| Insomnia | |
|---|---|
| Other names | Sleeplessness, trouble sleeping |
 | |
| Depiction of insomnia from the 14th century medical manuscript Tacuinum Sanitatis | |
| Pronunciation | |
| Specialty | Psychiatry, sleep medicine |
| Symptoms | Trouble sleeping, daytime sleepiness, low energy, irritability, depressed mood[1] |
| Complications | Motor vehicle collisions[1] |
| Causes | Unknown, psychological stress, chronic pain, heart failure, hyperthyroidism, heartburn, restless leg syndrome, others[2] |
| Diagnostic method | Based on symptoms, sleep study[3] |
| Differential diagnosis | Delayed sleep phase disorder, restless leg syndrome, sleep apnea, psychiatric disorder[4] |
| Treatment | Sleep hygiene, cognitive behavioral therapy, sleeping pills[5][6][7] |
| Frequency | ~20%[8][9][10] |
Insomnia, also known as sleeplessness, is a sleep disorder where people have trouble sleeping.[1] They may have difficulty falling asleep, or staying asleep for as long as desired.[1][9][11] Insomnia is typically followed by daytime sleepiness, low energy, irritability, and a depressed mood.[1] It may result in an increased risk of accidents of all kinds as well as problems focusing and learning.[9] Insomnia can be short term, lasting for days or weeks, or long term, lasting more than a month.[1] The concept of the word insomnia has two possibilities: insomnia disorder (ID) and insomnia symptoms, and many abstracts of randomized controlled trials and systematic reviews often underreport on which of these two possibilities the word insomnia refers to.[12]
Insomnia can occur independently or as a result of another problem.[2] Conditions that can result in insomnia include ADHD, psychological stress, chronic pain, heart failure, hyperthyroidism, heartburn, restless leg syndrome, menopause, certain medications, and drugs such as caffeine, nicotine, and alcohol.[2][8] Other risk factors include working night shifts and sleep apnea.[9] Diagnosis is based on sleep habits and an examination to look for underlying causes.[3] A sleep study may be done to look for underlying sleep disorders.[3] Screening may be done with two questions: "do you experience difficulty sleeping?" and "do you have difficulty falling or staying asleep?"[9]
Although their efficacy as first line treatments is not unequivocally established,[13] sleep hygiene and lifestyle changes are typically the first treatment for insomnia.[5][7] Sleep hygiene includes a consistent bedtime, a quiet and dark room, exposure to sunlight during the day and regular exercise.[7] Cognitive behavioral therapy may be added to this.[6][14] While sleeping pills may help, they are sometimes associated with injuries, dementia, and addiction.[5][6] These medications are not recommended for more than four or five weeks.[6] The effectiveness and safety of alternative medicine is unclear.[5][6]
Between 10% and 30% of adults have insomnia at any given point in time and up to half of people have insomnia in a given year.[8][9][10] About 6% of people have insomnia that is not due to another problem and lasts for more than a month.[9] People over the age of 65 are affected more often than younger people.[7] Women are more often affected than men.[8] Descriptions of insomnia occur at least as far back as ancient Greece.[15]
Signs and symptoms
[edit]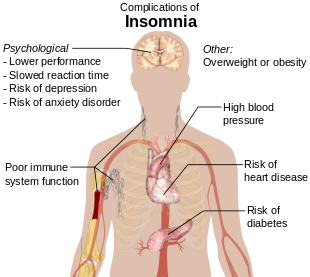
Symptoms of insomnia:[17]
- Difficulty falling asleep, including difficulty finding a comfortable sleeping position
- Waking during the night, being unable to return to sleep and waking up early
- Not able to focus on daily tasks, difficulty in remembering
- Daytime sleepiness, irritability, depression or anxiety
- Feeling tired or having low energy during the day[18]
- Trouble concentrating
- Being irritable, acting aggressive or impulsive
Sleep onset insomnia is difficulty falling asleep at the beginning of the night, often a symptom of anxiety disorders. Delayed sleep phase disorder can be misdiagnosed as insomnia, as sleep onset is delayed to much later than normal while awakening spills over into daylight hours.[19]
It is common for patients who have difficulty falling asleep to also have nocturnal awakenings with difficulty returning to sleep. Two-thirds of these patients wake up in the middle of the night, with more than half having trouble falling back to sleep after a middle-of-the-night awakening.[20]
Early morning awakening is an awakening occurring earlier (more than 30 minutes) than desired with an inability to go back to sleep, and before total sleep time reaches 6.5 hours. Early morning awakening is often a characteristic of depression.[21] Anxiety symptoms may well lead to insomnia. Some of these symptoms include tension, compulsive worrying about the future, feeling overstimulated, and overanalyzing past events.[22]
Poor sleep quality
[edit]Poor sleep quality can occur as a result of, for example, restless legs, sleep apnea or major depression. Poor sleep quality is defined as the individual not reaching stage 3 or delta sleep which has restorative properties.[23]
Major depression leads to alterations in the function of the hypothalamic–pituitary–adrenal axis, causing excessive release of cortisol which can lead to poor sleep quality.
Nocturnal polyuria, excessive night-time urination, can also result in a poor quality of sleep.[24]
Subjectivity
[edit]Some cases of insomnia are not really insomnia in the traditional sense, because people experiencing sleep state misperception often sleep for a normal amount of time.[25] The problem is that, despite sleeping for multiple hours each night and typically not experiencing significant daytime sleepiness or other symptoms of sleep loss, they do not feel like they have slept very much, if at all.[25] Because their perception of their sleep is incomplete, they incorrectly believe it takes them an abnormally long time to fall asleep, and they underestimate how long they stay asleep.[25]
Problematic digital media use
[edit]In August 2018, Sleep Science and Practice published a systematic review and meta-analysis of 19 studies comprising 253,904 adolescent subjects that found that excessive technology use had a strong and consistent association with reduced sleep duration and prolonged sleep onset latency for adolescents 14 years of age or older.[26] Also in August 2018, Sleep Science published a systematic review of 12 studies investigating associations between exposure to video games, sleep outcomes, and post-sleep cognitive abilities that found the data present in the studies indicated associations between a reduction in sleep duration, increased sleep onset latency, modifications to rapid eye movement sleep and slow-wave sleep, increased sleepiness and self-perceived fatigue, and impaired post-sleep attention span and verbal memory.[27] In October 2019, Sleep Medicine Reviews published a systematic review and meta-analysis of 23 studies comprising 35,684 subjects that found a statistically significant odds ratio for sleep problems and reduced sleep duration for subjects with internet addiction.[28] In February 2020, Psychiatry Research published a systematic review and meta-analysis of 14 studies that found positive associations between problematic smartphone use and poor sleep quality and between higher levels of problematic smartphone use and elevated risk of poor sleep quality.[29]
Also in February 2020, Sleep Medicine Reviews published a systematic review of 31 studies examining associations between screen time and sleep outcomes in children younger than 5 years and found that screen time is associated with poorer sleep outcomes for children under the age of 5, with meta-analysis only confirming poor sleep outcomes among children under 2 years.[30] In March 2020, Developmental Review published a systematic review of 9 studies that found a weak-to-moderate association between sleep quantity and quality and problematic smartphone use among adolescents.[31] In October 2020, the International Journal of Environmental Research and Public Health published a systematic review and meta-analysis of 80 studies that found that greater screen time was associated with shorter sleep duration among toddlers and preschoolers,[32] while the Journal of Behavioral Addictions published a systematic review and meta-analysis of 40 studies with 33,650 post-secondary student subjects that found a weak-to-moderate positive association between mobile phone addiction and poor sleep quality.[33] In April 2021, Sleep Medicine Reviews published a systematic review of 36 cross-sectional studies and 6 longitudinal studies that found that 24 of the cross-sectional studies and 5 of the longitudinal studies established significant associations between more frequent social media use and poor sleep outcomes.[34]
In June 2021, Frontiers in Psychiatry published a systematic review and meta-analysis of 34 studies comprising 51,901 subjects that established significant associations between problematic gaming and sleep duration, poor sleep quality, daytime sleepiness, and other sleep problems.[35] In September 2021, BMC Public Health published a systematic review of 49 studies investigating associations between electronic media use and various sleep outcomes among children and adolescents 15 years of age or younger that found a strong association with sleep duration and stronger evidence for an association with sleep duration between the ages of 6 and 15 years than for 5 years of age or younger, while evidence for associations between electronic media use with other sleep outcomes was more inconclusive.[36] In December 2021, Frontiers in Neuroscience published a systematic review of 12 studies published from January 2000 to April 2020 that found that adult subjects with higher gaming addiction scores were more likely to have shorter sleep quantity, poorer sleep quality, delayed sleep timing, and greater daytime sleepiness and insomnia scores than subjects with lower gaming addiction scores and non-gamer subjects.[37] In January 2022, Early Childhood Research Quarterly published a systematic review and meta-analysis of 26 studies that found a weak but statistically significant association with increased smartphone and tablet computer use and poorer sleep in early childhood.[38]
In May 2022, the Journal of Affective Disorders published a meta-analysis of 29 studies comprising 20,041 subjects that found a weak-to-moderate association between mobile phone addiction and sleep disorder and that adolescents with mobile phone addiction were at higher risk of developing sleep disorder.[39] In August 2022, the International Journal of Environmental Research and Public Health published a systematic review and meta-analysis of 16 studies comprising 8,077 subjects that established a significant association between binge-watching and sleep problems and a stronger association between binge-watching and sleep problems was found during the COVID-19 pandemic than pre-pandemic.[40] In October 2022, Reports in Public Health published a systematic review of 23 studies that found that excessive use of digital screens by adolescents was associated with poor sleep quality, nighttime awakenings, long sleep latency, and daytime sleepiness.[41] In December 2022, Sleep Epidemiology published a systematic review of 18 studies investigating associations between sleep problems and screen time during COVID-19 lockdowns that found that the increased screen time during the lockdowns negatively impacted sleep duration, sleep quality, sleep onset latency, and wake time.[42] In March 2023, the Journal of Clinical Sleep Medicine published a systematic review and meta-analysis of 17 studies comprising 36,485 subjects that found that smartphone overuse was closely associated with self-reported poor sleep quality, sleep deprivation, and prolonged sleep latency.[43]
In April 2023, Sleep Medicine Reviews published a systematic review of 42 studies that found digital media use to be associated with shorter sleep duration and poorer sleep quality and bedtime or nighttime use with poor sleep outcomes, but only found associations for general screen use, mobile phone use, computer and internet use, internet, and social media and not for television, game console, and tablet use.[44] In July 2023, Healthcare published a systematic review and meta-analysis of 16 studies that established a correlation coefficient of 0.56 between nomophobia and insomnia.[45] In September 2023, PLOS One published a systematic review and meta-analysis of 16 studies of smartphone addiction and sleep among medical students found that 57% of subjects had poor sleep and 39% of subjects had smartphone addiction with a correlation index of 0.3,[46] while Computers in Human Behavior published a meta-analysis of 23 longitudinal studies comprising 116,431 adolescent subjects that found that adolescent screen time with computers, smartphones, social media, and television are positively associated with negative impacts on sleep health later in life.[47]Causes
[edit]While insomnia can be caused by a number of conditions, it can also occur without any identifiable cause. This is known as Primary Insomnia.[48] Primary Insomnia may also have an initial identifiable cause, but continues after the cause is no longer present. For example, a bout of insomnia may be triggered by a stressful work or life event. However the condition may continue after the stressful event has been resolved. In such cases, the insomnia is usually perpetuated by the anxiety or fear caused by the sleeplessness itself, rather than any external factors.[49]
Symptoms of insomnia can be caused by or be associated with:
- Sleep breathing disorders, such as sleep apnea or upper airway resistance syndrome[50]
- Use of psychoactive drugs (such as stimulants), including certain medications, herbs, caffeine, nicotine, cocaine, amphetamines, methylphenidate, aripiprazole, MDMA, modafinil, or excessive alcohol intake[51]
- Use of or withdrawal from alcohol and other sedatives, such as anti-anxiety and sleep drugs like benzodiazepines[51]
- Use of or withdrawal from pain-relievers such as opioids[51]
- Heart disease[52]
- Restless legs syndrome, which can cause sleep onset insomnia due to the discomforting sensations felt and the need to move the legs or other body parts to relieve these sensations[53]
- Periodic limb movement disorder (PLMD), which occurs during sleep and can cause arousals of which the sleeper is unaware[54]
- Pain:[55] an injury or condition that causes pain can preclude an individual from finding a comfortable position in which to fall asleep, and can also cause awakening.
- Hormone shifts such as those that precede menstruation and those during menopause[56]
- Life events such as fear, stress, anxiety, emotional or mental tension, work problems, financial stress, birth of a child, and bereavement[53]
- Gastrointestinal issues such as heartburn or constipation[57]
- Mental, neurobehavioral, or neurodevelopmental disorders such as bipolar disorder, clinical depression, generalized anxiety disorder, post traumatic stress disorder, schizophrenia, obsessive compulsive disorder, autism, dementia,[58]: 326 ADHD,[59] and FASD
- Disturbances of the circadian rhythm, such as shift work and jet lag, can cause an inability to sleep at some times of the day and excessive sleepiness at other times of the day. Chronic circadian rhythm disorders are characterized by similar symptoms.[51]
- Certain neurological disorders such as brain lesions, or a history of traumatic brain injury[60]
- Medical conditions such as hyperthyroidism[2]
- Abuse of over-the-counter or prescription sleep aids (sedative or depressant drugs) can produce rebound insomnia[51]
- Poor sleep hygiene, e.g., noise or over-consumption of caffeine[51]
- A rare genetic condition can cause a prion-based, permanent and eventually fatal form of insomnia called fatal familial insomnia[61]
- Physical exercise: exercise-induced insomnia is common in athletes in the form of prolonged sleep onset latency[62]
- Increased exposure to the blue light from artificial sources, such as phones or computers[63]
- Chronic pain[64][65]
- Lower back pain[65]
- Asthma[65]
Sleep studies using polysomnography have suggested that people who have sleep disruption have elevated night-time levels of circulating cortisol and adrenocorticotropic hormone.[66] They also have an elevated metabolic rate, which does not occur in people who do not have insomnia but whose sleep is intentionally disrupted during a sleep study. Studies of brain metabolism using positron emission tomography (PET) scans indicate that people with insomnia have higher metabolic rates by night and by day. The question remains whether these changes are the causes or consequences of long-term insomnia.[67]
Genetics
[edit]Heritability estimates of insomnia vary between 38% in males to 59% in females.[68] A genome-wide association study (GWAS) identified 3 genomic loci and 7 genes that influence the risk of insomnia, and showed that insomnia is highly polygenic.[69] In particular, a strong positive association was observed for the MEIS1 gene in both males and females. This study showed that the genetic architecture of insomnia strongly overlaps with psychiatric disorders and metabolic traits.
It has been hypothesized that epigenetics might also influence insomnia through a controlling process of both sleep regulation and brain-stress response having an impact as well on the brain plasticity.[70]
Substance-induced
[edit]Alcohol-induced
[edit]Alcohol is often used as a form of self-treatment of insomnia to induce sleep. However, alcohol use to induce sleep can be a cause of insomnia. Long-term use of alcohol is associated with a decrease in NREM stage 3 and 4 sleep as well as suppression of REM sleep and REM sleep fragmentation. Frequent moving between sleep stages occurs with; awakenings due to headaches, the need to urinate, dehydration, and excessive sweating. Glutamine rebound also plays a role as when someone is drinking; alcohol inhibits glutamine, one of the body's natural stimulants. When the person stops drinking, the body tries to make up for lost time by producing more glutamine than it needs. The increase in glutamine levels stimulates the brain while the drinker is trying to sleep, keeping them from reaching the deepest levels of sleep.[71] Stopping chronic alcohol use can also lead to severe insomnia with vivid dreams. During withdrawal, REM sleep is typically exaggerated as part of a rebound effect.[72]
Benzodiazepine-induced
[edit]Like alcohol, benzodiazepines, such as alprazolam, clonazepam, lorazepam, and diazepam, are commonly used to treat insomnia in the short-term (both prescribed and self-medicated), but worsen sleep in the long-term. While benzodiazepines can put people to sleep (i.e., inhibit NREM stage 1 and 2 sleep), while asleep, the drugs disrupt sleep architecture: decreasing sleep time, delaying time to REM sleep, and decreasing deep slow-wave sleep (the most restorative part of sleep for both energy and mood).[73][74][75]
Opioid-induced
[edit]Opioid medications such as hydrocodone, oxycodone, and morphine are used for insomnia that is associated with pain due to their analgesic properties and hypnotic effects. Opioids can fragment sleep and decrease REM and stage 2 sleep. By producing analgesia and sedation, opioids may be appropriate in carefully selected patients with pain-associated insomnia.[55] However, dependence on opioids can lead to long-term sleep disturbances.[76]
Risk factors
[edit]Insomnia affects people of all age groups but people in the following groups have a higher chance of acquiring insomnia:[77]
- Individuals older than 60
- History of mental health disorder including depression, etc.
- Emotional stress
- Working late night shifts
- Traveling through different time zones[11]
- Having chronic diseases such as diabetes, kidney disease, lung disease, Alzheimer's, or heart disease[78]
- Alcohol or drug use disorders
- Gastrointestinal reflux disease
- Heavy smoking
- Work stress[79]
- Individuals of low SES[80]
- Urban Neighborhoods [80]
- Household stress[80]
Mechanism
[edit]Two main models exists as to the mechanism of insomnia, cognitive and physiological. The cognitive model suggests rumination and hyperarousal contribute to preventing a person from falling asleep and might lead to an episode of insomnia.
The physiological model is based upon three major findings in people with insomnia; firstly, increased urinary cortisol and catecholamines have been found suggesting increased activity of the HPA axis and arousal; second, increased global cerebral glucose utilization during wakefulness and NREM sleep in people with insomnia; and lastly, increased full body metabolism and heart rate in those with insomnia. All these findings taken together suggest a deregulation of the arousal system, cognitive system, and HPA axis all contributing to insomnia.[9][81] However, it is unknown if the hyperarousal is a result of, or cause of insomnia. Altered levels of the inhibitory neurotransmitter GABA have been found, but the results have been inconsistent, and the implications of altered levels of such a ubiquitous neurotransmitter are unknown. Studies on whether insomnia is driven by circadian control over sleep or a wake dependent process have shown inconsistent results, but some literature suggests a deregulation of the circadian rhythm based on core temperature.[82] Increased beta activity and decreased delta wave activity has been observed on electroencephalograms; however, the implication of this is unknown.[83]
Around half of post-menopausal women experience sleep disturbances, and generally sleep disturbance is about twice as common in women as men; this appears to be due in part, but not completely, to changes in hormone levels, especially in and post-menopause.[56][84]
Changes in sex hormones in both men and women as they age may account in part for increased prevalence of sleep disorders in older people.[85]
Diagnosis
[edit]In medicine, insomnia is widely measured using the Athens insomnia scale.[86] It is measured using eight different parameters related to sleep, finally represented as an overall scale which assesses an individual's sleep pattern.
A qualified sleep specialist should be consulted for the diagnosis of any sleep disorder so the appropriate measures can be taken. Past medical history and a physical examination need to be done to eliminate other conditions that could be the cause of insomnia. After all other conditions are ruled out a comprehensive sleep history should be taken. The sleep history should include sleep habits, medications (prescription and non-prescription), alcohol consumption, nicotine and caffeine intake, co-morbid illnesses, and sleep environment.[87] A sleep diary can be used to keep track of the individual's sleep patterns. The diary should include time to bed, total sleep time, time to sleep onset, number of awakenings, use of medications, time of awakening, and subjective feelings in the morning.[87] The sleep diary can be replaced or validated by the use of out-patient actigraphy for a week or more, using a non-invasive device that measures movement.[88]
Workers who complain of insomnia should not routinely have polysomnography to screen for sleep disorders.[89] This test may be indicated for patients with symptoms in addition to insomnia, including sleep apnea, obesity, a thick neck diameter, or high-risk fullness of the flesh in the oropharynx.[89] Usually, the test is not needed to make a diagnosis, and insomnia especially for working people can often be treated by changing a job schedule to make time for sufficient sleep and by improving sleep hygiene.[89]
Some patients may need to do an overnight sleep study to determine if insomnia is present. Such a study will commonly involve assessment tools including a polysomnogram and the multiple sleep latency test. Specialists in sleep medicine are qualified to diagnose disorders within the, according to the ICSD, 81 major sleep disorder diagnostic categories.[90] Patients with some disorders, including delayed sleep phase disorder, are often mis-diagnosed with primary insomnia; when a person has trouble getting to sleep and awakening at desired times, but has a normal sleep pattern once asleep, a circadian rhythm disorder is a likely cause.
In many cases, insomnia is co-morbid with another disease, side-effects from medications, or a psychological problem. Approximately half of all diagnosed insomnia is related to psychiatric disorders.[91] For those who have depression, "insomnia should be regarded as a co-morbid condition, rather than as a secondary one;" insomnia typically predates psychiatric symptoms.[91] "In fact, it is possible that insomnia represents a significant risk for the development of a subsequent psychiatric disorder."[9] Insomnia occurs in between 60% and 80% of people with depression.[92] This may partly be due to treatment used for depression.[92]
Determination of causation is not necessary for a diagnosis.[91]
DSM-5 criteria
[edit]The DSM-5 criteria for insomnia include the following:[93]
Predominant complaint of dissatisfaction with sleep quantity or quality, associated with one (or more) of the following symptoms:
- Difficulty initiating sleep. (In children, this may manifest as difficulty initiating sleep without caregiver intervention.)
- Difficulty maintaining sleep, characterized by frequent awakenings or problems returning to sleep after awakenings. (In children, this may manifest as difficulty returning to sleep without caregiver intervention.)
- Early-morning awakening with inability to return to sleep.
In addition:
- The sleep disturbance causes clinically significant distress or impairment in social, occupational, educational, academic, behavioral, or other important areas of functioning.
- The sleep difficulty occurs at least three nights per week.
- The sleep difficulty is present for at least three months.
- The sleep difficulty occurs despite adequate opportunity for sleep.
- The insomnia is not better explained by and does not occur exclusively during the course of another sleep-wake disorder (e.g., narcolepsy, a breathing-related sleep disorder, a circadian rhythm sleep-wake disorder, a parasomnia).
- The insomnia is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a medication).
The DSM-IV TR includes insomnia but does not fully elaborate on the symptoms compared to the DSM-5. Instead of early-morning waking as a symptom, the DSM-IV-TR listed “nonrestorative sleep” as a primary symptom. The duration of the experience was also vague in the DSM-IV-TR. The DSM-IV-TR stated that symptoms had to be present for a month, whereas in the DSM-5 it stated symptoms had to be present for three months and occur at least 3 nights a week (Gillette).
Types
[edit]Insomnia can be classified as transient, acute, or chronic.
- Transient insomnia lasts for less than a week. It can be caused by another disorder, by changes in the sleep environment, by the timing of sleep, severe depression, or by stress. Its consequences – sleepiness and impaired psychomotor performance – are similar to those of sleep deprivation.[94]
- Acute insomnia is the inability to consistently sleep well for a period of less than a month. Insomnia is present when there is difficulty initiating or maintaining sleep or when the sleep that is obtained is non-refreshing or of poor quality. These problems occur despite adequate opportunity and circumstances for sleep and they must result in problems with daytime function.[95] Hyperarousal can be linked to acute insomnia since it activates the body's fight-or-flight response. When we encounter stress or danger, our bodies naturally become more alert, which can interfere with our capacity to both fall asleep and remain asleep. This heightened state of arousal can be useful in the short term during threatening situations, but if it continues over an extended period, it can result in acute insomnia.[96] Acute insomnia is also known as short term insomnia or stress related insomnia.[97]
- Chronic insomnia lasts for longer than a month. It can be caused by another disorder, or it can be a primary disorder. Common causes of chronic insomnia include persistent stress, trauma, work schedules, poor sleep habits, medications, and other mental health disorders.[98] When an individual consistently engages in behaviors that disrupt their sleep, such as irregular sleep schedules, spending excessive time awake in bed, or engaging in stimulating activities close to bedtime, it can lead to conditioned wakefulness contributing to chronic insomnia.[99] People with high levels of stress hormones or shifts in the levels of cytokines are more likely than others to have chronic insomnia.[100] Its effects can vary according to its causes. They might include muscular weariness, hallucinations, and/or mental fatigue.[94]
Prevention
[edit]Prevention and treatment of insomnia may require a combination of cognitive behavioral therapy,[14] medications,[101] and lifestyle changes.[102]
Among lifestyle practices, going to sleep and waking up at the same time each day can create a steady pattern which may help to prevent insomnia.[11] Avoidance of vigorous exercise and caffeinated drinks a few hours before going to sleep is recommended, while exercise earlier in the day may be beneficial.[102] Other practices to improve sleep hygiene may include:[102][103]
- Avoiding or limiting naps
- Treating pain at bedtime
- Avoiding large meals, beverages, alcohol, and nicotine before bedtime
- Finding soothing ways to relax into sleep, including use of white noise
- Making the bedroom suitable for sleep by keeping it dark, cool, and free of devices, such as clocks, cell phones, or televisions
- Maintain regular exercise
- Try relaxing activities before sleeping
Management
[edit]It is recommended to rule out medical and psychological causes before deciding on the treatment for insomnia.[104] Cognitive behavioral therapy is generally the first line treatment once this has been done.[105] It has been found to be effective for chronic insomnia.[14] The beneficial effects, in contrast to those produced by medications, may last well beyond the stopping of therapy.[106]
Medications have been used mainly to reduce symptoms in insomnia of short duration; their role in the management of chronic insomnia remains unclear.[8] Several different types of medications may be used.[107][108][101] Many doctors do not recommend relying on prescription sleeping pills for long-term use.[102] It is also important to identify and treat other medical conditions that may be contributing to insomnia, such as depression, breathing problems, and chronic pain.[102][109] As of 2022, many people with insomnia were reported as not receiving overall sufficient sleep or treatment for insomnia.[110][111]
Non-medication based
[edit]Non-medication based strategies have comparable efficacy to hypnotic medication for insomnia and they may have longer lasting effects. Hypnotic medication is only recommended for short-term use because dependence with rebound withdrawal effects upon discontinuation or tolerance can develop.[112]
Non medication based strategies provide long lasting improvements to insomnia and are recommended as a first line and long-term strategy of management. Behavioral sleep medicine (BSM) tries to address insomnia with non-pharmacological treatments. The BSM strategies used to address chronic insomnia include attention to sleep hygiene, stimulus control, behavioral interventions, sleep-restriction therapy, paradoxical intention, patient education, and relaxation therapy.[113] Some examples are keeping a journal, restricting the time spent awake in bed, practicing relaxation techniques, and maintaining a regular sleep schedule and a wake-up time.[109] Behavioral therapy can assist a patient in developing new sleep behaviors to improve sleep quality and consolidation. Behavioral therapy may include, learning healthy sleep habits to promote sleep relaxation, undergoing light therapy to help with worry-reduction strategies and regulating the circadian clock.[109]
Music may improve insomnia in adults (see music and sleep).[114] EEG biofeedback has demonstrated effectiveness in the treatment of insomnia with improvements in duration as well as quality of sleep.[115] Self-help therapy (defined as a psychological therapy that can be worked through on one's own) may improve sleep quality for adults with insomnia to a small or moderate degree.[116]
Stimulus control therapy is a treatment for patients who have conditioned themselves to associate the bed, or sleep in general, with a negative response. As stimulus control therapy involves taking steps to control the sleep environment, it is sometimes referred interchangeably with the concept of sleep hygiene. Examples of such environmental modifications include using the bed for sleep and sex only, not for activities such as reading or watching television; waking up at the same time every morning, including on weekends; going to bed only when sleepy and when there is a high likelihood that sleep will occur; leaving the bed and beginning an activity in another location if sleep does not occur in a reasonably brief period of time after getting into bed (commonly ~20 min); reducing the subjective effort and energy expended trying to fall asleep; avoiding exposure to bright light during night-time hours, and eliminating daytime naps.[117]
A component of stimulus control therapy is sleep restriction, a technique that aims to match the time spent in bed with actual time spent asleep. This technique involves maintaining a strict sleep-wake schedule, sleeping only at certain times of the day and for specific amounts of time to induce mild sleep deprivation. Complete treatment usually lasts up to 3 weeks and involves making oneself sleep for only a minimum amount of time that they are actually capable of on average, and then, if capable (i.e. when sleep efficiency improves), slowly increasing this amount (~15 min) by going to bed earlier as the body attempts to reset its internal sleep clock. Bright light therapy may be effective for insomnia.[118]
Paradoxical intention is a cognitive reframing technique where the insomniac, instead of attempting to fall asleep at night, makes every effort to stay awake (i.e. essentially stops trying to fall asleep). One theory that may explain the effectiveness of this method is that by not voluntarily making oneself go to sleep, it relieves the performance anxiety that arises from the need or requirement to fall asleep, which is meant to be a passive act. This technique has been shown to reduce sleep effort and performance anxiety and also lower subjective assessment of sleep-onset latency and overestimation of the sleep deficit (a quality found in many insomniacs).[119]
Sleep hygiene
[edit]Sleep hygiene is a common term for all of the behaviors which relate to the promotion of good sleep. They include habits which provide a good foundation for sleep and help to prevent insomnia. However, sleep hygiene alone may not be adequate to address chronic insomnia.[88] Sleep hygiene recommendations are typically included as one component of cognitive behavioral therapy for insomnia (CBT-I).[88][6] Recommendations include reducing caffeine, nicotine, and alcohol consumption, maximizing the regularity and efficiency of sleep episodes, minimizing medication usage and daytime napping, the promotion of regular exercise, and the facilitation of a positive sleep environment.[120] The creation of a positive sleep environment may also be helpful in reducing the symptoms of insomnia.[121] On the other hand, a systematic review by the AASM concluded that clinicians should not prescribe sleep hygiene for insomnia due to the evidence of absence of its efficacy and potential delaying of adequate treatment, recommending instead that effective therapies such as CBT-i should be preferred.[13]
Cognitive behavioral therapy
[edit]There is some evidence that cognitive behavioral therapy for insomnia (CBT-I) is superior in the long-term to benzodiazepines and the nonbenzodiazepines in the treatment and management of insomnia.[122] In this therapy, patients are taught improved sleep habits and relieved of counter-productive assumptions about sleep. Common misconceptions and expectations that can be modified include:
- Unrealistic sleep expectations.
- Misconceptions about insomnia causes.
- Amplifying the consequences of insomnia.
- Performance anxiety after trying for so long to have a good night's sleep by controlling the sleep process.
Numerous studies have reported positive outcomes of combining cognitive behavioral therapy for insomnia treatment with treatments such as stimulus control and the relaxation therapies. Hypnotic medications are equally effective in the short-term treatment of insomnia, but their effects wear off over time due to tolerance. The effects of CBT-I have sustained and lasting effects on treating insomnia long after therapy has been discontinued.[123][124] The addition of hypnotic medications with CBT-I adds no benefit in insomnia. The long lasting benefits of a course of CBT-I shows superiority over pharmacological hypnotic drugs. Even in the short term when compared to short-term hypnotic medication such as zolpidem, CBT-I still shows significant superiority. Thus CBT-I is recommended as a first line treatment for insomnia.[125]
Common forms of CBT-I treatments include stimulus control therapy, sleep restriction, sleep hygiene, improved sleeping environments, relaxation training, paradoxical intention, and biofeedback.[126]
CBT is the well-accepted form of therapy for insomnia since it has no known adverse effects, whereas taking medications to alleviate insomnia symptoms have been shown to have adverse side effects.[127] Nevertheless, the downside of CBT is that it may take a lot of time and motivation.[128]
Acceptance and commitment therapy
[edit]Treatments based on the principles of acceptance and commitment therapy (ACT) and metacognition have emerged as alternative approaches to treating insomnia.[129] ACT rejects the idea that behavioral changes can help insomniacs achieve better sleep, since they require "sleep efforts" - actions which create more "struggle" and arouse the nervous system, leading to hyperarousal.[130] The ACT approach posits that acceptance of the negative feelings associated with insomnia can, in time, create the right conditions for sleep. Mindfulness practice is a key feature of this approach, although mindfulness is not practised to induce sleep (this in itself is a sleep effort to be avoided) but rather as a longer-term activity to help calm the nervous system and create the internal conditions from which sleep can emerge.
A key distinction between CBT-i and ACT lies in the divergent approaches to time spent awake in bed. Proponents of CBT-i advocate minimizing time spent awake in bed, on the basis that this creates cognitive association between being in bed and wakefulness. The ACT approach proposes that avoiding time in bed may increase the pressure to sleep and arouse the nervous system further.[130]
Research has shown that "ACT has a significant effect on primary and comorbid insomnia and sleep quality, and ... can be used as an appropriate treatment method to control and improve insomnia".[131]
Internet interventions
[edit]Despite the therapeutic effectiveness and proven success of CBT, treatment availability is significantly limited by a lack of trained clinicians, poor geographical distribution of knowledgeable professionals, and expense.[132] One way to potentially overcome these barriers is to use the Internet to deliver treatment, making this effective intervention more accessible and less costly. The Internet has already become a critical source of health-care and medical information.[133] Although the vast majority of health websites provide general information,[133][134] there is growing research literature on the development and evaluation of Internet interventions.[135][136]
These online programs are typically behaviorally-based treatments that have been operationalized and transformed for delivery via the Internet. They are usually highly structured; automated or human supported; based on effective face-to-face treatment; personalized to the user; interactive; enhanced by graphics, animations, audio, and possibly video; and tailored to provide follow-up and feedback.[136]
There is good evidence for the use of computer based CBT for insomnia.[137]
Medications
[edit]Many people with insomnia use sleeping tablets and other sedatives. In some places medications are prescribed in over 95% of cases.[138] They, however, are a second line treatment.[139] In 2019, the US Food and Drug Administration stated it is going to require warnings for eszopiclone, zaleplon, and zolpidem, due to concerns about serious injuries resulting from abnormal sleep behaviors, including sleepwalking or driving a vehicle while asleep.[140]
The percentage of adults using a prescription sleep aid increases with age. During 2005–2010, about 4% of U.S. adults aged 20 and over reported that they took prescription sleep aids in the past 30 days. Rates of use were lowest among the youngest age group (those aged 20–39) at about 2%, increased to 6% among those aged 50–59, and reached 7% among those aged 80 and over. More adult women (5%) reported using prescription sleep aids than adult men (3%). Non-Hispanic white adults reported higher use of sleep aids (5%) than non-Hispanic black (3%) and Mexican-American (2%) adults. No difference was shown between non-Hispanic black adults and Mexican-American adults in use of prescription sleep aids.[141]
Antihistamines
[edit]As an alternative to taking prescription drugs, some evidence shows that an average person seeking short-term help may find relief by taking over-the-counter antihistamines such as diphenhydramine or doxylamine.[142] Diphenhydramine and doxylamine are widely used in nonprescription sleep aids. They are the most effective over-the-counter sedatives currently available, at least in much of Europe, Canada, Australia, and the United States, and are more sedating than some prescription hypnotics.[143] Antihistamine effectiveness for sleep may decrease over time, and anticholinergic side-effects (such as dry mouth) may also be a drawback with these particular drugs. While addiction does not seem to be an issue with this class of drugs, they can induce dependence and rebound effects upon abrupt cessation of use.[144] However, people whose insomnia is caused by restless legs syndrome may have worsened symptoms with antihistamines.[145]
Antidepressants
[edit]While insomnia is a common symptom of depression, antidepressants are effective for treating sleep problems whether or not they are associated with depression. While all antidepressants help regulate sleep, some antidepressants, such as amitriptyline, doxepin, mirtazapine, trazodone, and trimipramine, can have an immediate sedative effect, and are prescribed to treat insomnia.[146] Trazodone was at the beginning of the 2020s the biggest prescribed drug for sleep in the United States despite not being indicated for sleep.[147]
Amitriptyline, doxepin, and trimipramine all have antihistaminergic, anticholinergic, antiadrenergic, and antiserotonergic properties, which contribute to both their therapeutic effects and side effect profiles, while mirtazapine's actions are primarily antihistaminergic and antiserotonergic and trazodone's effects are primarily antiadrenergic and antiserotonergic. Mirtazapine is known to decrease sleep latency (i.e., the time it takes to fall asleep), promoting sleep efficiency and increasing the total amount of sleeping time in people with both depression and insomnia.[148][149]
Agomelatine, a melatonergic antidepressant with claimed sleep-improving qualities that does not cause daytime drowsiness,[150] is approved for the treatment of depression though not sleep conditions in the European Union[151] and Australia.[152] After trials in the United States, its development for use there was discontinued in October 2011[153] by Novartis, who had bought the rights to market it there from the European pharmaceutical company Servier.[154]
A 2018 Cochrane review found the safety of taking antidepressants for insomnia to be uncertain with no evidence supporting long term use.[155]
Melatonin agonists
[edit]Melatonin receptor agonists such as melatonin and ramelteon are used in the treatment of insomnia. The evidence for melatonin in treating insomnia is generally poor.[156] There is low-quality evidence that it may speed the onset of sleep by 6 minutes.[156] Ramelteon does not appear to speed the onset of sleep or the amount of sleep a person gets.[156]
Usage of melatonin as a treatment for insomnia in adults has increased from 0.4% between 1999 and 2000 to nearly 2.1% between 2017 and 2018.[157]
While the use of melatonin in the short-term has been proven to be generally safe and it is shown to not be a dependent medication, side effects can still occur.[158]
Most common side effects of melatonin include:[159]
- Headache
- Dizziness
- Nausea
- Daytime drowsiness
Prolonged-release melatonin may improve quality of sleep in older people with minimal side effects.[160][161]
Studies have also shown that children who are on the autism spectrum or have learning disabilities, attention-deficit hyperactivity disorder (ADHD) or related neurological diseases can benefit from the use of melatonin. This is because they often have trouble sleeping due to their disorders. For example, children with ADHD tend to have trouble falling asleep because of their hyperactivity and, as a result, tend to be tired during most of the day. Another cause of insomnia in children with ADHD is the use of stimulants used to treat their disorder. Children who have ADHD then, as well as the other disorders mentioned, may be given melatonin before bedtime in order to help them sleep.[162]
Benzodiazepines
[edit]
The most commonly used class of hypnotics for insomnia are the benzodiazepines.[58]: 363 Benzodiazepines are not significantly better for insomnia than antidepressants.[164] Chronic users of hypnotic medications for insomnia do not have better sleep than chronic insomniacs not taking medications. In fact, chronic users of hypnotic medications have more regular night-time awakenings than insomniacs not taking hypnotic medications.[165] Many have concluded that these drugs cause an unjustifiable risk to the individual and to public health and lack evidence of long-term effectiveness. It is preferred that hypnotics be prescribed for only a few days at the lowest effective dose and avoided altogether wherever possible, especially in the elderly.[166] Between 1993 and 2010, the prescribing of benzodiazepines to individuals with sleep disorders has decreased from 24% to 11% in the US, coinciding with the first release of nonbenzodiazepines.[167]
The benzodiazepine and nonbenzodiazepine hypnotic medications also have a number of side-effects such as day time fatigue, motor vehicle crashes and other accidents, cognitive impairments, and falls and fractures. Elderly people are more sensitive to these side-effects.[168] Some benzodiazepines have demonstrated effectiveness in sleep maintenance in the short term but in the longer term benzodiazepines can lead to tolerance, physical dependence, benzodiazepine withdrawal syndrome upon discontinuation, and long-term worsening of sleep, especially after consistent usage over long periods of time. Benzodiazepines, while inducing unconsciousness, actually worsen sleep as – like alcohol – they promote light sleep while decreasing time spent in deep sleep.[169] A further problem is, with regular use of short-acting sleep aids for insomnia, daytime rebound anxiety can emerge.[170] Although there is little evidence for benefit of benzodiazepines in insomnia compared to other treatments and evidence of major harm, prescriptions have continued to increase.[171] This is likely due to their addictive nature, both due to misuse and because – through their rapid action, tolerance and withdrawal they can "trick" insomniacs into thinking they are helping with sleep. There is a general awareness that long-term use of benzodiazepines for insomnia in most people is inappropriate and that a gradual withdrawal is usually beneficial due to the adverse effects associated with the long-term use of benzodiazepines and is recommended whenever possible.[172][173]
Benzodiazepines all bind unselectively to the GABAA receptor.[164] Some theorize that certain benzodiazepines (hypnotic benzodiazepines) have significantly higher activity at the α1 subunit of the GABAA receptor compared to other benzodiazepines (for example, triazolam and temazepam have significantly higher activity at the α1 subunit compared to alprazolam and diazepam, making them superior sedative-hypnotics – alprazolam and diazepam, in turn, have higher activity at the α2 subunit compared to triazolam and temazepam, making them superior anxiolytic agents). Modulation of the α1 subunit is associated with sedation, motor impairment, respiratory depression, amnesia, ataxia, and reinforcing behavior (drug-seeking behavior). Modulation of the α2 subunit is associated with anxiolytic activity and disinhibition. For this reason, certain benzodiazepines may be better suited to treat insomnia than others.[121]
Z-Drugs
[edit]Nonbenzodiazepine or Z-drug sedative–hypnotic drugs, such as zolpidem, zaleplon, zopiclone, and eszopiclone, are a class of hypnotic medications that are similar to benzodiazepines in their mechanism of action, and indicated for mild to moderate insomnia. Their effectiveness at improving time to sleeping is slight, and they have similar—though potentially less severe—side effect profiles compared to benzodiazepines.[174] Prescribing of nonbenzodiazepines has seen a general increase since their initial release on the US market in 1992, from 2.3% in 1993 among individuals with sleep disorders to 13.7% in 2010.[167]
Orexin antagonists
[edit]Orexin receptor antagonists are a more recently introduced class of sleep medications and include suvorexant, lemborexant, and daridorexant, all of which are FDA-approved for treatment of insomnia characterized by difficulties with sleep onset and/or sleep maintenance.[175][176] They are oriented towards blocking signals in the brain that stimulate wakefulness, therefore claiming to address insomnia without creating dependence. There are three dual orexin receptor (DORA) drugs on the market: Belsomra (Merck), Dayvigo (Eisai) and Quviviq (Idorsia).[147]
Antipsychotics
[edit]Certain atypical antipsychotics, particularly quetiapine, olanzapine, and risperidone, are used in the treatment of insomnia.[177][178] However, while common, use of antipsychotics for this indication is not recommended as the evidence does not demonstrate a benefit, and the risk of adverse effects are significant.[177][179][180][181] A major 2022 systematic review and network meta-analysis of medications for insomnia in adults found that quetiapine did not demonstrate any short-term benefits for insomnia.[182] Some of the more serious adverse effects may also occur at the low doses used, such as dyslipidemia and neutropenia.[183][184] Such concerns of risks at low doses are supported by Danish observational studies that showed an association of use of low-dose quetiapine (excluding prescriptions filled for tablet strengths >50 mg) with an increased risk of major cardiovascular events as compared to use of Z-drugs, with most of the risk being driven by cardiovascular death.[185] Laboratory data from an unpublished analysis of the same cohort also support the lack of dose-dependency of metabolic side effects, as new use of low-dose quetiapine was associated with a risk of increased fasting triglycerides at one-year follow-up.[186] Concerns regarding side effects are greater in the elderly.[187]
Other sedatives
[edit]Gabapentinoids like gabapentin and pregabalin have sleep-promoting effects but are not commonly used for treatment of insomnia.[188] Gabapentin is not effective in helping alcohol related insomnia.[189][190]
Barbiturates, while once used, are no longer recommended for insomnia due to the risk of addiction and other side effects.[191]
Comparative effectiveness
[edit]Medications for the treatment of insomnia have a wide range of effect sizes.[182] When comparing drugs such as benzodiazepines, Z-drugs, sedative antidepressants and antihistamines, quetiapine, orexin receptor antagonists, and melatonin receptor agonists, the orexin antagonist lemborexant and the Z-drug eszopiclone had the best profiles overall in terms of efficacy, tolerability, and acceptability.[182]
Alternative medicine
[edit]Herbal products, such as valerian, kava, chamomile, and lavender, have been used to treat insomnia.[192][193][194][195] However, there is no quality evidence that they are effective and safe.[192][193][194][195] The same is true for cannabis and cannabinoids.[196][197][198] It is likewise unclear whether acupuncture is useful in the treatment of insomnia.[199]
Prognosis
[edit]
A survey of 1.1 million residents in the United States found that those that reported sleeping about 7 hours per night had the lowest rates of mortality, whereas those that slept for fewer than 6 hours or more than 8 hours had higher mortality rates. Severe insomnia – sleeping less than 3.5 hours in women and 4.5 hours in men – is associated with a 15% increase in mortality, while getting 8.5 or more hours of sleep per night was associated with a 15% higher mortality rate.[200]
With this technique, it is difficult to distinguish lack of sleep caused by a disorder which is also a cause of premature death, versus a disorder which causes a lack of sleep, and the lack of sleep causing premature death. Most of the increase in mortality from severe insomnia was discounted after controlling for associated disorders. After controlling for sleep duration and insomnia, use of sleeping pills was also found to be associated with an increased mortality rate.[200]
The lowest mortality was seen in individuals who slept between six and a half and seven and a half hours per night. Even sleeping only 4.5 hours per night is associated with very little increase in mortality. Thus, mild to moderate insomnia for most people is associated with increased longevity and severe insomnia is associated only with a very small effect on mortality.[200] It is unclear why sleeping longer than 7.5 hours is associated with excess mortality.[200]
Epidemiology
[edit]Between 10% and 30% of adults have insomnia at any given point in time and up to half of people have insomnia in a given year, making it the most common sleep disorder.[9][8][10][201] About 6% of people have insomnia that is not due to another problem and lasts for more than a month.[9] People over the age of 65 are affected more often than younger people.[7] Females are more often affected than males.[8] Insomnia is 40% more common in women than in men.[202]
There are higher rates of insomnia reported among university students compared to the general population.[203]
Society and culture
[edit]The word insomnia is from Latin: in + somnus "without sleep" and -ia as a nominalizing suffix.
The popular press have published stories about people who supposedly never sleep, such as that of Thái Ngọc and Al Herpin.[204] Horne writes "everybody sleeps and needs to do so", and generally this appears true. However, he also relates from contemporary accounts the case of Paul Kern, who was shot in 1915 fighting in World War I and then "never slept again" until his death in 1955.[205] Kern appears to be a completely isolated, unique case.
References
[edit]- ^ a b c d e f g "What Is Insomnia?". Health Topics. NHLBI. 24 March 2022. Archived from the original on 28 July 2016. Retrieved 26 November 2023.
- ^ a b c d "What Causes Insomnia?". NHLBI. 13 December 2011. Archived from the original on 28 July 2016. Retrieved 9 August 2016.
- ^ a b c "How Is Insomnia Diagnosed?". NHLBI. 13 December 2011. Archived from the original on 11 August 2016. Retrieved 9 August 2016.
- ^ Watson NF, Vaughn BV (2006). Clinician's Guide to Sleep Disorders. CRC Press. p. 10. ISBN 978-0-8493-7449-4.
- ^ a b c d "How Is Insomnia Treated?". NHLBI. 13 December 2011. Archived from the original on 28 July 2016. Retrieved 9 August 2016.
- ^ a b c d e f Qaseem A, Kansagara D, Forciea MA, Cooke M, Denberg TD (July 2016). "Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians". Annals of Internal Medicine. 165 (2): 125–133. doi:10.7326/M15-2175. PMID 27136449.
- ^ a b c d e Wilson JF (January 2008). "In the clinic. Insomnia". Annals of Internal Medicine. 148 (1): ITC13–1–ITC13–16. doi:10.7326/0003-4819-148-1-200801010-01001. PMID 18166757. S2CID 42686046.
- ^ a b c d e f g "Dyssomnias" (PDF). WHO. pp. 7–11. Archived from the original (PDF) on 18 March 2009. Retrieved 25 January 2009.
- ^ a b c d e f g h i j k Roth T (August 2007). "Insomnia: definition, prevalence, etiology, and consequences". Journal of Clinical Sleep Medicine (Supplement). 3 (5 Suppl): S7–10. doi:10.5664/jcsm.26929. PMC 1978319. PMID 17824495.
- ^ a b c Tasman A, Kay J, Lieberman JA, First MB, Riba M (2015). Psychiatry, 2 Volume Set (4 ed.). John Wiley & Sons. p. 4253. ISBN 978-1-118-75336-1. Archived from the original on 2023-01-12. Retrieved 2017-09-01.
- ^ a b c Punnoose AR, Golub RM, Burke AE (June 2012). "Insomnia". JAMA (JAMA patient page). 307 (24): 2653. doi:10.1001/jama.2012.6219. PMID 22735439.
- ^ Banno M, Tsujimoto Y, Kohmura K, Dohi E, Taito S, Someko H, et al. (September 2022). "Unclear Insomnia Concept in Randomized Controlled Trials and Systematic Reviews: A Meta-Epidemiological Study". International Journal of Environmental Research and Public Health. 19 (19): 12261. doi:10.3390/ijerph191912261. PMC 9566752. PMID 36231555.
- ^ a b Edinger JD, Arnedt JT, Bertisch SM, Carney CE, Harrington JJ, Lichstein KL, et al. (February 2021). "Behavioral and psychological treatments for chronic insomnia disorder in adults: an American Academy of Sleep Medicine systematic review, meta-analysis, and GRADE assessment". Journal of Clinical Sleep Medicine. 17 (2): 263–298. doi:10.5664/jcsm.8988. PMC 7853211. PMID 33164741.
- ^ a b c Trauer JM, Qian MY, Doyle JS, Rajaratnam SM, Cunnington D (August 2015). "Cognitive Behavioral Therapy for Chronic Insomnia: A Systematic Review and Meta-analysis". Annals of Internal Medicine. 163 (3): 191–204. doi:10.7326/M14-2841. PMID 26054060. S2CID 21617330.
- ^ Attarian HP (2003). "chapter 1". Clinical Handbook of Insomnia. Springer Science & Business Media. ISBN 978-1-59259-662-1.
- ^ "Insomnia > Complications". Mayo Clinic. Archived from the original on 8 February 2009. Retrieved 5 May 2009.
- ^ Consumer Reports, Drug Effectiveness Review Project (January 2012). "Evaluating New Sleeping Pills Used to Treat: Insomnia Comparing Effectiveness, Safety, and Price" (PDF). Best Buy Drugs Consumer Reports: 4. Archived (PDF) from the original on 9 December 2013. Retrieved 4 June 2013.
- ^ "Symptoms". Archived from the original on 15 April 2019. Retrieved 15 April 2019.
- ^ Kertesz RS, Cote KA (2011). "Event-related potentials during the transition to sleep for individuals with sleep-onset insomnia". Behavioral Sleep Medicine. 9 (2): 68–85. doi:10.1080/15402002.2011.557989. PMID 21491230. S2CID 30439961.
- ^ Doghramji K (2007). Clinical Management of Insomnia. Caddo, OK: Professional Communications, Inc. p. 28. ISBN 978-1-932610-14-7.
- ^ Morin C (2003). Insomnia: A Clinician's Guide to Assessment and Treatment. New York: Kluwer Academic/Plenum Publishers. p. 16. ISBN 978-0-306-47750-8.
- ^ "What Causes Insomnia?". Archived from the original on 15 April 2019. Retrieved 24 April 2019.
- ^ "What Happens When You Sleep?". 22 December 2009. Archived from the original on 5 March 2017. Retrieved 24 February 2017.
- ^ Adler CH, Thorpy MJ (June 2005). "Sleep issues in Parkinson's disease". Neurology. 64 (12 Suppl 3): S12–20. doi:10.1212/WNL.64.12_suppl_3.S12. PMID 15994219. S2CID 24024570.
- ^ a b c Harvey AG, Tang NK (January 2012). "(Mis)perception of sleep in insomnia: a puzzle and a resolution". Psychological Bulletin. 138 (1): 77–101. doi:10.1037/a0025730. PMC 3277880. PMID 21967449.
- ^ Mei X, Zhou Q, Li X, Jing P, Wang X, Hu Z (2018). "Sleep problems in excessive technology use among adolescent: a systemic review and meta-analysis". Sleep Science and Practice. 2 (9). Springer. doi:10.1186/s41606-018-0028-9.
- ^ Peracchia S, Curcio G (2018). "Exposure to video games: effects on sleep and on post-sleep cognitive abilities. A sistematic review of experimental evidences". Sleep Science. 11 (4). Thieme Medical Publishers: 302–314. doi:10.5935/1984-0063.20180046. PMC 6361300. PMID 30746049.
- ^ Alimoradi Z, Lin CY, Broström A, Bülow PH, Bajalan Z, Griffiths MD, et al. (2019). "Internet addiction and sleep problems: A systematic review and meta-analysis". Sleep Medicine Reviews. 47. Elsevier: 51–61. doi:10.1016/j.smrv.2019.06.004. PMID 31336284. S2CID 198193864.
- ^ Jiaxin Y, Xi F, Xiaoli L, Yamin L (2020). "Association of problematic smartphone use with poor sleep quality, depression, and anxiety: A systematic review and meta-analysis". Psychiatry Research. 284. Elsevier: 112686. doi:10.1016/j.psychres.2019.112686. PMID 31757638. S2CID 207974088.
- ^ Janssen X, Martin A, Hughes AR, Hill CM, Kotronoulas G, Hesketh KR (2020). "Associations of screen time, sedentary time and physical activity with sleep in under 5s: A systematic review and meta-analysis". Sleep Medicine Reviews. 49 (101226). Elsevier: 101226. doi:10.1016/j.smrv.2019.101226. PMC 7034412. PMID 31778942.
- ^ Mac Cárthaigh S, Griffin C, Perry J (2020). "The relationship between sleep and problematic smartphone use among adolescents: A systematic review". Developmental Review. 55. Elsevier: 100897. doi:10.1016/j.dr.2020.100897. S2CID 213952365.
- ^ Li C, Cheng G, Sha T, Cheng W, Yan Y (2020). "The Relationships between Screen Use and Health Indicators among Infants, Toddlers, and Preschoolers: A Meta-Analysis and Systematic Review". International Journal of Environmental Research and Public Health. 17 (19). MDPI: 7324. doi:10.3390/ijerph17197324. PMC 7579161. PMID 33036443.
- ^ Li Y, Li G, Liu L, Wu H (2020). "Correlations between mobile phone addiction and anxiety, depression, impulsivity, and poor sleep quality among college students: A systematic review and meta-analysis". Journal of Behavioral Addictions. 9 (3). Akadémiai Kiadó: 551–571. doi:10.1556/2006.2020.00057. PMC 8943681. PMID 32903205.
- ^ Alonzo R, Hussain J, Stranges S, Anderson KK (2021). "Interplay between social media use, sleep quality, and mental health in youth: A systematic review" (PDF). Sleep Medicine Reviews. 56. Elsevier: 101414. doi:10.1016/j.smrv.2020.101414. PMID 33385767. S2CID 230107960.
- ^ Kristensen JH, Pallesen S, King DL, Hysing M, Erevik EK (2021). "Problematic Gaming and Sleep: A Systematic Review and Meta-Analysis". Frontiers in Psychiatry. 12. Frontiers Media: 675237. doi:10.3389/fpsyt.2021.675237. PMC 8216490. PMID 34163386.
- ^ Lund L, Sølvhøj IN, Danielsen D, Andersen S (2021). "Electronic media use and sleep in children and adolescents in western countries: a systematic review". BMC Public Health. 21 (1). BioMed Central: 1598. doi:10.1186/s12889-021-11640-9. PMC 8482627. PMID 34587944.
- ^ Kemp C, Pienaar PR, Rosslee DT, Lipinska G, Roden LC, Rae DE (2021). "Sleep in Habitual Adult Video Gamers: A Systematic Review". Frontiers in Neuroscience. 15. Frontiers Media: 781351. doi:10.3389/fnins.2021.781351. PMC 8797142. PMID 35095395.
- ^ Mallawaarachchi SR, Anglim J, Hooley M, Horwood S (2022). "Associations of smartphone and tablet use in early childhood with psychosocial, cognitive and sleep factors: a systematic review and meta-analysis". Early Childhood Research Quarterly. 60. Elsevier: 13–33. doi:10.1016/j.ecresq.2021.12.008.
- ^ Zhang J, Zhang X, Zhang K, Lu X, Yuan G, Yang H, et al. (2022). "An updated of meta-analysis on the relationship between mobile phone addiction and sleep disorder". Journal of Affective Disorders. 305. Elsevier: 94–101. doi:10.1016/j.jad.2022.02.008. PMID 35149136. S2CID 246738576.
- ^ Alimoradi Z, Jafari E, Potenza MN, Lin CY, Wu CY, Pakpour AH (2022). "Binge-Watching and Mental Health Problems: A Systematic Review and Meta-Analysis". International Journal of Environmental Research and Public Health. 19 (15). MDPI: 9707. doi:10.3390/ijerph19159707. PMC 9368441. PMID 35955069.
- ^ da Silva SS, da Silveira MA, de Almeida HC, do Nascimento MC, Dos Santos MA, Heimer MV (2022). "Use of digital screens by adolescents and association on sleep quality: a systematic review". Reports in Public Health. 38 (10). Sérgio Arouca National School of Public Health: e00300721. doi:10.1590/0102-311XEN300721. PMID 36259788.
- ^ Drumheller K, Fan CW (2022). "Unprecedented times and uncertain connections: A systematic review examining sleep problems and screentime during the COVID-19 pandemic". Sleep Epidemiology. 2. Elsevier: 100029. doi:10.1016/j.sleepe.2022.100029. PMC 9076584. PMID 35692715.
- ^ Chu Y, Oh Y, Gwon M, Hwang S, Jeong H, Kim HW, et al. (2023). "Dose-response analysis of smartphone usage and self-reported sleep quality: a systematic review and meta-analysis of observational studies". Journal of Clinical Sleep Medicine. 19 (3). American Academy of Sleep Medicine: 621–630. doi:10.5664/jcsm.10392. PMC 9978438. PMID 36546366.
- ^ Brautsch LA, Lund L, Andersen MM, Jennum PJ, Folker AP, Andersen S (2023). "Digital media use and sleep in late adolescence and young adulthood: A systematic review". Sleep Medicine Reviews. 68. Elsevier: 101742. doi:10.1016/j.smrv.2022.101742. PMID 36638702.
- ^ Daraj LR, AlGhareeb M, Almutawa YM, Trabelsi K, Jahrami H (2023). "Systematic Review and Meta-Analysis of the Correlation Coefficients between Nomophobia and Anxiety, Smartphone Addiction, and Insomnia Symptoms". Healthcare. 11 (14). MDPI: 2066. doi:10.3390/healthcare11142066. PMC 10380081. PMID 37510507.
- ^ Leow MQ, Chiang J, Chua TJ, Wang S, Tan NC (2023). "The relationship between smartphone addiction and sleep among medical students: A systematic review and meta-analysis". PLOS ONE. 18 (9). PLOS: e0290724. Bibcode:2023PLoSO..1890724L. doi:10.1371/journal.pone.0290724. PMC 10503710. PMID 37713408.
- ^ Pagano M, Bacaro V, Crocetti E (2023). ""Using digital media or sleeping … that is the question". A meta-analysis on digital media use and unhealthy sleep in adolescence". Computers in Human Behavior. 146. Elsevier: 107813. doi:10.1016/j.chb.2023.107813. hdl:11585/950006.
- ^ Moawad H (2020). "Primary insomnia: A lifelong problem". Psychiatric Times. Archived from the original on 29 December 2022. Retrieved 29 December 2022.
- ^ Meadows G (2015). The sleep book: How to sleep well every night. London, UK: Orion Publishing Group. p. 21.
- ^ Edinger JD (2013). Insomnia, An Issue of Sleep Medicine Clinics. Elsevier Health Sciences. p. 389. ISBN 978-0-323-18872-2. Archived from the original on 2023-03-26. Retrieved 2023-03-19.
- ^ a b c d e f "Insomnia". University of Maryland Medical Center. Archived from the original on 3 July 2013. Retrieved 11 July 2013.
- ^ Taylor DJ, Mallory LJ, Lichstein KL, Durrence HH, Riedel BW, Bush AJ (February 2007). "Comorbidity of chronic insomnia with medical problems". Sleep. 30 (2): 213–18. doi:10.1093/sleep/30.2.213. PMID 17326547.
- ^ a b "Insomnia Causes". Mayo Clinic. Archived from the original on 21 October 2013. Retrieved 11 July 2013.
- ^ "Restless Legs Syndrome/Periodic Limb Movement Disorder". National Heart Lung and Blood Institute. Archived from the original on 3 August 2013. Retrieved 11 July 2013.
- ^ a b Ramakrishnan K, Scheid DC (August 2007). "Treatment options for insomnia". American Family Physician. 76 (4): 517–26. PMID 17853625.
- ^ a b Santoro N, Epperson CN, Mathews SB (September 2015). "Menopausal Symptoms and Their Management". Endocrinology and Metabolism Clinics of North America. 44 (3): 497–515. doi:10.1016/j.ecl.2015.05.001. PMC 4890704. PMID 26316239.
- ^ "What causes insomnia?". National Heart, Lung, and Blood Institute. Archived from the original on 3 July 2013. Retrieved 11 July 2013.
- ^ a b Geddes J, Price J, McKnight R, Gelder M, Mayou R (2012). Psychiatry (4th ed.). Oxford: Oxford University Press. ISBN 978-0-19-923396-0.
- ^ Bendz LM, Scates AC (January 2010). "Melatonin treatment for insomnia in pediatric patients with attention-deficit/hyperactivity disorder". The Annals of Pharmacotherapy. 44 (1): 185–91. doi:10.1345/aph.1M365. PMID 20028959. S2CID 207263711.
- ^ Ouellet MC, Beaulieu-Bonneau S, Morin CM (2006). "Insomnia in patients with traumatic brain injury: frequency, characteristics, and risk factors". The Journal of Head Trauma Rehabilitation. 21 (3): 199–212. doi:10.1097/00001199-200605000-00001. PMID 16717498. S2CID 28255648.
- ^ Schenkein J, Montagna P (September 2006). "Self management of fatal familial insomnia. Part 1: what is FFI?". MedGenMed. 8 (3): 65. PMC 1781306. PMID 17406188.
- ^ Shi Y, Zhou Z, Ning K, Liu J (2004). "The epidemiological survey of exercise-induced insomnia in chinese athletes". Pre-Olympic Congress. Athens. Archived from the original on 9 September 2009.
- ^ Schmerler J. "Q&A: Why Is Blue Light before Bedtime Bad for Sleep?". Scientific American. Archived from the original on 16 February 2021. Retrieved 19 October 2018.
- ^ Roth T (August 2007). "Insomnia: definition, prevalence, etiology, and consequences". Journal of Clinical Sleep Medicine. 3 (5 Suppl): S7-10. doi:10.5664/jcsm.26929. PMC 1978319. PMID 17824495.
- ^ a b c "What Causes Insomnia?". Sleep Foundation. 2021. Archived from the original on 15 April 2019. Retrieved 26 February 2021.
- ^ Hirotsu C, Tufik S, Andersen ML (November 2015). "Interactions between sleep, stress, and metabolism: From physiological to pathological conditions". Sleep Science. 8 (3): 143–152. doi:10.1016/j.slsci.2015.09.002. PMC 4688585. PMID 26779321.
- ^ Mendelson WB (2008). "New Research on Insomnia: Sleep Disorders May Precede or Exacerbate Psychiatric Conditions". Psychiatric Times. 25 (7). Archived from the original on 19 October 2009.
- ^ Lind MJ, Aggen SH, Kirkpatrick RM, Kendler KS, Amstadter AB (September 2015). "A Longitudinal Twin Study of Insomnia Symptoms in Adults". Sleep. 38 (9): 1423–30. doi:10.5665/sleep.4982. PMC 4531410. PMID 26132482.
- ^ Hammerschlag AR, Stringer S, de Leeuw CA, Sniekers S, Taskesen E, Watanabe K, et al. (November 2017). "Genome-wide association analysis of insomnia complaints identifies risk genes and genetic overlap with psychiatric and metabolic traits". Nature Genetics. 49 (11): 1584–92. doi:10.1038/ng.3888. PMC 5600256. PMID 28604731.
- ^ Palagini L, Biber K, Riemann D (June 2014). "The genetics of insomnia – evidence for epigenetic mechanisms?". Sleep Medicine Reviews. 18 (3): 225–35. doi:10.1016/j.smrv.2013.05.002. PMID 23932332.
- ^ Perry L (12 October 2004). "How Hangovers Work". HowStuffWorks. Archived from the original on 15 March 2010. Retrieved 20 November 2011.
- ^ Lee-chiong T (24 April 2008). Sleep Medicine: Essentials and Review. Oxford University Press. p. 105. ISBN 978-0-19-530659-0.
- ^ Ashton H (May 2005). "The diagnosis and management of benzodiazepine dependence". Current Opinion in Psychiatry. 18 (3): 249–55. doi:10.1097/01.yco.0000165594.60434.84. PMID 16639148. S2CID 1709063.
- ^ Morin CM, Bélanger L, Bastien C, Vallières A (January 2005). "Long-term outcome after discontinuation of benzodiazepines for insomnia: a survival analysis of relapse". Behaviour Research and Therapy. 43 (1): 1–14. doi:10.1016/j.brat.2003.12.002. PMID 15531349.
- ^ Poyares D, Guilleminault C, Ohayon MM, Tufik S (1 June 2004). "Chronic benzodiazepine usage and withdrawal in insomnia patients". Journal of Psychiatric Research. 38 (3): 327–34. doi:10.1016/j.jpsychires.2003.10.003. PMID 15003439.
- ^ Asaad TA, Ghanem MH, Samee AM, El-Habiby MM (2011). "Sleep Profile in Patients with Chronic Opioid Abuse". Addictive Disorders & Their Treatment. 10: 21–28. doi:10.1097/ADT.0b013e3181fb2847. S2CID 76376646.
- ^ "Insomnia – Symptoms and causes". Mayo Clinic. Archived from the original on 24 January 2018. Retrieved 5 February 2018.
- ^ "Risk Factors For Insomnia". Archived from the original on 19 February 2020. Retrieved 14 April 2019.
- ^ Lichstein KL, Taylor DJ, McCrae CS, Ruiter ME (November 2010). "Insomnia: epidemiology and risk factors.". Principles and Practice of Sleep Medicine (Fifth ed.). Elsevier Inc. pp. 827–837. doi:10.1016/B978-1-4160-6645-3.00076-1.
- ^ a b c Billings ME, Cohen RT, Baldwin CM, Johnson DA, Palen BN, Parthasarathy S, et al. (March 2021). "Disparities in Sleep Health and Potential Intervention Models: A Focused Review". Chest. 159 (3): 1232–1240. doi:10.1016/j.chest.2020.09.249. PMC 7525655. PMID 33007324.
- ^ Bonnet MH (April 2009). "Evidence for the pathophysiology of insomnia". Sleep. 32 (4): 441–42. doi:10.1093/sleep/32.4.441. PMC 2663857. PMID 19413138.
- ^ Levenson JC, Kay DB, Buysse DJ (April 2015). "The pathophysiology of insomnia". Chest. 147 (4): 1179–92. doi:10.1378/chest.14-1617. PMC 4388122. PMID 25846534.
- ^ Mai E, Buysse DJ (1 January 2008). "Insomnia: Prevalence, Impact, Pathogenesis, Differential Diagnosis, and Evaluation". Sleep Medicine Clinics. 3 (2): 167–74. doi:10.1016/j.jsmc.2008.02.001. PMC 2504337. PMID 19122760.
- ^ Shaver JL, Woods NF (August 2015). "Sleep and menopause: a narrative review". Menopause. 22 (8): 899–915. doi:10.1097/GME.0000000000000499. PMID 26154276. S2CID 23937236.
- ^ Lord C, Sekerovic Z, Carrier J (October 2014). "Sleep regulation and sex hormones exposure in men and women across adulthood". Pathologie-Biologie. 62 (5): 302–10. doi:10.1016/j.patbio.2014.07.005. PMID 25218407.
- ^ Soldatos CR, Dikeos DG, Paparrigopoulos TJ (June 2000). "Athens Insomnia Scale: validation of an instrument based on ICD-10 criteria". Journal of Psychosomatic Research. 48 (6): 555–60. doi:10.1016/S0022-3999(00)00095-7. PMID 11033374.
- ^ a b Passarella, S, Duong, M. "Diagnosis and treatment of insomnia." 2008.
- ^ a b c Schutte-Rodin S, Broch L, Buysse D, Dorsey C, Sateia M (October 2008). "Clinical guideline for the evaluation and management of chronic insomnia in adults" (PDF). Journal of Clinical Sleep Medicine. 4 (5): 487–504. doi:10.5664/jcsm.27286. PMC 2576317. PMID 18853708. Archived (PDF) from the original on 9 February 2015. Retrieved 30 July 2015.
Actigraphy is indicated as a method to characterize circadian patterns or sleep disturbances in individuals with insomnia, ...
- ^ a b c American College of Occupational and Environmental Medicine (February 2014), "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American College of Occupational and Environmental Medicine, archived from the original on 11 September 2014, retrieved 24 February 2014
- ^ Thorpy MJ (October 2012). "Classification of sleep disorders". Neurotherapeutics. 9 (4): 687–701. doi:10.1007/s13311-012-0145-6. PMC 3480567. PMID 22976557.
- ^ a b c Wilson SJ, Nutt DJ, Alford C, Argyropoulos SV, Baldwin DS, Bateson AN, et al. (November 2010). "British Association for Psychopharmacology consensus statement on evidence-based treatment of insomnia, parasomnias and circadian rhythm disorders". Journal of Psychopharmacology. 24 (11): 1577–1601. doi:10.1177/0269881110379307. PMID 20813762. S2CID 16823040.
- ^ a b Luca A, Luca M, Calandra C (2013). "Sleep disorders and depression: brief review of the literature, case report, and nonpharmacologic interventions for depression". Clinical Interventions in Aging. 8: 1033–39. doi:10.2147/CIA.S47230. PMC 3760296. PMID 24019746.
- ^ "Sleep Wake Disorders". Diagnostic and statistical manual of mental disorders: DSM-5. Washington, D.C.: American Psychiatric Association. 2013.
- ^ a b Roth T, Roehrs T (2003). "Insomnia: epidemiology, characteristics, and consequences". Clinical Cornerstone. 5 (3): 5–15. doi:10.1016/S1098-3597(03)90031-7. PMID 14626537.
- ^ "Insomnia – sleeplessness, chronic insomnia, acute insomnia, mental ..." Archived from the original on 29 March 2008. Retrieved 29 April 2008.
- ^ Vargas I, Nguyen AM, Muench A, Bastien CH, Ellis JG, Perlis ML (January 2020). "Acute and Chronic Insomnia: What Has Time and/or Hyperarousal Got to Do with It?". Brain Sciences. 10 (2): 71. doi:10.3390/brainsci10020071. PMC 7071368. PMID 32013124.
- ^ "Acute Insomnia – What is Acute Insomnia". Sleepdisorders.about.com. Archived from the original on 29 March 2013. Retrieved 10 March 2013.
- ^ "Types of Insomnia". Sleep Foundation. 2020-08-31. Archived from the original on 2022-07-14. Retrieved 2022-07-15.
- ^ Vargas I, Nguyen AM, Muench A, Bastien CH, Ellis JG, Perlis ML (January 2020). "Acute and Chronic Insomnia: What Has Time and/or Hyperarousal Got to Do with It?". Brain Sciences. 10 (2): 71. doi:10.3390/brainsci10020071. PMC 7071368. PMID 32013124.
- ^ Simon H. "In-Depth Report: Causes of Chronic Insomnia". The New York Times. Archived from the original on 8 November 2011. Retrieved 4 November 2011.
- ^ a b Abad VC, Guilleminault C (September 2018). "Insomnia in Elderly Patients: Recommendations for Pharmacological Management". Drugs & Aging. 35 (9): 791–817. doi:10.1007/s40266-018-0569-8. PMID 30058034. S2CID 51866276.
- ^ a b c d e "Insomnia: Diagnosis and treatment". Mayo Clinic. 15 October 2016. Archived from the original on 4 October 2017. Retrieved 11 October 2018.
- ^ Pathak N (17 January 2017). "Insomnia (Acute & Chronic): Symptoms, Causes, and Treatment". WebMD. Archived from the original on 11 October 2018. Retrieved 11 October 2018.
- ^ Wortelboer U, Cohrs S, Rodenbeck A, Rüther E (2002). "Tolerability of hypnosedatives in older patients". Drugs & Aging. 19 (7): 529–39. doi:10.2165/00002512-200219070-00006. PMID 12182689. S2CID 38910586.
- ^ van Straten A, van der Zweerde T, Kleiboer A, Cuijpers P, Morin CM, Lancee J (April 2018). "Cognitive and behavioral therapies in the treatment of insomnia: A meta-analysis" (PDF). Sleep Medicine Reviews. 38: 3–16. doi:10.1016/j.smrv.2017.02.001. hdl:1871.1/6fbbd685-d526-41ec-9961-437833035f53. PMID 28392168. S2CID 3359815. Archived (PDF) from the original on 2020-11-05. Retrieved 2020-09-18.
- ^ "NIH State-of-the-Science Conference Statement on manifestations and management of chronic insomnia in adults". NIH Consensus and State-Of-The-Science Statements. 22 (2): 1–30. 2005. PMID 17308547.
- ^ Sateia MJ, Buysse DJ, Krystal AD, Neubauer DN, Heald JL (February 2017). "Clinical Practice Guideline for the Pharmacologic Treatment of Chronic Insomnia in Adults: An American Academy of Sleep Medicine Clinical Practice Guideline". Journal of Clinical Sleep Medicine. 13 (2): 307–349. doi:10.5664/jcsm.6470. PMC 5263087. PMID 27998379.
- ^ Riemann D, Perlis ML (June 2009). "The treatments of chronic insomnia: a review of benzodiazepine receptor agonists and psychological and behavioral therapies". Sleep Medicine Reviews. 13 (3): 205–14. doi:10.1016/j.smrv.2008.06.001. PMID 19201632.
- ^ a b c Merrigan JM, Buysse DJ, Bird JC, Livingston EH (February 2013). "JAMA patient page. Insomnia". JAMA. 309 (7): 733. doi:10.1001/jama.2013.524. PMID 23423421.
- ^ "Sleep Statistics - Facts and Data About Sleep 2022". Sleep Foundation. 2021-10-25. Archived from the original on 2022-07-15. Retrieved 2022-07-15.
- ^ Drake CL, Roehrs T, Roth T (December 2003). "Insomnia causes, consequences, and therapeutics: an overview". Depression and Anxiety. 18 (4): 163–76. doi:10.1002/da.10151. PMID 14661186. S2CID 19203612.
- ^ National Prescribing Service (1 February 2010). "Addressing hypnotic medicines use in primary care". NPS News. 67. Archived from the original on 1 November 2013.
- ^ Kirkwood CK (1999). "Management of insomnia". Journal of the American Pharmaceutical Association. 39 (5): 688–96, quiz 713–14. doi:10.1016/s1086-5802(15)30354-5. PMID 10533351.
- ^ Jespersen KV, Pando-Naude V, Koenig J, Jennum P, Vuust P (August 2022). "Listening to music for insomnia in adults". The Cochrane Database of Systematic Reviews. 2022 (8): CD010459. doi:10.1002/14651858.CD010459.pub3. PMC 9400393. PMID 36000763.
- ^ Lake JA (2006). Textbook of Integrative Mental Health Care. Thieme Medical Publishers. p. 313. ISBN 978-1-58890-299-3.
- ^ van Straten A, Cuijpers P (February 2009). "Self-help therapy for insomnia: a meta-analysis". Sleep Medicine Reviews. 13 (1): 61–71. doi:10.1016/j.smrv.2008.04.006. PMID 18952469.
- ^ Lande RG, Gragnani C (December 2010). "Nonpharmacologic approaches to the management of insomnia". The Journal of the American Osteopathic Association. 110 (12): 695–701. PMID 21178150.
- ^ van Maanen A, Meijer AM, van der Heijden KB, Oort FJ (October 2016). "The effects of light therapy on sleep problems: A systematic review and meta-analysis". Sleep Med Rev. 29: 52–62. doi:10.1016/j.smrv.2015.08.009. PMID 26606319. S2CID 3410636. Archived from the original on 2021-08-28. Retrieved 2020-06-30.
- ^ Kierlin L (November 2008). "Sleeping without a pill: nonpharmacologic treatments for insomnia". Journal of Psychiatric Practice. 14 (6): 403–07. doi:10.1097/01.pra.0000341896.73926.6c. PMID 19057243. S2CID 22141056.
- ^ Ellis J, Hampson SE, Cropley M (May 2002). "Sleep hygiene or compensatory sleep practices: An examination of behaviours affecting sleep in older adults". Psychology, Health & Medicine. 7 (2): 156–161. doi:10.1080/13548500120116094. S2CID 143141307.
- ^ a b "Insomnia". The Lecturio Medical Concept Library. Archived from the original on 2021-06-24. Retrieved 2021-06-24.
- ^ Mitchell MD, Gehrman P, Perlis M, Umscheid CA (May 2012). "Comparative effectiveness of cognitive behavioral therapy for insomnia: a systematic review". BMC Family Practice. 13: 40. doi:10.1186/1471-2296-13-40. PMC 3481424. PMID 22631616.
- ^ Jacobs GD, Pace-Schott EF, Stickgold R, Otto MW (September 2004). "Cognitive behavior therapy and pharmacotherapy for insomnia: a randomized controlled trial and direct comparison". Archives of Internal Medicine. 164 (17): 1888–96. doi:10.1001/archinte.164.17.1888. PMID 15451764.
- ^ Morin CM, Colecchi C, Stone J, Sood R, Brink D (March 1999). "Behavioral and pharmacological therapies for late-life insomnia: a randomized controlled trial". JAMA. 281 (11): 991–99. doi:10.1001/jama.281.11.991. PMID 10086433.
- ^ Miller KE (2005). "Cognitive Behavior Therapy vs. Pharmacotherapy for Insomnia". American Family Physician. 72 (2): 330. Archived from the original on 6 June 2011.
- ^ Ramakrishnan K, Scheid DC (August 2007). "Treatment options for insomnia". American Family Physician. 76 (4): 517–526. PMID 17853625. Archived from the original on 2022-07-27. Retrieved 2022-07-15.
- ^ Krystal AD (August 2009). "A compendium of placebo-controlled trials of the risks/benefits of pharmacological treatments for insomnia: the empirical basis for U.S. clinical practice". Sleep Medicine Reviews. 13 (4): 265–74. doi:10.1016/j.smrv.2008.08.001. PMID 19153052.
- ^ Matthews EE, Arnedt JT, McCarthy MS, Cuddihy LJ, Aloia MS (December 2013). "Adherence to cognitive behavioral therapy for insomnia: a systematic review". Sleep Medicine Reviews. 17 (6): 453–64. doi:10.1016/j.smrv.2013.01.001. PMC 3720832. PMID 23602124.
- ^ Ong JC, Ulmer CS, Manber R (November 2012). "Improving sleep with mindfulness and acceptance: a metacognitive model of insomnia". Behaviour Research and Therapy. 50 (11): 651–60. doi:10.1016/j.brat.2012.08.001. PMC 3466342. PMID 22975073.
- ^ a b Meadows, G. (2015) The sleep book: How to sleep well every night. London, UK: Orion Publishing Group, p.2-7
- ^ Salari N, Khazaie H, Hosseinian-Far A, Khaledi-Paveh B, Ghasemi H, Mohammadi M, et al. (August 2020). "The effect of acceptance and commitment therapy on insomnia and sleep quality: A systematic review". BMC Neurology. 20 (1): 300. doi:10.1186/s12883-020-01883-1. PMC 7425538. PMID 32791960.
- ^ Edinger JD, Means MK (July 2005). "Cognitive-behavioral therapy for primary insomnia". Clinical Psychology Review. 25 (5): 539–58. doi:10.1016/j.cpr.2005.04.003. PMID 15951083.
- ^ a b Fox S, Fallows D (5 October 2005). "Digital Divisions". Internet health resources. Washington, DC: Pew Internet & American Life Project. Archived from the original on 21 October 2005.
- ^ Rabasca L (2000). "Taking telehealth to the next step". Monitor on Psychology. 31: 36–37. doi:10.1037/e378852004-017. Archived from the original on 30 December 2012.
- ^ Marks IM, Cavanagh K, Gega L (2007). Hands-on Help: Computer-Aided Psychotherapy. Hove, England and New York: Psychology Press. ISBN 978-1-84169-679-9.
- ^ a b Ritterband LM, Gonder-Frederick LA, Cox DJ, Clifton AD, West RW, Borowitz SM (2003). "Internet interventions: In review, in use, and into the future". Professional Psychology: Research and Practice. 34 (5): 527–34. doi:10.1037/0735-7028.34.5.527. S2CID 161666.
- ^ Cheng SK, Dizon J (2012). "Computerised cognitive behavioural therapy for insomnia: a systematic review and meta-analysis". Psychotherapy and Psychosomatics. 81 (4): 206–16. doi:10.1159/000335379. PMID 22585048. S2CID 10527276.
- ^ Charles J, Harrison C, Britt H (May 2009). "Insomnia" (PDF). Australian Family Physician. 38 (5): 283. PMID 19458795. Archived from the original (PDF) on 12 March 2011.
- ^ Qaseem A, Kansagara D, Forciea MA, Cooke M, Denberg TD (July 2016). "Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians". Annals of Internal Medicine. 165 (2): 125–133. doi:10.7326/m15-2175. PMID 27136449.
- ^ "FDA adds Boxed Warning for risk of serious injuries caused by sleepwalking with certain prescription insomnia medicines". US Food and Drug Administration. 30 April 2019. Archived from the original on 2 May 2019. Retrieved 2 May 2019.
- ^ Chong Y, Fryer CD, Gu Q (August 2013). "Prescription sleep aid use among adults: United States, 2005-2010" (PDF). NCHS Data Brief (127). Hyattsville, Md.: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics: 1–8. PMID 24152538. Archived from the original on 2021-08-28.
- ^ Consumer Reports, Drug Effectiveness Review Project (January 2012). "Evaluating Newer Sleeping Pills Used to Treat: Insomnia. Comparing Effectiveness, Safety, and Price" (PDF). Best Buy Drugs: 3, 8, 11. Archived (PDF) from the original on 9 December 2013. Retrieved 4 June 2013.
- ^ "Doxylamine". DrugBank. DB00366. Archived from the original on 3 December 2009.
- ^ Lie JD, Tu KN, Shen DD, Wong BM (November 2015). "Pharmacological Treatment of Insomnia". P & T. 40 (11): 759–771. PMC 4634348. PMID 26609210.
- ^ "Restless Legs Syndrome Fact Sheet | National Institute of Neurological Disorders and Stroke". www.ninds.nih.gov. Archived from the original on 28 July 2017. Retrieved 29 August 2017.
- ^ Bertschy G, Ragama-Pardos E, Muscionico M, Aït-Ameur A, Roth L, Osiek C, et al. (January 2005). "Trazodone addition for insomnia in venlafaxine-treated, depressed inpatients: a semi-naturalistic study". Pharmacological Research. 51 (1): 79–84. doi:10.1016/j.phrs.2004.06.007. PMID 15519538.
- ^ a b Dunleavy K (2023-04-07). "Idorsia petitions DEA to de-schedule its insomnia drug—plus Merck and Eisai rivals". Fierce Pharma. Archived from the original on 2023-08-31. Retrieved 2023-08-31.
- ^ Winokur A, DeMartinis NA, McNally DP, Gary EM, Cormier JL, Gary KA (October 2003). "Comparative effects of mirtazapine and fluoxetine on sleep physiology measures in patients with major depression and insomnia". The Journal of Clinical Psychiatry. 64 (10): 1224–29. doi:10.4088/JCP.v64n1013. PMID 14658972.
- ^ Schittecatte M, Dumont F, Machowski R, Cornil C, Lavergne F, Wilmotte J (2002). "Effects of mirtazapine on sleep polygraphic variables in major depression". Neuropsychobiology. 46 (4): 197–201. doi:10.1159/000067812. PMID 12566938. S2CID 25351993.
- ^ Le Strat Y, Gorwood P (September 2008). "Agomelatine, an innovative pharmacological response to unmet needs". Journal of Psychopharmacology. 22 (7 Suppl): 4–8. doi:10.1177/0269881108092593. PMID 18753276. S2CID 29745284.
- ^ "Summary of Product Characteristics" (PDF). European Medicine Agency. Archived (PDF) from the original on 29 October 2014. Retrieved 14 October 2013.
- ^ "VALDOXAN® Product Information" (PDF). TGA eBusiness Services. Servier Laboratories Pty Ltd. 23 September 2013. Archived from the original on 24 March 2017. Retrieved 14 October 2013.
- ^ "Novartis drops future blockbuster agomelatine". Scrip Intelligence. 25 October 2011. Archived from the original on 11 November 2011. Retrieved 30 October 2011.
- ^ Bentham C (29 March 2006). "Servier and Novartis sign licensing agreement for agomelatine, a novel treatment for depression". Servier UK. Archived from the original on 16 April 2009. Retrieved 15 May 2009.
- ^ Everitt H, Baldwin DS, Stuart B, Lipinska G, Mayers A, Malizia AL, et al. (May 2018). "Antidepressants for insomnia in adults". The Cochrane Database of Systematic Reviews. 2018 (5): CD010753. doi:10.1002/14651858.CD010753.pub2. PMC 6494576. PMID 29761479.
- ^ a b c Brasure M, MacDonald R, Fuchs E, Olson CM, Carlyle M, Diem S, et al. (December 2015). "Management of Insomnia Disorder". AHRQ Comparative Effectiveness Reviews. Rockville (MD): Agency for Healthcare Research and Quality (US). PMID 26844312.
- ^ "Use of melatonin supplements rising among adults". National Institutes of Health (NIH). 2022-02-28. Archived from the original on 2022-06-29. Retrieved 2022-06-29.
- ^ "Pros and cons of melatonin". Mayo Clinic. Retrieved 2024-05-01.
- ^ "Pros and cons of melatonin". Mayo Clinic. Retrieved 2024-05-01.
- ^ Lyseng-Williamson KA (November 2012). "Melatonin prolonged release: in the treatment of insomnia in patients aged ≥55 years". Drugs & Aging. 29 (11): 911–23. doi:10.1007/s40266-012-0018-z. PMID 23044640. S2CID 1403262.
- ^ Lemoine P, Zisapel N (April 2012). "Prolonged-release formulation of melatonin (Circadin) for the treatment of insomnia". Expert Opinion on Pharmacotherapy. 13 (6): 895–905. doi:10.1517/14656566.2012.667076. PMID 22429105. S2CID 23291045.
- ^ Sánchez-Barceló EJ, Mediavilla MD, Reiter RJ (2011). "Clinical uses of melatonin in pediatrics". International Journal of Pediatrics. 2011: 892624. doi:10.1155/2011/892624. PMC 3133850. PMID 21760817.
- ^ "Temazepam". Websters-online-dictionary.org. Archived from the original on 30 May 2013. Retrieved 20 November 2011.
- ^ a b Buscemi N, Vandermeer B, Friesen C, Bialy L, Tubman M, Ospina M, et al. (September 2007). "The efficacy and safety of drug treatments for chronic insomnia in adults: a meta-analysis of RCTs". Journal of General Internal Medicine. 22 (9): 1335–50. doi:10.1007/s11606-007-0251-z. PMC 2219774. PMID 17619935.
- ^ Ohayon MM, Caulet M (May 1995). "Insomnia and psychotropic drug consumption". Progress in Neuro-Psychopharmacology & Biological Psychiatry. 19 (3): 421–31. doi:10.1016/0278-5846(94)00023-B. PMID 7624493. S2CID 20655328.
- ^ "What's wrong with prescribing hypnotics?". Drug and Therapeutics Bulletin. 42 (12): 89–93. December 2004. doi:10.1136/dtb.2004.421289. PMID 15587763. S2CID 40188442.
- ^ a b Kaufmann CN, Spira AP, Alexander GC, Rutkow L, Mojtabai R (June 2016). "Trends in prescribing of sedative-hypnotic medications in the USA: 1993–2010". Pharmacoepidemiology and Drug Safety. 25 (6): 637–45. doi:10.1002/pds.3951. PMC 4889508. PMID 26711081.
- ^ Glass J, Lanctôt KL, Herrmann N, Sproule BA, Busto UE (November 2005). "Sedative hypnotics in older people with insomnia: meta-analysis of risks and benefits". BMJ. 331 (7526): 1169. doi:10.1136/bmj.38623.768588.47. PMC 1285093. PMID 16284208.
- ^ Tsoi WF (March 1991). "Insomnia: drug treatment". Annals of the Academy of Medicine, Singapore. 20 (2): 269–72. PMID 1679317.
- ^ Montplaisir J (August 2000). "Treatment of primary insomnia". CMAJ. 163 (4): 389–91. PMC 80369. PMID 10976252.
- ^ Carlstedt RA (2009). Handbook of Integrative Clinical Psychology, Psychiatry, and Behavioral Medicine: Perspectives, Practices, and Research. Springer. pp. 128–30. ISBN 978-0-8261-1094-7. Archived from the original on 2020-06-04. Retrieved 2020-05-12.
- ^ Lader M, Cardinali DP, Pandi-Perumal SR (2006). Sleep and sleep disorders: a neuropsychopharmacological approach. Georgetown, Tex.: Landes Bioscience/Eurekah.com. p. 127. ISBN 978-0-387-27681-6.
- ^ Authier N, Boucher A, Lamaison D, Llorca PM, Descotes J, Eschalier A (2009). "Second meeting of the French CEIP (Centres d'Evaluation et d'Information sur la Pharmacodépendance). Part II: benzodiazepine withdrawal". Therapie. 64 (6): 365–70. doi:10.2515/therapie/2009051. PMID 20025839.
- ^ Huedo-Medina TB, Kirsch I, Middlemass J, Klonizakis M, Siriwardena AN (December 2012). "Effectiveness of non-benzodiazepine hypnotics in treatment of adult insomnia: meta-analysis of data submitted to the Food and Drug Administration". BMJ. 345: e8343. doi:10.1136/bmj.e8343. PMC 3544552. PMID 23248080.
- ^ Jacobson LH, Hoyer D, de Lecea L (January 2022). "Hypocretins (orexins): The ultimate translational neuropeptides". J Intern Med. 291 (5): 533–556. doi:10.1111/joim.13406. PMID 35043499. S2CID 248119793.
- ^ "Highlights of prescribing information" (PDF). Archived (PDF) from the original on 12 September 2014.
- ^ a b Thompson W, Quay TA, Rojas-Fernandez C, Farrell B, Bjerre LM (June 2016). "Atypical antipsychotics for insomnia: a systematic review". Sleep Med. 22: 13–17. doi:10.1016/j.sleep.2016.04.003. PMID 27544830.
- ^ Morin AK (1 March 2014). "Off-label use of atypical antipsychotic agents for treatment of insomnia". Mental Health Clinician. 4 (2): 65–72. doi:10.9740/mhc.n190091. eISSN 2168-9709.
- ^ American Psychiatric Association (September 2013), "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American Psychiatric Association, archived from the original on 3 December 2013, retrieved 30 December 2013, which cites
- American Association of Clinical Endocrinologists, North American Association for the Study of Obesity (February 2004). "Consensus development conference on antipsychotic drugs and obesity and diabetes". Diabetes Care. 27 (2): 596–601. doi:10.2337/diacare.27.2.596. PMID 14747245.
- Maglione M, Maher AR, Hu J, Wang Z, Shanman R, Shekelle PG, et al. (Sep 2011). "Off-Label Use of Atypical Antipsychotics: An Update". AHRQ Comparative Effectiveness Reviews. Rockville (MD): Agency for Healthcare Research and Quality (US). PMID 22132426.
- Nasrallah HA (January 2008). "Atypical antipsychotic-induced metabolic side effects: insights from receptor-binding profiles". Molecular Psychiatry. 13 (1): 27–35. doi:10.1038/sj.mp.4002066. PMID 17848919. S2CID 205678886.
- ^ Coe HV, Hong IS (May 2012). "Safety of low doses of quetiapine when used for insomnia". The Annals of Pharmacotherapy. 46 (5): 718–722. doi:10.1345/aph.1Q697. PMID 22510671. S2CID 9888209.
- ^ Maglione M, Maher AR, Hu J, Wang Z, Shanman R, Shekelle PG, et al. (2011). Off-Label Use of Atypical Antipsychotics: An Update. Comparative Effectiveness Reviews, No. 43. Rockville: Agency for Healthcare Research and Quality. PMID 22973576.
- ^ a b c De Crescenzo F, D'Alò GL, Ostinelli EG, Ciabattini M, Di Franco V, Watanabe N, et al. (July 2022). "Comparative effects of pharmacological interventions for the acute and long-term management of insomnia disorder in adults: a systematic review and network meta-analysis". Lancet. 400 (10347): 170–184. doi:10.1016/S0140-6736(22)00878-9. hdl:11380/1288245. PMID 35843245. S2CID 250536370.
- ^ Pillinger T, McCutcheon RA, Vano L, Mizuno Y, Arumuham A, Hindley G, et al. (January 2020). "Comparative effects of 18 antipsychotics on metabolic function in patients with schizophrenia, predictors of metabolic dysregulation, and association with psychopathology: a systematic review and network meta-analysis". The Lancet. Psychiatry. 7 (1): 64–77. doi:10.1016/s2215-0366(19)30416-x. PMC 7029416. PMID 31860457.
- ^ Yoshida K, Takeuchi H (March 2021). "Dose-dependent effects of antipsychotics on efficacy and adverse effects in schizophrenia". Behavioural Brain Research. 402: 113098. doi:10.1016/j.bbr.2020.113098. PMID 33417992. S2CID 230507941.
- ^ Højlund M, Andersen K, Ernst MT, Correll CU, Hallas J (October 2022). "Use of low-dose quetiapine increases the risk of major adverse cardiovascular events: results from a nationwide active comparator-controlled cohort study". World Psychiatry. 21 (3): 444–451. doi:10.1002/wps.21010. PMC 9453914. PMID 36073694.
- ^ Højlund M (2022-09-12). Low-dose Quetiapine: Utilization and Cardiometabolic Risk (Thesis). Syddansk Universitet. Det Sundhedsvidenskabelige Fakultet. doi:10.21996/mr3m-1783. Archived from the original on 2022-10-18. Retrieved 2022-10-18.
- ^ Conn DK, Madan R (2006). "Use of sleep-promoting medications in nursing home residents: risks versus benefits". Drugs & Aging. 23 (4): 271–87. doi:10.2165/00002512-200623040-00001. PMID 16732687. S2CID 38394552.
- ^ Atkin T, Comai S, Gobbi G (April 2018). "Drugs for Insomnia beyond Benzodiazepines: Pharmacology, Clinical Applications, and Discovery". Pharmacol Rev. 70 (2): 197–245. doi:10.1124/pr.117.014381. PMID 29487083. S2CID 3578916.
- ^ "Review finds little evidence to support gabapentinoid use in bipolar disorder or insomnia". NIHR Evidence (Plain English summary). National Institute for Health and Care Research. 17 October 2022. doi:10.3310/nihrevidence_54173. S2CID 252983016. Archived from the original on 27 November 2022. Retrieved 21 November 2022.
- ^ Hong JS, Atkinson LZ, Al-Juffali N, Awad A, Geddes JR, Tunbridge EM, et al. (March 2022). "Gabapentin and pregabalin in bipolar disorder, anxiety states, and insomnia: Systematic review, meta-analysis, and rationale". Molecular Psychiatry. 27 (3): 1339–1349. doi:10.1038/s41380-021-01386-6. PMC 9095464. PMID 34819636.
- ^ Aschenbrenner DS, Venable SJ (2009). Drug Therapy in Nursing. Lippincott Williams & Wilkins. p. 277. ISBN 978-0-7817-6587-9.
- ^ a b Leach MJ, Page AT (December 2015). "Herbal medicine for insomnia: A systematic review and meta-analysis". Sleep Med Rev. 24: 1–12. doi:10.1016/j.smrv.2014.12.003. PMID 25644982.
- ^ a b Kim J, Lee SL, Kang I, Song YA, Ma J, Hong YS, et al. (May 2018). "Natural Products from Single Plants as Sleep Aids: A Systematic Review". J Med Food. 21 (5): 433–444. doi:10.1089/jmf.2017.4064. PMID 29356580.
- ^ a b Meolie AL, Rosen C, Kristo D, Kohrman M, Gooneratne N, Aguillard RN, et al. (April 2005). "Oral nonprescription treatment for insomnia: an evaluation of products with limited evidence". J Clin Sleep Med. 1 (2): 173–87. doi:10.5664/jcsm.26314. PMID 17561634.
- ^ a b Wheatley D (July 2005). "Medicinal plants for insomnia: a review of their pharmacology, efficacy and tolerability". J Psychopharmacol. 19 (4): 414–21. doi:10.1177/0269881105053309. PMID 15982998. S2CID 34484538.
- ^ Bhagavan C, Kung S, Doppen M, John M, Vakalalabure I, Oldfield K, et al. (December 2020). "Cannabinoids in the Treatment of Insomnia Disorder: A Systematic Review and Meta-Analysis". CNS Drugs. 34 (12): 1217–1228. doi:10.1007/s40263-020-00773-x. PMID 33244728. S2CID 227174084.
- ^ Suraev AS, Marshall NS, Vandrey R, McCartney D, Benson MJ, McGregor IS, et al. (October 2020). "Cannabinoid therapies in the management of sleep disorders: A systematic review of preclinical and clinical studies". Sleep Med Rev. 53: 101339. doi:10.1016/j.smrv.2020.101339. PMID 32603954. S2CID 219452622.
- ^ Gates PJ, Albertella L, Copeland J (December 2014). "The effects of cannabinoid administration on sleep: a systematic review of human studies". Sleep Med Rev. 18 (6): 477–87. doi:10.1016/j.smrv.2014.02.005. PMID 24726015.
- ^ Cheuk DK, Yeung WF, Chung KF, Wong V (September 2012). "Acupuncture for insomnia". The Cochrane Database of Systematic Reviews. 9 (9): CD005472. doi:10.1002/14651858.CD005472.pub3. hdl:10722/198790. PMID 22972087.
- ^ a b c d Kripke DF, Garfinkel L, Wingard DL, Klauber MR, Marler MR (February 2002). "Mortality associated with sleep duration and insomnia". Archives of General Psychiatry. 59 (2): 131–36. doi:10.1001/archpsyc.59.2.131. PMID 11825133.
- ^ "What are Sleep Disorders?". Psychiatry.org. Archived from the original on 2022-10-27. Retrieved 2022-10-27.
- ^ Lamberg L (2007). "Several Sleep Disorders Reflect Gender Differences". Psychiatric News. 42 (8): 40. doi:10.1176/pn.42.10.0040.
- ^ Jiang XL, Zheng XY, Yang J, Ye CP, Chen YY, Zhang ZG, et al. (December 2015). "A systematic review of studies on the prevalence of insomnia in university students". Public Health. 129 (12): 1579–84. doi:10.1016/j.puhe.2015.07.030. PMID 26298588.
- ^ Horne J (2016). Sleeplessness Assessing Sleep Need in Society Today. Springer. p. 114. ISBN 978-3-319-30572-1. Archived from the original on 2023-01-12. Retrieved 2017-09-01.
Everyone sleeps and needs to do so
- ^ Horne J (2016). Sleeplessness Assessing Sleep Need in Society Today. Springer. p. 116. ISBN 978-3-319-30572-1. Archived from the original on 2023-01-12. Retrieved 2017-09-01.
External links
[edit]Sleep and sleep disorders | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Stages of sleep cycles | |||||||||||||||
| Brain waves | |||||||||||||||
| Sleep disorders |
| ||||||||||||||
| Daily life | |||||||||||||||
| GABAA receptor positive modulators |
|
|---|---|
| Antihistamines (H1 receptor inverse agonists) |
|
| Orexin receptor antagonists | |
| Melatonin receptor agonists | |
| Miscellaneous |
|
| |
| Proposed or recognised diagnostic categories | |
|---|---|
| Disciplines involved | |
| Associated psychiatric conditions | |
| Related topics |
|