| Rotavirus | |
|---|---|
| |
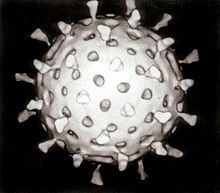
| Computer–aided reconstruction of a rotavirus based on several electron micrographs | |
| Virus classification | |
| (unranked): | Virus |
| Realm: | Riboviria |
| Kingdom: | Orthornavirae |
| Phylum: | Duplornaviricota |
| Class: | Resentoviricetes |
| Order: | Reovirales |
| Family: | Sedoreoviridae |
| Subfamily: | Sedoreovirinae |
| Genus: | Rotavirus |
| Species | |
| |
Rotaviruses are the most common cause of diarrhoeal disease among infants and young children.[1] Nearly every child in the world is infected with a rotavirus at least once by the age of five.[2] Immunity develops with each infection, so subsequent infections are less severe. Adults are rarely affected.[3] Rotavirus is a genus of double-stranded RNA viruses in the family Reoviridae. There are nine species of the genus, referred to as A, B, C, D, F, G, H, I and J. Rotavirus A is the most common species, and these rotaviruses cause more than 90% of rotavirus infections in humans.[4]
The virus is transmitted by the faecal–oral route. It infects and damages the cells that line the small intestine and causes gastroenteritis (which is often called "stomach flu" despite having no relation to influenza). Although rotavirus was discovered in 1973 by Ruth Bishop and her colleagues by electron micrograph images[5] and accounts for approximately one third of hospitalisations for severe diarrhoea in infants and children,[6] its importance has historically been underestimated within the public health community, particularly in developing countries.[7] In addition to its impact on human health, rotavirus also infects other animals, and is a pathogen of livestock.[8]
Rotaviral enteritis is usually an easily managed disease of childhood, but among children under 5 years of age rotavirus caused an estimated 151,714 deaths from diarrhoea in 2019.[9] In the United States, before initiation of the rotavirus vaccination programme in the 2000s, rotavirus caused about 2.7 million cases of severe gastroenteritis in children, almost 60,000 hospitalisations, and around 37 deaths each year.[10] Following rotavirus vaccine introduction in the United States, hospitalisation rates have fallen significantly.[11][12] Public health campaigns to combat rotavirus focus on providing oral rehydration therapy for infected children and vaccination to prevent the disease.[13] The incidence and severity of rotavirus infections has declined significantly in countries that have added rotavirus vaccine to their routine childhood immunisation policies.[14][15][16]
Virology
[edit]Types of rotavirus
[edit]There are nine species of rotavirus (sometimes informally called groups) referred to as A, B, C, D, F, G, H, I and J.[17][18] Humans are primarily infected by rotaviruses in the species Rotavirus A. A–I species cause disease in other animals,[19] species H in pigs, D, F and G in birds, I in cats and J in bats.[20][21][22][23]
Within group A rotaviruses there are different strains, called serotypes.[24] As with influenza virus, a dual classification system is used based on two proteins on the surface of the virus. The glycoprotein VP7 defines the G serotypes and the protease-sensitive protein VP4 defines P serotypes.[25] Because the two genes that determine G-types and P-types can be passed on separately to progeny viruses, different combinations are found.[25] A whole genome genotyping system has been established for group A rotaviruses, which has been used to determine the origin of atypical strains.[26] The prevalence of the individual G-types and P-types varies between, and within, countries and years.[27] There are at least 36 G types and 51 P types[28] but in infections of humans only a few combinations of G and P types predominate. They are G1P[8], G2P[4], G3P[8], G4P[8], G9P[8] and G12P[8].[29]
Structure
[edit]The genome of rotaviruses consists of 11 unique double helix molecules of RNA (dsRNA) which are 18,555 nucleotides in total. Each helix, or segment, is a gene, numbered 1 to 11 by decreasing size. Each gene codes for one protein, except genes 9, which codes for two.[30] The RNA is surrounded by a three-layered icosahedral protein capsid. Viral particles are up to 76.5 nm in diameter[31][32] and are not enveloped.[33]
Proteins
[edit]
There are six viral proteins (VPs) that form the virus particle (virion). These structural proteins are called VP1, VP2, VP3, VP4, VP6 and VP7. In addition to the VPs, there are six nonstructural proteins (NSPs), that are only produced in cells infected by rotavirus. These are called NSP1, NSP2, NSP3, NSP4, NSP5 and NSP6.[19]
At least six of the twelve proteins encoded by the rotavirus genome bind RNA.[35] The role of these proteins in rotavirus replication is not entirely understood; their functions are thought to be related to RNA synthesis and packaging in the virion, mRNA transport to the site of genome replication, and mRNA translation and regulation of gene expression.[36]
Structural proteins
[edit]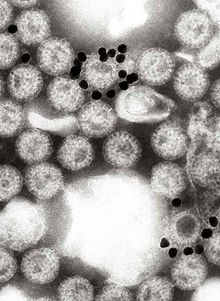
VP1 is located in the core of the virus particle and is an RNA-dependent RNA polymerase enzyme.[37] In an infected cell this enzyme produces mRNA transcripts for the synthesis of viral proteins and produces copies of the rotavirus genome RNA segments for newly produced virus particles.[38]
VP2 forms the core layer of the virion and binds the RNA genome.[39]
VP3 is part of the inner core of the virion and is an enzyme called guanylyl transferase. This is a capping enzyme that catalyses the formation of the 5' cap in the post-transcriptional modification of mRNA.[40] The cap stabilises viral mRNA by protecting it from nucleic acid degrading enzymes called nucleases.[41]
VP4 is on the surface of the virion that protrudes as a spike.[42] It binds to molecules on the surface of cells called receptors and drives the entry of the virus into the cell.[43] VP4 has to be modified by the protease enzyme trypsin, which is found in the gut, into VP5* and VP8* before the virus is infectious.[44] VP4 determines how virulent the virus is and it determines the P-type of the virus.[45] In humans there is an association between the blood group (Lewis antigen system, ABO blood group system and secretor status) and susceptibility to infection. Non-secretors seem resistant to infection by types P[4] and P[8], indicating that blood group antigens are the receptors for these genotypes.[46] This resistance is dependent on the rotavirus genotype.[47]
VP6 forms the bulk of the capsid. It is highly antigenic and can be used to identify rotavirus species.[48] This protein is used in laboratory tests for rotavirus infections.[49]
VP7 is a glycoprotein that forms the outer surface of the virion. Apart from its structural functions, it determines the G-type of the strain and, along with VP4, is involved in immunity to infection.[31]
Nonstructural viral proteins
[edit]NSP1, the product of gene 5, is a nonstructural RNA-binding protein.[50] NSP1 also blocks the interferon response, the part of the innate immune system that protects cells from viral infection. NSP1 causes the proteosome to degrade key signaling components required to stimulate production of interferon in an infected cell and to respond to interferon secreted by adjacent cells.
Targets for degradation include several IRF transcription factors required for interferon gene transcription.[51]
NSP2 is an RNA-binding protein that accumulates in cytoplasmic inclusions (viroplasms) and is required for genome replication.[52][39]
NSP3 is bound to viral mRNAs in infected cells and it is responsible for the shutdown of cellular protein synthesis.[53] NSP3 inactivates two translation initiation factors essential for synthesis of proteins from host mRNA.
First, NSP3 ejects poly(A)-binding protein (PABP) from the translation initiation factor eIF4F. PABP is required for efficient translation of transcripts with a 3' poly(A) tail, which is found on most host cell transcripts. Second, NSP3 inactivates eIF2 by stimulating its phosphorylation.[54] Efficient translation of rotavirus mRNA, which lacks the 3' poly(A) tail, does not require either of these factors.[55]
NSP4 is a viral enterotoxin that induces diarrhoea and was the first viral enterotoxin discovered.[56] It is a viroporin that elevates cytosolic Ca2+ in mammalian cells.[57]
NSP5 is encoded by genome segment 11 of rotavirus A. In virus-infected cells NSP5 accumulates in the viroplasm.[58]
NSP6 is a nucleic acid binding protein[59] and is encoded by gene 11 from an out-of-phase open reading frame.[60]
| RNA Segment (Gene) | Size (base pairs) | Protein | UniProt | Molecular weight kDa | Location | Copies per particle | Function |
|---|---|---|---|---|---|---|---|
| 1 | 3302 | VP1 | P22678 | 125 | At the vertices of the core | 12 | RNA-dependent RNA polymerase |
| 2 | 2690 | VP2 | A2T3R5 | 102 | Forms inner shell of the core | 120 | RNA binding |
| 3 | 2591 | VP3 | A2T3S5 | 88 | At the vertices of the core | 12 | methyltransferase mRNA capping enzyme |
| 4 | 2362 | VP4 | A2T3T2 | 87 | Surface spike | 180 | Cell attachment, virulence |
| 5 | 1611 | NSP1 | Q99FX5 | 59 | Nonstructural | 0 | 5'RNA binding, interferon antagonist |
| 6 | 1356 | VP6 | Q6LE89 | 45 | Inner Capsid | 780 | Structural and species-specific antigen |
| 7 | 1104 | NSP3 | P03536 | 37 | Nonstructural | 0 | Enhances viral mRNA activity and shut-offs cellular protein synthesis |
| 8 | 1059 | NSP2 | A2T3P0 | 35 | Nonstructural | 0 | NTPase involved in RNA packaging |
| 9 | 1062 | VP71 VP72 | P03533 | 38 and 34 | Surface | 780 | Structural and neutralisation antigen |
| 10 | 751 | NSP4 | P04512 | 20 | Nonstructural | 0 | Viroporin (enterotoxin) |
| 11 | 667 | NSP5 NSP6 | A2T3Q9 P11203 | 22 | Nonstructural | 0 | ssRNA and dsRNA binding modulator of NSP2, phosphoprotein |
This table is based on the simian rotavirus strain SA11. RNA-protein coding assignments differ in some strains.
Replication
[edit]
- Attachment of the virus to the host cells, which is mediated by VP4 and VP7
- Penetration of the cell by the virus and uncoating of the viral capsid
- Plus strand ssRNA synthesis (this acts as the mRNA) synthesis, which is mediated by VP1, VP3 and VP2
- Formation of the viroplasm, viral RNA packaging and minus strand RNA synthesis and formation of the double-layered virus particles
- Virus particle maturation and release of progeny virions
The attachment of the virus to the host cell is initiated by VP4, which attaches to molecules, called glycans, on the surface of the cell.[33] The virus enters cells by receptor mediated endocytosis and form a vesicle known as an endosome. Proteins in the third layer (VP7 and the VP4 spike) disrupt the membrane of the endosome, creating a difference in the calcium concentration. This causes the breakdown of VP7 trimers into single protein subunits, leaving the VP2 and VP6 protein coats around the viral dsRNA, forming a double-layered particle (DLP).[62]
The eleven dsRNA strands remain within the protection of the two protein shells and the viral RNA-dependent RNA polymerase creates mRNA transcripts of the double-stranded viral genome. By remaining in the core, the viral RNA evades innate host immune responses including RNA interference that are triggered by the presence of double-stranded RNA.[63]
During the infection, rotaviruses produce mRNA for both protein biosynthesis and gene replication. Most of the rotavirus proteins accumulate in viroplasm, where the RNA is replicated and the DLPs are assembled. In the viroplasm the positive sense viral RNAs that are used as templates for the synthesis of viral genomic dsRNA are protected from siRNA-induced RNase degradation.[64] Viroplasm is formed around the cell nucleus as early as two hours after virus infection, and consists of viral factories thought to be made by two viral nonstructural proteins: NSP5 and NSP2. Inhibition of NSP5 by RNA interference in vitro results in a sharp decrease in rotavirus replication. The DLPs migrate to the endoplasmic reticulum where they obtain their third, outer layer (formed by VP7 and VP4). The progeny viruses are released from the cell by lysis.[44][65][66]
Transmission
[edit]
Rotaviruses are transmitted by the faecal–oral route, via contact with contaminated hands, surfaces and objects,[67] and possibly by the respiratory route.[68] Viral diarrhoea is highly contagious. The faeces of an infected person can contain more than 10 trillion infectious particles per gram;[48] fewer than 100 of these are required to transmit infection to another person.[3]
Rotaviruses are stable in the environment and have been found in estuary samples at levels up to 1–5 infectious particles per US gallon. The viruses survive between 9 and 19 days.[69] Sanitary measures adequate for eliminating bacteria and parasites seem to be ineffective in control of rotavirus, as the incidence of rotavirus infection in countries with high and low health standards is similar.[68]
Signs and symptoms
[edit]Rotaviral enteritis is a mild to severe disease characterised by nausea, vomiting, watery diarrhoea and low-grade fever. Once a child is infected by the virus, there is an incubation period of about two days before symptoms appear.[70] The period of illness is acute. Symptoms often start with vomiting followed by four to eight days of profuse diarrhoea. Dehydration is more common in rotavirus infection than in most of those caused by bacterial pathogens, and is the most common cause of death related to rotavirus infection.[71]
Rotavirus infections can occur throughout life: the first usually produces symptoms, but subsequent infections are typically mild or asymptomatic,[72][48] as the immune system provides some protection.[73] Consequently, symptomatic infection rates are highest in children under two years of age and decrease progressively towards 45 years of age.[74] The most severe symptoms tend to occur in children six months to two years of age, the elderly, and those with immunodeficiency. Due to immunity acquired in childhood, most adults are not susceptible to rotavirus; gastroenteritis in adults usually has a cause other than rotavirus, but asymptomatic infections in adults may maintain the transmission of infection in the community.[75] There is some evidence to suggest blood group can impact on the susceptibility to infection by rotaviruses.[76]
Disease mechanisms
[edit]
Rotaviruses replicate mainly in the gut,[77] and infect enterocytes of the villi of the small intestine, leading to structural and functional changes of the epithelium.[78] There is evidence in humans, and particularly in animal models of extraintestinal dissemination of infectious virus to other organs and macrophages.[79]
The diarrhoea is caused by multiple activities of the virus.[80] Malabsorption occurs because of the destruction of gut cells called enterocytes. The toxic rotavirus protein NSP4 induces age- and calcium ion-dependent chloride secretion, disrupts SGLT1 (sodium/glucose cotransporter 2) transporter-mediated reabsorption of water, apparently reduces activity of brush-border membrane disaccharidases, and activates the calcium ion-dependent secretory reflexes of the enteric nervous system.[56] The elevated concentrations of calcium ions in the cytosol (which are required for the assembly of the progeny viruses) is achieved by NSP4 acting as a viroporin. This increase in calcium ions leads to autophagy (self destruction) of the infected enterocytes.[81]
NSP4 is also secreted. This extracellular form, which is modified by protease enzymes in the gut, is an enterotoxin which acts on uninfected cells via integrin receptors, which in turn cause and increase in intracellular calcium ion concentrations, secretory diarrhoea and autophagy.[82]
The vomiting, which is a characteristic of rotaviral enteritis, is caused by the virus infecting the enterochromaffin cells on the lining of the digestive tract. The infection stimulates the production of 5' hydroxytryptamine (serotonin). This activates vagal afferent nerves, which in turn activates the cells of the brain stem that control the vomiting reflex.[83]
Healthy enterocytes secrete lactase into the small intestine; milk intolerance due to lactase deficiency is a symptom of rotavirus infection,[84] which can persist for weeks.[85] A recurrence of mild diarrhoea often follows the reintroduction of milk into the child's diet, due to bacterial fermentation of the disaccharide lactose in the gut.[86]
Immune responses
[edit]Specific responses
[edit]Rotaviruses elicit both B and T cell immune responses. Antibodies to the rotavirus VP4 and VP7 proteins neutralise viral infectivity in vitro and in vivo.[87] Specific antibodies of the classes IgM, IgA and IgG are produced, which have been shown to protect against rotavirus infection by the passive transfer of the antibodies in other animals.[88] Maternal trans-placental IgG might play a role in the protection neonates from rotavirus infections, but on the other hand might reduce vaccine efficacy.[89]
Innate responses
[edit]Following infection by rotaviruses there is a rapid innate immune response involving types I and III interferons and other cytokines (particularly Th1 and Th2)[90] which inhibit the replication of the virus and recruit macrophages and natural killer cells to the rotavirus infected cells.[91] The rotavirus dsRNA activates pattern recognition receptors such toll-like receptors that stimulate the production of interferons.[92] The rotavirus protein NSP1 counteracts the effects of type 1 interferons by suppressing the activity of the interferon regulatory proteins IRF3, IRF5 and IRF7.[92]
Markers of protection
[edit]The levels of IgG and IgA in the blood and IgA in the gut correlate with protection from infection.[93] Rotavirus specific serum IgG and IgA at high titres (e.g. >1:200) have been claimed to be protective and there is a significant correlation between IgA titres and rotavirus vaccine efficacy.[94]
Diagnosis and detection
[edit]Diagnosis of infection with a rotavirus normally follows diagnosis of gastroenteritis as the cause of severe diarrhoea. Most children admitted to hospital with gastroenteritis are tested for rotavirus.[95][96]
Specific diagnosis of infection with rotavirus is made by finding the virus in the child's stool by enzyme immunoassay. There are several licensed test kits on the market which are sensitive, specific and detect all serotypes of rotavirus.[97] Other methods, such as electron microscopy and PCR (polymerase chain reaction), are used in research laboratories.[98] Reverse transcription-polymerase chain reaction (RT-PCR) can detect and identify all species and serotypes of human rotaviruses.[99]
Treatment and prognosis
[edit]Treatment of acute rotavirus infection is nonspecific and involves management of symptoms and, most importantly, management of dehydration.[13] If untreated, children can die from the resulting severe dehydration.[100] Depending on the severity of diarrhoea, treatment consists of oral rehydration therapy, during which the child is given extra water to drink that contains specific amounts of salt and sugar.[101] In 2004, the World Health Organisation (WHO) and UNICEF recommended the use of low-osmolarity oral rehydration solution and zinc supplementation as a two-pronged treatment of acute diarrhoea.[102] Some infections are serious enough to warrant hospitalisation where fluids are given by intravenous therapy or nasogastric intubation, and the child's electrolytes and blood sugar are monitored.[95] Rotavirus infections rarely cause other complications and for a well managed child the prognosis is excellent.[103] Probiotics have been shown to reduce the duration of rotavirus diarrhoea,[104] and according to the European Society for Pediatric Gastroenterology "effective interventions include administration of specific probiotics such as Lactobacillus rhamnosus or Saccharomyces boulardii, diosmectite or racecadotril."[105]
Prevention
[edit]Rotaviruses are highly contagious and cannot be treated with antibiotics or other drugs. Because improved sanitation does not decrease the prevalence of rotaviral disease, and the rate of hospitalisations remains high despite the use of oral rehydrating medicines, the primary public health intervention is vaccination.[2] In 1998, a rotavirus vaccine was licensed for use in the United States. Clinical trials in the United States, Finland, and Venezuela had found it to be 80–100% effective at preventing severe diarrhoea caused by rotavirus A, and researchers had detected no statistically significant serious adverse effects.[106][107] The manufacturer, however, withdrew it from the market in 1999, after it was discovered that the vaccine may have contributed to an increased risk for intussusception, a type of bowel obstruction, in one of every 12,000 vaccinated infants.[108] The experience provoked intense debate about the relative risks and benefits of a rotavirus vaccine.[109]
In 2006, two new vaccines against rotavirus A infection were shown to be safe and effective in children,[110] and in 2009, the WHO recommended that rotavirus vaccine be included in all national immunisation programmes.[111]
The incidence and severity of rotavirus infections has declined significantly in countries that have acted on this recommendation.[14][15][16] A 2014 review of available clinical trial data from countries routinely using rotavirus vaccines in their national immunisation programs found that rotavirus vaccines have reduced rotavirus hospitalisations by 49–92% and all cause diarrhoea hospitalisations by 17–55%.[112] In Mexico, which in 2006 was among the first countries in the world to introduce rotavirus vaccine, diarrhoeal disease death rates dropped during the 2009 rotavirus season by more than 65 percent among children age two and under.[113] In Nicaragua, which in 2006 became the first developing country to introduce a rotavirus vaccine, severe rotavirus infections were reduced by 40 percent and emergency room visits by a half.[114] In the United States, rotavirus vaccination since 2006 has led to drops in rotavirus-related hospitalisations by as much as 86 percent.[115] The vaccines may also have prevented illness in non-vaccinated children by limiting the number of circulating infections.[115][116] In developing countries in Africa and Asia, where the majority of rotavirus deaths occur, a large number of safety and efficacy trials as well as recent post-introduction impact and effectiveness studies of Rotarix and RotaTeq have found that vaccines dramatically reduced severe disease among infants.[16][117][118][119] In September 2013, the vaccine was offered to all children in the UK, aged between two and three months, and it is expected to halve the cases of severe infection and reduce the number of children admitted to hospital because of the infection by 70 percent.[120] In Europe, hospitalisation rates following infection by rotaviruses have decreased by 65% to 84% following the introduction of the vaccine.[121] Globally, vaccination has reduced hospital admissions and emergency department visits by a median of 67%.[122]
Rotavirus vaccines are licensed in over 100 countries, and more than 80 countries have introduced routine rotavirus vaccination, almost half with the support of the GAVI vaccine alliance.[123] To make rotavirus vaccines available, accessible, and affordable in all countries—particularly low- and middle-income countries in Africa and Asia where the majority of rotavirus deaths occur, PATH (formerly Program for Appropriate Technology in Health), the WHO, the U.S. Centers for Disease Control and Prevention, and GAVI have partnered with research institutions and governments to generate and disseminate evidence, lower prices, and accelerate introduction.[124]
The vaccine may prevent type 1 diabetes.[125][126]
Epidemiology
[edit]Rotavirus A, which accounts for more than 90% of rotavirus gastroenteritis in humans,[4] is endemic worldwide. Each year rotaviruses cause millions of cases of diarrhoea in developing countries, almost 2 million of which result in hospitalisation.[7] In 2019, an estimated 151,714 children younger than five died from rotavirus infections, 90 percent of whom were in developing countries.[9] Almost every child has been infected with rotaviruses by age five.[2][127] Rotaviruses are the leading single cause of severe diarrhoea among infants and children, are responsible for about a third of the cases requiring hospitalisation,[11] and cause 37% of deaths attributable to diarrhoea and 5% of all deaths in children younger than five.[128] Boys are twice as likely as girls to be admitted to hospital for rotavirus infections.[129][130] In the pre-vaccination era, rotavirus infections occurred primarily during cool, dry seasons.[131][132] The number attributable to food contamination is unknown.[133]
Outbreaks of rotavirus A diarrhoea are common among hospitalised infants, young children attending day care centres, and elderly people in nursing homes.[75][134] An outbreak caused by contaminated municipal water occurred in Colorado in 1981.[135] During 2005, the largest recorded epidemic of diarrhoea occurred in Nicaragua. This unusually large and severe outbreak was associated with mutations in the rotavirus A genome, possibly helping the virus escape the prevalent immunity in the population.[136] A similar large outbreak occurred in Brazil in 1977.[137]
Rotavirus B, also called adult diarrhoea rotavirus or ADRV, has caused major epidemics of severe diarrhoea affecting thousands of people of all ages in China. These epidemics occurred as a result of sewage contamination of drinking water.[138][139] Rotavirus B infections also occurred in India in 1998; the causative strain was named CAL. Unlike ADRV, the CAL strain is endemic.[140][141] To date, epidemics caused by rotavirus B have been confined to mainland China, and surveys indicate a lack of immunity to this species in the United States.[142] Rotavirus C has been associated with rare and sporadic cases of diarrhoea in children, and small outbreaks have occurred in families.[143]
-
The seasonal variation of rotavirus A infections in England: rates of infection peak during the winter months.[144]
-
Preventable child deaths from rotavirus vaccination, 2016. Annual number of preventable deaths in children under five years old from rotavirus if full coverage of the rotavirus vaccine was achieved.[145]
Other animals
[edit]Rotaviruses infect the young of many species of animals and they are a major cause of diarrhoea in wild and reared animals worldwide.[8] As a pathogen of livestock, notably in young calves and piglets, rotaviruses cause economic loss to farmers because of costs of treatment associated with high morbidity and mortality rates.[146] These rotaviruses are a potential reservoir for genetic exchange with human rotaviruses.[146] There is evidence that animal rotaviruses can infect humans, either by direct transmission of the virus or by contributing one or several RNA segments to reassortants with human strains.[147][148][149]
History
[edit]
In 1943, Jacob Light and Horace Hodes proved that a filterable agent in the faeces of children with infectious diarrhoea also caused scours (livestock diarrhoea) in cattle.[150] Three decades later, preserved samples of the agent were shown to be rotavirus.[151] In the intervening years, a virus in mice[152] was shown to be related to the virus causing scours.[153] In 1973, Ruth Bishop and colleagues described related viruses found in children with gastroenteritis.[5]
In 1974, Thomas Henry Flewett suggested the name rotavirus after observing that, when viewed through an electron microscope, a rotavirus particle looks like a wheel (rota in Latin)[154][155] the name was officially recognised by the International Committee on Taxonomy of Viruses four years later.[156] In 1976, related viruses were described in several other species of animals.[153] These viruses, all causing acute gastroenteritis, were recognised as a collective pathogen affecting humans and other animals worldwide.[154] Rotavirus serotypes were first described in 1980,[157] and in the following year, rotaviruses from humans were first grown in cell cultures derived from monkey kidneys, by adding trypsin (an enzyme found in the duodenum of mammals and now known to be essential for rotavirus to replicate) to the culture medium.[158] The ability to grow rotaviruses in culture accelerated the pace of research, and by the mid-1980s the first candidate vaccines were being evaluated.[159]
References
[edit]- ^ Dennehy PH (September 2015). "Rotavirus Infection: A Disease of the Past?". Infectious Disease Clinics of North America. 29 (4): 617–635. doi:10.1016/j.idc.2015.07.002. PMID 26337738.
- ^ a b c Bernstein DI (2009). "Rotavirus overview". The Pediatric Infectious Disease Journal. 28 (Suppl 3): S50–S53. doi:10.1097/INF.0b013e3181967bee. PMID 19252423. S2CID 30544613.
- ^ a b Grimwood K, Lambert SB (2009). "Rotavirus vaccines: opportunities and challenges". Human Vaccines. 5 (2): 57–69. doi:10.4161/hv.5.2.6924. PMID 18838873. S2CID 31164630.
- ^ a b Leung AK, Kellner JD, Davies HD (2005). "Rotavirus gastroenteritis". Advances in Therapy. 22 (5): 476–487. doi:10.1007/BF02849868. PMID 16418157. S2CID 39847059.
- ^ a b Bishop R (2009). "Discovery of rotavirus: Implications for child health". Journal of Gastroenterology and Hepatology. 24 (Suppl 3): S81–S85. doi:10.1111/j.1440-1746.2009.06076.x. PMID 19799704.
- ^ Hallowell BD, Chavers T, Parashar U, Tate JE (April 2022). "Global Estimates of Rotavirus Hospitalizations Among Children Below 5 Years in 2019 and Current and Projected Impacts of Rotavirus Vaccination". Journal of the Pediatric Infectious Diseases Society. 11 (4): 149–158. doi:10.1093/jpids/piab114. PMID 34904636.
- ^ a b Simpson E, Wittet S, Bonilla J, Gamazina K, Cooley L, Winkler JL (2007). "Use of formative research in developing a knowledge translation approach to rotavirus vaccine introduction in developing countries". BMC Public Health. 7: 281. doi:10.1186/1471-2458-7-281. PMC 2173895. PMID 17919334. S2CID 424503.
- ^ a b Dubovi EJ, MacLachlan NJ (2010). Fenner's Veterinary Virology (4th ed.). Boston: Academic Press. p. 288. ISBN 978-0-12-375158-4.
- ^ a b Janko MM, Joffe J, Michael D, Earl L, Rosettie KL, Sparks GW, Albertson SB, Compton K, Pedroza Velandia P, Stafford L, Zheng P, Aravkin A, Kyu HH, Murray CJ, Weaver MR (June 2022). "Cost-effectiveness of rotavirus vaccination in children under five years of age in 195 countries: A meta-regression analysis". Vaccine. 40 (28): 3903–3917. doi:10.1016/j.vaccine.2022.05.042. PMC 9208428. PMID 35643565. S2CID 249072461.
- ^ Fischer TK, Viboud C, Parashar U, Malek M, Steiner C, Glass R, Simonsen L (April 2007). "Hospitalizations and deaths from diarrhea and rotavirus among children <5 years of age in the United States, 1993–2003". The Journal of Infectious Diseases. 195 (8): 1117–1125. doi:10.1086/512863. PMID 17357047.
- ^ a b Leshem E, Moritz RE, Curns AT, Zhou F, Tate JE, Lopman BA, Parashar UD (July 2014). "Rotavirus vaccines and health care utilization for diarrhea in the United States (2007–2011)". Pediatrics. 134 (1): 15–23. doi:10.1542/peds.2013-3849. PMC 7975848. PMID 24913793.
- ^ Tate JE, Cortese MM, Payne DC, Curns AT, Yen C, Esposito DH, et al. (January 2011). "Uptake, impact, and effectiveness of rotavirus vaccination in the United States: review of the first 3 years of postlicensure data". The Pediatric Infectious Disease Journal. 30 (1 Suppl): S56–60. doi:10.1097/INF.0b013e3181fefdc0. PMID 21183842. S2CID 20940659.
- ^ a b Diggle L (2007). "Rotavirus diarrhea and future prospects for prevention". British Journal of Nursing. 16 (16): 970–974. doi:10.12968/bjon.2007.16.16.27074. PMID 18026034.
- ^ a b Giaquinto C, Dominiak-Felden G, Van Damme P, Myint TT, Maldonado YA, Spoulou V, Mast TC, Staat MA (2011). "Summary of effectiveness and impact of rotavirus vaccination with the oral pentavalent rotavirus vaccine: a systematic review of the experience in industrialized countries". Human Vaccines. 7 (7): 734–748. doi:10.4161/hv.7.7.15511. PMID 21734466. S2CID 23996836.
- ^ a b Jiang V, Jiang B, Tate J, Parashar UD, Patel MM (July 2010). "Performance of rotavirus vaccines in developed and developing countries". Human Vaccines. 6 (7): 532–42. doi:10.4161/hv.6.7.11278. PMC 3322519. PMID 20622508.
- ^ a b c Parashar UD, Johnson H, Steele AD, Tate JE (May 2016). Parashar UD, Tate JE (eds.). "Health Impact of Rotavirus Vaccination in Developing Countries: Progress and Way Forward". Clinical Infectious Diseases. 62 (Suppl 2): S91–95. doi:10.1093/cid/civ1015. PMID 27059361.
- ^ "Virus Taxonomy: 2021 Release". International Committee on Taxonomy of Viruses (ICTV). Retrieved 19 May 2022.
- ^ Suzuki H (August 2019). "Rotavirus Replication: Gaps of Knowledge on Virus Entry and Morphogenesis". The Tohoku Journal of Experimental Medicine. 248 (4): 285–296. doi:10.1620/tjem.248.285. PMID 31447474.
- ^ a b Kirkwood CD (September 2010). "Genetic and antigenic diversity of human rotaviruses: potential impact on vaccination programs". The Journal of Infectious Diseases. 202 (Suppl 1): S43–48. doi:10.1086/653548. PMID 20684716.
- ^ Wakuda M, Ide T, Sasaki J, Komoto S, Ishii J, Sanekata T, Taniguchi K (August 2011). "Porcine rotavirus closely related to novel group of human rotaviruses". Emerging Infectious Diseases. 17 (8): 1491–1493. doi:10.3201/eid1708.101466. PMC 3381553. PMID 21801631.
- ^ Marthaler D, Rossow K, Culhane M, Goyal S, Collins J, Matthijnssens J, Nelson M, Ciarlet M (July 2014). "Widespread rotavirus H in commercially raised pigs, United States". Emerging Infectious Diseases. 20 (7): 1195–1198. doi:10.3201/eid2007.140034. PMC 4073875. PMID 24960190.
- ^ Phan TG, Leutenegger CM, Chan R, Delwart E (June 2017). "Rotavirus I in feces of a cat with diarrhea". Virus Genes. 53 (3): 487–490. doi:10.1007/s11262-017-1440-4. PMC 7089198. PMID 28255929.
- ^ Bányai K, Kemenesi G, Budinski I, Földes F, Zana B, Marton S, Varga-Kugler R, Oldal M, Kurucz K, Jakab F (March 2017). "Candidate new rotavirus species in Schreiber's bats, Serbia". Infection, Genetics and Evolution. 48: 19–26. doi:10.1016/j.meegid.2016.12.002. PMC 7106153. PMID 27932285.
- ^ O'Ryan M (March 2009). "The ever-changing landscape of rotavirus serotypes". The Pediatric Infectious Disease Journal. 28 (3 Suppl): S60–62. doi:10.1097/INF.0b013e3181967c29. PMID 19252426. S2CID 22421988.
- ^ a b Patton JT (January 2012). "Rotavirus diversity and evolution in the post-vaccine world". Discovery Medicine. 13 (68): 85–97. PMC 3738915. PMID 22284787.
- ^ Phan MV, Anh PH, Cuong NV, Munnink BB, van der Hoek L, My PT, Tri TN, Bryant JE, Baker S, Thwaites G, Woolhouse M, Kellam P, Rabaa MA, Cotten M (July 2016). "Unbiased whole-genome deep sequencing of human and porcine stool samples reveals circulation of multiple groups of rotaviruses and a putative zoonotic infection". Virus Evolution. 2 (2): vew027. doi:10.1093/ve/vew027. PMC 5522372. PMID 28748110.
- ^ Beards GM, Desselberger U, Flewett TH (December 1989). "Temporal and geographical distributions of human rotavirus serotypes, 1983 to 1988". Journal of Clinical Microbiology. 27 (12): 2827–2833. doi:10.1128/JCM.27.12.2827-2833.1989. PMC 267135. PMID 2556435.
- ^ Rakau KG, Nyaga MM, Gededzha MP, Mwenda JM, Mphahlele MJ, Seheri LM, Steele AD (January 2021). "Genetic characterization of G12P[6] and G12P[8] rotavirus strains collected in six African countries between 2010 and 2014". BMC Infectious Diseases. 21 (1): 107. doi:10.1186/s12879-020-05745-6. PMC 7821174. PMID 33482744.
- ^ Antoni S, Nakamura T, Cohen AL, Mwenda JM, Weldegebriel G, Biey JN, Shaba K, Rey-Benito G, de Oliveira LH, Oliveira MT, Ortiz C, Ghoniem A, Fahmy K, Ashmony HA, Videbaek D, Daniels D, Pastore R, Singh S, Tondo E, Liyanage JB, Sharifuzzaman M, Grabovac V, Batmunkh N, Logronio J, Armah G, Dennis FE, Seheri M, Magagula N, Mphahlele J, Leite JP, Araujo IT, Fumian TM, El Mohammady H, Semeiko G, Samoilovich E, Giri S, Kang G, Thomas S, Bines J, Kirkwood CD, Liu N, Lee DY, Iturriza-Gomara M, Page NA, Esona MD, Ward ML, Wright CN, Mijatovic-Rustempasic S, Tate JE, Parashar UD, Gentsch J, Bowen MD, Serhan F (2023). "Rotavirus genotypes in children under five years hospitalized with diarrhea in low and middle-income countries: Results from the WHO-coordinated Global Rotavirus Surveillance Network". PLOS Global Public Health. 3 (11): e0001358. doi:10.1371/journal.pgph.0001358. PMC 10683987. PMID 38015834.
- ^ Estes MK, Cohen J (1989). "Rotavirus gene structure and function". Microbiological Reviews. 53 (4): 410–449. doi:10.1128/MMBR.53.4.410-449.1989. PMC 372748. PMID 2556635.
- ^ a b Pesavento JB, Crawford SE, Estes MK, Prasad BV (2006). "Rotavirus proteins: structure and assembly". In Roy P (ed.). Reoviruses: Entry, Assembly and Morphogenesis. Current Topics in Microbiology and Immunology. Vol. 309. New York: Springer. pp. 189–219. doi:10.1007/3-540-30773-7_7. ISBN 978-3-540-30772-3. PMID 16913048. S2CID 11290382.
- ^ Prasad BV, Chiu W (1994). "Structure of Rotavirus". In Ramig RF (ed.). Rotaviruses. Current Topics in Microbiology and Immunology. Vol. 185. New York: Springer. pp. 9–29. doi:10.1007/978-3-642-78256-5_2 (inactive 22 March 2024). ISBN 978-3-540-56761-5. PMID 8050286.
((cite book)): CS1 maint: DOI inactive as of March 2024 (link) - ^ a b Rodríguez JM, Luque D (2019). "Structural Insights into Rotavirus Entry". Physical Virology. Advances in Experimental Medicine and Biology. Vol. 1215. pp. 45–68. doi:10.1007/978-3-030-14741-9_3. hdl:20.500.12105/10344. ISBN 978-3-030-14740-2. PMID 31317495. S2CID 197541267.
- ^ Gray J, Desselberger U (2000). Rotaviruses : methods and protocols. Totowa, N.J.: Humana Press. p. 15. ISBN 978-1-59259-078-0. OCLC 55684328.
- ^ Patton JT (1995). "Structure and function of the rotavirus RNA-binding proteins". The Journal of General Virology. 76 (11): 2633–2644. doi:10.1099/0022-1317-76-11-2633. PMID 7595370.
- ^ Patton JT (2001). "Rotavirus RNA Replication and Gene Expression". Gastroenteritis Viruses. Novartis Foundation Symposia. Vol. 238. pp. 64–77, discussion 77–81. doi:10.1002/0470846534.ch5. ISBN 978-0-470-84653-7. PMID 11444036.
- ^ Vásquez-del Carpió R, Morales JL, Barro M, Ricardo A, Spencer E (2006). "Bioinformatic prediction of polymerase elements in the rotavirus VP1 protein". Biological Research. 39 (4): 649–659. doi:10.4067/S0716-97602006000500008. PMID 17657346.
- ^ Trask SD, Ogden KM, Patton JT (2012). "Interactions among capsid proteins orchestrate rotavirus particle functions". Current Opinion in Virology. 2 (4): 373–379. doi:10.1016/j.coviro.2012.04.005. PMC 3422376. PMID 22595300.
- ^ a b Taraporewala ZF, Patton JT (2004). "Nonstructural proteins involved in genome packaging and replication of rotaviruses and other members of the Reoviridae". Virus Research. 101 (1): 57–66. doi:10.1016/j.virusres.2003.12.006. PMID 15010217.
- ^ Angel J, Franco MA, Greenberg HB (2009). Mahy BW, Van Regenmortel MH (eds.). Desk Encyclopedia of Human and Medical Virology. Boston: Academic Press. p. 277. ISBN 978-0-12-375147-8.
- ^ Cowling VH (2009). "Regulation of mRNA cap methylation". The Biochemical Journal. 425 (2): 295–302. doi:10.1042/BJ20091352. PMC 2825737. PMID 20025612.
- ^ Gardet A, Breton M, Fontanges P, Trugnan G, Chwetzoff S (2006). "Rotavirus spike protein VP4 binds to and remodels actin bundles of the epithelial brush border into actin bodies". Journal of Virology. 80 (8): 3947–3456. doi:10.1128/JVI.80.8.3947-3956.2006. PMC 1440440. PMID 16571811.
- ^ Arias CF, Isa P, Guerrero CA, Méndez E, Zárate S, López T, Espinosa R, Romero P, López S (2002). "Molecular biology of rotavirus cell entry". Archives of Medical Research. 33 (4): 356–361. doi:10.1016/S0188-4409(02)00374-0. PMID 12234525.
- ^ a b Jayaram H, Estes MK, Prasad BV (2004). "Emerging themes in rotavirus cell entry, genome organization, transcription and replication". Virus Research. 101 (1): 67–81. doi:10.1016/j.virusres.2003.12.007. PMID 15010218.
- ^ Hoshino Y, Jones RW, Kapikian AZ (2002). "Characterization of neutralization specificities of outer capsid spike protein VP4 of selected murine, lapine, and human rotavirus strains". Virology. 299 (1): 64–71. doi:10.1006/viro.2002.1474. PMID 12167342.
- ^ Van Trang N, Vu HT, Le NT, Huang P, Jiang X, Anh DD (2014). "Association between norovirus and rotavirus infection and histo-blood group antigen types in Vietnamese children". Journal of Clinical Microbiology. 52 (5): 1366–1374. doi:10.1128/JCM.02927-13. PMC 3993640. PMID 24523471.
- ^ Sharma S, Hagbom M, Svensson L, Nordgren J (March 2020). "The Impact of Human Genetic Polymorphisms on Rotavirus Susceptibility, Epidemiology, and Vaccine Take". Viruses. 12 (3): 324. doi:10.3390/v12030324. PMC 7150750. PMID 32192193.
- ^ a b c Bishop RF (1996). "Natural history of human rotavirus infection". Archives of Virology. Supplementum. 12: 119–28. doi:10.1007/978-3-7091-6553-9_14. ISBN 978-3-211-82875-5. PMID 9015109.
- ^ Beards GM, Campbell AD, Cottrell NR, Peiris JS, Rees N, Sanders RC, Shirley JA, Wood HC, Flewett TH (1984). "Enzyme-linked immunosorbent assays based on polyclonal and monoclonal antibodies for rotavirus detection" (PDF). Journal of Clinical Microbiology. 19 (2): 248–54. doi:10.1128/JCM.19.2.248-254.1984. PMC 271031. PMID 6321549.
- ^ Hua J, Mansell EA, Patton JT (1993). "Comparative analysis of the rotavirus NS53 gene: conservation of basic and cysteine-rich regions in the protein and possible stem-loop structures in the RNA". Virology. 196 (1): 372–378. doi:10.1006/viro.1993.1492. PMID 8395125.
- ^ Arnold MM (2016). "The Rotavirus Interferon Antagonist NSP1: Many Targets, Many Questions". Journal of Virology. 90 (11): 5212–5215. doi:10.1128/JVI.03068-15. PMC 4934742. PMID 27009959.
- ^ Kattoura MD, Chen X, Patton JT (1994). "The rotavirus RNA-binding protein NS35 (NSP2) forms 10S multimers and interacts with the viral RNA polymerase". Virology. 202 (2): 803–13. doi:10.1006/viro.1994.1402. PMID 8030243.
- ^ Poncet D, Aponte C, Cohen J (1993). "Rotavirus protein NSP3 (NS34) is bound to the 3' end consensus sequence of viral mRNAs in infected cells" (PDF). Journal of Virology. 67 (6): 3159–3165. doi:10.1128/JVI.67.6.3159-3165.1993. PMC 237654. PMID 8388495.
- ^ Gratia M, Vende P, Charpilienne A, Baron HC, Laroche C, Sarot E, Pyronnet S, Duarte M, Poncet D (2016). "Challenging the Roles of NSP3 and Untranslated Regions in Rotavirus mRNA Translation". PLOS ONE. 11 (1): e0145998. Bibcode:2016PLoSO..1145998G. doi:10.1371/journal.pone.0145998. PMC 4699793. PMID 26727111.
- ^ López S, Arias CF (2012). "Rotavirus-host cell interactions: an arms race". Current Opinion in Virology. 2 (4): 389–398. doi:10.1016/j.coviro.2012.05.001. PMID 22658208.
- ^ a b Hyser JM, Estes MK (2009). "Rotavirus vaccines and pathogenesis: 2008". Current Opinion in Gastroenterology. 25 (1): 36–43. doi:10.1097/MOG.0b013e328317c897. PMC 2673536. PMID 19114772.
- ^ Pham T, Perry JL, Dosey TL, Delcour AH, Hyser JM (March 2017). "The Rotavirus NSP4 Viroporin Domain is a Calcium-conducting Ion Channel". Scientific Reports. 7: 43487. Bibcode:2017NatSR...743487P. doi:10.1038/srep43487. PMC 5335360. PMID 28256607.
- ^ Afrikanova I, Miozzo MC, Giambiagi S, Burrone O (1996). "Phosphorylation generates different forms of rotavirus NSP5". Journal of General Virology. 77 (9): 2059–2065. doi:10.1099/0022-1317-77-9-2059. PMID 8811003.
- ^ Rainsford EW, McCrae MA (2007). "Characterization of the NSP6 protein product of rotavirus gene 11". Virus Research. 130 (1–2): 193–201. doi:10.1016/j.virusres.2007.06.011. PMID 17658646.
- ^ Mohan KV, Atreya CD (2001). "Nucleotide sequence analysis of rotavirus gene 11 from two tissue culture-adapted ATCC strains, RRV and Wa". Virus Genes. 23 (3): 321–329. doi:10.1023/A:1012577407824. PMID 11778700. S2CID 21538632.
- ^ Gray J, Desselberger U (2000). Rotaviruses : methods and protocols. Totowa, N.J.: Humana Press. p. 5. ISBN 978-1-59259-078-0. OCLC 55684328.
- ^ Baker M, Prasad BV (2010). "Rotavirus cell entry". In Johnson J (ed.). Cell Entry by Non-Enveloped Viruses. Current Topics in Microbiology and Immunology. Vol. 343. pp. 121–148. doi:10.1007/82_2010_34. ISBN 978-3-642-13331-2. PMID 20397068.
- ^ Arnold MM (2016). "The Rotavirus Interferon Antagonist NSP1: Many Targets, Many Questions". Journal of Virology. 90 (11): 5212–5215. doi:10.1128/JVI.03068-15. PMC 4934742. PMID 27009959.
- ^ Silvestri LS, Taraporewala ZF, Patton JT (2004). "Rotavirus replication: plus-sense templates for double-stranded RNA synthesis are made in viroplasms". Journal of Virology. 78 (14): 7763–7774. doi:10.1128/JVI.78.14.7763-7774.2004. PMC 434085. PMID 15220450.
- ^ Patton JT, Vasquez-Del Carpio R, Spencer E (2004). "Replication and transcription of the rotavirus genome". Current Pharmaceutical Design. 10 (30): 3769–3777. doi:10.2174/1381612043382620. PMID 15579070.
- ^ Ruiz MC, Leon T, Diaz Y, Michelangeli F (2009). "Molecular biology of rotavirus entry and replication". The Scientific World Journal. 9: 1476–1497. doi:10.1100/tsw.2009.158. PMC 5823125. PMID 20024520.
- ^ Butz AM, Fosarelli P, Dick J, Cusack T, Yolken R (1993). "Prevalence of rotavirus on high-risk fomites in day-care facilities". Pediatrics. 92 (2): 202–205. doi:10.1542/peds.92.2.202. PMID 8393172. S2CID 20327842.
- ^ a b Dennehy PH (2000). "Transmission of rotavirus and other enteric pathogens in the home". Pediatric Infectious Disease Journal. 19 (Suppl 10): S103–105. doi:10.1097/00006454-200010001-00003. PMID 11052397. S2CID 28625697.
- ^ Rao VC, Seidel KM, Goyal SM, Metcalf TG, Melnick JL (1984). "Isolation of enteroviruses from water, suspended solids, and sediments from Galveston Bay: survival of poliovirus and rotavirus adsorbed to sediments" (PDF). Applied and Environmental Microbiology. 48 (2): 404–409. Bibcode:1984ApEnM..48..404R. doi:10.1128/AEM.48.2.404-409.1984. PMC 241526. PMID 6091548.
- ^ Hochwald C, Kivela L (1999). "Rotavirus vaccine, live, oral, tetravalent (RotaShield)". Pediatric Nursing. 25 (2): 203–204, 207. PMID 10532018.
- ^ Maldonado YA, Yolken RH (1990). "Rotavirus". Baillière's Clinical Gastroenterology. 4 (3): 609–625. doi:10.1016/0950-3528(90)90052-I. PMID 1962726.
- ^ Glass RI, Parashar UD, Bresee JS, Turcios R, Fischer TK, Widdowson MA, Jiang B, Gentsch JR (2006). "Rotavirus vaccines: current prospects and future challenges". The Lancet. 368 (9532): 323–332. doi:10.1016/S0140-6736(06)68815-6. PMID 16860702. S2CID 34569166.
- ^ Offit PA (2001). Gastroenteritis viruses. New York: Wiley. pp. 106–124. ISBN 978-0-471-49663-2.
- ^ Ramsay M, Brown D (2000). "Epidemiology of Group A Rotaviruses: Surveillance and Burden of Disease Studies". In Desselberger U, Gray J (eds.). Rotaviruses: Methods and Protocols. Methods in Molecular Medicine. Vol. 34. Totowa, NJ: Humana Press. pp. 217–238. doi:10.1385/1-59259-078-0:217. ISBN 978-0-89603-736-6. PMID 21318862.
- ^ a b Anderson EJ, Weber SG (2004). "Rotavirus infection in adults". The Lancet Infectious Diseases. 4 (2): 91–99. doi:10.1016/S1473-3099(04)00928-4. PMC 7106507. PMID 14871633.
- ^ Elhabyan A, Elyaacoub S, Sanad E, Abukhadra A, Elhabyan A, Dinu V (November 2020). "The role of host genetics in susceptibility to severe viral infections in humans and insights into host genetics of severe COVID-19: A systematic review". Virus Research. 289: 198163. doi:10.1016/j.virusres.2020.198163. PMC 7480444. PMID 32918943.
- ^ Greenberg HB, Estes MK (2009). "Rotaviruses: from pathogenesis to vaccination". Gastroenterology. 136 (6): 1939–1951. doi:10.1053/j.gastro.2009.02.076. PMC 3690811. PMID 19457420.
- ^ Greenberg HB, Clark HF, Offit PA (1994). "Rotavirus Pathology and Pathophysiology". In Ramig RF (ed.). Rotaviruses. Current Topics in Microbiology and Immunology. Vol. 185. New York: Springer. pp. 255–283. doi:10.1007/978-3-642-78256-5_9 (inactive 22 March 2024). ISBN 978-3-540-56761-5. PMID 8050281.
((cite book)): CS1 maint: DOI inactive as of March 2024 (link) - ^ Crawford SE, Patel DG, Cheng E, Berkova Z, Hyser JM, Ciarlet M, Finegold MJ, Conner ME, Estes MK (2006). "Rotavirus viremia and extraintestinal viral infection in the neonatal rat model". Journal of Virology. 80 (10): 4820–4832. doi:10.1128/JVI.80.10.4820-4832.2006. PMC 1472071. PMID 16641274.
- ^ Ramig RF (2004). "Pathogenesis of intestinal and systemic rotavirus infection". Journal of Virology. 78 (19): 10213–10220. doi:10.1128/JVI.78.19.10213-10220.2004. PMC 516399. PMID 15367586.
- ^ Hyser JM, Collinson-Pautz MR, Utama B, Estes MK (2010). "Rotavirus disrupts calcium homeostasis by NSP4 viroporin activity". mBio. 1 (5). doi:10.1128/mBio.00265-10. PMC 2999940. PMID 21151776.
- ^ Berkova Z, Crawford SE, Trugnan G, Yoshimori T, Morris AP, Estes MK (2006). "Rotavirus NSP4 induces a novel vesicular compartment regulated by calcium and associated with viroplasms". Journal of Virology. 80 (12): 6061–6071. doi:10.1128/JVI.02167-05. PMC 1472611. PMID 16731945.
- ^ Hagbom M, Sharma S, Lundgren O, Svensson L (2012). "Towards a human rotavirus disease model". Current Opinion in Virology. 2 (4): 408–418. doi:10.1016/j.coviro.2012.05.006. PMID 22722079.
- ^ Farnworth ER (2008). "The evidence to support health claims for probiotics". The Journal of Nutrition. 138 (6): 1250S–1254S. doi:10.1093/jn/138.6.1250S. PMID 18492865.
- ^ Ouwehand A, Vesterlund S (2003). "Health aspects of probiotics". IDrugs: The Investigational Drugs Journal. 6 (6): 573–580. PMID 12811680.
- ^ Arya SC (1984). "Rotaviral infection and intestinal lactase level". Journal of Infectious Diseases. 150 (5): 791. doi:10.1093/infdis/150.5.791. PMID 6436397.
- ^ Ward R (2009). "Mechanisms of protection against rotavirus infection and disease". The Pediatric Infectious Disease Journal. 28 (Suppl 3): S57–S59. doi:10.1097/INF.0b013e3181967c16. PMID 19252425.
- ^ Vega CG, Bok M, Vlasova AN, Chattha KS, Fernández FM, Wigdorovitz A, Parreño VG, Saif LJ (2012). "IgY antibodies protect against human Rotavirus induced diarrhea in the neonatal gnotobiotic piglet disease model". PLOS ONE. 7 (8): e42788. Bibcode:2012PLoSO...742788V. doi:10.1371/journal.pone.0042788. PMC 3411843. PMID 22880110.
- ^ Mwila K, Chilengi R, Simuyandi M, Permar SR, Becker-Dreps S (2017). "Contribution of Maternal Immunity to Decreased Rotavirus Vaccine Performance in Low- and Middle-Income Countries". Clinical and Vaccine Immunology. 24 (1). doi:10.1128/CVI.00405-16. PMC 5216432. PMID 27847365.
- ^ Gandhi GR, Santos VS, Denadai M, da Silva Calisto VK, de Souza Siqueira Quintans J, de Oliveira e Silva AM, de Souza Araújo AA, Narain N, Cuevas LE, Júnior LJ, Gurgel RQ (2017). "Cytokines in the management of rotavirus infection: A systematic review of in vivo studies". Cytokine. 96: 152–160. doi:10.1016/j.cyto.2017.04.013. PMID 28414969. S2CID 3568330.
- ^ Holloway G, Coulson BS (2013). "Innate cellular responses to rotavirus infection". The Journal of General Virology. 94 (6): 1151–1160. doi:10.1099/vir.0.051276-0. PMID 23486667.
- ^ a b Villena J, Vizoso-Pinto MG, Kitazawa H (2016). "Intestinal Innate Antiviral Immunity and Immunobiotics: Beneficial Effects against Rotavirus Infection". Frontiers in Immunology. 7: 563. doi:10.3389/fimmu.2016.00563. PMC 5136547. PMID 27994593.
- ^ Offit PA (1994). "Rotaviruses: immunological determinants of protection against infection and disease". Advances in Virus Research. 44: 161–202. doi:10.1016/s0065-3527(08)60329-2. ISBN 978-0-12-039844-7. PMC 7130874. PMID 7817873.
- ^ Patel M, Glass RI, Jiang B, Santosham M, Lopman B, Parashar U (2013). "A systematic review of anti-rotavirus serum IgA antibody titer as a potential correlate of rotavirus vaccine efficacy". The Journal of Infectious Diseases. 208 (2): 284–294. doi:10.1093/infdis/jit166. PMID 23596320.
- ^ a b Patel MM, Tate JE, Selvarangan R, Daskalaki I, Jackson MA, Curns AT, Coffin S, Watson B, Hodinka R, Glass RI, Parashar UD (2007). "Routine laboratory testing data for surveillance of rotavirus hospitalizations to evaluate the impact of vaccination". The Pediatric Infectious Disease Journal. 26 (10): 914–919. doi:10.1097/INF.0b013e31812e52fd. PMID 17901797. S2CID 10992309.
- ^ The Pediatric ROTavirus European CommitTee (PROTECT) (2006). "The paediatric burden of rotavirus disease in Europe". Epidemiology and Infection. 134 (5): 908–916. doi:10.1017/S0950268806006091. PMC 2870494. PMID 16650331.
- ^ Angel J, Franco MA, Greenberg HB (2009). Mahy WJ, Van Regenmortel MH (eds.). Desk Encyclopedia of Human and Medical Virology. Boston: Academic Press. p. 278. ISBN 978-0-12-375147-8.
- ^ Goode J, Chadwick D (2001). Gastroenteritis viruses. New York: Wiley. p. 14. ISBN 978-0-471-49663-2.
- ^ Fischer TK, Gentsch JR (2004). "Rotavirus typing methods and algorithms". Reviews in Medical Virology. 14 (2): 71–82. doi:10.1002/rmv.411. PMC 7169166. PMID 15027000.
- ^ Alam NH, Ashraf H (2003). "Treatment of infectious diarrhea in children". Paediatric Drugs. 5 (3): 151–165. doi:10.2165/00128072-200305030-00002. PMID 12608880. S2CID 26076784.
- ^ Sachdev HP (1996). "Oral rehydration therapy". Journal of the Indian Medical Association. 94 (8): 298–305. PMID 8855579.
- ^ World Health Organization, UNICEF. "Joint Statement: Clinical Management of Acute Diarrhoea" (PDF). Retrieved 3 May 2012.
- ^ Ramig RF (2007). "Systemic rotavirus infection". Expert Review of Anti-infective Therapy. 5 (4): 591–612. doi:10.1586/14787210.5.4.591. PMID 17678424. S2CID 27763488.
- ^ Ahmadi E, Alizadeh-Navaei R, Rezai MS (2015). "Efficacy of probiotic use in acute rotavirus diarrhea in children: A systematic review and meta-analysis". Caspian Journal of Internal Medicine. 6 (4): 187–195. PMC 4649266. PMID 26644891.
- ^ Guarino A, Ashkenazi S, Gendrel D, Lo Vecchio A, Shamir R, Szajewska H (2014). "European Society for Pediatric Gastroenterology, Hepatology, and Nutrition/European Society for Pediatric Infectious Diseases evidence-based guidelines for the management of acute gastroenteritis in children in Europe: update 2014". Journal of Pediatric Gastroenterology and Nutrition. 59 (1): 132–152. doi:10.1097/MPG.0000000000000375. PMID 24739189. S2CID 4845135.
- ^ "Rotavirus vaccine for the prevention of rotavirus gastroenteritis among children. Recommendations of the Advisory Committee on Immunization Practices (ACIP)". MMWR. Recommendations and Reports. 48 (RR-2): 1–20. 1999. PMID 10219046.
- ^ Kapikian AZ (2001). "A rotavirus vaccine for prevention of severe diarrhoea of infants and young children: development, utilization and withdrawal". Gastroenteritis Viruses. Novartis Foundation Symposia. Vol. 238. pp. 153–171, discussion 171–179. doi:10.1002/0470846534.ch10. ISBN 978-0-470-84653-7. PMID 11444025.
- ^ Bines JE (2005). "Rotavirus vaccines and intussusception risk". Current Opinion in Gastroenterology. 21 (1): 20–25. PMID 15687880. Archived from the original on 11 May 2013. Retrieved 21 January 2008.
- ^ Bines J (2006). "Intussusception and rotavirus vaccines". Vaccine. 24 (18): 3772–3776. doi:10.1016/j.vaccine.2005.07.031. PMID 16099078.
- ^ Dennehy PH (2008). "Rotavirus vaccines: an overview". Clinical Microbiology Reviews. 21 (1): 198–208. doi:10.1128/CMR.00029-07. PMC 2223838. PMID 18202442.
- ^ Tate JE, Patel MM, Steele AD, Gentsch JR, Payne DC, Cortese MM, Nakagomi O, Cunliffe NA, Jiang B, Neuzil KM, de Oliveira LH, Glass RI, Parashar UD (2010). "Global impact of rotavirus vaccines". Expert Review of Vaccines. 9 (4): 395–407. doi:10.1586/erv.10.17. PMID 20370550. S2CID 28963507.
- ^ Tate JE, Parashar UD (2014). "Rotavirus Vaccines in Routine Use". Clinical Infectious Diseases. 59 (9): 1291–1301. doi:10.1093/cid/ciu564. PMID 25048849.
- ^ Richardson V, Hernandez-Pichardo J, et al. (2010). "Effect of Rotavirus Vaccination on Death From Childhood Diarrhea in Mexico". The New England Journal of Medicine. 362 (4): 299–305. doi:10.1056/NEJMoa0905211. PMID 20107215. S2CID 27287753.
- ^ Patel M, Pedreira C, De Oliveira LH, Umaña J, Tate J, Lopman B, Sanchez E, Reyes M, Mercado J, Gonzalez A, Perez MC, Balmaceda A, Andrus J, Parashar U (2012). "Duration of protection of pentavalent rotavirus vaccination in Nicaragua". Pediatrics. 130 (2): e365–e372. doi:10.1542/peds.2011-3478. PMID 22753550. S2CID 7723807.
- ^ a b Omatola CA, Olaniran AO (April 2022). "Rotaviruses: From Pathogenesis to Disease Control-A Critical Review". Viruses. 14 (5): 875. doi:10.3390/v14050875. PMC 9143449. PMID 35632617.
- ^ Patel MM, Parashar UD, et al. (2011). "Real World Impact of Rotavirus Vaccination". Pediatric Infectious Disease Journal. 30 (1): S1–S5. doi:10.1097/INF.0b013e3181fefa1f. PMID 21183833. S2CID 1893099.
- ^ Neuzil KM, Armah GE, Parashar UD, Steele AD (2010). Steele AD, Armah GE, Page NA, Cunliffe NA (eds.). "Rotavirus Infection in Africa: Epidemiology, Burden of Disease, and Strain Diversity". Journal of Infectious Diseases. 202 (Suppl 1): S1–S265. doi:10.1086/653545. PMID 20684687.
- ^ Nelson EA, Widdowson MA, Kilgore PE, Steele D, Parashar UD, eds. (2009). "Rotavirus in Asia: Updates on Disease Burden, Genotypes and Vaccine Introduction". Vaccine. 27 (Suppl 5): F1–F138.
- ^ World Health Organization (2009). "Rotavirus vaccines: an update" (PDF). Weekly Epidemiological Record. 51–52 (84): 533–540. Retrieved 8 May 2012.
- ^ "New vaccine to help protect babies against rotavirus". UK Department of Health. 10 November 2012. Retrieved 10 November 2012.
- ^ Karafillakis E, Hassounah S, Atchison C (2015). "Effectiveness and impact of rotavirus vaccines in Europe, 2006–2014". Vaccine. 33 (18): 2097–2107. doi:10.1016/j.vaccine.2015.03.016. PMID 25795258.
- ^ Burnett E, Jonesteller CL, Tate JE, Yen C, Parashar UD (2017). "Global Impact of Rotavirus Vaccination on Childhood Hospitalizations and Mortality from Diarrhea". The Journal of Infectious Diseases. 215 (11): 1666–1672. doi:10.1093/infdis/jix186. PMC 5543929. PMID 28430997.
- ^ "Rotavirus Deaths & Rotavirus Vaccine Introduction Maps – ROTA Council". rotacouncil.org. Archived from the original on 12 July 2016. Retrieved 29 July 2016.
- ^ Moszynski P (2011). "GAVI rolls out vaccines against child killers to more countries". BMJ. 343: d6217. doi:10.1136/bmj.d6217. PMID 21957215. S2CID 7567316.
- ^ "Rotavirus vaccination tied to lower rates of type 1 diabetes". Reuters. 22 January 2019. Retrieved 10 February 2019.
- ^ Bakalar N (30 January 2019). "Rotavirus Vaccine May Protect Against Type 1 Diabetes". The New York Times. ISSN 0362-4331. Retrieved 10 February 2019.
- ^ Parashar UD, Gibson CJ, Bresse JS, Glass RI (2006). "Rotavirus and severe childhood diarrhea". Emerging Infectious Diseases. 12 (2): 304–306. doi:10.3201/eid1202.050006. PMC 3373114. PMID 16494759.
- ^ Tate JE, Burton AH, Boschi-Pinto C, Steele AD, Duque J, Parashar UD (2012). "2008 estimate of worldwide rotavirus-associated mortality in children younger than 5 years before the introduction of universal rotavirus vaccination programmes: a systematic review and meta-analysis". The Lancet Infectious Diseases. 12 (2): 136–141. doi:10.1016/S1473-3099(11)70253-5. PMID 22030330.
- ^ Rheingans RD, Heylen J, Giaquinto C (2006). "Economics of rotavirus gastroenteritis and vaccination in Europe: what makes sense?". Pediatric Infectious Disease Journal. 25 (Suppl 1): S48–S55. doi:10.1097/01.inf.0000197566.47750.3d. PMID 16397429. S2CID 3272810.
- ^ Ryan MJ, Ramsay M, Brown D, Gay NJ, Farrington CP, Wall PG (1996). "Hospital admissions attributable to rotavirus infection in England and Wales". Journal of Infectious Diseases. 174 (Suppl 1): S12–S18. doi:10.1093/infdis/174.Supplement_1.S12. PMID 8752285.
- ^ Atchison CJ, Tam CC, Hajat S, van Pelt W, Cowden JM, Lopman BA (2010). "Temperature-dependent transmission of rotavirus in Great Britain and The Netherlands". Proceedings of the Royal Society B: Biological Sciences. 277 (1683): 933–942. doi:10.1098/rspb.2009.1755. PMC 2842727. PMID 19939844.
- ^ Levy K, Hubbard AE, Eisenberg JN (2009). "Seasonality of rotavirus disease in the tropics: a systematic review and meta-analysis". International Journal of Epidemiology. 38 (6): 1487–1496. doi:10.1093/ije/dyn260. PMC 2800782. PMID 19056806.
- ^ Koopmans M, Brown D (1999). "Seasonality and diversity of Group A rotaviruses in Europe". Acta Paediatrica. 88 (Suppl 426): 14–19. doi:10.1111/j.1651-2227.1999.tb14320.x. PMID 10088906. S2CID 10969637.
- ^ Sassi HP, Sifuentes LY, Koenig DW, Nichols E, Clark-Greuel J, Wong LF, McGrath K, Gerba CP, Reynolds KA (2015). "Control of the spread of viruses in a long-term care facility using hygiene protocols". American Journal of Infection Control. 43 (7): 702–706. doi:10.1016/j.ajic.2015.03.012. PMID 25944726.
- ^ Hopkins RS, Gaspard GB, Williams FP, Karlin RJ, Cukor G, Blacklow NR (1984). "A community waterborne gastroenteritis outbreak: evidence for rotavirus as the agent". American Journal of Public Health. 74 (3): 263–265. doi:10.2105/AJPH.74.3.263. PMC 1651463. PMID 6320684.
- ^ Bucardo F, Karlsson B, Nordgren J, Paniagua M, González A, Amador JJ, Espinoza F, Svensson L (2007). "Mutated G4P[8] rotavirus associated with a nationwide outbreak of gastroenteritis in Nicaragua in 2005". Journal of Clinical Microbiology. 45 (3): 990–997. doi:10.1128/JCM.01992-06. PMC 1829148. PMID 17229854.
- ^ Linhares AC, Pinheiro FP, Freitas RB, Gabbay YB, Shirley JA, Beards GM (1981). "An outbreak of rotavirus diarrhea among a non-immune, isolated South American Indian community". American Journal of Epidemiology. 113 (6): 703–710. doi:10.1093/oxfordjournals.aje.a113151. PMID 6263087.
- ^ Hung T, Wang C, Fang Z, Chou Z, Chang X, Liong X, Chen G, Yao H, Chao T, Ye W, Den S, Chang W (1984). "Waterborne outbreak of rotavirus diarrhea in adults in China caused by a novel rotavirus". The Lancet. 323 (8387): 1139–1142. doi:10.1016/S0140-6736(84)91391-6. PMID 6144874. S2CID 54346351.
- ^ Fang ZY, Ye Q, Ho MS, Dong H, Qing S, Penaranda ME, Hung T, Wen L, Glass RI (1989). "Investigation of an outbreak of adult diarrhea rotavirus in China". Journal of Infectious Diseases. 160 (6): 948–953. doi:10.1093/infdis/160.6.948. PMID 2555422.
- ^ Kelkar SD, Zade JK (2004). "Group B rotaviruses similar to strain CAL-1, have been circulating in Western India since 1993". Epidemiology and Infection. 132 (4): 745–749. doi:10.1017/S0950268804002171. PMC 2870156. PMID 15310177.
- ^ Ahmed MU, Kobayashi N, Wakuda M, Sanekata T, Taniguchi K, Kader A, Naik TN, Ishino M, Alam MM, Kojima K, Mise K, Sumi A (2004). "Genetic analysis of group B human rotaviruses detected in Bangladesh in 2000 and 2001". Journal of Medical Virology. 72 (1): 149–155. doi:10.1002/jmv.10546. PMID 14635024. S2CID 21258083.
- ^ Penaranda ME, Ho MS, Fang ZY, Dong H, Bai XS, Duan SC, Ye WW, Estes MK, Echeverria P, Hung T (1989). "Seroepidemiology of adult diarrhea rotavirus in China, 1977 to 1987". Journal of Clinical Microbiology. 27 (10): 2180–2183. doi:10.1128/JCM.27.10.2180-2183.1989. PMC 266989. PMID 2479654.
- ^ Moon S, Humphrey CD, Kim JS, Baek LJ, Song JW, Song KJ, Jiang B (2011). "First detection of group C rotavirus in children with acute gastroenteritis in South Korea". Clinical Microbiology and Infection. 17 (2): 244–247. doi:10.1111/j.1469-0691.2010.03270.x. PMID 20491826.
- ^ "Rotavirus vaccination programme for infants". www.gov.uk. Public Health England. 26 July 2013.
- ^ Dadonaite B, Ritchie H (2019). "Rotavirus vaccine – an effective tool that prevents children dying from diarrhea". Our World in Data.
- ^ a b Martella V, Bányai K, Matthijnssens J, Buonavoglia C, Ciarlet M (2010). "Zoonotic aspects of rotaviruses". Veterinary Microbiology. 140 (3–4): 246–255. doi:10.1016/j.vetmic.2009.08.028. PMID 19781872.
- ^ Müller H, Johne R (2007). "Rotaviruses: diversity and zoonotic potential—a brief review". Berliner und Munchener Tierarztliche Wochenschrift. 120 (3–4): 108–112. PMID 17416132.
- ^ Cook N, Bridger J, Kendall K, Gomara MI, El-Attar L, Gray J (2004). "The zoonotic potential of rotavirus". The Journal of Infection. 48 (4): 289–302. doi:10.1016/j.jinf.2004.01.018. PMID 15066329.
- ^ Dóró R, Farkas SL, Martella V, Bányai K (2015). "Zoonotic transmission of rotavirus: surveillance and control". Expert Review of Anti-infective Therapy. 13 (11): 1337–1350. doi:10.1586/14787210.2015.1089171. PMID 26428261. S2CID 42693014.
- ^ Light JS, Hodes HL (1943). "Studies on Epidemic Diarrhea of the New-born: Isolation of a Filtrable Agent Causing Diarrhea in Calves". American Journal of Public Health and the Nation's Health. 33 (12): 1451–1454. doi:10.2105/AJPH.33.12.1451. PMC 1527675. PMID 18015921.
- ^ Mebus CA, Wyatt RG, Sharpee RL, Sereno MM, Kalica AR, Kapikian AZ, Twiehaus MJ (1976). "Diarrhea in gnotobiotic calves caused by the reovirus-like agent of human infantile gastroenteritis" (PDF). Infection and Immunity. 14 (2): 471–474. doi:10.1128/IAI.14.2.471-474.1976. PMC 420908. PMID 184047.
- ^ Rubenstein D, Milne RG, Buckland R, Tyrrell DA (1971). "The growth of the virus of epidemic diarrhoea of infant mice (EDIM) in organ cultures of intestinal epithelium". British Journal of Experimental Pathology. 52 (4): 442–445. PMC 2072337. PMID 4998842.
- ^ a b Woode GN, Bridger JC, Jones JM, Flewett TH, Davies HA, Davis HA, White GB (1976). "Morphological and antigenic relationships between viruses (rotaviruses) from acute gastroenteritis in children, calves, piglets, mice, and foals" (PDF). Infection and Immunity. 14 (3): 804–810. doi:10.1128/IAI.14.3.804-810.1976. PMC 420956. PMID 965097.
- ^ a b Flewett TH, Woode GN (1978). "The rotaviruses". Archives of Virology. 57 (1): 1–23. doi:10.1007/BF01315633. PMC 7087197. PMID 77663.
- ^ Flewett TH, Bryden AS, Davies H, Woode GN, Bridger JC, Derrick JM (1974). "Relation between viruses from acute gastroenteritis of children and newborn calves". The Lancet. 304 (7872): 61–63. doi:10.1016/S0140-6736(74)91631-6. PMID 4137164.
- ^ Matthews RE (1979). "Third report of the International Committee on Taxonomy of Viruses. Classification and nomenclature of viruses". Intervirology. 12 (3–5): 129–296. doi:10.1159/000149081. PMID 43850.
- ^ Beards GM, Brown DW (1988). "The antigenic diversity of rotaviruses: significance to epidemiology and vaccine strategies". European Journal of Epidemiology. 4 (1): 1–11. doi:10.1007/BF00152685. PMID 2833405. S2CID 11547573.
- ^ Urasawa T, Urasawa S, Taniguchi K (1981). "Sequential passages of human rotavirus in MA-104 cells". Microbiology and Immunology. 25 (10): 1025–1035. doi:10.1111/j.1348-0421.1981.tb00109.x. PMID 6273696. S2CID 25276891.
- ^ Ward RL, Bernstein DI (2009). "Rotarix: a rotavirus vaccine for the world". Clinical Infectious Diseases. 48 (2): 222–228. doi:10.1086/595702. PMID 19072246.
External links
[edit] Medicine portal
Medicine portal Viruses portal
Viruses portal Media related to Rotavirus at Wikimedia Commons
Media related to Rotavirus at Wikimedia Commons
| DNA |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| RNA |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| RT |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| DNA |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| RNA |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| RT |
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Adulterants, food contaminants | |
|---|---|
| Food additives | |
| Intestinal parasites, parasitic disease | |
| Microorganisms | |
| Pesticides | |
| Preservatives | |
| Sugar substitutes | |
| Toxins, poisons, environment pollution | |
| Food fraud | |
| Food processing | |
| Food contamination incidents |
|
| Regulation, standards, watchdogs | |
| Institutions |
|
| Related topics | |
![The seasonal variation of rotavirus A infections in England: rates of infection peak during the winter months.[144]](https://upload.wikimedia.org/wikipedia/commons/thumb/4/4e/Rotavirus_seasonal_distribution.png/650px-Rotavirus_seasonal_distribution.png)
![Preventable child deaths from rotavirus vaccination, 2016. Annual number of preventable deaths in children under five years old from rotavirus if full coverage of the rotavirus vaccine was achieved.[145]](https://upload.wikimedia.org/wikipedia/commons/thumb/8/81/Avertable-deaths-from-rotavirus-with-full-vaccine-coverage.png/650px-Avertable-deaths-from-rotavirus-with-full-vaccine-coverage.png)