 | |
| Clinical data | |
|---|---|
| Trade names | Bonine, Antivert, others |
| Other names | Meclozine |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a682548 |
| License data | |
| Routes of administration | By mouth, under the tongue, in the cheek |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 22 - 32%[1] |
| Metabolism | Liver (CYP2D6) |
| Elimination half-life | 5-6 hours[2] |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.008.477 |
| Chemical and physical data | |
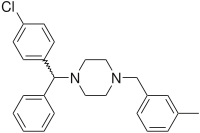
| Formula | C25H27ClN2 |
| Molar mass | 390.96 g·mol−1 |
| 3D model (JSmol) | |
| Boiling point | 230 °C (446 °F) |
| |
| |
| | |
Meclizine, sold under the brand name Bonine, among others, is an antihistamine used to treat motion sickness and dizziness (vertigo).[3] It is taken by mouth.[3] Effects generally begin in an hour and last for up to a day.[3]
Common side effects include sleepiness and dry mouth.[3] Serious side effects may include allergic reactions.[3] Use in pregnancy appears safe, but has not been well studied; use in breastfeeding is of unclear safety.[4] It is believed to work in part by anticholinergic and antihistamine mechanisms.[3]
Meclizine was patented in 1951 and came into medical use in 1953.[5] It is available as a generic medication and often over the counter.[3][6] In 2021, it was the 136th most commonly prescribed medication in the United States, with more than 4 million prescriptions.[7][8]
Medical uses
[edit]Meclizine is used to treat symptoms of motion sickness.[9]
Motion sickness
[edit]Meclizine is effective in inhibiting nausea, vomiting, and dizziness caused by motion sickness.[10]
The drug is safe for treating nausea in pregnancy and is a first-line therapy for this use.[11][12] Meclizine may not be strong enough for especially sickening motion stimuli, and second-line defenses should be tried in those cases.[13]
Vertigo
[edit]Meclizine may be used to treat vertigo, such as in those with Ménière's disease.[14][15]
Side effects
[edit]Some common side effects such as drowsiness, dry mouth, and tiredness may occur. Meclizine has been shown to have fewer dry mouth side effects than the traditional treatment for motion sickness, transdermal scopolamine.[16] A very serious allergic reaction to this drug is unlikely, but immediate medical attention should be sought if it occurs. Symptoms of a serious allergic reaction may include rash, itching, swelling, severe dizziness, and trouble breathing.[17]
Pharmacology
[edit]Pharmacodynamics
[edit]Meclizine is an antagonist at H1 receptors (Ki = 250 nM).[18] It possesses anticholinergic, central nervous system depressant, and local anesthetic effects. Its antiemetic and antivertigo effects are not fully understood, but its central anticholinergic properties are partially responsible. The drug depresses labyrinth excitability and vestibular stimulation, and it may affect the medullary chemoreceptor trigger zone.[9] The drug has been shown to reduce the magnitude of the vestibulo-ocular reflex in healthy volunteers.[19] At the same time the drug was found to have only a small (and statistically insignificant) effect on the motion sensitivity of the utricles.[19] Much as motion sickness arises from a discrepancy between multiple senses, meclizine most likely affects a wide array of sensory mechanisms related to self-motion while leaving the core vestibular response intact.[20]
Meclizine also has been reported to be a weak dopamine antagonist at D1-like and D2-like receptors[citation needed] but it does not cause catalepsy in mice, perhaps because of its anticholinergic activity.[21] The drug does not effect dopamine or serotonin reuptake.[22]
Pharmacokinetics
[edit]Meclizine reaches peak plasma concentration in about 1.5 hours and has an elimination half-life of 5-6 hours.[2] Despite its relatively short half-life, the drug is reported to remain effective for motion sickness for 12 - 24 hours.[23] Meclizine has low bioavailability (22–32%) and a delayed onset to action in part due to its poor solubility in water (0.1 mg/ml) and gastrointestinal fluid.[1] In children it has been found that taking meclizine with food increases its bioavailability slightly.[24] It is metabolized in the liver by the CYP2D6 enzyme.[2] Ten metabolites have been identified.[25] In rats, the main metabolite is norchlorcyclizine, which distributes extensively through body tissue.[26]
Chemistry
[edit]Meclizine is a first-generation antihistamine (nonselective H1 antagonist) of the piperazine class. It is structurally and pharmacologically similar to buclizine, cyclizine, and hydroxyzine.
Synthesis
[edit](4-Chlorophenyl)-phenylmethanol is halogenated with thionyl chloride before adding acetylpiperazine. The acetyl group is cleaved with diluted sulfuric acid. An N-alkylation of the piperazine ring with 3-methylbenzylchloride completes the synthesis.[27]
Alternatively, the last step can be replaced by a reductive N-alkylation with 3-methylbenzaldehyde. The reductive agent is hydrogen, and Raney nickel is used as a catalyst.[28][29]
Meclizine is obtained and used as a racemate, a 1:1 mixture of the two stereoisomers. Drug forms contain the racemic dihydrochloride.[citation needed]
Society and culture
[edit]Brand names
[edit]Meclizine is an international nonproprietary name.[30]
It is sold under the brand names Bonine, Bonamine, Antivert, Postafen, Sea Legs, and Dramamine II (Less Drowsy Formulation). Emesafene is a combination of meclizine (1/3) and pyridoxine (2/3). In Canada, Antivert Tab was a combination of meclizine and nicotinic acid.[31]
References
[edit]- ^ a b Sun J, Liu J, Zhang J, Xia H (June 2021). "Meclizine-loaded nanostructured lipid carriers to manage nausea and vomiting: Oral bioavailability improvement". Journal of Drug Delivery Science and Technology. 63: 102432. doi:10.1016/j.jddst.2021.102432.
- ^ a b c Wang Z, Lee B, Pearce D, Qian S, Wang Y, Zhang Q, et al. (September 2012). "Meclizine metabolism and pharmacokinetics: formulation on its absorption". Journal of Clinical Pharmacology. 52 (9): 1343–1349. doi:10.1177/0091270011414575. PMID 21903894.
- ^ a b c d e f g "Meclizine Hydrochloride Monograph for Professionals". Drugs.com. American Society of Health-System Pharmacists. Retrieved 22 March 2019.
- ^ "Meclizine Use During Pregnancy". Drugs.com. Retrieved 3 March 2019.
- ^ Fischer J, Ganellin CR (2006). Analogue-based Drug Discovery. John Wiley & Sons. p. 547. ISBN 9783527607495.
- ^ Cappa M, Cianfarani S, Ghizzoni L, Loche S, Maghnie M (2015). Advanced Therapies in Pediatric Endocrinology and Diabetology: Workshop, Rome, October 2014. Karger Medical and Scientific Publishers. p. 101. ISBN 9783318056372.
- ^ "The Top 300 of 2021". ClinCalc. Archived from the original on 15 January 2024. Retrieved 14 January 2024.
- ^ "Meclizine - Drug Usage Statistics". ClinCalc. Retrieved 14 January 2024.
- ^ a b Houston BT, Chowdhury YS (18 July 2022). "Meclizine". StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. PMID 32809480.
- ^ "Drugs & Medications". www.webmd.com. Retrieved 28 December 2018.
- ^ "Antiemetische Therapie bei Schwangerschaftserbrechen" [Antiemetic therapy in pregnancy]. Arznei-Telegramm (in German). 40: 87–89. 2009.
- ^ "Meclozin" [Federal Ministry of Health]. Embryotox (in German). Bundesministerium für Gesundheit.
- ^ Lawson BD, McGee HA, Castaneda MA, Golding JF, Kass SJ, McGrath CM (2 December 2009). "Evaluation of several common antimotion sickness medications and recommendations concerning their potential usefulness during special operations". Pensacola, Florida: Naval Aerospace Research Lab. Archived from the original on 27 April 2016. Retrieved 7 February 2016.
- ^ Nakashima T, Pyykkö I, Arroll MA, Casselbrant ML, Foster CA, Manzoor NF, et al. (May 2016). "Meniere's disease". Nature Reviews. Disease Primers. 2: 16028. doi:10.1038/nrdp.2016.28. PMID 27170253. S2CID 3987838.
- ^ "Meclizine". LiverTox: Clinical and Research Information on Drug-Induced Liver Injury. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases. January 2017. PMID 31643231.
- ^ Dahl E, Offer-Ohlsen D, Lillevold PE, Sandvik L (July 1984). "Transdermal scopolamine, oral meclizine, and placebo in motion sickness". Clinical Pharmacology and Therapeutics. 36 (1): 116–120. doi:10.1038/clpt.1984.148. PMID 6734040. S2CID 40691502.
- ^ "Meclizine - oral, Antivert, D-vert, Dramamine II". MedicineNet. Retrieved 7 November 2010.
- ^ Tran VT, Chang RS, Snyder SH (December 1978). "Histamine H1 receptors identified in mammalian brain membranes with [3H]mepyramine". Proceedings of the National Academy of Sciences of the United States of America. 75 (12): 6290–6294. doi:10.1073/pnas.75.12.6290. PMC 393167. PMID 282646.
- ^ a b Weerts AP, De Meyer G, Pauwels G, Vanspauwen R, Dornhoffer JL, Van de Heyning PH, et al. (2012). "Pharmaceutical countermeasures have opposite effects on the utricles and semicircular canals in man". Audiology & Neuro-Otology. 17 (4): 235–242. doi:10.1159/000337273. PMID 22517315.
- ^ Wibble T, Engström J, Verrecchia L, Pansell T (August 2020). "The effects of meclizine on motion sickness revisited". British Journal of Clinical Pharmacology. 86 (8): 1510–1518. doi:10.1111/bcp.14257. PMC 7373708. PMID 32077140.
- ^ Haraguchi K, Ito K, Kotaki H, Sawada Y, Iga T (June 1997). "Prediction of drug-induced catalepsy based on dopamine D1, D2, and muscarinic acetylcholine receptor occupancies". Drug Metabolism and Disposition. 25 (6): 675–684. PMID 9193868. Archived from the original on 28 August 2021. Retrieved 12 June 2014. "Catalepsy was assessed by the bar method: the front paws were gently placed on a horizontal metal bar with 2 mm diameter suspended 4 cm above, and the length of time the mouse maintains this abnormal posture was measured."
- ^ Oishi R, Shishido S, Yamori M, Saeki K (February 1994). "Comparison of the effects of eleven histamine H1-receptor antagonists on monoamine turnover in the mouse brain". Naunyn-Schmiedeberg's Archives of Pharmacology. 349 (2): 140–144. doi:10.1007/BF00169830. PMID 7513381.
- ^ "ANTIVERT FDA Drug Facts" (PDF). FDA. Retrieved 18 June 2024.
- ^ Kitoh H, Matsushita M, Mishima K, Nagata T, Kamiya Y, Ueda K, et al. (13 April 2020). "Pharmacokinetics and safety after once and twice a day doses of meclizine hydrochloride administered to children with achondroplasia". PLOS ONE. 15 (4): e0229639. Bibcode:2020PLoSO..1529639K. doi:10.1371/journal.pone.0229639. PMC 7153885. PMID 32282831.
- ^ Goenechea VS, Rücker G, Brzezinka H, Hoffmann G, Neugebauer M, Glanzmann G (February 1988). "[Biotransformation of meclozine in the human body]". Journal of Clinical Chemistry and Clinical Biochemistry. Zeitschrift Fur Klinische Chemie und Klinische Biochemie. 26 (2): 105–115. PMID 3367105.
- ^ Narrod SA, Wilk AL, King CT (March 1965). "Metabolism of Meclizine in the Rat". The Journal of Pharmacology and Experimental Therapeutics. 147: 380–384. PMID 14269614.
- ^ Fuhrkop JH, Li G (2003). Organic Synthesis. Concepts and Methods. Wiley. p. 237. ISBN 978-3-527-30272-7.
- ^ US 2709169, Morren H, issued 24 May 1955, assigned to Union Chimique Belge Société Anonyme
- ^ Kleemann A, Engel J, Kutscher B, Reichert D (2001). Pharmaceutical Substances. Synthesis, Patents, Applications (4th ed.). Thieme. ISBN 3-13-115134-X.
- ^ "Guidelines on the Use of INNs for Pharmaceutical Substances" (PDF). WHO. 1997. Retrieved 1 November 2013.
- ^ Wishard D. "Drug card for Meclizine". DrugBank. Canada: University of Alberta. Retrieved 7 November 2010.

