 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Glucotrol, Glucotrol XL, others |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a684060 |
| License data | |
| Pregnancy category |
|
| Routes of administration | By mouth |
| Drug class | Sulfonylurea |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 100% (regular formulation) 90% (extended release) |
| Protein binding | 98 to 99% |
| Metabolism | Liver hydroxylation |
| Elimination half-life | 2 to 5 hours |
| Excretion | Kidney and fecal |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.044.919 |
| Chemical and physical data | |
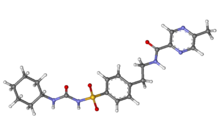
| Formula | C21H27N5O4S |
| Molar mass | 445.54 g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 208 to 209 °C (406 to 408 °F) |
| |
| |
| | |
Glipizide, sold under the brand name Glucotrol among others, is an anti-diabetic medication of the sulfonylurea class used to treat type 2 diabetes.[1][2] It is used together with a diabetic diet and exercise.[1][2] It is not indicated for use by itself in type 1 diabetes.[1][2] It is taken by mouth.[1][2] Effects generally begin within half an hour and can last for up to a day.[1]
Common side effects include nausea, diarrhea, low blood sugar, and headache.[1] Other side effects include sleepiness, skin rash, and shakiness.[3] The dose may need to be adjusted in those with liver or kidney disease.[1] Use during pregnancy or breastfeeding is not recommended.[3] It works by stimulating the pancreas to release insulin and increases tissue sensitivity to insulin.[1]
Glipizide was approved for medical use in the United States in 1984.[1] It is available as a generic medication.[1] In 2021, it was the 48th most commonly prescribed medication in the United States, with more than 13 million prescriptions.[4][5]