaccines.[431]
WHO

The WHO spearheaded initiatives such as the COVID-19 Solidarity Response Fund to raise money for the pandemic response, the UN COVID-19 Supply Chain Task Force, and the solidarity trial for investigating potential treatment options for the disease. The COVAX program, co-led by the WHO, GAVI, and the Coalition for Epidemic Preparedness Innovations (CEPI), aimed to accelerate the development, manufacture, and distribution of COVID-19 vaccines, and to guarantee fair and equitable access across the world.[432][433]
Restrictions

The pandemic shook the world's economy, with especially severe economic damage in the United States, Europe and Latin America.[434][435] A consensus report by American intelligence agencies in April 2021 concluded, "Efforts to contain and manage the virus have reinforced nationalist trends globally, as some states turned inward to protect their citizens and sometimes cast blame on marginalized groups." COVID-19 inflamed partisanship and polarisation around the world as bitter arguments exploded over how to respond. International trade was disrupted amid the formation of no-entry enclaves.[436]
Travel restrictions
The pandemic led many countries and regions to impose quarantines, entry bans, or other restrictions, either for citizens, recent travellers to affected areas,[437] or for all travellers.[438][439] Travel collapsed worldwide, damaging the travel sector. The effectiveness of travel restrictions was questioned as the virus spread across the world.[440] One study found that travel restrictions only modestly affected the initial spread, unless combined with other infection prevention and control measures.[441][442] Researchers concluded that "travel restrictions are most useful in the early and late phase of an epidemic" and "restrictions of travel from Wuhan unfortunately came too late".[443] The European Union rejected the idea of suspending the Schengen free travel zone.[444][445]
Repatriation of foreign citizens

Several countries repatriated their citizens and diplomatic staff from Wuhan and surrounding areas, primarily through charter flights. Canada, the United States, Japan, India, Sri Lanka, Australia, France, Argentina, Germany and Thailand were among the first to do so.[446] Brazil and New Zealand evacuated their own nationals and others.[447][448] On 14 March, South Africa repatriated 112 South Africans who tested negative, while four who showed symptoms were left behind.[449] Pakistan declined to evacuate its citizens.[450]
On 15 February, the US announced it would evacuate Americans aboard the Diamond Princess cruise ship,[451] and on 21 February, Canada evacuated 129 Canadians from the ship.[452] In early March, the Indian government began repatriating its citizens from Iran.[453][454] On 20 March, the United States began to withdraw some troops from Iraq.[455]
Impact
Economics

The pandemic and responses to it damaged the global economy. On 27 February 2020, worries about the outbreak crushed US stock indexes, which posted their sharpest falls since 2008.[456]
Tourism collapsed due to travel restrictions, closing of public places including travel attractions, and advice of governments against travel. Airlines cancelled flights, while British regional airline Flybe collapsed.[457] The cruise line industry was hard hit,[458] and train stations and ferry ports closed.[459] International mail stopped or was delayed.[460]
The retail sector faced reductions in store hours or closures.[461] Retailers in Europe and Latin America faced traffic declines of 40 percent. North America and Middle East retailers saw a 50–60 percent drop.[462] Shopping centres faced a 33–43 percent drop in foot traffic in March compared to February. Mall operators around the world coped by increasing sanitation, installing thermal scanners to check the temperature of shoppers, and cancelling events.[463]
Hundreds of millions of jobs were lost,[464][465] including more than 40 million jobs in the US.[466] According to a report by Yelp, about 60% of US businesses that closed will stay shut permanently.[467] The International Labour Organization (ILO) reported that the income generated in the first nine months of 2020 from work across the world dropped by 10.7 percent, or $3.5 trillion.[468]
Supply shortages

Pandemic fears led to panic buying, emptying groceries of essentials such as food, toilet paper, and bottled water. Panic buying stemmed from perceived threat, perceived scarcity, fear of the unknown, coping behaviour and social psychological factors (e.g. social influence and trust).[469]
Supply shortages were due to disruption to factory and logistic operations; shortages were worsened by supply chain disruptions from factory and port shutdowns, and labour shortages.[470]
Shortages continued as managers underestimated the speed of economic recovery after the initial economic crash. The technology industry, in particular, warned of delays from underestimates of semiconductor demand for vehicles and other products.[471]
According to WHO Secretary-General Tedros Ghebreyesus, demand for personal protective equipment (PPE) rose one hundredfold, pushing prices up twentyfold.[472][473] PPE stocks were exhausted everywhere.[474][475][476]
In September 2021, the World Bank reported that food prices remained generally stable and the supply outlook remained positive. However, the poorest countries witnessed a sharp increase in food prices, reaching the highest level since the pandemic began.[477][478] The Agricultural Commodity Price Index stabilized in the third quarter but remained 17% higher than in January 2021.[479][478]
By contrast, petroleum products were in surplus at the beginning of the pandemic, as demand for gasoline and other products collapsed due to reduced commuting and other trips.[480] The 2021 global energy crisis was driven by a global surge in demand as the world economy recovered. Energy demand was particularly strong in Asia.[481][482]
Arts and cultural heritage
The performing arts and cultural heritage sectors were profoundly affected by the pandemic. Both organisations' and individuals' operations have been impacted globally. By March 2020, across the world and to varying degrees, museums, libraries, performance venues, and other cultural institutions had been indefinitely closed with their exhibitions, events and performances cancelled or postponed.[483] A 2021 UNESCO report estimated ten million job losses worldwide in the culture and creative industries.[484][485] Some services continued through digital platforms,[486][487][488] such as live streaming concerts[489] or web-based arts festivals.[490]
Politics
The pandemic affected political systems, causing suspensions of legislative activities,[491] isolations or deaths of politicians,[492] and rescheduled elections.[493] Although they developed broad support among epidemiologists, NPIs (non-pharmaceutical interventions) were controversial in many countries. Intellectual opposition came primarily from other fields, along with heterodox epidemiologists.[494]
Brazil
The pandemic (and the response of Brazilian politicians to it) led to widespread panic, confusion, and pessimism in Brazil.[495] When questioned regarding record deaths in the country in April 2020, Brazilian President Jair Bolsonaro said "So what? I'm sorry. What do you want me to do about it?"[496] Bolsonaro disregarded WHO-recommended mitigation techniques and instead downplayed the risks of the virus, promoted increased economic activity, spread misinformation about the efficacy of masks, vaccines and public health measures, and distributed unproven treatments including hydroxychloroquine and ivermectin.[495] A series of federal health ministers resigned or were dismissed after they refused to implement Bolsonaro's policies.[497]
Disagreements between federal and state governments led to a chaotic and delayed response to the rapid spread of the virus,[498] exacerbated by preexisting social and economic disparities in the country.[495][499] Employment, investment and valuation of the Brazilian real plummeted to record lows.[495][500] Brazil was also heavily affected by the Delta and Omicron variants.[501] At the height of the outbreak in the spring of 2021, 3,000+ Brazilians were dying per day.[502][503] Bolsonaro's loss to Lula da Silva in the 2022 presidential election is widely credited to the former's mishandling of the pandemic.[504][505][506]
China
Multiple provincial-level administrators of the Chinese Communist Party (CCP) were dismissed over their handling of quarantine measures. Some commentators claimed this move was intended to protect CCP General Secretary Xi Jinping.[507] The US intelligence community claimed that China intentionally under-reported its COVID-19 caseload.[508] The Chinese government maintained that it acted swiftly and transparently.[509][510] Journalists and activists in China who reported on the pandemic were detained by authorities,[511][512] including Zhang Zhan, who was arrested and tortured.[513][514]
Italy

In early March 2020, the Italian government criticised the EU's lack of solidarity with Italy.[515][516][517] On 22 March 2020, after a phone call with Italian Prime Minister Giuseppe Conte, Russian President Vladimir Putin ordered the Russian army to send military medics, disinfection vehicles, and other medical equipment to Italy.[518][519] In early April, Norway and EU states like Romania and Austria started to offer help by sending medical personnel and disinfectant,[520] and European Commission President Ursula von der Leyen offered an official apology to the country.[521]
United States

Beginning in mid-April 2020, protestors objected to government-imposed business closures and restrictions on personal movement and assembly.[523] Simultaneously, essential workers protested unsafe conditions and low wages by participating in a brief general strike.[524] Some political analysts claimed that the pandemic contributed to President Donald Trump's 2020 defeat.[525][526]
The COVID-19 pandemic in the United States prompted calls for the United States to adopt social policies common in other wealthy countries, including universal health care, universal child care, paid sick leave, and higher levels of funding for public health.[527][528][529] The Kaiser Family Foundation estimated that preventable hospitalizations of unvaccinated Americans in the second half of 2021 cost US$13.8 billion.[530]
There were also protest in regards to vaccine mandates in the United States.[531] In January 2022, the US Supreme Court struck down an OSHA rule that mandated vaccination or a testing regimen for all companies with greater than 100 employees.[532][533]
Other countries
The number of journalists imprisoned or detained increased worldwide; some detentions were related to the pandemic.[534][535] The planned NATO "Defender 2020" military exercise in Germany, Poland and the Baltic states, the largest NATO war exercise since the end of the Cold War, was held on a reduced scale.[536][537]
The Iranian government was heavily affected by the virus, which infected some two dozen parliament members and political figures.[303][538] Iran President Hassan Rouhani wrote a public letter to world leaders asking for help on 14 March 2020, due to a lack of access to international markets.[539] Saudi Arabia, which had launched a military intervention in Yemen in March 2015, declared a ceasefire.[540]
Diplomatic relations between Japan and South Korea worsened.[541] South Korea criticised Japan's "ambiguous and passive quarantine efforts" after Japan announced travellers from South Korea must quarantine for two weeks.[542] South Korean society was initially polarised on President Moon Jae-in's response to the crisis; many Koreans signed petitions calling for Moon's impeachment or praising his response.[312]
Some countries passed emergency legislation. Some commentators expressed concern that it could allow governments to strengthen their grip on power.[543][544] In Hungary, the parliament voted to allow Prime Minister Viktor Orbán to rule by decree indefinitely, suspend parliament and elections, and punish those deemed to have spread false information.[545] In countries such as Egypt,[546] Turkey,[547] and Thailand,[548] opposition activists and government critics were arrested for allegedly spreading fake news.[549] In India, journalists criticising the government's response were arrested or issued warnings by police and authorities.[550]
Food systems
The pandemic disrupted food systems worldwide,[551][552] hitting at a time when hunger and undernourishment were rising- an estimated 690 million people lacked food security in 2019.[553] Food access fell – driven by falling incomes, lost remittances, and disruptions to food production.[554] In some cases, food prices rose.[551][553] The pandemic and its accompanying lockdowns and travel restrictions slowed movement of food aid. According to the WHO, 811 million people were undernourished in 2020, "likely related to the fallout of COVID-19".[555][435]
Education

The pandemic impacted educational systems in many countries. Many governments temporarily closed educational institutions, often replaced by online education. Other countries, such as Sweden, kept their schools open. As of September 2020, approximately 1.077 billion learners were affected due to school closures. School closures impacted students, teachers, and families with far-reaching economic and societal consequences.[556] They shed light on social and economic issues, including student debt, digital learning, food insecurity, and homelessness, as well as access to childcare, health care, housing, internet, and disability services. The impact was more severe for disadvantaged children.[557] The Higher Education Policy Institute reported that around 63% of students claimed worsened mental health as a result of the pandemic.[558]
Health
The pandemic impacted global health for many conditions. Hospital visits fell.[559] Visits for heart attack symptoms declined by 38% in the US and 40% in Spain.[560] The head of cardiology at the University of Arizona said, "My worry is some of these people are dying at home because they're too scared to go to the hospital."[561] People with strokes and appendicitis were less likely to seek treatment.[562][563][561] Medical supply shortages impacted many people.[564] The pandemic impacted mental health,[565][566] increasing anxiety, depression, and post-traumatic stress disorder, affecting healthcare workers, patients and quarantined individuals.[567][568]
In late 2022, during the first northern hemisphere autumn and winter seasons following the widespread relaxation of global public health measures, North America and Europe experienced a surge in respiratory viruses and coinfections in both adults and children.[569] This formed the beginning of the 2022–2023 pediatric care crisis and what some experts termed a "tripledemic" of seasonal influenza, respiratory syncytial virus (RSV), and SARS-CoV-2 throughout North America.[570][571] In the United Kingdom, pediatric infections also began to spike beyond pre-pandemic levels, albeit with different illnesses, such as Group A streptococcal infection and resultant scarlet fever.[572][573] As of mid-December 2022, 19 children in the UK had died due to Strep A and the wave of infections had begun to spread into North America and Mainland Europe.[574][575]
The B/Yamagata lineage of influenza B might have become extinct in 2020/2021 due to COVID-19 pandemic measures.[576][577] There have been no naturally occurring cases confirmed since March 2020.[578][579] In 2023, the World Health Organization concluded that protection against the Yamagata lineage was no longer necessary in the seasonal flu vaccine, reducing the number of lineages targeted by the vaccine from four to three.[578][579]
Environment

The pandemic and the reaction to it positively affected the environment and climate as a result of reduced human activity. During the "anthropause", fossil fuel use decreased, resource consumption declined, and waste disposal improved, generating less pollution.[581] Planned air travel and vehicle transportation declined. In China, lockdowns and other measures resulted in a 26% decrease in coal consumption, and a 50% reduction in nitrogen oxides emissions.[581][582][583]
In 2020, a worldwide study on mammalian wildlife responses to human presence during COVID lockdowns found complex patterns of animal behavior. Carnivores were generally less active when humans were around, while herbivores in developed areas were more active. Among other findings, this suggested that herbivores may view humans as a shield against predators, highlighting the importance of location and human presence history in understanding wildlife responses to changes in human activity in a given area.[584]
A wide variety of largely mammalian species, both captive and wild, have been shown to be susceptible to SARS-CoV-2, with some encountering a particularly high degree of fatal outcomes.[585] In particular, both farmed and wild mink have developed highly symptomatic and severe COVID-19 infections, with a mortality rate as high as 35–55% according to one study.[586][587] White-tailed deer, on the other hand, have largely avoided severe outcomes but have effectively become natural reservoirs of the virus, with large numbers of free-ranging deer infected throughout the US and Canada, including approximately 80% of Iowa's wild deer herd.[588][589] An August 2023 study appeared to confirm the status of white-tailed deer as a disease reservoir, noting that the viral evolution of SARS-CoV-2 in deer occurs at triple the rate of its evolution in humans and that infection rates remained high, even in areas rarely frequented by humans.[590]
Discrimination and prejudice

Heightened prejudice, xenophobia, and racism toward people of Chinese and East Asian descent were documented around the world.[592][593] Reports from February 2020, when most confirmed cases were confined to China, cited racist sentiments about Chinese people 'deserving' the virus.[594][595][596] Individuals of Asian descent in Europe and North America reported increasing instances of racially-motivated abuse and assaults as a result of the pandemic.[597][598][599] US President Donald Trump was criticised for referring to SARS-CoV-2 as the "Chinese Virus" and "Kung Flu", terms which were condemned as being racist and xenophobic.[600][601][602]
Age-based discrimination against older adults increased during the pandemic. This was attributed to their perceived vulnerability and subsequent physical and social isolation measures, which, coupled with their reduced social activity, increased dependency on others. Similarly, limited digital literacy left the elderly more vulnerable to isolation, depression, and loneliness.[603]
In a correspondence published in The Lancet in 2021, German epidemiologist Günter Kampf described the harmful effects of "inappropriate stigmatisation of unvaccinated people, who include our patients, colleagues, and other fellow citizens", noting the evidence that vaccinated individuals play a large role in transmission.[604] American bioethicist Arthur Caplan responded to Kampf, writing "Criticising [the unvaccinated] who... wind up in hospitals and morgues in huge numbers, put stress on finite resources, and prolong the pandemic... is not stigmatising, it is deserved moral condemnation."[605]
In January 2022, Amnesty International urged Italy to change their anti-COVID-19 restrictions to avoid discrimination against unvaccinated people, saying that "the government must continue to ensure that the entire population can enjoy its fundamental rights." The restrictions included mandatory vaccination over the age of 50, and mandatory vaccination to use public transport.[606]
Lifestyle changes

The pandemic triggered massive changes in behaviour, from increased Internet commerce to cultural changes in the workplace. Online retailers in the US posted $791.70 billion in sales in 2020, an increase of 32.4% from $598.02 billion the year before.[607] Home delivery orders increased, while indoor restaurant dining shut down due to lockdown orders or low sales.[608][609] Hackers, cybercriminals and scammers took advantage of the changes to launch new online attacks.[610]
Education in some countries temporarily shifted from physical attendance to video conferencing.[611] Massive layoffs shrank the airline, travel, hospitality, and other industries.[612][613] Despite most corporations implementing measures to address COVID-19 in the workplace, a poll from Catalyst found that as many as 68% of employees around the world felt that these policies were only performative and "not genuine".[614]
The pandemic led to a surge in remote work. According to a Gallup poll, only 4% of US employees were fully remote before the pandemic, compared to 43% in May 2020. Among white collar workers, that shift was more pronounced, with 6% increasing to 65% in the same period.[615] That trend continued in later stages of the pandemic, with many workers choosing to remain remote even after workplaces reopened.[616][617] Many Nordic, European, and Asian companies increased their recruitment of international remote workers even as the pandemic waned, partially to save on labor costs.[618][619] This also led to a talent drain in the global south and in remote areas in the global north.[619][620] High cost of living and dense urban areas also lost office real estate value due to remote worker exodus.[621] By May 2023, due to increasing layoffs and concerns over productivity, some white collar workplaces in the US had resorted to performance review penalties and indirect incentives (e.g. donations to charity) to encourage workers to return to the office.[622]
Historiography
A 2021 study noted that the COVID-19 pandemic had increased interest in epidemics and infectious diseases among both historians and the general public. Prior to the pandemic, these topics were usually overlooked by "general" history and only received attention in the history of medicine.[623] Many comparisons were made between the COVID-19 and 1918 influenza pandemics,[624][625] including the development of anti-mask movements,[626][627] the widespread promotion of misinformation[628][629] and the impact of socioeconomic disparities.[630]
Religion

In some areas, religious groups exacerbated the spread of the virus, through large gatherings and the dissemination of misinformation.[631][632][633] Some religious leaders decried what they saw as violations of religious freedom.[634] In other cases, religious identity was a beneficial factor for health, increasing compliance with public health measures and protecting against the negative effects of isolation on mental wellbeing.[635][636][637]
Information dissemination
Some news organizations removed their online paywalls for some or all of their pandemic-related articles and posts.[638] Many scientific publishers provided pandemic-related journal articles to the public free of charge as part of the National Institutes of Health's COVID-19 Public Health Emergency Initiative.[639][640][641] According to one estimate from researchers at the University of Rome, 89.5% of COVID-19-related papers were open access, compared to an average of 48.8% for the ten most deadly human diseases.[642] The share of papers published on preprint servers prior to peer review increased dramatically.[643]
Misinformation
Misinformation and conspiracy theories about the pandemic have been widespread; they travel through mass media, social media and text messaging.[644] In March 2020, WHO declared an "infodemic" of incorrect information.[645] Cognitive biases, such as confirmation bias, are linked to conspiracy beliefs, including COVID-19 vaccine hesitancy.[646]
Culture and society
The COVID-19 pandemic had a major impact on popular culture. It was included in the narratives of ongoing pre-pandemic television series and become a central narrative in new ones, with mixed results.[647] Writing for The New York Times about the then-upcoming BBC sitcom Pandemonium on 16 December 2020, David Segal asked, "Are we ready to laugh about Covid-19? Or rather, is there anything amusing, or recognizable in a humorous way, about life during a plague, with all of its indignities and setbacks, not to mention its rituals and rules."[648]
The pandemic had driven some people to seek peaceful escapism in media, while others were drawn towards fictional pandemics (e.g. zombie apocalypses) as an alternate form of escapism.[649] Common themes have included contagion, isolation and loss of control.[650] Many drew comparisons to the fictional film Contagion (2011),[651][652] praising its accuracies while noting some differences,[653] such as the lack of an orderly vaccine rollout.[654][655]
As people turned to music to relieve emotions evoked by the pandemic, Spotify listenership showed that classical, ambient and children's genres grew, while pop, country and dance remained relatively stable.[656][657]
Transition to later phases
On 5 May 2023, the WHO declared that the pandemic was no longer a public health emergency of international concern.[658] This led several media outlets to incorrectly report that this meant the pandemic was "over". The WHO commented to Full Fact that it was unlikely to declare the pandemic over "in the near future" and mentioned cholera, which it considers to have been a pandemic since 1961 (i.e., continuously for the last 63 years).[659] The WHO does not have an official category for pandemics or make declarations of when pandemics start or end.[4][260][660][11]
In June 2023, Hans Kluge, director of the WHO in Europe, commented that "While the international public health emergency may have ended, the pandemic certainly has not". The WHO in Europe launched a transition plan to manage the public health response to COVID-19 in the coming years and prepare for possible future emergencies.[661]
Epidemics and pandemics usually end when the disease becomes endemic, and when the disease becomes “an accepted, manageable part of normal life in a given society.”[13] As of March 2024, there was no widely agreed definition of when a disease is or is not a pandemic, though efforts at a formal definition were underway. Experts asked by Time that month noted that COVID-19 continued to circulate and cause disease, but expressed uncertainty as to whether it should still be described as a pandemic.[11]
Future endemic phase
In June 2022, an article in Human Genomics said that the pandemic was still "raging", but that "now is the time to explore the transition from the pandemic to the endemic phase."[662]
A March 2022 review declared the transition to endemic status to be "inevitable".[663] A June 2022 review predicted that the virus that causes COVID-19 would become the fifth endemic seasonal coronavirus, alongside four other human coronaviruses.[664] A February 2023 review of the four common cold coronaviruses concluded that the virus would become seasonal and, like the common cold, cause less severe disease for most people.[665] As of 2023[update] the transition to endemic COVID-19 may take years or decades.[666]
Long-term effects
Economic
Despite strong economic rebounds following the initial lockdowns in early 2020, towards the latter phases of the pandemic, many countries began to experience long-term economic effects. Several countries saw high inflation rates which had global impacts, particularly in developing countries.[667] Some economic impacts such as supply chain and trade operations were seen as more permanent as the pandemic exposed major weaknesses in these systems.[668]
In Australia, the pandemic caused an increase in occupational burnout in 2022.[669]
During the pandemic, a large percentage of workers in Canada came to prefer working from home, which had an impact on the traditional work model. Some corporations made efforts to force workers to return to work on-site, while some embraced the idea.[670]
Travel
There was a "travel boom" causing air travel to recover at rates faster than anticipated, and the aviation industry became profitable in 2023 for the first time since 2019, before the pandemic.[671] However, economic issues meant some predicted that the boom would begin to slow down.[672] Business travel on airlines was still below pre-pandemic levels and is predicted not to recover.[673]
Health
An increase in excess deaths from underlying causes not related to COVID-19 has been largely blamed on systematic issues causing delays in health care and screening during the pandemic, which has resulted in an increase of non-COVID-19 related deaths.[674]
Immunizations
During the pandemic, millions of children missed out on vaccinations as countries focused efforts on combating COVID-19. Efforts were made to increase vaccination rates among children in low-income countries. These efforts were successful in increasing vaccination rates for some diseases, though the UN noted that post-pandemic measles vaccinations were still falling behind.[675]
Some of the decrease in immunization was driven by an increase in mistrust of public health officials. This was seen in both low-income and high-income countries. Several African countries saw a decline in vaccinations due to misinformation around the pandemic flowing into other areas.[676] Immunization rates have yet to recover in the United States[677] and the United Kingdom.[678]
See also
- Coronavirus diseases
- Emerging infectious disease
- Globalization and disease
- List of epidemics and pandemics
- Memorials for the COVID-19 pandemic
Notes
References
- ^ Zoumpourlis V, Goulielmaki M, Rizos E, Baliou S, Spandidos DA (October 2020). "[Comment] The COVID‑19 pandemic as a scientific and social challenge in the 21st century". Molecular Medicine Reports. 22 (4): 3035–3048. doi:10.3892/mmr.2020.11393. PMC 7453598. PMID 32945405.
- ^ a b "WHO-convened global study of origins of SARS-CoV-2: China Part". World Health Organization. 30 March 2021. Retrieved 31 March 2021.
- ^ a b c "Archived: WHO Timeline - COVID-19". Word Health Organization. 27 April 2020. Archived from the original on 29 April 2020. Retrieved 7 March 2024.
- ^ a b c d Rigby J, Satija B (8 May 2023). "WHO declares end to COVID global health emergency". Reuters. Retrieved 9 May 2023.
- ^ a b c d e f g h i Ritchie H, Mathieu E, Rodés-Guirao L, Appel C, Giattino C, Ortiz-Ospina E, et al. (2020–2022). "Coronavirus Pandemic (COVID-19)". Our World in Data. Retrieved 26 July 2024.
- ^ Mathieu E, Ritchie H, Rodés-Guirao L, Appel C, Giattino C, Hasell J, et al. (5 March 2020). "Coronavirus Pandemic (COVID-19)". Our World in Data. Archived from the original on 24 February 2024. Retrieved 24 February 2024.
- ^ a b "The pandemic's true death toll". The Economist. 26 July 2023 [18 November 2021]. Retrieved 26 July 2023.
- ^ a b c "COVID-19 Dashboard by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU)". ArcGIS. Johns Hopkins University. Retrieved 10 March 2023.
- ^ "Clinical questions about COVID-19: Questions and answers". CDC Stacks. 25 June 2020. Retrieved 26 May 2023.
- ^ Gita G (14 April 2020). "The Great Lockdown: Worst Economic Downturn Since the Great Depression". IMF Blog. Retrieved 23 April 2020.
- ^ a b c d Ducharme J (11 March 2024). "Experts Can't Agree If We're Still in a Pandemic". TIME. Retrieved 31 May 2024.
- ^ Colarossi J (5 March 2024). "Is COVID-19 Still a Pandemic?". The Brink. Boston University. Archived from the original on 15 May 2024. Retrieved 9 June 2024.
- ^ a b c Charters E, Heitman K (2021). "How epidemics end". Centaurus; International Magazine of the History of Science and Medicine. 63 (1): 210–224. doi:10.1111/1600-0498.12370. PMC 8014506. PMID 33821019.
- ^ Doraiswamy S, Mamtani R, Cheema S (August 2022). "An in-depth analysis of 10 epidemiological terminologies used in the context of COVID-19". Scand J Public Health. 50 (6): 819–826. doi:10.1177/14034948211057736. PMC 9361413. PMID 34903120.
- ^ Multiple sources:
- "2nd U.S. Case Of Wuhan Coronavirus Confirmed". NPR.org. NPR. Retrieved 4 April 2020.
- McNeil Jr DG (2 February 2020). "Wuhan Coronavirus Looks Increasingly Like a Pandemic, Experts Say". The New York Times. ISSN 0362-4331. Retrieved 4 April 2020.
- Griffiths J. "Wuhan coronavirus deaths spike again as outbreak shows no signs of slowing". CNN. Retrieved 4 April 2020.
- ^ Zhu H, Wei L, Niu P (2 March 2020). "The novel coronavirus outbreak in Wuhan, China". Global Health Research and Policy. 5 (1): 6. doi:10.1186/s41256-020-00135-6. PMC 7050114. PMID 32226823.
- ^ Jiang S, Xia S, Ying T, Lu L (May 2020). "A novel coronavirus (2019-nCoV) causing pneumonia-associated respiratory syndrome". Cellular & Molecular Immunology. 17 (5): 554. doi:10.1038/s41423-020-0372-4. PMC 7091741. PMID 32024976.
- ^ Chan JF, Yuan S, Kok KH, To KK, Chu H, Yang J, et al. (February 2020). "A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster". Lancet. 395 (10223): 514–523. doi:10.1016/S0140-6736(20)30154-9. PMC 7159286. PMID 31986261.
- ^ "Novel Coronavirus (2019-nCoV) Situation Report – 1" (PDF). World Health Organization (WHO). 21 January 2020.
- ^ "Novel Coronavirus(2019-nCoV) Situation Report – 10" (PDF). World Health Organization (WHO). 30 January 2020.
- ^ Multiple sources:
- "Novel coronavirus named 'Covid-19': WHO". Today. Singapore. Archived from the original on 21 March 2020. Retrieved 11 February 2020.
- "The coronavirus spreads racism against – and among – ethnic Chinese". The Economist. 17 February 2020. Archived from the original on 17 February 2020. Retrieved 17 February 2020.
- World Health Organization Best Practices for the Naming of New Human Infectious Diseases (PDF) (Report). World Health Organization (WHO). May 2015. hdl:10665/163636.
- ^ a b "Naming the coronavirus disease (COVID-19) and the virus that causes it". World Health Organization (WHO). Archived from the original on 28 February 2020. Retrieved 13 March 2020.
- ^ Coronavirus disease 2019 (COVID-19) in the EU/EEA and the UK – eighth update (PDF) (Report). ecdc. Archived (PDF) from the original on 14 March 2020. Retrieved 19 April 2020.
- ^ "Covid Indian variant: Where is it, how does it spread and is it more infectious?". BBC News. 7 June 2021. Retrieved 20 July 2021.
- ^ "Covid: WHO renames UK and other variants with Greek letters". BBC News. 31 May 2021. Retrieved 8 June 2021.
- ^ Patel V (27 November 2021). "How Omicron, the New Covid-19 Variant, Got Its Name". The New York Times. ISSN 0362-4331. Archived from the original on 28 November 2021. Retrieved 28 November 2021.
- ^ "There are several COVID-19 variants you haven't heard of". NewsNation Now. 27 November 2021. Archived from the original on 27 November 2021. Retrieved 27 November 2021.
- ^ Perlman S (February 2020). "Another Decade, Another Coronavirus". The New England Journal of Medicine. 382 (8): 760–762. doi:10.1056/NEJMe2001126. PMC 7121143. PMID 31978944.
- ^ Cyranoski D (March 2020). "Mystery deepens over animal source of coronavirus". Nature. 579 (7797): 18–19. Bibcode:2020Natur.579...18C. doi:10.1038/d41586-020-00548-w. PMID 32127703. S2CID 211836524.
- ^ Zhang T, Wu Q, Zhang Z (April 2020). "Probable Pangolin Origin of SARS-CoV-2 Associated with the COVID-19 Outbreak". Current Biology. 30 (7): 1346–1351.e2. Bibcode:2020CBio...30E1346Z. doi:10.1016/j.cub.2020.03.022. PMC 7156161. PMID 32197085.
- ^ "Outbreak of severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2): increased transmission beyond China – fourth update" (PDF). European Centre for Disease Prevention and Control. 14 February 2020. Retrieved 8 March 2020.
- ^ Liu J, Liu S, Wei H, Yang X (October 2020). "Epidemiology, clinical characteristics of the first cases of COVID-19". Eur J Clin Invest (Review). 50 (10): e13364. doi:10.1111/eci.13364. PMID 32725884. S2CID 220852984.
- ^ Sun J, He WT, Wang L, Lai A, Ji X, Zhai X, et al. (May 2020). "COVID-19: Epidemiology, Evolution, and Cross-Disciplinary Perspectives". Trends in Molecular Medicine. 26 (5): 483–495. doi:10.1016/j.molmed.2020.02.008. PMC 7118693. PMID 32359479.
- ^ "WHO Points To Wildlife Farms In Southern China As Likely Source Of Pandemic". NPR. 15 March 2021.
- ^ a b Maxmen A (April 2021). "WHO report into COVID pandemic origins zeroes in on animal markets, not labs". Nature. 592 (7853): 173–174. Bibcode:2021Natur.592..173M. doi:10.1038/d41586-021-00865-8. PMID 33785930. S2CID 232429241.
- ^ a b c Hu B, Guo H, Zhou P, Shi ZL (March 2021). "Characteristics of SARS-CoV-2 and COVID-19". Nature Reviews. Microbiology. 19 (3): 141–154. doi:10.1038/s41579-020-00459-7. PMC 7537588. PMID 33024307.
- ^ a b Graham RL, Baric RS (May 2020). "SARS-CoV-2: Combating Coronavirus Emergence". Immunity. 52 (5): 734–736. doi:10.1016/j.immuni.2020.04.016. PMC 7207110. PMID 32392464.
- ^ To KK, Sridhar S, Chiu KH, Hung DL, Li X, Hung IF, et al. (December 2021). "Lessons learned 1 year after SARS-CoV-2 emergence leading to COVID-19 pandemic". Emerging Microbes & Infections. 10 (1): 507–535. doi:10.1080/22221751.2021.1898291. PMC 8006950. PMID 33666147.
- ^ Multiple sources:
- "The COVID-19 coronavirus epidemic has a natural origin, scientists say – Scripps Research's analysis of public genome sequence data from SARS‑CoV‑2 and related viruses found no evidence that the virus was made in a laboratory or otherwise engineered". EurekAlert!. Scripps Research Institute. 17 March 2020. Retrieved 15 April 2020.
- Andersen KG, Rambaut A, Lipkin WI, Holmes EC, Garry RF (April 2020). "The proximal origin of SARS-CoV-2". Nature Medicine. 26 (4): 450–452. doi:10.1038/s41591-020-0820-9. PMC 7095063. PMID 32284615.
- Latinne A, Hu B, Olival KJ, Zhu G, Zhang L, Li H, et al. (August 2020). "Origin and cross-species transmission of bat coronaviruses in China". Nature Communications. 11 (1): 4235. Bibcode:2020NatCo..11.4235L. doi:10.1038/s41467-020-17687-3. PMC 7447761. PMID 32843626.
- Fox M (7 July 2021). "Coronavirus almost certainly came from an animal, not a lab leak, top scientists argue". CNN. Retrieved 9 July 2021.
- "Market in China's Wuhan likely origin of COVID-19 outbreak – study". Reuters. 19 November 2021. Retrieved 19 November 2021.
- ^ To KK, Sridhar S, Chiu KH, Hung DL, Li X, Hung IF, et al. (March 2021). "Lessons learned 1 year after SARS-CoV-2 emergence leading to COVID-19 pandemic". Emerging Microbes & Infections. 10 (1): 507–535. doi:10.1080/22221751.2021.1898291. PMC 8006950. PMID 33666147.
- ^ Horowitz J, Stanway D (9 February 2021). "COVID may have taken 'convoluted path' to Wuhan, WHO team leader says". Reuters. Archived from the original on 10 February 2021. Retrieved 10 February 2021.
- ^ Pauls K, Yates J (27 January 2020). "Online claims that Chinese scientists stole coronavirus from Winnipeg lab have 'no factual basis'". Canadian Broadcasting Corporation. Archived from the original on 8 February 2020. Retrieved 8 February 2020.
- ^ "China's rulers see the coronavirus as a chance to tighten their grip". The Economist. 8 February 2020. Archived from the original on 29 February 2020. Retrieved 29 February 2020.
- ^ Holmes EC, Goldstein SA, Rasmussen AL, Robertson DL, Crits-Christoph A, Wertheim JO, et al. (August 2021). "The Origins of SARS-CoV-2: A Critical Review". Cell. 184 (19): 4848–4856. doi:10.1016/j.cell.2021.08.017. PMC 8373617. PMID 34480864.
- ^ "Laboratory testing for 2019 novel coronavirus (2019-nCoV) in suspected human cases". World Health Organization (WHO). Retrieved 30 March 2020.
- ^ "Total tests for COVID-19 per 1,000 people". Our World in Data. Retrieved 16 April 2020.
- ^ "Report 13 – Estimating the number of infections and the impact of non-pharmaceutical interventions on COVID-19 in 11 European countries". Imperial College London. Retrieved 7 April 2020.
- ^ Lau H, Khosrawipour V, Kocbach P, Mikolajczyk A, Ichii H, Schubert J, et al. (June 2020). "Internationally lost COVID-19 cases". Journal of Microbiology, Immunology, and Infection = Wei Mian Yu Gan Ran Za Zhi. 53 (3): 454–458. doi:10.1016/j.jmii.2020.03.013. PMC 7102572. PMID 32205091.
- ^ Sevillano EG, Linde P, Vizoso S (23 March 2020). "640,000 rapid coronavirus tests arrive in Spain". El País English Edition. Retrieved 2 April 2020.
- ^ Parodi E, Jewkes S, Cha S, Park JM (12 March 2020). "Special Report: Italy and South Korea virus outbreaks reveal disparity in deaths and tactics". Reuters. Archived from the original on 12 March 2020. Retrieved 11 May 2022.
- ^ Kompaniyets L, Pennington AF, Goodman AB, Rosenblum HG, Belay B, Ko JY, et al. (July 2021). "Underlying Medical Conditions and Severe Illness Among 540,667 Adults Hospitalized With COVID-19, March 2020 – March 2021". Preventing Chronic Disease. 18. Centers for Disease Control and Prevention: E66. doi:10.5888/pcd18.210123. PMC 8269743. PMID 34197283.
- ^ Scott D (23 March 2020). "The Covid-19 risks for different age groups, explained". Vox. Retrieved 12 April 2020.
- ^ Bi Q, Wu Y, Mei S, Ye C, Zou X, Zhang Z, et al. (August 2020). "Epidemiology and transmission of COVID-19 in 391 cases and 1286 of their close contacts in Shenzhen, China: a retrospective cohort study". The Lancet. Infectious Diseases. 20 (8): 911–919. doi:10.1016/S1473-3099(20)30287-5. PMC 7185944. PMID 32353347.
- ^ Streeck H (9 April 2020). "Vorläufiges Ergebnis und Schlussfolgerungen der COVID-19 Case-Cluster-Study (Gemeinde Gangelt)" (PDF). Land NRW – State of North Rhine-Westphalia. Retrieved 13 April 2020.
- ^ Sutton D, Fuchs K, D'Alton M, Goffman D (May 2020). "Universal Screening for SARS-CoV-2 in Women Admitted for Delivery". The New England Journal of Medicine. 382 (22): 2163–2164. doi:10.1056/NEJMc2009316. PMC 7175422. PMID 32283004.
- ^ "Dutch study suggests 3% of population may have coronavirus antibodies". Reuters. 16 April 2020. Retrieved 20 April 2020.
- ^ "Interactive Serology Dashboard for Commercial Laboratory Surveys". Centres for Disease Control and Prevention. 21 July 2020. Retrieved 24 July 2020.
- ^ "Statement on the meeting of the International Health Regulations (2005) Emergency Committee regarding the outbreak of novel coronavirus 2019 (n-CoV) on 23 January 2020". World Health Organization (WHO). Retrieved 9 April 2020.
- ^ Sanche S, Lin YT, Xu C, Romero-Severson E, Hengartner N, Ke R (July 2020). "High Contagiousness and Rapid Spread of Severe Acute Respiratory Syndrome Coronavirus 2". Emerging Infectious Diseases. 26 (7): 1470–1477. doi:10.3201/eid2607.200282. PMC 7323562. PMID 32255761. S2CID 215410037.
- ^ "ArcGIS Dashboards". gisanddata.maps.arcgis.com. Retrieved 22 December 2021.
- ^ Kavya B, Mazumder A (14 April 2022). "Worldwide COVID cases surpass 500 mln as Omicron variant BA.2 surges". Reuters. Retrieved 21 April 2022.
- ^ a b "COVID-19 Results Briefing" (PDF). healthdata.org. Retrieved 7 February 2022.
- ^ a b "COVID Evaluation Model Estimates 57 Percent of World Population Infected at Least Once". MSN. Retrieved 7 February 2022.
- ^ a b c d e f Msemburi W, Karlinsky A, Knutson V, Aleshin-Guendel S, Chatterji S, Wakefield J (January 2023). "The WHO estimates of excess mortality associated with the COVID-19 pandemic". Nature. 613 (7942): 130–137. Bibcode:2023Natur.613..130M. doi:10.1038/s41586-022-05522-2. PMC 9812776. PMID 36517599.
- ^ "Coronavirus Death Toll Climbs in China, and a Lockdown Widens". The New York Times. 23 January 2020. Archived from the original on 6 February 2020. Retrieved 10 February 2020.
- ^ Multiple sources:
- "The Best Global Responses to the COVID-19 Pandemic". Time. Retrieved 18 August 2020.
- Barrio PL, del Javier M (11 May 2020). "Portugal and Spain: same peninsula, very different coronavirus impact". El País. Retrieved 25 May 2020.
- Johnson M (5 April 2020). "Fewer deaths in Veneto offer clues for fight against virus". Financial Times. Retrieved 25 May 2020.
- ^ Ritchie H, Roser M (25 March 2020). Chivers T (ed.). "What do we know about the risk of dying from COVID-19?". Our World in Data. Retrieved 28 March 2020.
- ^ "Principles of Epidemiology | Lesson 3 – Section 3". US Centers for Disease Control and Prevention (CDC). 18 February 2019. Retrieved 28 March 2020.
- ^ "Italy's coronavirus deaths could be underestimated in data: Official". Reuters. 31 March 2020.
- ^ "Coronavirus: Is Covid-19 really the cause of all the fatalities in Italy?". Stuff. 20 March 2020. Retrieved 16 April 2020.
- ^ Schultz T (22 April 2020). "Why Belgium's Death Rate Is So High: It Counts Lots Of Suspected COVID-19 Cases". NPR. Retrieved 25 April 2020.
- ^ a b "Tracking covid-19 excess deaths across countries". The Economist. Retrieved 6 November 2022.
- ^ "COVID-19 Projections". Institute for Health Metrics and Evaluation. Retrieved 20 January 2022.
- ^ a b Wang H, Paulson KR, Pease SA, Watson S, Comfort H, Zheng P, et al. (April 2022). "Estimating excess mortality due to the COVID-19 pandemic: a systematic analysis of COVID-19-related mortality, 2020–21". Lancet. 399 (10334): 1513–1536. doi:10.1016/S0140-6736(21)02796-3. PMC 8912932. PMID 35279232.
News article about the study: Adam D (March 2022). "COVID's true death toll: much higher than official records". Nature. 603 (7902): 562. Bibcode:2022Natur.603..562A. doi:10.1038/d41586-022-00708-0. PMID 35277684. S2CID 247407282. - ^ "What 'Excess Deaths' Do and Don't Tell Us About COVID-19". Reason. 29 April 2020. Retrieved 4 May 2020.
- ^ Naomi G, Cornish J, Stylianou N (5 May 2022). "Covid: World's true pandemic death toll nearly 15 million, says WHO". BBC News.
- ^ "Nearly 15 million deaths directly or indirectly linked to COVID-19 | UN News". news.un.org. 5 May 2022. Retrieved 4 February 2023.
- ^ "Nearly 15 million excess deaths occurred globally in 2020 and 2021". New Scientist. Retrieved 17 January 2023.
- ^ "Globale Übersterblichkeit durch COVID-19". www.sciencemediacenter.de. Retrieved 17 January 2023.
- ^ Rothan HA, Byrareddy SN (May 2020). "The epidemiology and pathogenesis of coronavirus disease (COVID-19) outbreak". Journal of Autoimmunity. 109: 102433. doi:10.1016/j.jaut.2020.102433. PMC 7127067. PMID 32113704.
- ^ Yanez ND, Weiss NS, Romand JA, Treggiari MM (November 2020). "COVID-19 mortality risk for older men and women". BMC Public Health. 20 (1): 1742. doi:10.1186/s12889-020-09826-8. PMC 7675386. PMID 33213391.
- ^ "People with Certain Medical Conditions". Centers for Disease Control and Prevention. 15 March 2021. Retrieved 19 March 2021.
- ^ a b c d Levin AT, Hanage WP, Owusu-Boaitey N, Cochran KB, Walsh SP, Meyerowitz-Katz G (December 2020). "Assessing the age specificity of infection fatality rates for COVID-19: systematic review, meta-analysis, and public policy implications". European Journal of Epidemiology. 35 (12): 1123–1138. doi:10.1007/s10654-020-00698-1. PMC 7721859. PMID 33289900.
- ^ Tate N. "What Changing Death Rates Tell Us About COVID-19". WebMD. Retrieved 19 September 2020.
- ^ a b "Estimating mortality from COVID-19". World Health Organization. 4 August 2020. Retrieved 21 September 2020.
- ^ "Coronavirus Disease 2019 (COVID-19)". Centers for Disease Control and Prevention. 11 February 2020. Retrieved 19 September 2020.
- ^ Multiple sources:
- Mallapaty S (June 2020). "How deadly is the coronavirus? Scientists are close to an answer". Nature. 582 (7813): 467–468. Bibcode:2020Natur.582..467M. doi:10.1038/d41586-020-01738-2. PMID 32546810. S2CID 219726496.
- Alwan NA, Burgess RA, Ashworth S, Beale R, Bhadelia N, Bogaert D, et al. (October 2020). "Scientific consensus on the COVID-19 pandemic: we need to act now". Lancet. 396 (10260): e71–e72. doi:10.1016/S0140-6736(20)32153-X. PMC 7557300. PMID 33069277.
- Meyerowitz-Katz G, Merone L (December 2020). "A systematic review and meta-analysis of published research data on COVID-19 infection fatality rates". International Journal of Infectious Diseases. 101: 138–148. doi:10.1016/j.ijid.2020.09.1464. PMC 7524446. PMID 33007452.
- ^ Yang W, Kandula S, Huynh M, Greene SK, Van Wye G, Li W, et al. (February 2021). "Estimating the infection-fatality risk of SARS-CoV-2 in New York City during the spring 2020 pandemic wave: a model-based analysis". The Lancet. Infectious Diseases. 21 (2): 203–212. doi:10.1016/S1473-3099(20)30769-6. PMC 7572090. PMID 33091374.
- ^ Pastor-Barriuso R, Pérez-Gómez B, Hernán MA, Pérez-Olmeda M, Yotti R, Oteo-Iglesias J, et al. (November 2020). "Infection fatality risk for SARS-CoV-2 in community dwelling population of Spain: nationwide seroepidemiological study". BMJ. 371: m4509. doi:10.1136/bmj.m4509. PMC 7690290. PMID 33246972.
- ^ O'Driscoll M, Ribeiro Dos Santos G, Wang L, Cummings DA, Azman AS, Paireau J, et al. (February 2021). "Age-specific mortality and immunity patterns of SARS-CoV-2". Nature. 590 (7844): 140–145. Bibcode:2021Natur.590..140O. doi:10.1038/s41586-020-2918-0. PMID 33137809. S2CID 226244375.
- ^ Pitlik SD (31 July 2020). "COVID-19 Compared to Other Pandemic Diseases". Rambam Maimonides Medical Journal. 11 (3): e0027. doi:10.5041/RMMJ.10418. PMC 7426550. PMID 32792043.
- ^ Spence ND, Sekercioglu F (31 August 2022). Indigenous Health and Well-Being in the COVID-19 Pandemic. Taylor & Francis. ISBN 978-1-000-64420-3. Retrieved 12 May 2023.
- ^ Hauser A, Counotte MJ, Margossian CC, Konstantinoudis G, Low N, Althaus CL, et al. (July 2020). "Estimation of SARS-CoV-2 mortality during the early stages of an epidemic: A modeling study in Hubei, China, and six regions in Europe". PLOS Medicine. 17 (7): e1003189. doi:10.1371/journal.pmed.1003189. PMC 7386608. PMID 32722715.
- ^ Lazzerini M, Putoto G (May 2020). "COVID-19 in Italy: momentous decisions and many uncertainties". The Lancet. Global Health. 8 (5): e641–e642. doi:10.1016/S2214-109X(20)30110-8. PMC 7104294. PMID 32199072.
- ^ "Weekly epidemiological update on COVID-19 – 25 May 2023". www.who.int. Retrieved 26 May 2023.
- ^ a b "Statement on the update of WHO's working definitions and tracking system for SARS-CoV-2 variants of concern and variants of interest". www.who.int. Retrieved 26 May 2023.
- ^ "Coronavirus Disease 2019 (COVID-19)". Centers for Disease Control and Prevention. 11 February 2020. Retrieved 30 October 2022.
- ^ "Tracking SARS-CoV-2 variants". www.who.int. Retrieved 7 November 2022.
- ^ a b "Symptoms of Coronavirus". U.S. Centers for Disease Control and Prevention (CDC). 22 February 2021. Archived from the original on 4 March 2021. Retrieved 4 March 2021.
- ^ Grant MC, Geoghegan L, Arbyn M, Mohammed Z, McGuinness L, Clarke EL, et al. (23 June 2020). "The prevalence of symptoms in 24,410 adults infected by the novel coronavirus (SARS-CoV-2; COVID-19): A systematic review and meta-analysis of 148 studies from 9 countries". PLOS ONE. 15 (6): e0234765. Bibcode:2020PLoSO..1534765G. doi:10.1371/journal.pone.0234765. PMC 7310678. PMID 32574165. S2CID 220046286.
- ^ "COVID-19/csse_covid_19_data/csse_covid_19_time_series at master · CSSEGISandData/COVID-19". GitHub. Retrieved 18 January 2022.
- ^ Krishnan A, Hamilton JP, Alqahtani SA, Woreta TA (January 2021). "COVID-19: An overview and a clinical update". World Journal of Clinical Cases. 9 (1): 8–23. doi:10.12998/wjcc.v9.i1.8. PMC 7809683. PMID 33511168.
- ^ Docherty AB, Harrison EM, Green CA, Hardwick HE, Pius R, Norman L, et al. (May 2020). "Features of 20 133 UK patients in hospital with covid-19 using the ISARIC WHO Clinical Characterisation Protocol: prospective observational cohort study". BMJ. 369: m1985. doi:10.1136/bmj.m1985. PMC 7243036. PMID 32444460.
- ^ Niazkar HR, Zibaee B, Nasimi A, Bahri N (July 2020). "The neurological manifestations of COVID-19: a review article". Neurological Sciences. 41 (7): 1667–1671. doi:10.1007/s10072-020-04486-3. PMC 7262683. PMID 32483687.
- ^ a b Wang CC, Prather KA, Sznitman J, Jimenez JL, Lakdawala SS, Tufekci Z, et al. (August 2021). "Airborne transmission of respiratory viruses". Science. 373 (6558). doi:10.1126/science.abd9149. PMC 8721651. PMID 34446582.
- ^ Greenhalgh T, Jimenez JL, Prather KA, Tufekci Z, Fisman D, Schooley R (May 2021). "Ten scientific reasons in support of airborne transmission of SARS-CoV-2". Lancet. 397 (10285): 1603–1605. doi:10.1016/s0140-6736(21)00869-2. PMC 8049599. PMID 33865497.
- ^ Bourouiba L (July 2021). "Fluid Dynamics of Respiratory Infectious Diseases". Annual Review of Biomedical Engineering. 23 (1): 547–577. doi:10.1146/annurev-bioeng-111820-025044. hdl:1721.1/131115. PMID 34255991. S2CID 235823756.
- ^ Stadnytskyi V, Bax CE, Bax A, Anfinrud P (June 2020). "The airborne lifetime of small speech droplets and their potential importance in SARS-CoV-2 transmission". Proceedings of the National Academy of Sciences of the United States of America. 117 (22): 11875–11877. Bibcode:2020PNAS..11711875S. doi:10.1073/pnas.2006874117. PMC 7275719. PMID 32404416.
- ^ Miller SL, Nazaroff WW, Jimenez JL, Boerstra A, Buonanno G, Dancer SJ, et al. (March 2021). "Transmission of SARS-CoV-2 by inhalation of respiratory aerosol in the Skagit Valley Chorale superspreading event". Indoor Air. 31 (2): 314–323. Bibcode:2021InAir..31..314M. doi:10.1111/ina.12751. PMC 7537089. PMID 32979298.
- ^ Fox D (January 2020). "What you need to know about the novel coronavirus". Nature. doi:10.1038/d41586-020-00209-y. PMID 33483684. S2CID 213064026.
- ^ V'kovski P, Kratzel A, Steiner S, Stalder H, Thiel V (March 2021). "Coronavirus biology and replication: implications for SARS-CoV-2". Nature Reviews. Microbiology. 19 (3): 155–170. doi:10.1038/s41579-020-00468-6. PMC 7592455. PMID 33116300.
- ^ Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, et al. (February 2020). "A Novel Coronavirus from Patients with Pneumonia in China, 2019". The New England Journal of Medicine. 382 (8): 727–733. doi:10.1056/NEJMoa2001017. PMC 7092803. PMID 31978945.
- ^ "2019 Novel Coronavirus (2019-nCoV) Situation Summary". U.S. Centers for Disease Control and Prevention (CDC). 30 January 2020. Archived from the original on 26 January 2020. Retrieved 30 January 2020.
- ^ "Coronavirus disease (COVID-19) technical guidance: Laboratory testing for 2019-nCoV in humans". World Health Organization (WHO). Archived from the original on 15 March 2020. Retrieved 14 March 2020.
- ^ Bullard J, Dust K, Funk D, Strong JE, Alexander D, Garnett L, et al. (December 2020). "Predicting Infectious Severe Acute Respiratory Syndrome Coronavirus 2 From Diagnostic Samples". Clinical Infectious Diseases. 71 (10): 2663–2666. doi:10.1093/cid/ciaa638. PMC 7314198. PMID 32442256.
- ^ "Interim Guidelines for Collecting, Handling, and Testing Clinical Specimens from Persons for Coronavirus Disease 2019 (COVID-19)". U.S. Centers for Disease Control and Prevention (CDC). 11 February 2020. Archived from the original on 4 March 2020. Retrieved 26 March 2020.
- ^ "Real-Time RT-PCR Panel for Detection 2019-nCoV". U.S. Centers for Disease Control and Prevention (CDC). 29 January 2020. Archived from the original on 30 January 2020. Retrieved 1 February 2020.
- ^ "Laboratory testing for 2019 novel coronavirus (2019-nCoV) in suspected human cases". World Health Organization (WHO). Archived from the original on 17 March 2020. Retrieved 13 March 2020.
- ^ "COVID-19: How to protect yourself and others". U.S. Centers for Disease Control and Prevention (CDC). 26 January 2023. Retrieved 3 February 2023.
- ^ "Advice for the public on COVID-19 – World Health Organization". www.who.int. Retrieved 27 May 2023.
- ^ "Isolation". Centers for Disease Control and Prevention. 11 May 2023. Retrieved 27 May 2023.
- ^ "Infection prevention and control and preparedness for COVID-19 in healthcare settings – sixth update". www.ecdc.europa.eu. 9 February 2021. Retrieved 27 May 2023.
- ^ "People with symptoms of a respiratory infection including COVID-19". GOV.UK. 10 June 2022. Retrieved 27 May 2023.
- ^ Li YD, Chi WY, Su JH, Ferrall L, Hung CF, Wu TC (December 2020). "Coronavirus vaccine development: from SARS and MERS to COVID-19". Journal of Biomedical Science. 27 (1): 104. doi:10.1186/s12929-020-00695-2. PMC 7749790. PMID 33341119.
- ^ Subbarao K (July 2021). "The success of SARS-CoV-2 vaccines and challenges ahead". Cell Host & Microbe. 29 (7): 1111–1123. doi:10.1016/j.chom.2021.06.016. PMC 8279572. PMID 34265245.
- ^ Vergano D (5 June 2021). "COVID-19 Vaccines Work Way Better Than We Had Ever Expected. Scientists Are Still Figuring Out Why". BuzzFeed News. Retrieved 24 June 2021.
- ^ Mallapaty S, Callaway E, Kozlov M, Ledford H, Pickrell J, Van Noorden R (December 2021). "How COVID vaccines shaped 2021 in eight powerful charts". Nature. 600 (7890): 580–583. Bibcode:2021Natur.600..580M. doi:10.1038/d41586-021-03686-x. PMID 34916666. S2CID 245262732.
- ^ Holder J (29 January 2021). "Tracking Coronavirus Vaccinations Around the World". The New York Times. ISSN 0362-4331. Retrieved 23 December 2021.
- ^ The Visual and Data Journalism Team. "Covid vaccines: How fast is progress around the world?". BBC News. Retrieved 18 August 2021.
- ^ Watson OJ, Barnsley G, Toor J, Hogan AB, Winskill P, Ghani AC (June 2022). "Global impact of the first year of COVID-19 vaccination: a mathematical modelling study". The Lancet Infectious Diseases. 22 (9): 1293–1302. doi:10.1016/s1473-3099(22)00320-6. PMC 9225255. PMID 35753318.
- ^ "COVID-19 vaccines saved nearly 20 million lives in a year, study says". CBS News. 24 June 2022. Archived from the original on 29 June 2022. Retrieved 27 June 2022.
- ^ Hammershaimb EA, Tapia MD (31 December 2023). "Can protein vaccines for COVID-19 win over the vaccine-hesitant?". Expert Review of Vaccines. 22 (1): 210–212. doi:10.1080/14760584.2023.2182293. ISSN 1476-0584. PMID 36803364. S2CID 257069394. Retrieved 27 May 2023.
- ^ Parums DV (1 March 2022). "Editorial: First Approval of the Protein-Based Adjuvanted Nuvaxovid (NVX-CoV2373) Novavax Vaccine for SARS-CoV-2 Could Increase Vaccine Uptake and Provide Immune Protection from Viral Variants". Medical Science Monitor. 28: e936523. doi:10.12659/MSM.936523. PMC 8897963. PMID 35228506.
- ^ "WHO releases first data on global vaccine market since COVID-19". www.who.int. Retrieved 12 November 2022.
- ^ Graham F (1 November 2022). "Daily briefing: China reports first roll-out of inhalable COVID-19 vaccine". Nature. Springer Nature. doi:10.1038/d41586-022-03548-0. Retrieved 27 May 2023.
- ^ a b c Siemieniuk RA, Bartoszko JJ, Ge L, Zeraatkar D, Izcovich A, Kum E, et al. (31 March 2021). "Drug treatments for covid-19: living systematic review and network meta-analysis". BMJ. 370: m2980. doi:10.1136/bmj.m2980. PMC 7390912. PMID 32732190.
- ^ a b "CDC Museum COVID-19 Timeline". Centers for Disease Control and Prevention. 15 March 2023. Retrieved 27 May 2023.
- ^ Priyan V (17 December 2021). "EMA CHMP advises use of Pfizer's Covid-19 oral antiviral Paxlovid". Pharmaceutical Technology. Archived from the original on 18 December 2021. Retrieved 18 December 2021.
- ^ "Paxlovid LOA 12222021 | FDA". www.fda.gov. Retrieved 23 December 2021.
- ^ Islam MA, Kundu S, Alam SS, Hossan T, Kamal MA, Hassan R (6 April 2021). "Prevalence and characteristics of fever in adult and paediatric patients with coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis of 17515 patients". PLOS ONE. 16 (4): e0249788. Bibcode:2021PLoSO..1649788I. doi:10.1371/journal.pone.0249788. PMC 8023501. PMID 33822812. S2CID 233173405.
- ^ Multiple sources:
- Wang Y, Wang Y, Chen Y, Qin Q (June 2020). "Unique epidemiological and clinical features of the emerging 2019 novel coronavirus pneumonia (COVID-19) implicate special control measures". Journal of Medical Virology. 92 (6): 568–576. doi:10.1002/jmv.25748. PMC 7228347. PMID 32134116.
- Martel J, Ko YF, Young JD, Ojcius DM (May 2020). "Could nasal nitric oxide help to mitigate the severity of COVID-19?". Microbes and Infection. 22 (4–5): 168–171. doi:10.1016/j.micinf.2020.05.002. PMC 7200356. PMID 32387333.
- "Coronavirus recovery: breathing exercises". hopkinsmedicine.org. Johns Hopkins Medicine. Retrieved 30 July 2020.
- ^ Wang L, Wang Y, Ye D, Liu Q (June 2020). "Review of the 2019 novel coronavirus (SARS-CoV-2) based on current evidence". International Journal of Antimicrobial Agents. 55 (6): 105948. doi:10.1016/j.ijantimicag.2020.105948. PMC 7156162. PMID 32201353.
- ^ Multiple sources:
- Fisher D, Heymann D (February 2020). "Q&A: The novel coronavirus outbreak causing COVID-19". BMC Medicine. 18 (1): 57. doi:10.1186/s12916-020-01533-w. PMC 7047369. PMID 32106852.
- Liu K, Fang YY, Deng Y, Liu W, Wang MF, Ma JP, et al. (May 2020). "Clinical characteristics of novel coronavirus cases in tertiary hospitals in Hubei Province". Chinese Medical Journal. 133 (9): 1025–1031. doi:10.1097/CM9.0000000000000744. PMC 7147277. PMID 32044814.
- Wang T, Du Z, Zhu F, Cao Z, An Y, Gao Y, et al. (March 2020). "Comorbidities and multi-organ injuries in the treatment of COVID-19". Lancet. 395 (10228). Elsevier BV: e52. doi:10.1016/s0140-6736(20)30558-4. PMC 7270177. PMID 32171074.
- ^ Multiple sources:
- "Update to living WHO guideline on drugs for covid-19". BMJ. 371: m4475. November 2020. doi:10.1136/bmj.m4475. PMID 33214213. S2CID 227059995.
- "Q&A: Dexamethasone and COVID-19". World Health Organization. Retrieved 11 July 2020.
- "Home". National COVID-19 Clinical Evidence Taskforce. Retrieved 11 July 2020.
- ^ "COVID-19 Treatment Guidelines". nih.gov. National Institutes of Health. Retrieved 18 January 2021.
- ^ Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, et al. (April 2020). "Clinical Characteristics of Coronavirus Disease 2019 in China". The New England Journal of Medicine. 382 (18). Massachusetts Medical Society: 1708–1720. doi:10.1056/nejmoa2002032. PMC 7092819. PMID 32109013.
- ^ Henry BM (April 2020). "COVID-19, ECMO, and lymphopenia: a word of caution". The Lancet. Respiratory Medicine. 8 (4). Elsevier BV: e24. doi:10.1016/s2213-2600(20)30119-3. PMC 7118650. PMID 32178774.
- ^ Kim PS, Read SW, Fauci AS (December 2020). "Therapy for Early COVID-19: A Critical Need". JAMA. 324 (21). American Medical Association (AMA): 2149–2150. doi:10.1001/jama.2020.22813. PMID 33175121. S2CID 226301949.
- ^ "COVID-19 Treatment Guidelines". nih.gov. National Institutes of Health. Retrieved 18 January 2021./
- ^ Hsu J (November 2020). "Covid-19: What now for remdesivir?". BMJ. 371: m4457. doi:10.1136/bmj.m4457. PMID 33214186. S2CID 227060756.
- ^ Doshi P (October 2020). "Will covid-19 vaccines save lives? Current trials aren't designed to tell us". BMJ. 371: m4037. doi:10.1136/bmj.m4037. PMID 33087398. S2CID 224817161.
- ^ Baranovskii DS, Klabukov ID, Krasilnikova OA, Nikogosov DA, Polekhina NV, Baranovskaia DR, et al. (January 2021). "Prolonged prothrombin time as an early prognostic indicator of severe acute respiratory distress syndrome in patients with COVID-19 related pneumonia". Current Medical Research and Opinion. 37 (1): 21–25. doi:10.1080/03007995.2020.1853510. PMC 7738209. PMID 33210948.
- ^ Christensen B, Favaloro EJ, Lippi G, Van Cott EM (October 2020). "Hematology Laboratory Abnormalities in Patients with Coronavirus Disease 2019 (COVID-19)". Seminars in Thrombosis and Hemostasis. 46 (7): 845–849. doi:10.1055/s-0040-1715458. PMC 7645834. PMID 32877961.
- ^ Ledford H (June 2022). "How common is long COVID? Why studies give different answers". Nature. 606 (7916): 852–853. Bibcode:2022Natur.606..852L. doi:10.1038/d41586-022-01702-2. PMID 35725828. S2CID 249887289. Archived from the original on 8 October 2022. Retrieved 13 August 2022.
- ^ "Post-COVID Conditions". Centers for Disease Control and Prevention. 14 March 2024. Archived from the original on 6 May 2022. Retrieved 28 May 2024.
- ^ "Researching long COVID: addressing a new global health challenge". NIHR Evidence. 12 May 2022. doi:10.3310/nihrevidence_50331. S2CID 249942230.
- ^ "Clinical characteristics of COVID-19". www.ecdc.europa.eu. 10 June 2020. Retrieved 26 May 2023.
- ^ Leviner S (7 May 2021). "Recognizing the Clinical Sequelae of COVID-19 in Adults: COVID-19 Long-Haulers". The Journal for Nurse Practitioners. 17 (8): 946–949. doi:10.1016/j.nurpra.2021.05.003. ISSN 1555-4155. PMC 8103144. PMID 33976591.
- ^ "Nearly half of people infected with COVID-19 experienced some 'long COVID' symptoms, study finds". University of Michigan. Retrieved 15 May 2022.
- ^ Chen C, Haupert SR, Zimmermann L, Shi X, Fritsche LG, Mukherjee B (16 April 2022). "Global Prevalence of Post COVID-19 Condition or Long COVID: A Meta-Analysis and Systematic Review". The Journal of Infectious Diseases. 226 (9): 1593–1607. doi:10.1093/infdis/jiac136. PMC 9047189. PMID 35429399.
- ^ a b c Anderson RM, Heesterbeek H, Klinkenberg D, Hollingsworth TD (March 2020). "How will country-based mitigation measures influence the course of the COVID-19 epidemic?". Lancet. 395 (10228): 931–934. doi:10.1016/S0140-6736(20)30567-5. PMC 7158572. PMID 32164834.
A key issue for epidemiologists is helping policy makers decide the main objectives of mitigation—e.g. minimising morbidity and associated mortality, avoiding an epidemic peak that overwhelms health-care services, keeping the effects on the economy within manageable levels, and flattening the epidemic curve to wait for vaccine development and manufacture on scale and antiviral drug therapies.
- ^ Qualls N, Levitt A, Kanade N, Wright-Jegede N, Dopson S, Biggerstaff M, et al. (April 2017). "Community Mitigation Guidelines to Prevent Pandemic Influenza – United States, 2017". MMWR. Recommendations and Reports. 66 (1): 1–34. doi:10.15585/mmwr.rr6601a1. PMC 5837128. PMID 28426646.
- ^ Barclay E, Scott D, Animashaun A (7 April 2020). "The US doesn't just need to flatten the curve. It needs to "raise the line."". Vox. Archived from the original on 7 April 2020.
- ^ a b Anna Llupià, Rodríguez-Giralt, Anna Fité, Lola Álamo, Laura de la Torre, Ana Redondo, Mar Callau and Caterina Guinovart (2020) What Is a Zero-COVID Strategy Archived 3 January 2022 at the Wayback Machine, Barcelona Institute for Global Health – COVID-19 & response strategy. "The strategy of control and maximum suppression (zero-COVID) has been implemented successfully in a number of countries. The objective of this strategy is to keep transmission of the virus as close to zero as possible and ultimately to eliminate it entirely from particular geographical areas. The strategy aims to increase the capacity to identify and trace chains of transmission and to identify and manage outbreaks, while also integrating economic, psychological, social and healthcare support to guarantee the isolation of cases and contacts. This approach is also known as "Find, Test, Trace, Isolate and Support" (FTTIS)"
- ^ Livermore D (28 March 2021). "'Zero Covid' – an impossible dream". HART – Health Advisory & Recovery Team. Archived from the original on 2 January 2022. Retrieved 2 January 2022.
- ^ Bhopal RS (September 2020). "To achieve "zero covid" we need to include the controlled, careful acquisition of population (herd) immunity". BMJ. 370: m3487. doi:10.1136/bmj.m3487. eISSN 1756-1833. PMID 32907816. S2CID 221538577.
- ^ Phillips N (February 2021). "The coronavirus is here to stay – here's what that means". Nature. 590 (7846): 382–384. Bibcode:2021Natur.590..382P. doi:10.1038/d41586-021-00396-2. PMID 33594289. S2CID 231945680.
- ^ "Fever Screening | IntelliSEC | Durban, Johannesburg, Cape Town". IntelliSEC.
- ^ Li Z, Chen Q, Feng L, Rodewald L, Xia Y, Yu H, et al. (July 2020). "Active case finding with case management: the key to tackling the COVID-19 pandemic". Lancet. 396 (10243): 63–70. doi:10.1016/S0140-6736(20)31278-2. PMC 7272157. PMID 32505220.
- ^ "Impact of non-pharmaceutical interventions (NPIs) to reduce COVID19 mortality and healthcare demand" (PDF). Imperial College COVID-19 Response Team. 16 March 2020.
- ^ US Census Bureau. "Those Who Switched to Telework Have Higher Income, Education and Better Health". Census.gov. Retrieved 25 December 2021.
- ^ "Community Mitigation Guidelines to Prevent Pandemic Influenza – United States, 2017". Recommendations and Reports. 66 (1). 12 April 2017.
- ^ Qin A (7 March 2020). "China May Be Beating the Coronavirus, at a Painful Cost". The New York Times.
- ^ McCurry J, Ratcliffe R, Davidson H (11 March 2020). "Mass testing, alerts and big fines: the strategies used in Asia to slow coronavirus". The Guardian.
- ^ "Expert interview: What is contact tracing?". Blog: Public Health Matters. Public Health England, Government of the United Kingdom. 13 February 2020. Retrieved 28 February 2020.
- ^ Webb G, Browne C, Huo X, Seydi O, Seydi M, Magal P (30 January 2015). "A model of the 2014 ebola epidemic in west Africa with contact tracing". PLOS Currents. 7: ecurrents.outbreaks.846b2a31ef37018b7d1126a9c8adf22a. doi:10.1371/currents.outbreaks.846b2a31ef37018b7d1126a9c8adf22a (inactive 1 July 2024). ISSN 2157-3999. PMC 4323422. PMID 25685636.
((cite journal)): CS1 maint: DOI inactive as of July 2024 (link) - ^ Ingram D, Ward J (7 April 2020). "Behind the global efforts to make a privacy-first coronavirus tracking app". NBC News. Retrieved 10 April 2020.
- ^ "Apple and Google are launching a joint COVID-19 tracing tool for iOS and Android". TechCrunch. 10 April 2020. Retrieved 10 April 2020.
- ^ "Privacy-Preserving Contact Tracing". Apple. 10 April 2020.
- ^ "Palantir provides COVID-19 tracking software to CDC and NHS, pitches European health agencies". TechCrunch. Retrieved 22 April 2020.
- ^ a b "Hospital readiness checklist for COVID-19". World Health Organization. 25 March 2020. Retrieved 27 March 2020.
- ^ Checklist for hospitals preparing for the reception and care of coronavirus 2019 (COVID-19) patients (Report). European Centre for Disease Prevention and Control. 26 February 2020. Retrieved 27 March 2020.
- ^ Multiple sources:
- Smith AC, Thomas E, Snoswell CL, Haydon H, Mehrotra A, Clemensen J, et al. (June 2020). "Telehealth for global emergencies: Implications for coronavirus disease 2019 (COVID-19)". Journal of Telemedicine and Telecare. 26 (5): 309–313. doi:10.1177/1357633x20916567. PMC 7140977. PMID 32196391.
- Ohannessian R, Duong TA, Odone A (April 2020). "Global Telemedicine Implementation and Integration Within Health Systems to Fight the COVID-19 Pandemic: A Call to Action". JMIR Public Health and Surveillance. 6 (2): e18810. doi:10.2196/18810. PMC 7124951. PMID 32238336.
- Keshvardoost S, Bahaadinbeigy K, Fatehi F (July 2020). "Role of Telehealth in the Management of COVID-19: Lessons Learned from Previous SARS, MERS, and Ebola Outbreaks". Telemedicine Journal and e-Health. 26 (7): 850–852. doi:10.1089/tmj.2020.0105. PMID 32329659. S2CID 216111135.
- ^ Temple J. "How 3D printing could save lives in the coronavirus outbreak". MIT Technology Review. Retrieved 5 April 2020.
- ^ Tibken S. "3D printing may help supply more essential coronavirus medical gear". CNET. Retrieved 5 April 2020.
- ^ Multiple sources:
- "[Updating] Italian hospital saves Covid-19 patients lives by 3D printing valves for reanimation devices". 3D Printing Media Network. 14 March 2020. Retrieved 20 March 2020.
- Peters J (17 March 2020). "Volunteers produce 3D-printed valves for life-saving coronavirus treatments". The Verge. Retrieved 20 March 2020.
- "Engineers 3D-print patented valves for free to save coronavirus patients in Italy". Global News.
- ^ Cavalcanti G, Cocciole C, Cole C, Forgues A, Jaqua V, Jones-Davis D, et al. (2021). Design, Make, Protect: A report on the Open Source Maker and Manufacturer Response to the COVID-19 PPE Crisis (PDF). Open Source Medical Supplies & Nation of Makers. pp. 18–22. Retrieved 17 June 2021.
- ^ Dyer O (August 2021). "Covid-19: Delta infections threaten herd immunity vaccine strategy". BMJ. 374: n1933. doi:10.1136/bmj.n1933. PMID 34340962. S2CID 236778544.
- ^ Katella K (13 August 2021). "5 Things To Know About the Delta Variant". Yale Medicine News. Retrieved 18 August 2021.
- ^ Ma J (13 March 2020). "China's first confirmed Covid-19 case traced back to November 17". South China Morning Post. Archived from the original on 13 March 2020.
- ^ Lu Z(. 最早上报疫情的她,怎样发现这种不一样的肺炎. 中国网新闻 (in Chinese (China)). Beijing. Archived from the original on 2 March 2020. Retrieved 11 February 2020.
- ^ "China delayed releasing coronavirus info, frustrating WHO". Associated Press. 2 June 2020. Archived from the original on 25 October 2021. Retrieved 26 October 2021.
- ^ Gao Y( (26 February 2020). 独家 | 新冠病毒基因测序溯源:警报是何时拉响的 [Exclusive | Tracing the New Coronavirus gene sequencing: when did the alarm sound]. Caixin (in Chinese). Archived from the original on 27 February 2020. Retrieved 1 March 2020.
- ^ "'Hero who told the truth': Chinese rage over coronavirus death of whistleblower doctor". The Guardian. 7 February 2020.
- ^ Kuo L (11 March 2020). "Coronavirus: Wuhan doctor speaks out against authorities". The Guardian. London.
- ^ "Undiagnosed pneumonia – China (HU): RFI". Promed-Mail. ProMED. 30 December 2019. Retrieved 7 May 2020.
- ^ a b "Novel Coronavirus". World Health Organization (WHO). Archived from the original on 22 January 2020. Retrieved 6 February 2020.
"COVID-19 timeline in the Western Pacific". World Health Organization (WHO). 18 May 2020. Archived from the original on 23 May 2020. Retrieved 6 July 2020. - ^ 武汉市卫健委关于当前我市肺炎疫情的情况通报. WJW.Wuhan.gov.cn (in Chinese). Wuhan Municipal Health Commission. 31 December 2019. Archived from the original on 9 January 2020. Retrieved 8 February 2020.
- ^ a b "Mystery pneumonia virus probed in China". BBC News. 3 January 2020. Archived from the original on 5 January 2020. Retrieved 29 January 2020.
- ^ a b "Novel Coronavirus (2019-nCoV) SITUATION REPORT – 1" (PDF). World Health Organization. 20 January 2020. Retrieved 7 June 2021.
- ^ "[The epidemiological characteristics of an outbreak of 2019 novel coronavirus diseases (COVID-19) in China]". Zhonghua Liu Xing Bing Xue Za Zhi = Zhonghua Liuxingbingxue Zazhi (in Chinese). 41 (2): 145–151. February 2020. doi:10.3760/cma.j.issn.0254-6450.2020.02.003. PMID 32064853. S2CID 211133882.
- ^ Areddy JT (26 May 2020). "China Rules Out Animal Market and Lab as Coronavirus Origin". The Wall Street Journal. Retrieved 29 May 2020.
- ^ Li Q, Guan X, Wu P, Wang X, Zhou L, Tong Y, et al. (March 2020). "Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia". The New England Journal of Medicine. 382 (13): 1199–1207. doi:10.1056/NEJMoa2001316. PMC 7121484. PMID 31995857.
- ^ WHO–China Joint Mission (24 February 2020). "Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19)" (PDF). World Health Organization (WHO). Retrieved 8 March 2020.
- ^ Enserink M (29 March 2023). "Dispute simmers over who first shared SARS-CoV-2's genome". Science. Archived from the original on 30 March 2023. Retrieved 20 May 2023.
- ^ The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team (17 February 2020). "The Epidemiological Characteristics of an Outbreak of 2019 Novel Coronavirus Diseases (COVID-19) – China, 2020". China CDC Weekly. 2 (8): 113–122. doi:10.46234/ccdcw2020.032. PMC 8392929. PMID 34594836. Retrieved 18 March 2020.
- ^ Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. (February 2020). "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China". Lancet. 395 (10223): 497–506. doi:10.1016/S0140-6736(20)30183-5. PMC 7159299. PMID 31986264.
- ^ Horton R (18 March 2020). "Scientists have been sounding the alarm on coronavirus for months. Why did Britain fail to act?". The Guardian. Retrieved 23 April 2020.
- ^ Wu JT, Leung K, Leung GM (February 2020). "Nowcasting and forecasting the potential domestic and international spread of the 2019-nCoV outbreak originating in Wuhan, China: a modelling study". Lancet. 395 (10225): 689–697. doi:10.1016/S0140-6736(20)30260-9. PMC 7159271. PMID 32014114.
- ^ "Novel Coronavirus(2019-nCoV): Situation Report – 10" (PDF). World Health Organization (WHO). 30 January 2020. Retrieved 14 October 2020.
- ^ "Statement on the second meeting of the International Health Regulations (2005) Emergency Committee regarding the outbreak of novel coronavirus (2019-nCoV)". World Health Organization (WHO). 30 January 2020. Archived from the original on 31 January 2020. Retrieved 30 January 2020.
- ^ Durrheim DN, Gostin LO, Moodley K (August 2020). "When does a major outbreak become a Public Health Emergency of International Concern?". The Lancet Infectious Diseases. 20 (8): 887–889. doi:10.1016/S1473-3099(20)30401-1. PMC 7237181. PMID 32442526.
- ^ a b Severgnini C (30 January 2020). "Coronavirus, primi due casi in Italia: sono due turisti cinesi". Corriere della Sera (in Italian). Retrieved 29 May 2023.
- ^ "Coronavirus: Number of COVID-19 deaths in Italy surpasses China as total reaches 3,405". Sky News. Retrieved 7 May 2020.
- ^ McNeil Jr DG (26 March 2020). "The U.S. Now Leads the World in Confirmed Coronavirus Cases". The New York Times. Retrieved 27 March 2020.
- ^ "Studies Show N.Y. Outbreak Originated in Europe". The New York Times. 8 April 2020.
- ^ Irish J (4 May 2020). Lough R, Graff P (eds.). "After retesting samples, French hospital discovers COVID-19 case from December". Reuters. Retrieved 4 May 2020.
- ^ Deslandes A, Berti V, Tandjaoui-Lambotte Y, Alloui C, Carbonnelle E, Zahar JR, et al. (June 2020). "SARS-CoV-2 was already spreading in France in late December 2019". International Journal of Antimicrobial Agents. 55 (6): 106006. doi:10.1016/j.ijantimicag.2020.106006. PMC 7196402. PMID 32371096.
- ^ Bean A (22 April 2020). "2 died with coronavirus weeks before 1st U.S. virus death". PBS NewsHour. Retrieved 29 May 2023.
- ^ "One in 10 worldwide may have had Covid – WHO". BBC. 5 October 2020. Retrieved 14 October 2020.
- ^ Boseley S, Olterman P (9 November 2020). "Covid-19 vaccine candidate is 90% effective, says Pfizer". The Guardian. ISSN 0261-3077. Retrieved 9 November 2020.
- ^ Linnane C. "Novavax wins FDA fast track designation for COVID-19 vaccine candidate". MarketWatch. Retrieved 9 November 2020.
- ^ "PHE investigating a novel strain of COVID-19". GOV.UK. 14 December 2020. Retrieved 15 December 2020.
- ^ Le Page M, McNamara A. "Alpha covid-19 variant (B.1.1.7)". New Scientist. Retrieved 29 May 2023.
- ^ Azar A (4 February 2020). "Notice of Declaration under the Public Readiness and Emergency Preparedness Act for medical countermeasures against COVID-19". Archived from the original on 25 April 2020. Retrieved 22 April 2020.
- ^ Sigalos M (17 December 2020). "You can't sue Pfizer or Moderna if you have severe Covid vaccine side effects. The government likely won't compensate you for damages either". CNBC. Retrieved 29 May 2023.
- ^ Hauck G (15 January 2021). "More contagious COVID-19 strain identified in 3 states and 33 countries: What to know". USA Today. Retrieved 2 January 2021.
- ^ "Genomic characterisation of an emergent SARS-CoV-2 lineage in Manaus: preliminary findings". Virological. 12 January 2021. Retrieved 6 May 2021.
- ^ Nedelman M (28 January 2021). "South Carolina detects first US cases of coronavirus strain first seen in South Africa". CNN. Retrieved 29 January 2021.
- ^ Johnson CY. "Novavax vaccine protects against coronavirus in variant hot spots but proved less effective against strain in South Africa". The Washington Post. Retrieved 29 January 2021.
- ^ "COVID variants test immunity, NIH chief and China's mixed vaccine data". Nature. 589 (7843): 497. 27 January 2021. Bibcode:2021Natur.589..497.. doi:10.1038/d41586-021-00186-w.
- ^ "AstraZeneca defends COVID vaccine as handful of nations pause use over fear of blood clots". CBS News. Retrieved 14 March 2021.
- ^ "WHO renews backing for AstraZeneca's COVID-19 jab as European countries resume vaccinations". SBS News. 20 March 2021. Retrieved 21 March 2021.
- ^ Callaway E (July 2021). "Delta coronavirus variant: scientists brace for impact". Nature. 595 (7865): 17–18. Bibcode:2021Natur.595...17C. doi:10.1038/d41586-021-01696-3. PMID 34158664. S2CID 235609029.
- ^ "Germany Advises Against Moderna Covid Vaccine For People Under 30". NDTV.com. Retrieved 23 December 2021.
- ^ Fink J (22 December 2021). "Omicron variant that may resist vaccines found in all U.S. states". Newsweek. Retrieved 25 December 2021.
- ^ Karim SS, Karim QA (December 2021). "Omicron SARS-CoV-2 variant: a new chapter in the COVID-19 pandemic". Lancet. 398 (10317): 2126–2128. doi:10.1016/S0140-6736(21)02758-6. PMC 8640673. PMID 34871545.
- ^ "Europe Tops 100 Million Coronavirus Cases in Pandemic". VOA. January 2022. Retrieved 2 January 2022.
- ^ Kmietowicz Z (13 January 2022). "Covid-19: WHO recommends baricitinib and sotrovimab to treat patients". BMJ. 376: o97. doi:10.1136/bmj.o97. PMID 35027362. S2CID 245907930. Retrieved 29 May 2023.
- ^ McPhillips D (7 March 2022). "Global Covid-19 deaths surpass 6 million". CNN. Retrieved 9 March 2022.
- ^ "BA.5, now dominant U.S. variant, may pose the biggest threat to immune protection yet". NBC News. 7 July 2022. Retrieved 13 August 2022.
- ^ "The end of the COVID-19 pandemic is in sight: WHO". 14 September 2022.
- ^ Mishra M (14 September 2022). "End of COVID pandemic is 'in sight' -WHO chief". Reuters.
- ^ "WHO says 'end is in sight' for the Covid pandemic as global deaths hit lowest since March 2020". NBC News.
- ^ "The end of the pandemic is in sight, WHO director-general says, 'so let's seize this opportunity'". CNN. 14 September 2022.
- ^ "Coronavirus Morning News Brief – Oct. 21: More Americans Are Getting the Updated Vaccine, BA.5 Continues Dominance in U.S." Frequent Business Traveller. Retrieved 21 October 2022.
- ^ "COVID-19 world weekly cases down 19% but new subvariant spreading". UPI. Retrieved 2 November 2022.
- ^ "What day is the real anniversary of the COVID-19 pandemic?". The Week. 9 March 2021. Retrieved 5 November 2022.
- ^ "WHO reports 90% drop in global COVID-19 deaths since February". MSN. Retrieved 11 November 2022.
- ^ "WHO estimates 90% of world have some resistance to Covid". The Guardian. 3 December 2022. Retrieved 3 December 2022.
- ^ "China Estimates Covid Surge Is Infecting 37 Million People a Day". Bloomberg. 23 December 2022.
- ^ "US will require COVID-19 testing for travelers from China". MSN. Retrieved 29 December 2022.
- ^ "EU calls screening of travellers from China 'unjustified'". BBC News. 29 December 2022. Archived from the original on 29 December 2022. Retrieved 29 December 2022.
- ^ "WHO worried about surge of COVID in China amid lack of info". AP NEWS. 4 January 2023. Retrieved 6 January 2023.
- ^ "WHO Europe: no immediate COVID-19 threat from China". AP NEWS. 10 January 2023. Retrieved 31 May 2023.
- ^ Tétrault-Farber G, Rigby J, Farge E (16 January 2023). "WHO recommends that China monitor excess COVID-19 mortality". Reuters. Retrieved 31 May 2023.
- ^ Lasarte D, Sofia LP (26 January 2023). "China's covid cases loom over upcoming WHO meeting on state of the pandemic". Quartz. Retrieved 31 May 2023.
- ^ "COVID-19 pandemic expected to end this year 'as a public health emergency,' says World Health Organization". MSN. Retrieved 20 March 2023.
- ^ Nolen S (5 May 2023). "W.H.O. Ends Global Health Emergency Designation for Covid". New York Times. Retrieved 5 May 2023.
- ^ a b Gregory A (5 May 2023). "Covid-19 is no longer a global health emergency, says WHO". The Guardian. Retrieved 9 May 2023.
- ^ a b "Statement on the fifteenth meeting of the International Health Regulations (2005) Emergency Committee regarding the coronavirus disease (COVID-19) pandemic". World Health Organization. 5 May 2023. Retrieved 5 May 2023.
- ^ Heyward G, Silver M (5 May 2023). "WHO ends global health emergency declaration for COVID-19". NPR. Retrieved 9 May 2023.
- ^ "WHO sees 'concerning' COVID trends before winter as hospitalisations rise". Al Jazeera. 6 September 2023. Archived from the original on 31 October 2023. Retrieved 31 October 2023.
- ^ "WHO updates its guidance on treatments for COVID-19". BMJ (Press release). 9 November 2023.
- ^ "Coronavirus: 7 dead, 229 infected in Italy as Europe braces for COVID-19". NBC News. 25 February 2020. Retrieved 29 February 2020.
- ^ Doyle M (11 October 2020). "WHO doctor says lockdowns should not be main coronavirus defence". ABC News. Retrieved 25 October 2020.
- ^ Jones S, Kassam A (26 March 2020). "Spain defends response to coronavirus as global cases exceed 500,000". The Guardian. Retrieved 29 March 2020.
- ^ "Coronavirus: Half of humanity now on lockdown as 90 countries call for confinement". Euronews. 3 April 2020.
- ^ "A third of the global population is on coronavirus lockdown – here's our constantly updated list of countries and restrictions". Business Insider. 28 March 2020.
- ^ "German anti-lockdown protests led to more coronavirus cases, study finds". Politico. 9 February 2021. Retrieved 17 February 2021.
- ^ "COVID-19 Data Explorer". Our World in Data. Archived from the original on 9 December 2021. Retrieved 9 December 2021.
- ^ "COVID-19 Data Explorer". Our World in Data. Archived from the original on 9 December 2021. Retrieved 9 December 2021.
- ^ a b Burki T (November 2020). "China's successful control of COVID-19". The Lancet. Infectious Diseases. 20 (11): 1240–1241. doi:10.1016/S1473-3099(20)30800-8. PMC 7544475. PMID 33038941.
- ^ Multiple sources:
- Hessler P. "How China Controlled the Coronavirus". The New Yorker. Retrieved 4 January 2021.
- "China's response shows how bold decision-making can contain coronavirus". World Economic Forum. 11 March 2020. Retrieved 4 January 2021.
- Kupferschmidt K, Cohen J (2 March 2020). "China's aggressive measures have slowed the coronavirus. They may not work in other countries". Science. doi:10.1126/science.abb5426. S2CID 216508232.
- ^ Pike LL (25 November 2020). "In China, nearly 1 million people have reportedly already gotten a coronavirus vaccine". Vox. Retrieved 26 November 2020.
- ^ "China vaccinates over 80% of its people against COVID-19". Reuters. 11 December 2021. Retrieved 11 December 2021.
- ^ "China's response shows how bold decision-making can contain coronavirus". World Economic Forum. 11 March 2020. Archived from the original on 4 January 2021. Retrieved 4 January 2021.
- ^ Kupferschmidt K, Cohen J (2 March 2020). "China's aggressive measures have slowed the coronavirus. They may not work in other countries". Science | AAAS. Archived from the original on 15 February 2021. Retrieved 4 January 2021.
- ^ Wang K, Song W (4 April 2022). "China: How is its zero-Covid strategy changing?". BBC.
- ^ Mcdonald J (12 November 2022). "China Returns to Lockdowns as Cases of COVID-19 Surge". NBC New York. Retrieved 13 November 2022.
- ^ "World stocks on back foot as China COVID cases rise". MSN. Retrieved 21 November 2022.
- ^ Magramo K (24 November 2022). "China's Covid cases hit record as dissent grows over tough restrictions". CNN. Retrieved 25 November 2022.
- ^ Gan N, Wang P (29 November 2022). "China's security apparatus swings into action to smother Covid protests". CNN. Retrieved 29 November 2022.
- ^ "China abandons key parts of zero-Covid strategy after protests". BBC. 7 December 2022.
- ^ Bradsher K, Chien AC, Dong J (23 December 2022). "As Cases Explode, China's Low Covid Death Toll Convinces No One". The New York Times. ISSN 0362-4331. Retrieved 23 December 2022.
- ^ "China's low covid death count is being criticized as implausible". The Washington Post. 20 December 2022. Retrieved 23 December 2022.
- ^ "Some hospitals in China overwhelmed in national COVID-19 wave". CBC. Retrieved 26 December 2022.
- ^ Gettleman J, Schultz K (24 March 2020). "Modi Orders 3-Week Total Lockdown for All 1.3 Billion Indians". The New York Times. ISSN 0362-4331. Retrieved 2 August 2020.
- ^ "Infections over 1 lakh, five cities with half the cases: India's coronavirus story so far". The Week. Retrieved 20 May 2020.
- ^ "India's Aarogya Setu becomes world's most downloaded contact-tracing app". WION. 16 July 2020. Retrieved 25 March 2022.
- ^ "India's Covid vaccination programme one of world's most successful: Govt". The Economic Times. Retrieved 25 March 2022.
- ^ "India rolls out the world's largest COVID-19 vaccination drive". www.who.int. Retrieved 25 March 2022.
- ^ Yeung J, Sud V. "India's second Covid wave hits like a 'tsunami' as hospitals buckle under weight". CNN. Retrieved 26 April 2021.
- ^ "India Has Hit The 100-crore Vaccination Mark". Moneycontrol. 21 October 2021. Retrieved 28 December 2021.
- ^ "Realizan jornada de limpieza en vagones del Metro de Panamá". Tvn-2.com. 12 March 2020. Retrieved 23 April 2020.
- ^ "Coronavirus Arrives in Iran: Two People Test Positive in Qom". IranGov.ir. Government of Iran. 19 February 2020. Retrieved 6 March 2020.
- ^ "Iran Confirms 3 New Coronavirus Cases". IranGov.ir. Government of Iran. 20 February 2020. Retrieved 6 March 2020.
- ^ "Iranian Doctors Call For 'Long Holiday' To Contain Coronavirus, As Sixth Victim Dies". Radio Farda. Radio Free Europe/Radio Liberty. 22 February 2020. Retrieved 8 March 2020.
- ^ Gambrell J. "Iran news agencies report Friday prayers canceled in Tehran". The Washington Post. Associated Press.
- ^ "Iran Announces Closure Of Universities, Schools As Coronavirus Death Toll Rises". Radio Farda. Radio Free Europe/Radio Liberty. 23 February 2020. Retrieved 8 March 2020.
- ^ Kirkpatrick DD, Fassihi F, Mashal M (24 February 2020). "'Recipe for a Massive Viral Outbreak': Iran Emerges as a Worldwide Threat". The New York Times.
- ^ a b Wright R (24 February 2020). "How Iran Became A New Epicenter of the Coronavirus Outbreak". The New Yorker.
- ^ a b Cunningham E, Bennett D (4 March 2020). "Coronavirus pummels Iran leadership as data show spread is far worse than reported". The Washington Post.
- ^ Haltiwanger J (3 March 2020). "8% of Iran's parliament has the coronavirus, and it released 54,000 prisoners as the country descends into chaos". Business Insider. Retrieved 4 March 2020.
- ^ "Coronavirus pandemic 'could kill millions' in Iran". Al Jazeera. 17 March 2020.
- ^ "Iranian Hospitals Overflow As Number Of Reported COVID-19 Cases Passes 4 Million". Radiofreeeurope/Radioliberty. 5 August 2021. Archived from the original on 5 August 2021. Retrieved 6 August 2021.
- ^ "42 Shincheonji followers came to S. Korea from virus-hit Wuhan over 8 months: gov't". Yonhap News Agency. 29 February 2020.
- ^ a b Normile D (17 March 2020). "Coronavirus cases have dropped sharply in South Korea. What's the secret to its success?". Science. doi:10.1126/science.abb7566. S2CID 216427938.
- ^ Moon G (24 March 2020). "This is how South Korea flattened its coronavirus curve". NBC News. Retrieved 31 March 2020.
- ^ Kuhn A (13 March 2020). "South Korea's Drive-Through Testing For Coronavirus Is Fast – And Free". NPR. Retrieved 16 March 2020.
- ^ "South Korea reports lowest number of new cases". BBC News Online. 23 March 2020. Retrieved 23 March 2020.
- ^ a b Kim S (4 March 2020). "How South Korea Lost Control of Its Coronavirus Outbreak". The New Yorker.
- ^ Kasulis K (19 March 2020). "South Korea's coronavirus lessons: Quick, easy tests; monitoring". Al Jazeera.
- ^ 'K방역 극찬' 빌 게이츠, KT 손잡고 제2 코로나 막을 연구에 60억 투자. 중앙일보 (in Korean). 17 May 2020. Retrieved 17 May 2020.
- ^ Government of Montenegro [@MeGovernment] (17 March 2020). "PM @DuskoMarkovicCG: #Montenegro confirmes first two #COVID19 cases #CoronaInfoCG https://t.co/Jxkrm4AMwK" (Tweet). Archived from the original on 12 May 2022. Retrieved 8 December 2022 – via Twitter.
- ^ Saglietto A, D'Ascenzo F, Zoccai GB, De Ferrari GM (April 2020). "COVID-19 in Europe: the Italian lesson". Lancet. 395 (10230): 1110–1111. doi:10.1016/S0140-6736(20)30690-5. PMC 7118630. PMID 32220279.
- ^ Nebehay S (13 March 2020). "Europe is epicenter of coronavirus pandemic: WHO". Reuters. Retrieved 8 May 2021.
- ^ "Coronavirus: Europe now epicentre of the pandemic, says WHO". BBC. 13 March 2020. Retrieved 8 May 2021.
- ^ Feuer W (22 May 2020). "South America is a 'new epicenter' of the coronavirus pandemic, WHO says".
- ^ Henley J (18 March 2020). "More than 250m in lockdown in EU as Belgium and Germany adopt measures". The Guardian. ISSN 0261-3077. Archived from the original on 1 April 2020. Retrieved 4 April 2020.
- ^ "COVID-19's epicentre again: Europe faces fresh reckoning". www.aljazeera.com. Retrieved 19 November 2021.
- ^ "With Covid cases rising, Europe is back at the epicenter of the pandemic". NBC News. 4 November 2021. Retrieved 15 January 2022.
- ^ "Italy suspends all China flights as coronavirus cases confirmed in Rome". TheLocal.it. 31 January 2020. Retrieved 26 February 2020.
- ^ "Coronavirus, in dieci comuni lombardi: 50 mila persone costrette a restare in casa. Quarantena all'ospedale milanese di Baggio". La Repubblica (in Italian). 21 February 2020. Retrieved 23 February 2020.
- ^ "Coronavirus: All sport in Italy suspended because of outbreak". BBC Sport. 9 March 2020.
- ^ "Italy coronavirus death toll overtakes China". The Independent. 19 March 2020.
- ^ "Coronavirus: sono 33.190 i positivi – Comunicato Stampa". Dipartimento della Protezione Civile. Archived from the original on 27 May 2021. Retrieved 7 April 2023.
- ^ Coleman J (19 April 2020). "Italy sees fewest coronavirus deaths in a week". The Hill. Retrieved 20 April 2020.
- ^ "Conte firma il dpcm: stop a movida e gite, niente didattica a distanza". ansa.it. 13 October 2020. Retrieved 13 October 2020.
- ^ "Italy passes 1 million Covid-19 cases, France overtakes Russia". South China Morning Post. 12 November 2020. Retrieved 13 November 2020.
- ^ "Coronavirus: Clinics in Naples, Italy, on the brink of collapse". Deutsche Welle. 23 November 2020. Retrieved 25 November 2020.
- ^ Linde P (31 January 2020). "Sanidad confirma en La Gomera el primer caso de coronavirus en España". El Pais (in Spanish). Archived from the original on 31 January 2020. Retrieved 31 January 2020.
- ^ Ansede M (22 April 2020). "El análisis genético sugiere que el coronavirus ya circulaba por España a mediados de febrero". El País (in Spanish). Retrieved 23 April 2020.
- ^ "Spain poised to tighten coronavirus lockdown after record daily toll". MSN. Retrieved 29 March 2020.
- ^ "Coronavirus: Spain drives fears of European 'second wave'". BBC. 25 July 2020.
- ^ "Spain's Basque region admits to second wave of Covid-19". El País. 6 August 2020.
- ^ Badcock J (14 August 2020). "Spain shuts down nightlife amid fears of major second wave of coronavirus". The Telegraph. Archived from the original on 10 January 2022.
- ^ "Spain won't declare another national state of alarm, allows regions to lockdown if necessary". Euroactiv. 26 August 2020.
- ^ a b Ritchie H, Mathieu E, Rodés-Guirao L, Appel C, Giattino C, Ortiz-Ospina E, et al. (5 March 2020). "Coronavirus Pandemic (COVID-19)". Our World in Data.
- ^ Leatherby L (15 May 2020). "Sweden Stayed Open. A Deadly Month Shows the Risks". The New York Times. Retrieved 18 May 2020.
- ^ Milne R (8 May 2020). "Architect of Sweden's no-lockdown strategy insists it will pay off". Financial Times. Retrieved 16 August 2020.
- ^ "Sverige diskuterar inte exitstrategier: "Vår strategi är hållbar, vi kan ligga kvar med den en väldigt lång tid"". svenska.yle.fi (in Swedish). Retrieved 16 August 2020.
- ^ "Inte längre någon överdödlighet i Sverige". Dagens Medicin (in Swedish). Retrieved 16 August 2020.
- ^ "Ignore the squabbling Devolution has become less dysfunctional during the pandemic". The Economist. 6 June 2020. Retrieved 22 July 2020.
- ^ "The U.K. is aiming for deliberate 'herd immunity'". Fortune. Retrieved 14 March 2020.
- ^ "60% of UK population need to get coronavirus so country can build 'herd immunity', chief scientist says". The Independent. 13 March 2020. Retrieved 14 March 2020.
- ^ Triggle N (16 March 2020). "What is the UK advice on coronavirus?". BBC News Online. Retrieved 17 March 2020.
- ^ Boseley S (16 March 2020). "New data, new policy: why UK's coronavirus strategy changed". The Guardian. Retrieved 17 March 2020.
- ^ Meredith S (20 March 2020). "UK PM Boris Johnson announces nationwide lockdown measures, telling cafes, pubs and restaurants to close". CNBC. Retrieved 20 March 2020.
- ^ "Coronavirus: Government to pay up to 80% of workers' wages". BBC News Online. Retrieved 20 March 2020.
- ^ "Coronavirus: Strict new curbs on life in UK announced by PM". BBC News. 24 March 2020. Retrieved 24 March 2020.
- ^ "Large-scale human trial of potential COVID-19 vaccine kicks off at Oxford". CBS News. 24 April 2020. Retrieved 24 April 2020.
- ^ "Coronavirus updates: Texas reports single highest daily rate increase of infections". MSN. Retrieved 17 May 2020.
- ^ Mueller B (2 December 2020). "U.K. Approves Pfizer Coronavirus Vaccine, a First in the West". The New York Times. Retrieved 2 December 2020.
- ^ "Coronavirus (COVID-19) Infection Survey, UK: 19 August 2022". UK Office for National Statistics. 19 August 2022. Retrieved 6 July 2023.
- ^ "Second Travel-related Case of 2019 Novel Coronavirus Detected in United States". Centers for Disease Control and Prevention. 18 February 2020.
- ^ "Update on Coronavirus (COVID-19) by Bonaire's Lt. Governor InfoBonaire". The Bonaire Information Site. 16 April 2020. Retrieved 17 April 2020.
- ^ "Mortality Analyses". Johns Hopkins University. Retrieved 17 December 2020.
- ^ "COVID-19 surpasses 1918 flu as deadliest pandemic in U.S. history". National Geographic. 21 September 2021. Retrieved 2 October 2021.
- ^ Stobbe M (21 December 2020). "US deaths in 2020 top 3 million, by far most ever counted". Associated Press. Retrieved 22 December 2020.
- ^ Bosman J, Kasakove S, Victor D (21 July 2021). "U.S. Life Expectancy Plunged in 2020, Especially for Black and Hispanic Americans". The New York Times. Archived from the original on 28 December 2021. Retrieved 21 July 2021.
- ^ Shapiro E, Pereira I, Deliso M (6 October 2021). "COVID-19 live updates: More Americans died of COVID this year than all of 2020". ABC News. Retrieved 6 October 2021.
- ^ FDA Approves First COVID-19 Vaccine. U.S. Food and Drug Administration (FDA). 23 August 2021. Retrieved 16 October 2021.
- ^ "COVID variants BQ.1/BQ.1.1 make up nearly half of U.S. cases – CDC". Reuters. 18 November 2022. Retrieved 19 November 2022.
- ^ Schnirring L (14 October 2022). "US COVID levels decline as new subvariants rise steadily". CIDRAP. Retrieved 19 November 2022.
- ^ McQuigge M (25 March 2020). "The Quarantine Act explained, as isolation becomes mandatory for some". CTV News. Retrieved 4 April 2021.
- ^ Grimes J. "COVID Cases in Atlantic Bubble Remain Low as Cases Grow Across Canada".
- ^ "Vaccine passports coming, Furey says, as N.L. reports 5 new cases". CBC News. 7 September 2021.
- ^ Austen I (3 September 2021). "Vaccine Passports Roll Out, and So Do Unruly Anti-Vaccine Protests". The New York Times. Archived from the original on 3 September 2021.
- ^ "Canada is seeing an early rise in flu cases. Is a 'tidal wave' of infection coming?". cbc. Retrieved 19 November 2022.
- ^ orwitz L, Nagovitch P, Sonneland HK, Zissis C. "Where Is the Coronavirus in Latin America?". AS/COA. Archived from the original on 22 March 2020. Retrieved 22 March 2020.
- ^ "Uncollected bodies lie for days in the streets of Ecuador the emerging epicentre of the coronavirus in Latin America". Stuff/Fairfax. 4 April 2020.
- ^ "WHO declares that South America is the new coronavirus epicenter". The Washington Post. Retrieved 23 May 2020.
- ^ Ward A (26 May 2020). "How South America became a coronavirus epicenter". Vox. Retrieved 28 May 2020.
- ^ Ankel S. "How Brazil went from carnival floats to mass graves. Photos show what it's like in the world's latest coronavirus hotspot". Business Insider. Retrieved 31 May 2023.
- ^ "Brasil confirma primeiro caso da doença". Ministry of Health (Brazil). 26 February 2020. Archived from the original on 6 March 2020. Retrieved 4 March 2020.
- ^ Oliveira E, Ortiz B (26 February 2020). "Ministério da Saúde confirma primeiro caso de coronavírus no Brasil". G1 (in Brazilian Portuguese). Retrieved 31 May 2023.
- ^ Charner F (19 June 2020). "Brazil tops 1 million Covid-19 cases. It may pass the US next, becoming the worst-hit country on the planet". CNN. Retrieved 19 June 2020.
- ^ "Painel Coronavírus". Retrieved 12 June 2020.
- ^ Kupek E (September 2021). "How many more? Under-reporting of the COVID-19 deaths in Brazil in 2020". Tropical Medicine & International Health. 26 (9): 1019–1028. doi:10.1111/tmi.13628. PMC 8242696. PMID 34008266.
- ^ Ibrahim NK (November 2020). "Epidemiologic surveillance for controlling Covid-19 pandemic: types, challenges and implications". Journal of Infection and Public Health. 13 (11): 1630–1638. doi:10.1016/j.jiph.2020.07.019. PMC 7441991. PMID 32855090.
- ^ Santos AM, Souza BF, Carvalho CA, Campos MA, Oliveira BL, Diniz EM, et al. (2021). "Excess deaths from all causes and by COVID-19 in Brazil in 2020". Revista de Saúde Pública. 55: 71. doi:10.11606/s1518-8787.2021055004137. PMC 8522736. PMID 34730751.
- ^ "Brazil "falls" to third place among covid-19 affected countries behind the U.S. and now India". MercoPress. Retrieved 5 September 2022.
- ^ "Beijing orders 14-day quarantine for all returnees". BBC News. 15 February 2020. Archived from the original on 14 February 2020. Retrieved 24 March 2020.
- ^ "Egypt announces first Coronavirus infection". EgyptToday. 14 February 2020. Archived from the original on 15 February 2020. Retrieved 24 March 2020.
- ^ "Nigeria confirms first coronavirus case". BBC News. 28 February 2020. Archived from the original on 2 March 2020. Retrieved 24 March 2020.
- ^ "Remote Lesotho becomes last country in Africa to record COVID-19 case". Reuters. 13 May 2020. Archived from the original on 14 May 2020. Retrieved 13 May 2020.
- ^ "Coronavirus live updates: Lesotho becomes last African nation to report a coronavirus case". Los Angeles Times. Archived from the original on 13 May 2020. Retrieved 13 May 2020.
- ^ Akinwotu E (26 May 2020). "Experts sound alarm over lack of Covid-19 test kits in Africa". The Guardian. Archived from the original on 29 May 2020. Retrieved 29 May 2020.
- ^ Maclean R (17 March 2020). "Africa Braces for Coronavirus, but Slowly". The New York Times. Archived from the original on 25 March 2020. Retrieved 25 March 2020.
- ^ Adebayo B, Busari S (9 March 2020). "Here are the African countries with confirmed coronavirus cases". CNN. Retrieved 2 June 2023.
- ^ Nolen S (23 March 2022). "Trying to Solve a Covid Mystery: Africa's Low Death Rates". The New York Times. Retrieved 13 June 2023.
- ^ Burke J (7 June 2021). "Third wave sweeps across Africa as Covid vaccine imports dry up". The Guardian. Retrieved 2 June 2023.
- ^ Mendez R (8 July 2021). "Africa suffers worst surge in Covid cases as delta variant spurs third wave of pandemic". CNBC. Retrieved 9 July 2021.
- ^ Dahir AL (8 July 2021). "Africa marks its 'worst pandemic week' yet, with cases surging and vaccine scarce, the W.H.O. says". The New York Times. ISSN 0362-4331. Archived from the original on 28 December 2021. Retrieved 9 July 2021.
- ^ Schlein L (20 October 2022). "Africa Lags Behind Rest of World in COVID-19 Vaccination Coverage". VOA. Retrieved 2 June 2023.
- ^ "First confirmed case of novel coronavirus in Australia". Australian Government Department of Health. 25 January 2020. Archived from the original on 15 February 2020. Retrieved 3 March 2020.
- ^ a b Lynch L (27 January 2021). "Going viral: Timeline shows how COVID-19 infected Queensland". Brisbane Times. Retrieved 2 June 2023.
- ^ "WHO COVID-19 Dashboard". 24 April 2020. Archived from the original on 16 April 2020. Retrieved 24 April 2020.
- ^ Pandey S (27 February 2021). "Australia records 10th day of no local COVID-19 cases". Reuters. Retrieved 28 June 2021.
- ^ Scott J (24 September 2020). "Australia's Island State Pays High Price for Virus Victory". www.bloomberg.com. Retrieved 28 June 2021.
- ^ Cave D (1 February 2021). "One Case, Total Lockdown: Australia's Lessons for a Pandemic World". The New York Times. Archived from the original on 31 March 2021. Retrieved 15 April 2021.
- ^ Briggs C (1 September 2021). "Another state has given up on COVID zero. It shows Delta is a formidable foe". ABC News. Retrieved 29 October 2021.
- ^ Corlett E (4 October 2021). "New Zealand Covid elimination strategy to be phased out, Ardern says". The Guardian. Archived from the original on 4 October 2021. Retrieved 4 October 2021.
- ^ Dayman I (27 November 2021). "SA opened its borders to COVID-19 this week. Here's what we've learned". ABC News. Retrieved 2 June 2023.
- ^ Lewin R (12 December 2021). "Everything you need to know as Queensland's border FINALLY reopens to Australia". 7NEWS. Retrieved 2 June 2023.
- ^ Humphries A (14 December 2021). "5,000 arrivals in a day: Hobart Airport predicted to have busiest day on record". ABC News. Retrieved 2 June 2023.
- ^ Truu M (29 January 2022). "Hitting the Omicron peak is just the beginning: This is what's in store next for Australia". ABC News. Retrieved 2 June 2023.
- ^ Mercer P (3 March 2022). "Western Australia Finally Opens Border After COVID-19 Closure". VOA. Retrieved 2 June 2023.
- ^ McNeill H (26 April 2022). "WATCH LIVE: WA to ditch masks, proof of vaccination and capacity limits". WAtoday. Retrieved 26 April 2022.
- ^ Young E (2 September 2022). "WA public health rules to change as COVID-19 case numbers drop". The Age. Retrieved 12 October 2022.
- ^ "COVID-19 update 9 September 2022". ww2.health.wa.gov.au. Retrieved 12 October 2022.
- ^ "Australia to move away from reporting daily COVID-19 case numbers". ABC News. 7 September 2022. Retrieved 2 June 2023.
- ^ Brown A (14 September 2022). "Paid pandemic leave extended while mandatory isolation continues". InDaily. Retrieved 2 June 2023.
- ^ Taylor H (21 September 2022). "Victoria becomes final state to scrap COVID mask rule". 7NEWS. Retrieved 2 June 2023.
- ^ Jose R, Jackson L (30 September 2022). "As Australia calls end to COVID emergency response, doctors warn of risk to public". Reuters.
- ^ Taylor A, Pitrelli S (24 March 2020). "One continent remains untouched by the coronavirus: Antarctica". The Washington Post. Archived from the original on 1 April 2020. Retrieved 3 April 2020.
- ^ Torres E (20 March 2020). "What life is like on Antarctica, the only continent without a case of coronavirus". ABC News. Archived from the original on 1 April 2020. Retrieved 3 April 2020.
- ^ "Pacific islands, Antarctic bases: coronavirus-free living in some of Earth's most isolated places". South China Morning Post. Agence France-Presse. 31 March 2020. Archived from the original on 3 April 2020. Retrieved 3 April 2020.
- ^ Ramos Miranda NA (22 December 2020). "Coronavirus reaches end of earth as first outbreak hits Antarctica". Reuters. Retrieved 2 June 2023.
- ^ McClure T (8 November 2022). "Antarctica's biggest Covid outbreak yet puts US station McMurdo on pause". The Guardian. Retrieved 12 June 2023.
- ^ "Global Ceasefire Call Deserves UN Security Council's Full Support". Crisis Group. 9 April 2020. Retrieved 1 August 2020.
- ^ "UN tallies action so far to fight COVID-19, and roadmap out of the pandemic". UN News. 25 June 2020. Retrieved 4 August 2020.
- ^ Charbonneau B (March 2021). "The COVID-19 test of the United Nations Security Council". International Journal: Canada's Journal of Global Policy Analysis. 76 (1): 6–16. doi:10.1177/0020702020986897. ISSN 0020-7020. S2CID 233202171. Retrieved 5 June 2023.
- ^ Gladstone R (2 April 2020). "U.N. Security Council 'Missing In Action' in Coronavirus Fight". The New York Times. Retrieved 5 June 2023.
- ^ "Transcript of the Secretary-General's virtual press encounter on the appeal for global ceasefire". United Nations Secretary-General. 23 March 2020. Retrieved 1 August 2020.
- ^ "COVID-19: UN chief calls for global ceasefire to focus on 'the true fight of our lives'". UN News. 23 March 2020. Retrieved 1 August 2020.
- ^ "170 signatories endorse UN ceasefire appeal during COVID crisis". UN News. 24 June 2020. Retrieved 1 August 2020.
- ^ "S/RES/2532(2020) – E – S/RES/2532(2020)". undocs.org. Retrieved 1 August 2020.
- ^ "Stalled Security Council resolution adopted, backing UN's global humanitarian ceasefire call". UN News. 1 July 2020. Retrieved 1 August 2020.
- ^ "U.N. chief urges increase in funding for IMF to help pandemic-hit countries". Reuters. 29 September 2020. Retrieved 5 June 2023.
- ^ "COVAX". www.who.int. Retrieved 9 December 2021.
- ^ "Factbox: Vaccines delivered under COVAX sharing scheme for poorer countries". Reuters. 25 November 2022. Retrieved 5 June 2023.
- ^ IMF. "The IMF's Response to COVID-19".
- ^ a b Kakaei H, Nourmoradi H, Bakhtiyari S, Jalilian M, Mirzaei A (2022). "Effect of COVID-19 on food security, hunger, and food crisis". COVID-19 and the Sustainable Development Goals: 3–29. doi:10.1016/B978-0-323-91307-2.00005-5. ISBN 9780323913072. PMC 9335023.
- ^ Barnes JE (8 April 2021). "U.S. Intelligence Report Warns of Global Consequences of Social Fragmentation". The New York Times. Archived from the original on 28 December 2021. Retrieved 8 May 2021.
- ^ "Coronavirus Travel Restrictions, Across the Globe". The New York Times. 26 March 2020.
- ^ Menon P (24 November 2021). "New Zealand sets date for reopening to tourists after nearly two years". Reuters. Retrieved 5 June 2023.
- ^ "Travel to Australia during Covid-19: What you need to know before you go". CNN. 11 March 2021. Retrieved 5 June 2023.
- ^ Nsikan A (24 February 2020). "Coronavirus spikes outside China show travel bans aren't working". National Geographic. Retrieved 2 April 2020.
- ^ Chinazzi M, Davis JT, Ajelli M, Gioannini C, Litvinova M, Merler S, et al. (April 2020). "The effect of travel restrictions on the spread of the 2019 novel coronavirus (COVID-19) outbreak". Science. 368 (6489): 395–400. Bibcode:2020Sci...368..395C. doi:10.1126/science.aba9757. PMC 7164386. PMID 32144116.
- ^ Kim KE (April 2023). "Ten Takeaways from the COVID-19 Pandemic for Transportation Planners". Transportation Research Record. 2677 (4): 517–530. doi:10.1177/03611981221090515. ISSN 0361-1981. PMC 10149348. PMID 37153166.
- ^ "COVID-19: Study shows that travel restrictions are most useful in the early and late phase of an epidemic". Oxford Martin School, University of Oxford. 25 March 2020.
- ^ "Coronavirus: EU rules out Schengen border closures amid Italy outbreak". Deutsche Welle. 24 February 2020.
- ^ "Commission chief warns against unilateral virus travel bans". EURACTIV. 13 March 2020.
- ^ "Countries Evaluate Evacuation of Citizens Amid Wuhan Coronavirus Panic". Associated Press. Retrieved 31 January 2020 – via The Diplomat.
- "Coronavirus: Second plane carrying 323 Indians from Wuhan to reach Delhi today". India Today. February 2020. Retrieved 2 February 2020.
- "België haalt landgenoten terug uit Chinese provincie Hubei na uitbraak coronavirus". VRT Nws. Vlaamse Radio- en Televisieomroeporganisatie. 27 January 2020.
- Nathalia T (30 January 2020). "Last-Minute Preparations Underway to Evacuate Indonesian Citizens From Coronavirus-Ravaged Wuhan". Jakarta Globe.
- "C130 aircraft on standby for Wuhan evacuation". Bangkok Post. 26 January 2020. Retrieved 26 January 2020.
- Jiang S, Stracqualursi V (25 January 2020). "US arranging charter flight to evacuate American diplomats and citizens out of China amid coronavirus outbreak, official says". CNN. Archived from the original on 26 January 2020. Retrieved 27 January 2020.
- "PH sending special flights to get Pinoys from Wuhan, Hubei in China". Tempo: News in a Flash. Manila, Philippines. 29 January 2020. Retrieved 29 January 2020.
- ^ "Aviões decolam de Wuhan, na China, com 40 passageiros repatriados ao Brasil e à Polônia". G1 (in Portuguese). 7 February 2020. Retrieved 9 February 2020.
- ^ "Air New Zealand flight with kiwi evacuees departs Wuhan". Stuff (company). 5 February 2020.
- ^ "Repatriated citizens to be reunited with families". SANews.gov.zanews24.com. 29 March 2020. Retrieved 31 March 2020.
- ^ "Pakistan cancels flights to China as fears of coronavirus spread". Dialogue Pakistan. 31 January 2020. Retrieved 5 April 2020.
- ^ Wang V, Rich M, Bradsher K (15 February 2020). "Shifting Ground in Coronavirus Fight: U.S. Will Evacuate Americans From Cruise Ship". The New York Times. Retrieved 15 February 2020.
- ^ "Cruise ship passengers begin 14-day quarantine in Cornwall, Ont". CBC News. 21 February 2020.
- ^ Roche E (9 March 2020). "Coronavirus: India sending IAF aircraft to evacuate its nationals from Iran". LiveMint.com. Retrieved 9 March 2020.
- ^ "4th batch of 53 Indians evacuated from Iran: S Jaishankar". The Economic Times. 16 March 2020. Retrieved 28 March 2020.
- ^ Kheel R (20 March 2020). "US-led coalition in Iraq drawing down over coronavirus concerns". The Hill. Retrieved 7 April 2020.
- ^ Oh S (28 February 2020). "Stocks record worst week since financial crisis as coronavirus concerns heat up". Market Watch. Retrieved 28 February 2020.
- ^ "Collapsed Flybe: 'Do not travel to the airport'". BBC News. 5 March 2020.
- ^ Turner B (4 April 2020). "'Most significant crisis in the history of travel': where to now for tourism?". The Sydney Morning Herald. Retrieved 5 April 2020.
- ^ "Coronavirus scare: Complete list of airlines suspending flights". India Today. Reuters. 27 February 2020. Retrieved 7 March 2020.
- ^ Cherney M, Craymer L (5 May 2020). "You've Got Mail ... Finally: The Pandemic Is Jamming Up the World's Post". The Wall Street Journal. Retrieved 15 May 2020.
- ^ Tyko K (17 March 2023). "How COVID permanently changed shopping and restaurants". Retrieved 5 June 2023.
- ^ "How Retailers Globally are Responding to Coronavirus by Aislelabs", Aislelabs, 2 April 2020, retrieved 3 April 2020
- ^ Aislelabs (23 March 2020), "How Shopping Centres Globally are Responding to Coronavirus by Aislelabs", Aislelabs, retrieved 23 March 2020
- ^ "Half the world's workers face losing their jobs, says ILO". Al Jazeera. 29 April 2020.
- ^ Temko N. "No jobs, so what future? Half the world's workforce on the edge". Christian Science Monitor. Retrieved 5 June 2023.
- ^ Romm T (28 May 2020). "Americans have filed more than 40 million jobless claims in past 10 weeks, as another 2.1 million filed for benefits last week". The Washington Post.
- ^ Sundaram A (16 September 2020). "Yelp data shows 60% of business closures due to the coronavirus pandemic are now permanent". CNBC. Retrieved 5 June 2023.
- ^ Nebehay S (23 September 2020). "Pandemic slashes worldwide income from work by a tenth: ILO". Reuters. Retrieved 23 September 2020.
- ^ Yuen KF, Wang X, Ma F, Li KX (May 2020). "The Psychological Causes of Panic Buying Following a Health Crisis". International Journal of Environmental Research and Public Health. 17 (10): 3513. doi:10.3390/ijerph17103513. PMC 7277661. PMID 32443427. S2CID 218856048.
- ^ Tyko K (29 February 2020). "Coronavirus fears empty store shelves of toilet paper, bottled water, masks as shoppers stock up". USA Today.
- ^ Strumpf D (31 January 2020). "Tech Sector Fears Supply Delays as Effects of Virus Ripple Through China". The Wall Street Journal. Retrieved 26 February 2020.
- ^ Nebehay S (7 February 2020). "Procura por máscaras aumenta 100 vezes e prejudica luta contra o coronavírus" (in Brazilian Portuguese). Reuters Brasil. Retrieved 20 May 2021.
- ^ Boseley S (7 February 2020). "WHO warns of global shortage of face masks and protective suits". The Guardian. Retrieved 12 February 2020.
- ^ "Shortage of personal protective equipment endangering health workers worldwide". World Health Organization (WHO). Retrieved 5 March 2020.
- ^ Lewis AC (19 April 2022). "The hustlers and scammers behind the pandemic supply chain nightmare". The Verge. Retrieved 5 June 2023.
- ^ Bauchner H, Fontanarosa PB, Livingston EH (19 May 2020). "Conserving Supply of Personal Protective Equipment—A Call for Ideas". JAMA. 323 (19): 1911. doi:10.1001/jama.2020.4770. PMID 32196543. S2CID 214600902. Retrieved 5 June 2023.
- ^ Ventura L (2 May 2023). "Global Finance Magazine – Poorest Countries in the World 2023". Global Finance Magazine. Retrieved 5 June 2023.
- ^ a b Anyanwu JC, Salami AO (April 2021). "The impact of COVID-19 on African economies: An introduction". African Development Review. 33 (S1): S1–S16. doi:10.1111/1467-8268.12531. PMC 8207010. PMID 34149237.
- ^ "Food Security and COVID-19". World Bank. Retrieved 23 December 2021.
- ^ US oil prices turn negative as demand dries up, BBC, 21 April 2020.
- ^ "Energy crunch: How high will oil prices climb?". Al-Jazeera. 27 September 2021.
- ^ Smith A (8 October 2021). "Cascade of problems fuels world energy crisis as another winter looms". NBC News. Retrieved 5 June 2023.
- ^ McGivern H, Kenny N (14 March 2020). "Here are the museums that have closed (so far) due to coronavirus". theartnewspaper.com. Archived from the original on 29 March 2020. Retrieved 29 March 2020.
- ^ Ottone E (2021). "Foreword". UNESCO The Universal Declaration on Cultural Diversity: Marking the 20th Anniversary. London: Khalili Foundation. pp. 13–15. ISBN 978-1-3999-1149-8.
- ^ "UNESCO: 10 million creative jobs lost in Covid crisis". The Stage. Retrieved 5 June 2023.
- ^ "The Ultimate Guide to Virtual Museum Resources". MCN. 15 March 2020. Retrieved 29 March 2020.
- ^ Burke D (14 March 2020). "What churches, mosques and temples are doing to fight the spread of coronavirus". CNN. Retrieved 16 March 2020.
- ^ Hadden J (2 March 2020). "Over 20,000 people have signed a petition to cancel SXSW over coronavirus worries. Here's a list of all the major event cancellations due to the outbreak so far". Business Insider. Retrieved 3 March 2020.
- ^ Fadroski KS (15 March 2020). "Coronavirus canceled their concerts, so artists like Yungblud are looking to live stream shows to fans". Daily Breeze.
- ^ Brenner WA (15 March 2020). "The Social Distancing Festival Is Live Online". The Austin Chronicle.
- ^ Tumilty R (13 March 2020). "Federal government announces aggressive measures to battle COVID-19 as parliament suspended until April". Nationalpost. Retrieved 30 April 2020.
- ^ Mackinnon A, Palder D (18 March 2020). "Coronavirus in the Corridors of Power". Foreign Policy. Retrieved 30 April 2020.
- ^ Corasaniti N, Saul S (27 April 2020). "15 States Have Postponed Primaries During the Pandemic. One Has Canceled". The New York Times. ISSN 0362-4331. Retrieved 30 April 2020.
- ^ The Economist, 4 April 2020, p. 14.
- ^ a b c d Sott MK, Bender MS, da Silva Baum K (4 September 2022). "Covid-19 Outbreak in Brazil: Health, Social, Political, and Economic Implications". International Journal of Health Services. 52 (4). SAGE Publications: 442–454. doi:10.1177/00207314221122658. ISSN 0020-7314. PMC 9445630. PMID 36062608.
- ^ Conde M (11 May 2020). "Brazil in the Time of Coronavirus". Geopolítica(s). Revista de estudios sobre espacio y poder. 11 (Especial). Universidad Complutense de Madrid (UCM): 239–249. doi:10.5209/geop.69349. ISSN 2172-7155. S2CID 219439973.
- ^ Londoño E (15 May 2020). "Another Health Minister in Brazil Exits Amid Chaotic Coronavirus Response". The New York Times. Retrieved 14 June 2023.
- ^ Dantas E (2020). "Brazilian report on the coronavirus crisis: A clash of pandemics". Medicine and Law (in Portuguese): 153–160. Retrieved 14 June 2023.
- ^ Carnut L, Mendes Á, Guerra L (18 October 2020). "Coronavirus, Capitalism in Crisis and the Perversity of Public Health in Bolsonaro's Brazil". International Journal of Health Services. 51 (1). SAGE Publications: 18–30. doi:10.1177/0020731420965137. ISSN 0020-7314. PMID 33070682. S2CID 224782017.
- ^ "Brazil stocks post steepest fall since 1998, real hits historic low 5.00 per dollar". Reuters. 12 March 2020.
- ^ Alcantara LC, Nogueira E, Shuab G, Tosta S, Fristch H, Pimentel V, et al. (2022). "SARS-CoV-2 epidemic in Brazil: how the displacement of variants has driven distinct epidemic waves". Virus Research. 315. Elsevier BV: 198785. doi:10.1016/j.virusres.2022.198785. ISSN 0168-1702. PMC 9022374. PMID 35461905.
- ^ "Covid: Brazil's daily deaths surpass 3,000 for first time". BBC News. 24 March 2021. Retrieved 14 June 2023.
- ^ Reeves P (15 April 2021). "Brazil COVID-19: 'Humanitarian Crisis' With More Than 3,000 Deaths A Day". NPR. Retrieved 14 June 2023.
- ^ Chomsky N, Polychroniou CJ (9 May 2023). Illegitimate Authority. Haymarket Books. ISBN 978-1-64259-934-3.
- ^ "Jair Bolsonaro is poised to lose the Brazilian election". The Economist. 8 September 2022. Retrieved 14 June 2023.
- ^ Milhorance F (30 October 2022). "Bolsonaro, in defeat, may now face charges". The New York Times. Retrieved 14 June 2023.
- ^ Bostock B (13 February 2020). "China sacked a brace of top officials in Hubei province, likely in a move to protect Xi Jinping from people's anger over the coronavirus outbreak". Business Insider. Retrieved 26 February 2020.
- ^ Barnes J (2 April 2020). "C.I.A. Hunts for Authentic Virus Totals in China, Dismissing Government Tallies". The New York Times.
- ^ "China Denies Cover-Up, Rejects 'Politicization' of Coronavirus". Bloomberg.com. 7 June 2020. Retrieved 7 June 2020.
- ^ "China says there has never been a cover-up on coronavirus outbreak". Reuters. 17 April 2020. Retrieved 6 June 2023.
- ^ "Chen Qiushi: Chinese journalist missing since February 'under state supervision'". BBC News. 24 September 2020. Retrieved 16 February 2021.
- ^ "Li Zehua: Journalist who 'disappeared' after Wuhan chase reappears". BBC News. 23 April 2020. Retrieved 16 February 2021.
- ^ "Zhang Zhan: China jails citizen journalist for Wuhan reports". BBC News. 28 December 2020. Retrieved 16 February 2021.
- ^ Davidson H (10 December 2020). "Citizen journalist detained over Wuhan reporting 'restrained and fed by tube'". The Guardian. Retrieved 16 February 2021.
- ^ Boffey D (11 March 2020). "Italy criticises EU for being slow to help over coronavirus epidemic". The Guardian. Retrieved 6 June 2023.
- ^ Braw E (14 March 2020). "The EU Is Abandoning Italy in Its Hour of Need". Foreign Policy. Retrieved 6 June 2023.
- ^ Karnitschnig M (18 March 2020). "China is winning the coronavirus propaganda war". Politico.
- ^ "Russian army to send coronavirus help to Italy after Putin phone call". Reuters. 22 March 2020.
- ^ Vivaldelli R (28 March 2020). "Quelle polemiche infondate sugli aiuti russi all'Italia". Il Giornale.
- ^ "Coronavirus: EU Medical Teams deployed to Italy". Europa (web portal). 1 July 2020.
- ^ "EU offers 'heartfelt apology' to Italy over coronavirus response". The Guardian. 1 July 2020.
- ^ Rouan R (20 April 2020). "Protesters at Statehouse demand state reopen as DeWine announces schools to remain closed". The Columbus Dispatch. Archived from the original on 25 April 2020. Retrieved 3 May 2020.
- ^ "Coronavirus: Anti-Lockdown Protests Grow Across US". BBC News. 17 April 2020. Archived from the original on 17 April 2020. Retrieved 17 April 2020.
- ^ Russ H (30 March 2020). "Instacart, Amazon workers strike as labor unrest grows during coronavirus crisis". Reuters. Retrieved 24 July 2020.
- ^ Haberman M, Martin M, Jonathan (12 March 2020). "Trump's Re-election Chances Suddenly Look Shakier". The New York Times. ISSN 0362-4331. Retrieved 15 March 2020.
- ^ Lowrey A (3 April 2020). "The Economy Is Collapsing. So Are Trump's Reelection Chances". The Atlantic. Retrieved 3 May 2020.
- ^ Miller CC (10 April 2020). "Could the Pandemic Wind Up Fixing What's Broken About Work in America?". The New York Times. Retrieved 3 May 2020.
- ^ Swanson I (2 May 2020). "Five ways the coronavirus could change American politics". The Hill. Retrieved 3 May 2020.
- ^ Cohen M. "America's botched response to the coronavirus is a problem bigger than Donald Trump". The Boston Globe.
- ^ Amin K, Cox C (22 December 2021). "Unvaccinated COVID-19 hospitalizations cost billions of dollars". Peterson-KFF Health System Tracker. Retrieved 3 May 2022.
- ^ Hughes T. "As Biden vaccine mandates loom, protests for personal freedoms swell. What happens next?". USA TODAY. Retrieved 6 June 2023.
- ^ Kimball S (25 January 2022). "Biden administration withdraws Covid vaccine mandate for businesses after losing Supreme Court case". CNBC. Retrieved 6 June 2023.
- ^ "National Federation of Independent Business v. Department of Labor, Occupational Safety and Health Administration". SCOTUSblog. Retrieved 6 June 2023.
- ^ "Record number of journalists imprisoned in 2020 – report". Reuters. 15 December 2020. Retrieved 16 February 2021.
- ^ Berry A (14 December 2020). "Press freedom: Journalists end up in jail for reporting on coronavirus crisis". Deutsche Welle. Retrieved 16 February 2021.
- ^ Simes D (20 March 2020). "How coronavirus derailed the largest Nato exercise in 25 years". The Spectator.
- ^ Emmott R (19 March 2020). "NATO scales down exercises due to coronavirus". Reuters. Retrieved 21 October 2020.
- ^ Berman I (12 March 2020). "Will Iran's Regime Survive Coronavirus?". National Review. Retrieved 7 June 2023.
- ^ "U.S. sanctions 'severely hamper' Iran coronavirus fight, Rouhani says". Reuters. 14 March 2020.
- ^ Haverty D, Gramer R, Detsch J (9 April 2020). "Coronavirus Pandemic Forces a Cease-Fire in Yemen". Foreign Policy. Retrieved 21 October 2020.
- ^ Sposato W (12 March 2020). "Japan and Korea Won't Let A Pandemic Stop Them Fighting". Foreign Policy. Retrieved 7 June 2023.
- ^ Farrer J, McCurry M (6 March 2020). "Coronavirus quarantine plans ignite row between South Korea and Japan". The Guardian. Retrieved 21 October 2020.
- ^ Walker S (31 March 2020). "Authoritarian leaders may use Covid-19 crisis to tighten their grip". The Guardian.
- ^ Gebrekidam S (30 March 2020). "For Autocrats, and Others, Coronavirus Is a Chance to Grab Even More Power". The New York Times.
- ^ Picheta R (30 March 2020). "Hungarian parliament votes to let Viktor Orban rule by decree in wake of coronavirus pandemic". CNN.
- ^ Michaelson R (3 April 2020). "Reporting on the coronavirus: Egypt muzzles critical journalists". Deutsche Welle.
- ^ Mchangama J (1 April 2020). "Coronavirus Has Started a Censorship Pandemic". The Foreign Policy.
- ^ Peck G (16 April 2020). "Some leaders use pandemic to sharpen tools against critics". The Seattle Times. Retrieved 7 June 2023.
- ^ "Asia cracks down on coronavirus 'fake news'". The Straits Times. 10 April 2020.
- ^ Bagri N (4 October 2020). "As COVID-19 spreads, India tries to control the narrative by targeting journalists". Los Angeles Times. Retrieved 16 February 2021.
- ^ a b "Q&A: COVID-19 pandemic – impact on food and agriculture". Food and Agriculture Organization of the United Nations. Retrieved 16 October 2020.
- ^ Pryor S, Dietz W (1 September 2022). "The COVID-19, Obesity, and Food Insecurity Syndemic". Current Obesity Reports. 11 (3): 70–79. doi:10.1007/s13679-021-00462-w. ISSN 2162-4968. PMC 9399358. PMID 35138590.
- ^ a b FAO, IFAD, UNICEF, WFP, WHO (2020). The State of Food Security and Nutrition in the World 2020. doi:10.4060/CA9692EN. ISBN 978-92-5-132901-6. S2CID 239729231. Retrieved 16 October 2020.
- ^ Swinnen J, Vos R (May 2021). "COVID-19 and impacts on global food systems and household welfare: Introduction to a special issue". Agricultural Economics. 52 (3): 365–374. doi:10.1111/agec.12623. ISSN 0169-5150. PMC 8206861. PMID 34149127.
- ^ "UN report: Pandemic year marked by spike in world hunger". www.who.int. Retrieved 14 December 2021.
- ^ Hoffman JA, Miller EA (August 2020). "Addressing the Consequences of School Closure Due to COVID-19 on Children's Physical and Mental Well-Being". World Medical & Health Policy. 12 (3): 300–310. doi:10.1002/wmh3.365. PMC 7461306. PMID 32904951.
- ^ "COVID afecta salud, educación y entorno familiar de niñas y niños, señala estudio del IBD". Senado de la República (in Spanish). 1 May 2021. Archived from the original on 6 December 2021. Retrieved 25 July 2021.
- ^ "Covid: Many students say their mental health is worse due to pandemic". BBC News. 31 March 2021. Retrieved 6 April 2021.
- ^ Yu S, Wan R, Bai L, Zhao B, Jiang Q, Jiang J, et al. (29 March 2023). "Transformation of chronic disease management: Before and after the COVID-19 outbreak". Frontiers in Public Health. 11. doi:10.3389/fpubh.2023.1074364. PMC 10090362. PMID 37064686.
- ^ Garcia S, Albaghdadi MS, Meraj PM, Schmidt C, Garberich R, Jaffer FA, et al. (June 2020). "Reduction in ST-Segment Elevation Cardiac Catheterization Laboratory Activations in the United States During COVID-19 Pandemic". Journal of the American College of Cardiology. 75 (22): 2871–2872. doi:10.1016/j.jacc.2020.04.011. PMC 7151384. PMID 32283124.
- ^ a b 'Where are all our patients?': Covid phobia is keeping people with serious heart symptoms away from ERs, Stat News, Usha Lee McFarling, 23 April 2020.
- ^ Dula AN, Gealogo Brown G, Aggarwal A, Clark KL (21 October 2020). "Decrease in Stroke Diagnoses During the COVID-19 Pandemic: Where Did All Our Stroke Patients Go?". JMIR Aging. 3 (2): e21608. doi:10.2196/21608. PMC 7581311. PMID 33006936.
- ^ Orthopoulos G, Santone E, Izzo F, Tirabassi M, Pérez-Caraballo AM, Corriveau N, et al. (1 May 2021). "Increasing incidence of complicated appendicitis during COVID-19 pandemic". The American Journal of Surgery. 221 (5): 1056–1060. doi:10.1016/j.amjsurg.2020.09.026. ISSN 0002-9610. PMC 7521886. PMID 33012500.
- ^ Faust JS (28 April 2020). "Medication Shortages Are the Next Crisis". The Atlantic. Retrieved 17 May 2020.
- ^ "Coronavirus Disease 2019 (COVID-19)". Centers for Disease Control and Prevention. 11 February 2020. Retrieved 17 May 2020.
- ^ Stix G. "Pandemic Year 1 Saw a Dramatic Global Rise in Anxiety and Depression". Scientific American. Retrieved 10 October 2021.
- ^ Luo Y, Chua CR, Xiong Z, Ho RC, Ho CS (23 November 2020). "A Systematic Review of the Impact of Viral Respiratory Epidemics on Mental Health: An Implication on the Coronavirus Disease 2019 Pandemic". Frontiers in Psychiatry. 11: 565098. doi:10.3389/fpsyt.2020.565098. PMC 7719673. PMID 33329106.
- ^ Santomauro DF, Herrera AM, Shadid J, Zheng P, Ashbaugh C, Pigott DM, et al. (8 October 2021). "Global prevalence and burden of depressive and anxiety disorders in 204 countries and territories in 2020 due to the COVID-19 pandemic". The Lancet. 398 (10312): 1700–1712. doi:10.1016/S0140-6736(21)02143-7. PMC 8500697. PMID 34634250. S2CID 238478261.
- ^ Principi N, Autore G, Ramundo G, Esposito S (13 May 2023). "Epidemiology of Respiratory Infections during the COVID-19 Pandemic". Viruses. 15 (5): 1160. doi:10.3390/v15051160. ISSN 1999-4915. PMC 10224029. PMID 37243246.
- ^ Wu K (31 October 2022). "The Worst Pediatric-Care Crisis in Decades". The Atlantic. Archived from the original on 31 October 2022. Retrieved 1 November 2022.
- ^ Mandavilli A (23 October 2022). "A 'Tripledemic'? Flu, R.S.V. and Covid May Collide This Winter, Experts Say". The New York Times. Archived from the original on 28 October 2022. Retrieved 5 November 2022.
- ^ Turner CE (February 2023). "Can group A streptococcus infections be influenced by viruses in the respiratory tract?". The Lancet Infectious Diseases. 23 (2): 142–144. doi:10.1016/S1473-3099(22)00865-9. PMID 36566769. S2CID 255018859. Retrieved 9 June 2023.
- ^ Mackintosh T, Durbin A (3 December 2022). "Father of girl, 4, fighting for life with Strep A infection is 'praying for a miracle'". BBC News. Archived from the original on 3 December 2022. Retrieved 4 December 2022.
- ^ Davis N (15 December 2022). "Strep A kills three more children as UK activates alternative medicines plan: At least 19 children have died and scarlet fever cases are more than treble what they were in previous high season". The Guardian. Archived from the original on 17 December 2022. Retrieved 17 December 2022.
- ^ Wetsman N, McLean N (16 December 2022). "US children's hospitals are tracking increases in severe strep infections". ABC News. Archived from the original on 17 December 2022. Retrieved 17 December 2022.
- ^ Alhoufie ST, Alsharif NH, Alfarouk KO, Ibrahim NA, Kheyami AM, Aljifri AA (November 2021). "COVID-19 with underdiagnosed influenza B and parainfluenza-2 co-infections in Saudi Arabia: Two case reports". Journal of Infection and Public Health. 14 (11): 1567–1570. doi:10.1016/j.jiph.2021.09.005. PMC 8442300. PMID 34627054.
- ^ Koutsakos M, Wheatley AK, Laurie K, Kent SJ, Rockman S (December 2021). "Influenza lineage extinction during the COVID-19 pandemic?". Nature Reviews Microbiology. 19 (12): 741–742. doi:10.1038/s41579-021-00642-4. PMC 8477979. PMID 34584246.
- ^ a b World Health Organization (29 September 2023). "Questions and Answers: Recommended composition of influenza virus vaccines for use in the southern hemisphere 2024 influenza season and development of candidate vaccine viruses for pandemic preparedness" (PDF). Retrieved 26 October 2023.
- ^ a b Schnirring L (29 September 2023). "WHO advisers recommend switch back to trivalent flu vaccines". CIDRAP. Retrieved 26 October 2023.
- ^ "Earth Observatory". 28 February 2020. Archived from the original on 2 April 2020. Retrieved 9 April 2020.
- ^ a b Rume T, Islam SM (September 2020). "Environmental effects of COVID-19 pandemic and potential strategies of sustainability". Heliyon. 6 (9): e04965. Bibcode:2020Heliy...604965R. doi:10.1016/j.heliyon.2020.e04965. PMC 7498239. PMID 32964165.
- ^ Hotle S, Mumbower S (1 March 2021). "The impact of COVID-19 on domestic U.S. air travel operations and commercial airport service". Transportation Research Interdisciplinary Perspectives. 9: 100277. Bibcode:2021TrRIP...900277H. doi:10.1016/j.trip.2020.100277. ISSN 2590-1982. S2CID 230597573. Retrieved 9 June 2023.
- ^ "The air got cleaner in 2020, thanks to the pandemic". CBS News. 19 November 2020.
- ^ Main D (18 March 2024). "How Wild Animals Actually Responded to Our COVID Lockdowns". Scientific American. Archived from the original on 19 March 2024. Retrieved 20 March 2024.
- ^ Pappas G, Vokou D, Sainis I, Halley JM (31 October 2022). "SARS-CoV-2 as a Zooanthroponotic Infection: Spillbacks, Secondary Spillovers, and Their Importance". Microorganisms. 10 (11): 2166. doi:10.3390/microorganisms10112166. ISSN 2076-2607. PMC 9696655. PMID 36363758.
- ^ Devaux CA, Pinault L, Delerce J, Raoult D, Levasseur A, Frutos R (20 September 2021). "Spread of Mink SARS-CoV-2 Variants in Humans: A Model of Sarbecovirus Interspecies Evolution". Frontiers in Microbiology. 12: 675528. doi:10.3389/fmicb.2021.675528. PMC 8488371. PMID 34616371.
- ^ Eckstrand CD, Baldwin TJ, Rood KA, Clayton MJ, Lott JK, Wolking RM, et al. (12 November 2021). "An outbreak of SARS-CoV-2 with high mortality in mink (Neovison vison) on multiple Utah farms". PLOS Pathogens. 17 (11): e1009952. doi:10.1371/journal.ppat.1009952. PMC 8589170. PMID 34767598.
- ^ Jacobs A (2 November 2021). "Widespread Coronavirus Infection Found in Iowa Deer, New Study Says". The New York Times. Archived from the original on 2 November 2021. Retrieved 5 November 2021.
- ^ Mallapaty S (26 April 2022). "COVID is spreading in deer. What does that mean for the pandemic?". Nature. Archived from the original on 26 April 2022. Retrieved 26 April 2022.
- ^ McBride DS, Garushyants SK, Franks J, Magee AF, Overend SH, Huey D, et al. (28 August 2023). "Accelerated evolution of SARS-CoV-2 in free-ranging white-tailed deer". Nature Communications. 14 (1): 5105. Bibcode:2023NatCo..14.5105M. doi:10.1038/s41467-023-40706-y. PMC 10462754. PMID 37640694.
- ^ McCormick E (7 February 2022). "'Homelessness is lethal': US deaths among those without housing are surging". The Guardian. Retrieved 20 August 2022.
- ^ Burton N (7 February 2020). "The coronavirus exposes the history of racism and "cleanliness"". Vox. Archived from the original on 7 February 2020. Retrieved 9 February 2020.
- ^ "Fears of new virus trigger anti-China sentiment worldwide". The Korea Times. 2 February 2020.
- ^ Wangkiat P (10 February 2020). "Virus-induced racism does no one any good". Bangkok Post.
- ^ Bartholomew R (6 February 2020). "The Coronavirus and the Search for Scapegoats". Psychology Today.
- ^ Smith N (1 February 2020). "Anti-Chinese racism spikes as virus spreads globally". The Daily Telegraph. Archived from the original on 10 January 2022.
'Some Muslims were claiming the disease was "divine retribution" for China's oppression of the Uighur minority. The problem lay in confusing the Chinese population with the actions of an authoritarian government known for its lack of transparency,' he said.
- ^ Tavernise S, Oppel Jr RA (23 March 2020). "Spit On, Yelled At, Attacked: Chinese-Americans Fear for Their Safety". The New York Times. Retrieved 23 March 2020.
- ^ "London Racially Motivated Assault due to Coronavirus". ITV News. 4 March 2020. Retrieved 4 March 2020.
- ^ La Gorce T (5 April 2020). "Chinese-Americans, Facing Abuse, Unite to Aid Hospitals in Coronavirus Battle". The New York Times. Retrieved 29 April 2020.
- ^ Rogers K, Jakes L, Swanson A (18 March 2020). "Trump Defends Using 'Chinese Virus' Label, Ignoring Growing Criticism". The New York Times. Archived from the original on 20 March 2020. Retrieved 20 March 2020.
- ^ Haltiwanger J (20 March 2020). "Republicans are using racism against China to try to distract from Trump's disastrous coronavirus response". Business Insider.
- ^ Lee BY. "Trump Once Again Calls Covid-19 Coronavirus The 'Kung Flu'". Forbes. Retrieved 9 July 2020.
- ^ Silva MF, Silva DS, Bacurau AG, Francisco PM, Assumpção D, Neri AL, et al. (2021). "Ageism against older adults in the context of the COVID-19 pandemic: an integrative review". Revista de Saúde Pública. 55: 4. doi:10.11606/s1518-8787.2021055003082. PMC 8023321. PMID 33886953.
- ^ Kampf G (20 November 2021). "COVID-19: stigmatising the unvaccinated is not justified". The Lancet. 398 (10314): 1871. doi:10.1016/S0140-6736(21)02243-1. PMC 8601682. PMID 34801101.
- ^ Caplan AL (February 2022). "Stigma, vaccination, and moral accountability". The Lancet. 399 (10325): 626–627. doi:10.1016/S0140-6736(22)00189-1. PMC 8830899. PMID 35151392.
- ^ "Don't discriminate against the unvaccinated, Amnesty International tells Italy". Reuters. 16 January 2022.
- ^ "Data dive: How COVID-19 impacted ecommerce in 2020". Digital Commerce 360. Retrieved 27 March 2021.
- ^ Kats R. "More Consumers Are Turning to Food Delivery Apps amid Indoor Dining Restrictions". eMarketer.com. Retrieved 28 March 2021.
- ^ Scotto M. "NYC Indoor Dining To Shut Down Monday, Cuomo Announces". Spectrum News NY1. Retrieved 28 March 2021.
- ^ DeLisi B. "The future of hacking: COVID-19 shifting the way hackers work and who they target". SECURITY magazine. Retrieved 28 March 2021.
- ^ "The COVID-19 pandemic has changed education forever. This is how". World Economic Forum. 29 April 2020. Retrieved 28 March 2021.
- ^ Benshoff L. "Pandemic Threatens Long-Term Job Security After Hospitality Industry Layoffs". NPR. Retrieved 28 March 2021.
- ^ Woodyard C. "Travel industry layoffs begin as Congress fails to come up with new relief package". USA Today. Retrieved 28 March 2021.
- ^ Chong J (30 June 2022). "Workers feel corporate COVID-19, equity policies 'not genuine,' study says". The Toronto Star. ISSN 0319-0781. Retrieved 30 June 2022.
- ^ "After Two Years of Remote Work, Workers Question Office Life". The New York Times. 10 March 2022. Retrieved 13 June 2023.
- ^ Mitchell T (16 February 2022). "COVID-19 Pandemic Continues To Reshape Work in America". Pew Research Center's Social & Demographic Trends Project. Retrieved 13 June 2023.
- ^ Kagubare I (20 February 2023). "Nearly 30 percent of work remains remote as workers dig in". The Hill. Retrieved 13 June 2023.
- ^ "As Covid fades away, what's the future of remote work in Europe?". ComputerWeekly.com. 14 March 2023. Retrieved 14 June 2023.
- ^ a b Braesemann F, Stephany F, Teutloff O, Kässi O, Graham M, Lehdonvirta V (20 October 2022). "The global polarisation of remote work". PLOS ONE. 17 (10). Public Library of Science (PLoS): e0274630. arXiv:2108.13356. Bibcode:2022PLoSO..1774630B. doi:10.1371/journal.pone.0274630. ISSN 1932-6203. PMC 9584402. PMID 36264859.
- ^ "What does remote working look like around the world?". The European Sting. 13 February 2023. Retrieved 14 June 2023.
- ^ "Will remote work stick after the pandemic?". The Economist. 15 January 2022. Retrieved 14 June 2023.
- ^ Peck E (13 June 2023). "Companies get aggressive on return-to-office". Axios. Retrieved 13 June 2023.
- ^ Fonzo E (18 July 2021). "Historiography and Covid-19. Some considerations". Journal of Mediterranean Knowledge. 6 (1): 129–158. ISSN 2499-930X.
- ^ Tambolkar S, Pustake M, Giri P, Tambolkar I (May 2022). "Comparison of public health measures taken during Spanish flu and COVID-19 pandemics: A Narrative Review". Journal of Family Medicine and Primary Care. 11 (5): 1642–1647. doi:10.4103/jfmpc.jfmpc_1612_21. PMC 9254789. PMID 35800503.
- ^ Beach B, Clay K, Saavedra M (March 2022). "The 1918 Influenza Pandemic and Its Lessons for COVID-19". Journal of Economic Literature. 60 (1): 41–84. doi:10.1257/jel.20201641. ISSN 0022-0515.
- ^ Ewing T (12 May 2020). "Flu Masks Failed In 1918, But We Need Them Now". Health Affairs Forefront. doi:10.1377/forefront.20200508.769108. Retrieved 9 June 2023.
- ^ "Mask Resistance During a Pandemic Isn't New – in 1918 Many Americans Were 'Slackers'". www.michiganmedicine.org. 29 October 2020. Retrieved 9 June 2023.
- ^ Devega C (8 May 2021). "Fake news, conspiracy theories and a deadly global pandemic — and that was in 1918". Salon. Retrieved 9 June 2023.
- ^ Cohut M (29 September 2020). "What the COVID-19 pandemic and the 1918 flu pandemic have in common". www.medicalnewstoday.com. Retrieved 9 June 2023.
- ^ Krishnan L, Ogunwole SM, Cooper LA (15 September 2020). "Historical Insights on Coronavirus Disease 2019 (COVID-19), the 1918 Influenza Pandemic, and Racial Disparities: Illuminating a Path Forward". Annals of Internal Medicine. 173 (6): 474–481. doi:10.7326/M20-2223. ISSN 0003-4819. PMC 7298913. PMID 32501754.
- ^ Lee M, Lim H, Xavier MS, Lee EY (1 February 2022). ""A Divine Infection": A Systematic Review on the Roles of Religious Communities During the Early Stage of COVID-19". Journal of Religion and Health. 61 (1): 866–919. doi:10.1007/s10943-021-01364-w. ISSN 1573-6571. PMC 8370454. PMID 34405313.
- ^ Kalocsányiová E, Essex R, Fortune V (19 July 2022). "Inequalities in Covid-19 Messaging: A Systematic Scoping Review". Health Communication. 38 (12): 2549–2558. doi:10.1080/10410236.2022.2088022. ISSN 1041-0236. PMID 35850593. S2CID 250642415. Retrieved 9 June 2023.
- ^ Lee Rogers R, Powe N (January 2022). "COVID-19 Information Sources and Misinformation by Faith Community". INQUIRY: The Journal of Health Care Organization, Provision, and Financing. 59: 004695802210813. doi:10.1177/00469580221081388. ISSN 0046-9580. PMC 9152626. PMID 35634989.
- ^ Majumdar S (29 November 2022). "Key findings about COVID-19 restrictions that affected religious groups around the world in 2020". Pew Research Center. Retrieved 9 June 2023.
- ^ Li H, Cao Y (1 April 2022). "Rules We Live by: How Religious Beliefs Relate to Compliance with Precautionary Measures Against COVID-19 in Tibetan Buddhists". Journal of Religion and Health. 61 (2): 1671–1683. doi:10.1007/s10943-022-01512-w. ISSN 1573-6571. PMC 8817637. PMID 35122555.
- ^ Syed U, Kapera O, Chandrasekhar A, Baylor BT, Hassan A, Magalhães M, et al. (February 2023). "The Role of Faith-Based Organizations in Improving Vaccination Confidence & Addressing Vaccination Disparities to Help Improve Vaccine Uptake: A Systematic Review". Vaccines. 11 (2): 449. doi:10.3390/vaccines11020449. ISSN 2076-393X. PMC 9966262. PMID 36851325.
- ^ Sisti LG, Buonsenso D, Moscato U, Costanzo G, Malorni W (January 2023). "The Role of Religions in the COVID-19 Pandemic: A Narrative Review". International Journal of Environmental Research and Public Health. 20 (3): 1691. doi:10.3390/ijerph20031691. ISSN 1660-4601. PMC 9914292. PMID 36767057.
- ^ Jerde S. "Major Publishers Take Down Paywalls for Coronavirus Coverage". www.adweek.com. Retrieved 9 June 2023.
- ^ "Call to Make COVID-19 Data/Research Publicly Available" (PDF). NIH. imagwiki.nibib.nih.gov. Retrieved 9 June 2023.
- ^ "PMC COVID-19 Collection". PubMed Central (PMC). Retrieved 9 June 2023.
- ^ "Coronavirus (COVID-19): sharing research data". Wellcome. 31 January 2020. Retrieved 9 June 2023.
- ^ Capocasa M, Anagnostou P, Bisol GD (15 June 2022). "A light in the dark: open access to medical literature and the COVID-19 pandemic". Information Research: An International Electronic Journal. 27 (2). doi:10.47989/irpaper929. S2CID 249615157. Retrieved 9 June 2023.
- ^ Rogers A. "Coronavirus Research Is Moving at Top Speed—With a Catch". Wired. Retrieved 9 June 2023.
- ^ Murphy H, Di Stefano M, Manson K (20 March 2020). "Huge text message campaigns spread coronavirus fake news". Financial Times.
- ^ Kassam N (25 March 2020). "Disinformation and coronavirus". The Interpreter. Lowy Institute.
- ^ Kuhn SA, Lieb R, Freeman D, Andreou C, Zander-Schellenberg T (March 2021). "Coronavirus conspiracy beliefs in the German-speaking general population: endorsement rates and links to reasoning biases and paranoia". Psychological Medicine. 52 (16): 4162–4176. doi:10.1017/S0033291721001124. PMC 8027560. PMID 33722315.
- ^ "How The Covid-19 Pandemic Is Affecting Popular Culture". augustman.com. August Man. 24 November 2020. Retrieved 18 December 2020.
In addition to existing shows, streaming platforms and cable channels have tried putting together new series centred on coronavirus, like HBO's "Coastal Elites" or Netflix's "Social Distance" – but with no real success.
- ^ Segal D (16 December 2020). "Are We Ready to Laugh About Covid-19? A British Sitcom Hopes So". The New York Times. Retrieved 18 December 2020.
Are we ready to laugh about Covid-19? Or rather, is there anything amusing, or recognizable in a humorous way, about life during a plague, with all of its indignities and setbacks, not to mention its rituals (clapping for health care workers) and rules (face masks, please).
- ^ Nobel E (13 April 2020). "COVID-19 will shape pop culture for years to come, but for now we love pandemic stories". abc.net.au. Australian Broadcasting Corporation. Retrieved 18 December 2020.
Fictitious stories about pandemics give us a way to experience the horror in a controlled way, with the pacing we've grown to expect, where resolution is always possible, and where we can always turn off the TV if it gets a bit too much.
- ^ McCluskey M (7 October 2020). "Horror Films Have Always Tapped Into Pop Culture's Most Urgent Fears. COVID-19 Will Be Their Next Inspiration". Time. Retrieved 19 December 2020.
- ^ Rogers K (2 April 2020). "'Contagion' vs. coronavirus: The film's connections to a real life pandemic". CNN. Retrieved 9 June 2023.
- ^ Kritz F. "Fact-Checking 'Contagion' — In Wake Of Coronavirus, The 2011 Movie Is Trending". Retrieved 9 June 2023.
- ^ "I've seen 'Contagion' four times. No, the coronavirus outbreak isn't the same". Los Angeles Times. 11 March 2020. Retrieved 9 June 2023.
- ^ McGuire K (March 2021). "COVID-19, Contagion, and Vaccine Optimism". Journal of Medical Humanities. 42 (1): 51–62. doi:10.1007/s10912-021-09677-3. PMC 7882858. PMID 33587203.
- ^ Freyne P. "The things my movie Contagion got wrong: The slow vaccine, the damaging president". The Irish Times. Retrieved 9 June 2023.
- ^ Jason J (23 April 2020). "How the Coronavirus Pandemic Affects Music Genres on Spotify". How Music Charts. Retrieved 10 April 2021.
- ^ Chow A. "The Pandemic Could Have Hurt Country Music. Instead, the Genre Is Booming". Time. Retrieved 10 April 2021.
- ^ "WHO declares end to Covid global health emergency". NBC News. 5 May 2023. Retrieved 6 May 2023.
- ^ Brown F (12 May 2023). "The WHO has not declared the Covid-19 pandemic over". FullFact.org.
- ^ Nebehay S (24 February 2020). "WHO says it no longer uses 'pandemic' category, but virus still emergency". Reuters. Retrieved 5 August 2023.
"There is no official category (for a pandemic)," WHO spokesman Tarik Jasarevic said.
- ^ "With the international public health emergency ending, WHO/Europe launches its transition plan for COVID-19". World Health Organization. 12 June 2023.
- ^ Biancolella M, Colona VL, Mehrian-Shai R, Watt JL, Luzzatto L, Novelli G, et al. (2022). "COVID-19 2022 update: Transition of the pandemic to the endemic phase". Human Genomics. 16 (1): 19. doi:10.1186/s40246-022-00392-1. PMC 9156835. PMID 35650595. S2CID 249274308.
- ^ Koelle K, Martin MA, Antia R, Lopman B, Dean NE (11 March 2022). "The changing epidemiology of SARS-CoV-2". Science. 375 (6585): 1116–1121. Bibcode:2022Sci...375.1116K. doi:10.1126/science.abm4915. ISSN 1095-9203. PMC 9009722. PMID 35271324.
- ^ Cohen LE, Spiro DJ, Viboud C (30 June 2022). "Projecting the SARS-CoV-2 transition from pandemicity to endemicity: Epidemiological and immunological considerations". PLOS Pathogens. 18 (6): e1010591. doi:10.1371/journal.ppat.1010591. ISSN 1553-7374. PMC 9246171. PMID 35771775.
- ^ Harrison CM, Doster JM, Landwehr EH, Kumar NP, White EJ, Beachboard DC, et al. (10 February 2023). "Evaluating the Virology and Evolution of Seasonal Human Coronaviruses Associated with the Common Cold in the COVID-19 Era". Microorganisms. 11 (2): 445. doi:10.3390/microorganisms11020445. ISSN 2076-2607. PMC 9961755. PMID 36838410.
After evaluating the biology, pathogenesis, and emergence of the human coronaviruses that cause the common cold, we can anticipate that with increased vaccine immunity to SARS-CoV-2, it will become a seasonal, endemic coronavirus that causes less severe disease in most individuals. Much like the common cold CoVs, the potential for severe disease will likely be present in those who lack a protective immune response or are immunocompromised.
- ^ Markov PV, Ghafari M, Beer M, Lythgoe K, Simmonds P, Stilianakis NI, et al. (June 2023). "The evolution of SARS-CoV-2". Nat Rev Microbiol (Review). 21 (6): 361–379. doi:10.1038/s41579-023-00878-2. PMID 37020110. S2CID 257983412.
- ^ "Post-pandemic world economy still feeling COVID-19's sting | UN News". news.un.org. 16 May 2023. Retrieved 30 July 2023.
- ^ "Not Everything Is Getting Back to Normal In the Post-Pandemic Economy". Bloomberg.com. 23 June 2023. Retrieved 30 July 2023.
- ^ Churchill B, Bissell D, Ruppanner L (19 March 2023). "The 'great resignation' didn't happen in Australia, but the 'great burnout' did". The Conversation. Retrieved 30 July 2023.
- ^ Granja AD, Champagne E, Choinière O (27 April 2023). "Post-pandemic work in the public sector: A new way forward or a return to the past?". The Conversation. Retrieved 30 July 2023.
- ^ "IATA says airline industry is rapidly returning to profitability". euronews. 5 June 2023. Retrieved 30 July 2023.
- ^ Sutherland B (28 July 2023). "Post-pandemic travel boom is running out of steam". The Japan Times. Retrieved 30 July 2023.
- ^ Sugiura E, Wright R (7 July 2023). "Can the post-pandemic travel boom endure?". Financial Times. Retrieved 30 July 2023.
- ^ "'Excess' Deaths Surging, but Why?". Medscape. Retrieved 30 July 2023.
- ^ "Global immunisation rates show sign of post-pandemic rebound | UN News". news.un.org. 17 July 2023. Retrieved 30 July 2023.
- ^ "COVID pandemic created immunisation gaps in Africa. Over half a million children are at risk | Gavi, the Vaccine Alliance". www.gavi.org. Retrieved 30 July 2023.
- ^ Joseph A (12 January 2023). "Routine vaccinations drop among U.S. kindergartners for the third year in a row". STAT. Retrieved 30 July 2023.
- ^ "Teenagers at risk after drop in vaccine take-up". BBC News. 24 April 2023. Retrieved 30 July 2023.
Further reading
- "Progress report on the coronavirus pandemic". Nature. 584 (7821): 325. August 2020. doi:10.1038/d41586-020-02414-1. PMID 32814893.
- Tay MZ, Poh CM, Rénia L, MacAry PA, Ng LF (June 2020). "The trinity of COVID-19: immunity, inflammation and intervention". Nature Reviews. Immunology. 20 (6): 363–374. doi:10.1038/s41577-020-0311-8. PMC 7187672. PMID 32346093.
- COVID-19 infection prevention and control measures for primary care, including general practitioner practices, dental clinics and pharmacy settings: first update. European Centre for Disease Prevention and Control (ECDC) (Report). October 2020.
- Bar-On YM, Flamholz A, Phillips R, Milo R (April 2020). "SARS-CoV-2 (COVID-19) by the numbers". eLife. 9. arXiv:2003.12886. Bibcode:2020arXiv200312886B. doi:10.7554/eLife.57309. PMC 7224694. PMID 32228860.
- Brüssow H (May 2020). "The Novel Coronavirus - A Snapshot of Current Knowledge". Microbial Biotechnology. 13 (3): 607–612. doi:10.1111/1751-7915.13557. PMC 7111068. PMID 32144890.
- Cascella M, Rajnik M, Aleem A, Dulebohn S, Di Napoli R (2020). "Features, Evaluation, and Treatment of Coronavirus". StatPearls. StatPearls Publishing. PMID 32150360.
- Funk CD, Laferrière C, Ardakani A (2020). "A Snapshot of the Global Race for Vaccines Targeting SARS-CoV-2 and the COVID-19 Pandemic". Frontiers in Pharmacology. 11: 937. doi:10.3389/fphar.2020.00937. PMC 7317023. PMID 32636754.
- "Development and Licensure of Vaccines to Prevent COVID-19" (PDF). U.S. Food and Drug Administration (FDA). June 2020.
- Birhane M, Bressler S, Chang G, Clark T, Dorough L, Fischer M, et al. (May 2021). "COVID-19 Vaccine Breakthrough Infections Reported to CDC – United States, January 1 – April 30, 2021". MMWR. Morbidity and Mortality Weekly Report. 70 (21): 792–793. doi:10.15585/mmwr.mm7021e3. PMC 8158893. PMID 34043615.
- Bieksiene K, Zaveckiene J, Malakauskas K, Vaguliene N, Zemaitis M, Miliauskas S (March 2021). "Post COVID-19 Organizing Pneumonia: The Right Time to Interfere". Medicina. 57 (3): 283. doi:10.3390/medicina57030283. PMC 8003092. PMID 33803690.
- Chen Q, Allot A, Lu Z (January 2021). "LitCovid: an open database of COVID-19 literature". Nucleic Acids Research. 49 (D1): D1534–D1540. doi:10.1093/nar/gkaa952. PMC 7778958. PMID 33166392.
- Aghagoli G, Gallo Marin B, Katchur NJ, Chaves-Sell F, Asaad WF, Murphy SA (June 2021). "Neurological Involvement in COVID-19 and Potential Mechanisms: A Review". Neurocritical Care. 34 (3): 1062–1071. doi:10.1007/s12028-020-01049-4. PMC 7358290. PMID 32661794.
External links
Health agencies
- COVID-19 (Questions & Answers, instructional videos; Facts/MythBusters) by the World Health Organization (WHO)
- COVID-19 by the Government of Canada
- COVID-19 (Q&A) by the European Centre for Disease Prevention and Control
- COVID-19 (Q&A) by the Ministry of Health, Singapore
- COVID-19 (Q&A) by the US Centers for Disease Control and Prevention (CDC)
- COVID-19 Information for the Workplace by the US National Institute for Occupational Safety and Health (NIOSH)
Data and graphs
- Coronavirus disease (COVID-19) situation reports and map by the World Health Organization (WHO)
- COVID-19 Resource Center, map, and historical data by Johns Hopkins University
- COVID-19 data sets published by the European Centre for Disease Prevention and Control (ECDC)
- COVID-19 Observer based on Johns Hopkins University data
- COVID-19 Statistics and Research published by Our World in Data
- COVID-19 Tracker from Stat News
- COVID-19 Projections for many countries published by Institute for Health Metrics and Evaluation
Medical journals
- Coronavirus (COVID-19) by The New England Journal of Medicine
- Coronavirus (COVID-19) Hub by BMJ Publishing Group
- Coronavirus Disease 2019 (COVID-19) by JAMA: The Journal of the American Medical Association
- COVID-19: Novel Coronavirus Outbreak Archived 24 September 2020 at the Wayback Machine by Wiley Publishing
- COVID-19 pandemic (2019–20) Collection by Public Library of Science (PLOS)
- COVID-19 Portfolio, a curated collection of publications and preprints by National Institutes of Health (NIH)
- COVID-19 Research Highlights by Springer Nature
- COVID-19 Resource Centre by The Lancet
- Novel Coronavirus Information Center by Elsevier
| Local |
| ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Global |
| ||||||||||||||||||||
History of infectious diseases | |
|---|---|
| Individual diseases | |
| People | |
| Major epidemics |
|
| Other | |
2020s articles | |
|---|---|
| History | |
| Events | |
| Govt | |
| Years | |
| Categories |
|
Overviews of the 2020s | |
|---|---|
| Political |
|
| Culture | |
| Societal | |
| Science | |
| Related | |
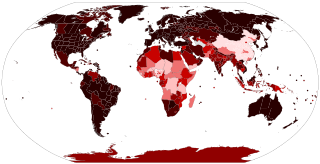

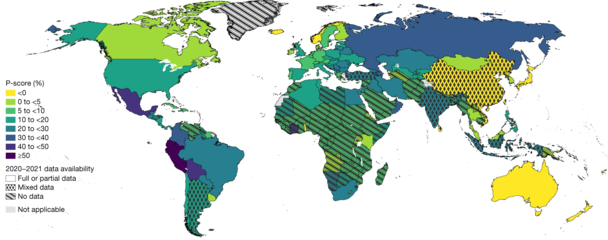
![Excess deaths relative to expected deaths (global and WHO region)[64]](https://upload.wikimedia.org/wikipedia/commons/thumb/2/2f/COVID-19_pandemic_excess_deaths_-_global_and_WHO_region_P-scores_%28excess_deaths_relative_to_expected_deaths%29.webp/309px-COVID-19_pandemic_excess_deaths_-_global_and_WHO_region_P-scores_%28excess_deaths_relative_to_expected_deaths%29.webp.png)
![The 25 countries with the highest total estimated COVID-19 pandemic excess deaths between January 2020 and December 2021[64]](https://upload.wikimedia.org/wikipedia/commons/thumb/e/e6/The_25_countries_with_the_highest_total_estimated_COVID-19_pandemic_excess_deaths_between_January_2020_and_December_2021.webp/335px-The_25_countries_with_the_highest_total_estimated_COVID-19_pandemic_excess_deaths_between_January_2020_and_December_2021.webp.png)
![The 25 countries with the highest mean P-scores (excess deaths relative to expected deaths)[64]](https://upload.wikimedia.org/wikipedia/commons/thumb/a/a2/The_25_countries_with_the_highest_mean_P-scores_%28excess_deaths_relative_to_expected_deaths%29.webp/328px-The_25_countries_with_the_highest_mean_P-scores_%28excess_deaths_relative_to_expected_deaths%29.webp.png)